

Is your new associate seeing enough patients? Are you leaving revenue on the table? How are your patients contacted before their bill is adjusted or sent to collections? You may know the answers to these questions based on data you have collected in your practice, but only by comparing these data over time to standards within your specialty will you know if there is room for improvement.
Practice consultants and administrators are not the only ones who should be able to identify and evaluate benchmarks to take an analytical look at a practice’s well-being. It is incumbent on practice owners, and especially a practice’s managing partner, to achieve at least a rudimentary command of relevant benchmarking values.
SEEING YOUR PRACTICE AS A PATIENT
If you want to use benchmarking to learn more about your practice, don’t try to think like a businessperson; instead, rely on your training as a physician and consider your practice as one very large, complex patient. In medicine, there are conventions for how things are measured; for instance, we measure pulse in beats per minute, not beats per hour. Similarly, there are conventions for how we measure what goes into effectively running a practice. These are known as key performance indicators (KPIs).
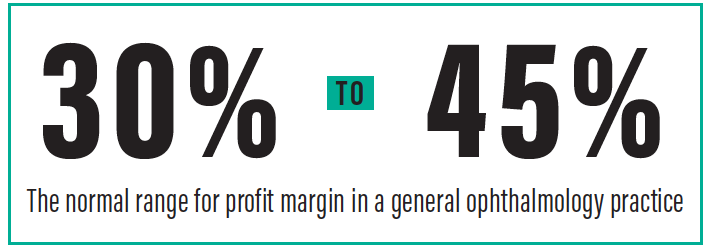
Like each of the physiologic norms that you use to track the health of your patients’ eyes, each KPI has a normal range. Just as the normal range for visual acuity is around 20/20, the normal range for profit margin in a general ophthalmology practice is 30% to 45%.
But the physiologic norms are not the same for every patient. For example, a young child might have a normal blood pressure different from that of an adult or an elderly person. In the same fashion, the objective measurements we take of a practice, and the norms for those measurements, will vary depending on the type of practice. For instance, we don’t expect the profit margin of a pediatric ophthalmology practice or a contact lens practice to be the same as the profit margin for a refractive surgery, retina, or oculoplastics practice.
There are about 50 KPIs described in great detail in John Pinto’s Little Green Book of Ophthalmology, 5th edition, which was recently updated to reflect current standards and norms.1 These are some of the KPIs used to assess ophthalmic practices:
- Profit margin;
- Revenue growth rate;
- Total and established patient growth rate;
- Average revenue per patient visit;
- Surgical density (the ratio of visits to surgical cases);
- Optical sales per patient visit; and
- Cost margins for staff, facilities, and marketing.
SEEKING CAUSES
Consultants typically look at several values to determine the reasons for any changes in the general health and well-being of a practice. For example, if a practice’s collections are faltering, this change could be driven by a number of things. Is the practice not seeing as many patients? Has surgical density gone down? Is the billing department not doing its work effectively? Or is someone diverting funds from the practice?
All of these primary data points must be considered in an effort to tease out secondary data. For example, if collections are decreasing, the practice might consider the following: Did we lose any doctors or key staff? Are patient visits down compared with an earlier period baseline? Are we doing less surgery? Or is the average ticket (ie, total fee collection per visit) going down?
Practice managers might pull up a Current Procedural Terminology (CPT) report to see if, for instance, the incidence of special testing has diminished, and, if so, what the drivers for that are. They would also want to consider factors such as patient recall and continuity of care.
Many times, if a practice has noticed a decline in collections, a thorough review will reveal that a clerical staffer responsible for handling recall left the practice 6 months to a year earlier. That person may have been replaced by someone who was not properly trained on patient recall. The (delayed) result was a decrease in patient volume, not noted until later.
WORKING THE NUMBERS
Adopting the benchmarking process and learning the language can initially be challenging, but with a bit of effort it can be learned.
Consider this scenario: You look down the hall and there are four technicians standing around not appearing to be engaged in work. You come out of an exam room a bit later, and again the same technicians are chatting about their weekend. You register a subjective impression, and you want to determine whether you are overstaffed. A simple formula can enable you to establish the number of technicians needed to adequately support your practice’s physicians.
The technician efficiency formula is computed as follows: total technician payroll hours in a month divided by total patient visits (including postoperative visits) during the same month. The quotient should be approximately 1 tech hour per visit (see example below).
Technician efficiency formula
Assuming a full-time equivalent (FTE) schedule is 173 hours per month, if a practice handling 1,050 visits per month employs six FTE technicians (including technicians, scribes, and testers), the quotient is 1 tech hour per visit:
6 tech FTEs x 173 hrs per month / 1,050 visits = 1 tech hr per visit

If the managers of a general practice arrive at this figure, they can be assured they have the right number of technicians. If the same practice had six technicians but handled only 800 visits per month, then the practice would be paying for 1.3 technician payroll hours per visit. This would indicate that the technician staffing could be cut to about 4.6 FTE techs.
MAKING IT WORK
In the same way that KPIs and benchmarking can help to determine if you are under- or overstaffed, they can be used to help to determine if you have too many or too few facilities, if you are doing the standard amount of surgery for a given patient base, or if you are doing more or less diagnostic testing than similar practices.
Once you embrace benchmarking as integral to practice success, consider the following:
- Business and medicine are more alike than they are different;
- You don’t need a business education—your medical education has prepared you well to implement benchmarking;
- Collaborate with your administrator to make benchmarking a priority;
- Decide which benchmarks to track and how often to track them; and
- Start collecting data and focus on improving KPIs that fall outside of normal limits.
lasting improvement
Ultimately, data are only as useful as what you do with them. Just knowing where your practice stands compared with others is interesting, but perhaps it is not particularly helpful. When used correctly, benchmarking can help you contain costs, drive revenue, and manage staffing levels.
Setting achievable and measurable goals, regularly monitoring progress, and holding staff members accountable for their performance will set you on the path to lasting improvement.
1. John Pinto’s Little Green Book of Ophthalmology, 5th edition. American Society of Ophthalmic Administrators; 2018; Fairfax, Virginia.




