
Topcon’s Swept Source (SS)-optical coherence tomography (OCT) has important physical properties that make it a more advanced and superior tool, in comparison to Spectral Domain (SD)-OCT, for visualisation of choroidal or retinal tumors. These properties include a wavelength of 1050 nm for SS-OCT versus 840 nm for SD-OCT, as well as an improved signal to noise ratio. While it's possible to obtain a scan in the deep choroid of almost equal quality by using modifications of an SD-OCT, such as the EDI module, there are still two major differences between taking a scan with SS-OCT and SD-OCT. First, with EDI the signal on the retinal surface and in the vitreous is not as clear; second, and perhaps even more importantly, the acquisition time has been found to be 83-fold shorter with the SS-OCT. This speed equates to efficiency that represents a clear benefit in daily practice.
SS-OCT offers advantages that can be demonstrated in numerous applications. For instance, this technology is effective for precise measurement and monitoring of choroidal nevi. SS-OCT is superior compared to the conventional ultrasonography especially in lesions less than 1.5 mm thick. Nevi may grow towards vitreous or even sclera. Though different morphological features are seen in melanomas and nevi, there is no clear criterion based on OCT helping to differentiate between these two entities.
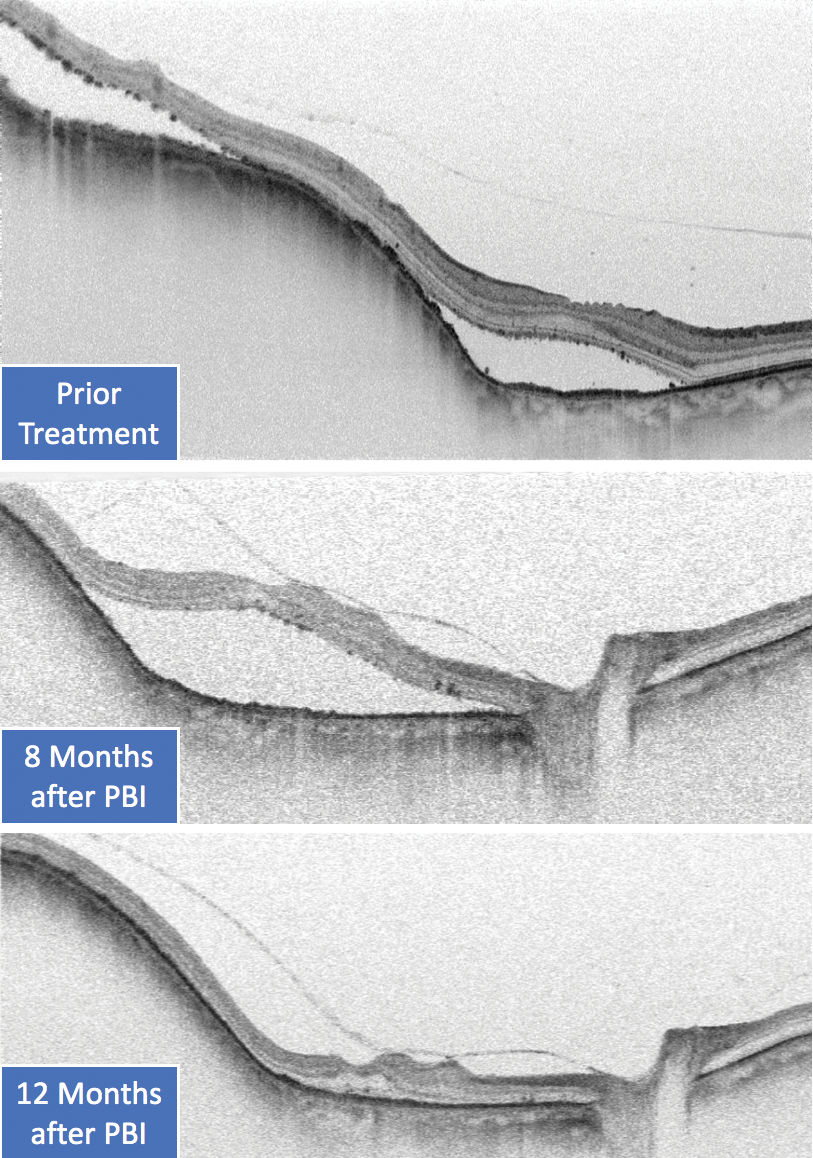
Figure 1. SS-OCT showing exudative detachment after radiotherapy of choroidal melanomas.
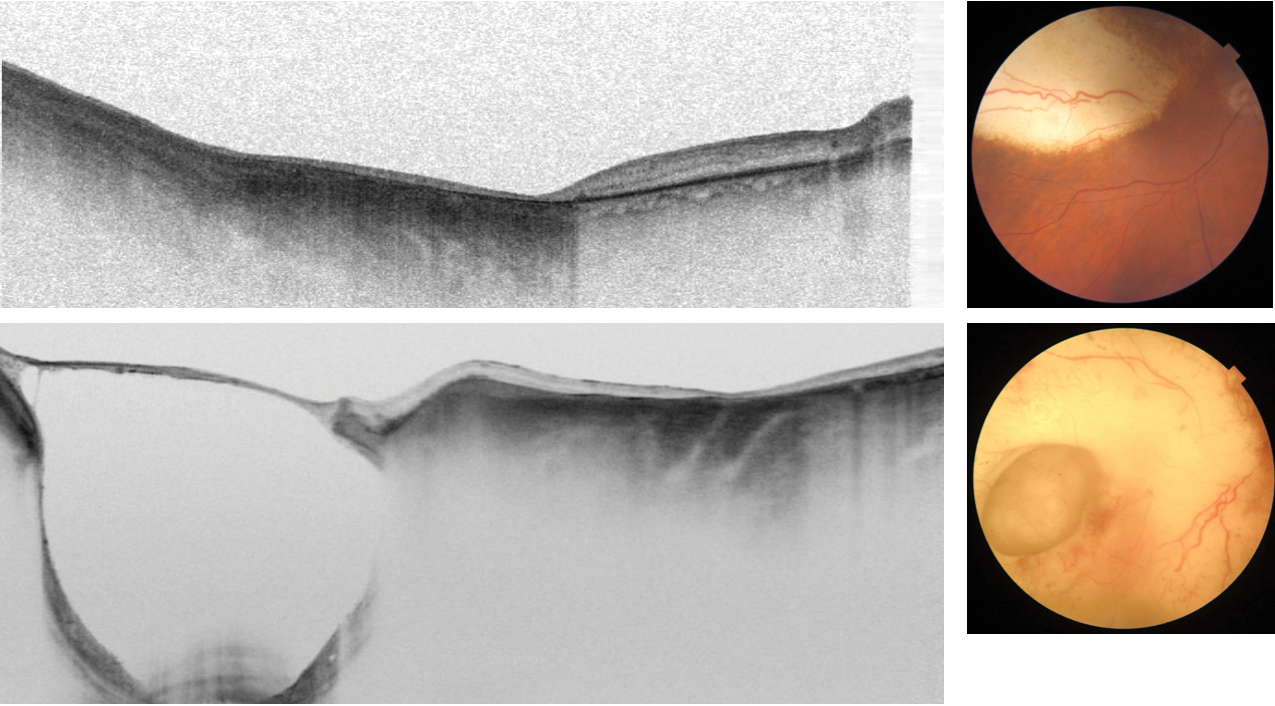
Figure 2. SS-OCT showing scleral ectasia/necrosis after radiotherapy of choroidal melanomas.
SS-OCT helps in the detection of secondary effects after radiotherapy of choroidal melanomas, such as exudative detachment (Figure 1) or scleral ectasia/necrosis (Figure 2). SS-OCT with a clear signal in vitreous, retina, and choroid is an ideal tool for monitoring treatment response in posterior uveitis via detection of the inflammatory response in the vitreous, the retina deposits, and exudative changes, as well the choroidal infiltrates in just one scan. In this example of posterior uveitis, SS-OCT imaging compares progress 1 week after oral steroids and 3 months after no medication (Figures 3 and 4).
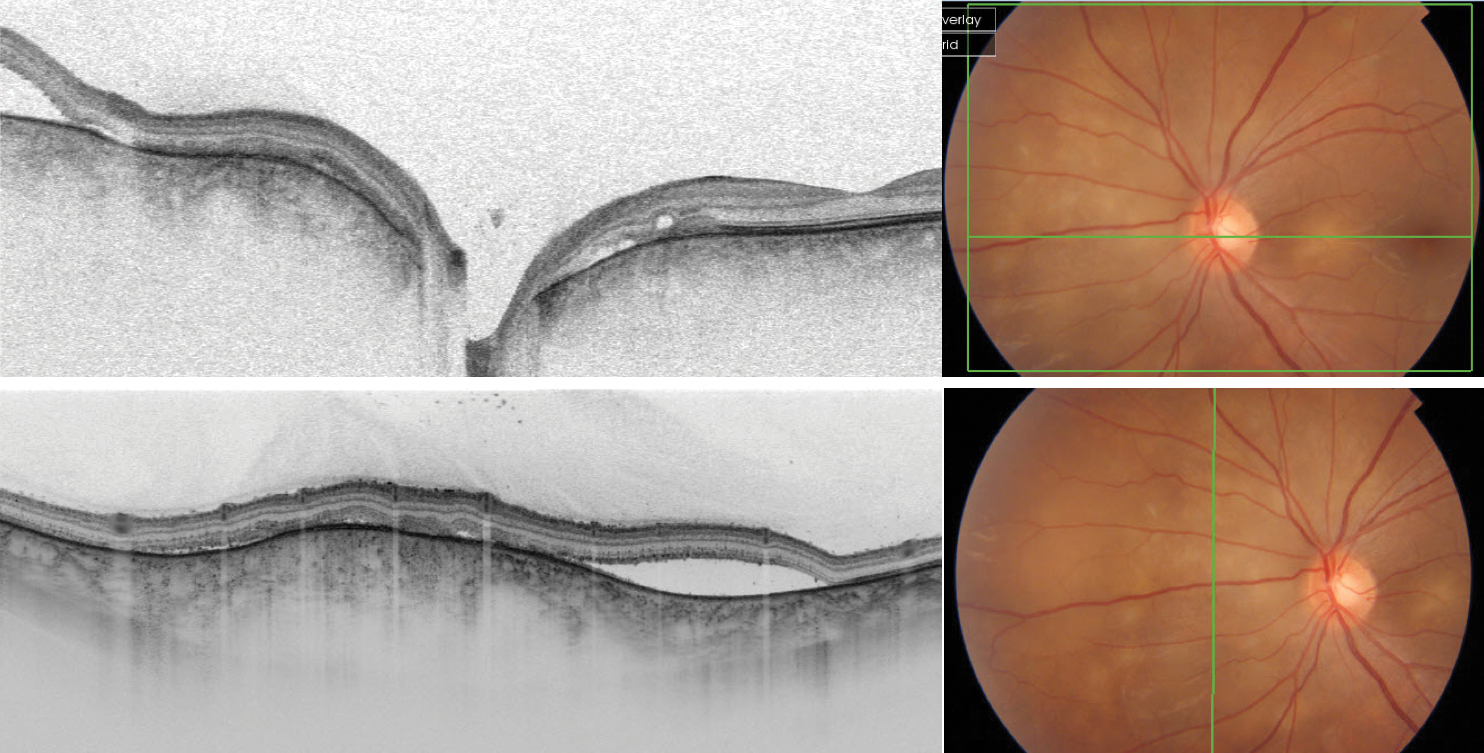
Figure 3. SS-OCT showing a case of posterior uveitis.
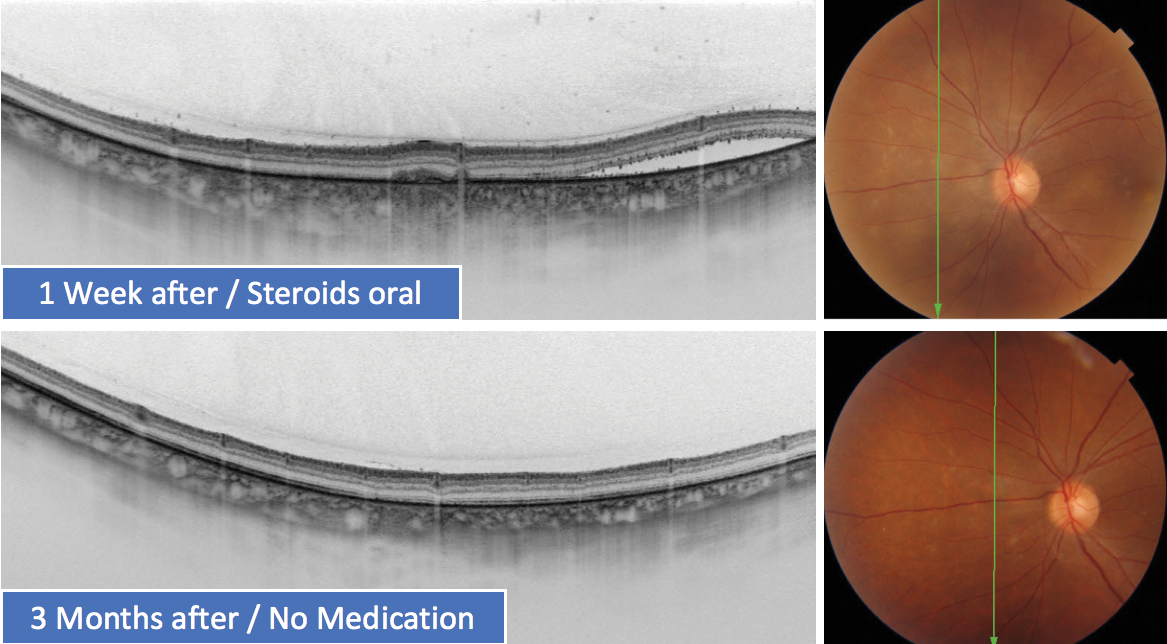
Figure 4. SS-OCT showing progress 1 week after oral steroids and 3 months after no medication in a case of posterior uveitis.
Choroidal hemangiomas can be well visualized by SS-OCT and have a typical pattern with the blood-filled cavernous, and retinal angiomas can be diagnosed and monitored by OCT angiography (OCTA), which also enables a clear differential diagnosis to juxtapapillary choroidal neovascularization (CNV) (Figure 5A, see Image Series).
IMAGE SERIES
Exophytic Papillary Angioma
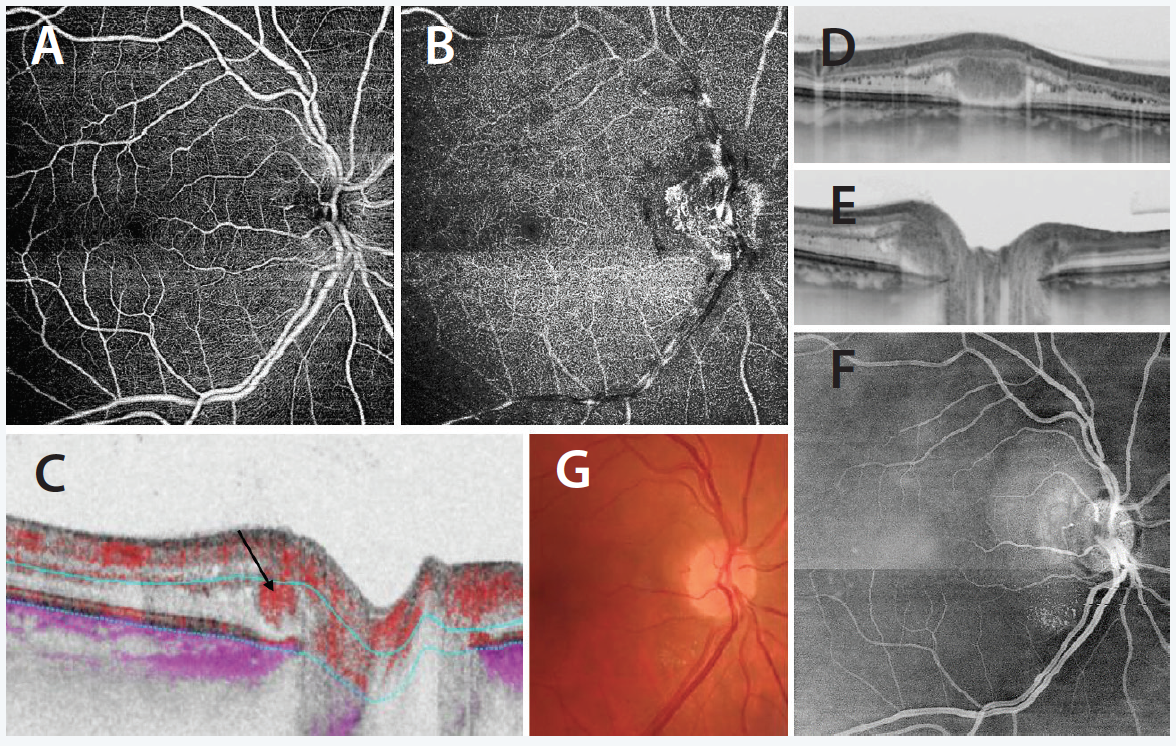
This imaging represents the diagnosis of exophytic papillary angioma (Figure 5A through 5G). We performed a 9x9 mm SS-OCTA scan using the central fixation to get both macula and optic disc visualized in one scan. The SS-OCTA of the superficial capillaries (5A) was normal, but in the deeper layer (5B), a vascular structure was detected at the temporal margin of the optic disc. On B-Scan a solid intraretinal mass with confined vascular flow (5C, arrow) was shown. There was no contact to retinal pigment epithelium (RPE), and the SS-OCTA of the sub-RPE layers was normal so that a juxtapapillary CNV could be excluded. The diagnosis of an exophytic papillary angioma was made. The dimension of the angioma (BxLxH 640x1028x276 µm) was measured by vertical and horizontal B-Scans (5D, 5E). The En Face mode (5F) demonstrated much more detailed information about the two-dimensional extend of the angioma and the surrounding exudation compared to the fundus photo (5G).
Our use of SS-OCT indicates that its limitations are minor. For instance, the signal is limited by heavy pigmentation of the tumor; tumors with a maximum thickness of up to 1.8 mm to 2.0 mm may be visualized in toto, and, of course, it does not detect lesions outside of the central 30° to 40° of the fundus.
In conclusion, SS-OCT is the best available OCT technology for visualising tumors within the eye. It's useful in differential diagnosis of flat melanocytic lesion, in measuring and monitoring lesion over time, in monitoring treatment, such as that of melanoma, angioma, and posterior uveitis; and OCTA adds valuable information especially in vascular tumors.
