This article provides an overview of anesthesia for complex cataract procedures. Most of the principles discussed are applicable to noncataract procedures as well.
WHAT CONSTITUTES A COMPLEX CATARACT PROCEDURE?
As defined by Current Procedural Terminology code 66982, a complex cataract procedure is an “extracapsular cataract extraction removal with insertion of intraocular lens prosthesis (one-stage procedure), manual or mechanical technique (eg, irrigation and aspiration or phacoemulsification), complex, requiring devices or techniques not generally used in routine cataract surgery (eg, iris expansion device, suture support for intraocular lens, or primary posterior capsulorrhexis) or performed on patients in the amblyogenic developmental stage.” Most ophthalmologists do not limit their concept of complex cases to those requiring additional devices or to surgery during infancy. Additional factors include ocular and systemic comorbidities or high-risk characteristics and the medical and surgical history of the eye.
THE GOALS
The primary goal of anesthesia is to make surgery safe and comfortable for the patient. It is also important to maintain physiologic homeostasis. In other words, the surgical experience should not induce cardiac, respiratory, renal, neurologic, psychological, or other systemic stress.
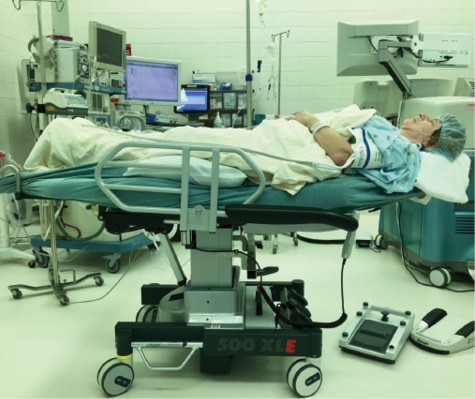
Figure 1. The patient should be made comfortable with one or more pillows beneath the knees and one or more towels beneath the head.
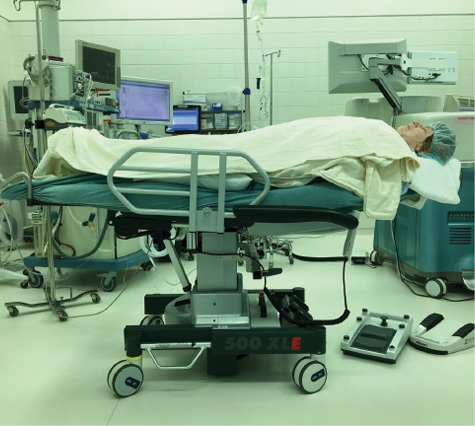
Figure 2. An extra blanket or two placed on top of the patient will provide additional comfort, particularly when the OR is cold.
Common obstacles to achieving these goals include patients’ expectations. People may carry emotional baggage from operations in which they experienced intraoperative or postoperative pain, postoperative nausea and vomiting, claustrophobia, or simply the cold of the OR. Patients may volunteer information on these negative experiences preoperatively. If not, physicians and their staff should make an effort to determine if a patient has such a history.
Many patients want to be “knocked out” and awakened after a procedure. Some, if not most, patients have to be informed that the administration of high doses of intravenous sedatives and narcotics without a secure airway is unsafe. Most people do not want a laryngeal mask airway or endotracheal tube down their throat, yet they do not want to be aware of anything, either. These individuals must be informed that they cannot have it both ways!
Regular communication before and during surgery is fundamental. In my experience, patients will tolerate a lot if they understand what is happening and why this or that is being done. I find this especially true of claustrophobic patients, who require handholding, a greater amount of intravenous sedation than is typical, and breathing room beneath the drape. They often do very well under topical anesthesia if they can see out of the eye having surgery, because it makes them feel less caged in.
Systemic comorbidities may also get in the way of effective anesthesia. Common conditions include kyphosis, osteoarthritis, fractures of the neck and back, disc disease, congestive heart failure, chronic obstructive pulmonary disease, tremors, chronic cough, postnasal drip, and overall poor health. Some patients are simply fidgety and cannot lie still. Each of these potential problems needs to be anticipated and managed.
MAKING EVERYONE COMFORTABLE
Everyone in the OR should be reasonably comfortable. This includes the patient, surgeon, anesthesia staff, scrub technician, and circulating nurse. The patient should be placed in a supine position with one or more pillows under the knees, one or more towels under the head, and warm blankets on top (Figures 1 and 2). If the patient’s elbows abut the frame of the gurney, he or she should be given elbow pads. The height of the gurney and the location of the microscope should be adjusted so that the surgeon is comfortable. Verbal communication between the surgeon and patient is crucial for smooth flow. In my experience, “vocal local” goes a long way toward easing patients’ anxiety. I provide a “color commentary” on each thing I expect a patient to feel or experience so that he or she is not taken by surprise.
DECIDING WHICH ANESTHETIC APPROACH IS BEST
Overview
Prior to surgery, it is important to come up with an anesthetic plan that takes all of the facts into account. The patient should be involved in the decision. Factors include the length and extent of the procedure, anticipated difficulty, and whether or not the patient is monocular. Manipulations that cause greater discomfort such as conjunctival incision, scleral dissection or puncture, cautery, intraocular suturing, and iris manipulation may favor an injection or general anesthesia approach over topical anesthesia. High-risk characteristics such as a deep-set eye, narrow lid fissure, shallow anterior chamber, poorly dilating pupil, dense brunescent cataract, or severe zonular laxity argue against topical anesthesia.
When Topical Anesthesia Is Appropriate
Topical anesthesia, usually with intracameral supplementation, is appropriate for most routine cases when performed by an experienced surgeon. It is also appropriate for more difficult procedures that will be relatively short and involve little manipulation of the iris, ciliary muscle, and sclera. Topical anesthesia is virtually a necessity for laser cataract surgery, because proper alignment during docking depends on patient fixation. Hooks, rings, and pupil expansion devices can be inserted or implanted comfortably under topical anesthesia as long as the ocular manipulations involving these devices are slow and deliberate. In addition, trabecular bypass devices can be implanted and goniotomy performed comfortably under topical anesthesia. For monocular patients, topical anesthesia is the approach of choice, barring significant ocular comorbidity or surgical difficulty.
Watch it Now
Kevin M. Miller, MD, supplements this article with a presentation on approaches to anesthesia for cataract surgery in patients with ocular comorbidities.
When Injection Anesthesia Is Better
Injection anesthesia is preferable whenever the surgeon expects ocular manipulations to cause the patient discomfort. This is likely to be the situation with long cases, during which topical anesthesia is likely to wear off, and when there will be iris or ciliary body manipulation such as when working in a tight anterior chamber. Injection anesthesia is generally preferred whenever cautery will be used.
When General Anesthesia May Be Necessary
General anesthesia is appropriate for infants, children, and uncooperative adults. The last includes patients who are immature, those who are mentally challenged or delayed, and those who have an extreme phobia regarding surgery. General anesthesia should also be offered to monocular patients who have ocular comorbidities or high-risk features that will make surgery under topical anesthesia risky or uncomfortable. It is important for monocular patients to be able to leave the surgical facility seeing from their only eye.
POSTOPERATIVE OCULAR DISCOMFORT AND PAIN
The surgeon’s responsibility to his or her patients does not end in the OR. It is important for the surgeon and the entire surgical team, including the anesthesia and nursing staff, to manage patients’ ocular discomfort or pain in the recovery room and to provide guidance on pain management after discharge.
CONCLUSION
A commonsense approach to anesthesia care dictates that patients participate in the decision-making process. The anesthetic approach is usually guided by the circumstances of the patient, the condition of the eye, and any concurrent systemic comorbidities or high-risk characteristics. The surgeon’s communication with patients, attention to their comfort, and management of their postoperative ocular discomfort or pain are important to the overall care process. n
Kevin M. Miller, MD
• Kolokotrones chair in ophthalmology, David Geffen School of Medicine at UCLA, Jules Stein Eye Institute, Los Angeles
• (310) 206-9951; kmiller@ucla.edu