The standard imaging system for ophthalmic surgery is the surgical microscope. Many models are available, including those with dual coaxial illumination, that provide adequate to outstanding magnification and resolution of fine anatomic detail for both anterior and posterior segment surgery. To display and record video of the surgical field, many imaging systems allow the addition of a camera through a 50-50 beam-splitting arrangement. While operating, the surgeon looks through oculars, which can be adjusted for the user’s spherical refractive error. Additional eyewear is only required by individuals with significant uncorrected astigmatism.
Digital three-dimensional high-definition (3-D HD) visualization, as developed by TrueVision Systems, offers an exciting alternative to the standard microscope, because it improves surgical ergonomics; permits digital interfacing with pre-, intra-, and postoperative measurements; and allows the OR staff to work from the same picture. Additionally, 3-D HD visualization presents unique opportunities for education and training.1
SURGICAL ERGONOMICS
Although a straighter posture is healthier, many eye surgeons sit on a chair or stool and lean forward slightly to look into the microscope. Few surgeons have improved workplace ergonomics by leaning back and tilting the microscope 45º, as originally described by R. Bruce Wallace III, MD.2 The location of the microscope’s oculars significantly limits the range of physical positions an ophthalmologist can assume. In fact, routine cataract surgery can strain operating surgeons’ muscles and joints. It can also produce a flexion relaxation phenomenon, in which there is reduced muscular activity, indicating a transfer of loads to soft tissue structures, including the posterior ligaments, intervertebral discs, and sensitive neural sheaths.3 The impact of surgical ergonomics on ophthalmologists spurred the American Academy of Ophthalmology to develop a special task force.4
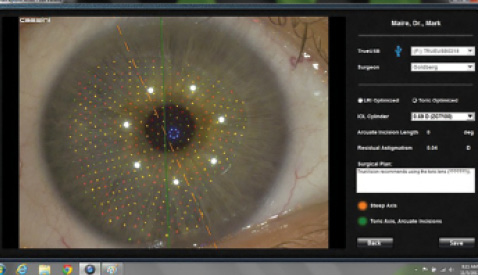
Figure. Preoperative corneal analysis from the Cassini Color LED Corneal Analyzer is registered to the intraoperative eye using automated feature detection.
Using a 3-D HD flat panel screen instead of looking through oculars frees the surgeon from restrictive positioning. The learning curve primarily involves repositioning some OR equipment to optimize the surgeon’s view and adjusting the color, contrast, brightness, and format of the image to create a surgeon-customized profile. Once accomplished, operating becomes easier. Thanks to improvements in the resolution and processing speed of TrueVision’s fifth-generation platform, the 3-D HD image on the screen is difficult to differentiate from the view through the oculars, in the author’s experience.
DIGITAL INTERFACES
The ability to wirelessly transmit data from the clinic to the OR creates efficiency and improves safety by eliminating the potential for errors in transcription and translation. For example, digital imaging and guidance facilitate the accurate placement of toric IOLs by eliminating the need to mark the ocular surface. Instead of carrying paper copies, printed instructions, and diagrams based on topography to the OR, information from preoperative diagnostic devices is transmitted digitally and displayed on the screen. As shown in the Figure, incorporating preoperative corneal analysis, including anterior and posterior corneal dimensions from the Cassini Color LED Corneal Analyzer (i-Optics), permits rapid determination of the correct astigmatic axis through the automated registration of ocular features. Additionally, software embedded in the imaging processor calculates the optimal placement of incisions within surgeon-prescribed parameters to minimize residual astigmatism.
THE OPERATING ENVIRONMENT
For the refractive cataract surgeon who sits temporally, the 3-D flat panel can be conveniently placed across from the operating bed at a comfortable distance. In this way, the scrub technician can observe the same image as the surgeon, in all its natural color and depth. Far superior to the small, standard video screens available in most ORs—and usually tucked away and hard to see in a far corner—the 3-D HD flat panel fosters the OR staff’s understanding of anterior segment surgery. The scrub technician remains aware of the surgeon’s every move, enhancing the flow of each procedure.
The impact of the 3-D surgical imagery on visiting surgeons, industry representatives, or family members is immediate and dramatic. I remember one woman who said, at the conclusion of her husband’s cataract procedure, that she was no longer afraid to have eye surgery herself. “Seeing it all on the big screen, it’s beautiful,” she told me.
EDUCATION AND BEYOND
Teaching a procedure that is performed in 3-D with video that is presented in two dimensions places unnecessary limitations on students’ understanding. For example, they have to extrapolate the depth of an instrument in the anterior chamber from clues such as angles and shadow. Sometimes, it is hard for surgeons to know with certainty where they are until, suddenly, it is all too clear. Presentations in 3-D HD make concepts easier to grasp through visualization.1
Today, the ophthalmic surgery suite is becoming more fully integrated in the clinic with the advent of wireless communication for preoperative diagnostic instruments and intraoperative imaging and guidance tools. Closing the loop by communicating intraoperative decision making to postoperative outcomes analysis encourages continuous quality improvement while eliminating data entry tasks that bog down a clinic. For instance, an implanted IOL’s spherical and toric powers and final alignment at the conclusion of a case may be wirelessly transmitted to an electronic medical record and database for later analysis of the postoperative refraction.
CONCLUSION
Digital imaging makes sense for refractive cataract surgery because of the array of information it makes available in the OR. Three-dimensional digital imaging also creates a healthier environment for the surgeon, allows complete integration of preoperative diagnostic testing, and promotes a cycle of innovation and learning.n
1. Packer M. TrueVision 3D HD for teaching and training. Cataract & Refractive Surgery Today. March 2011;11(3):41-42. http://crstoday.com/2011/03/truevision-3d-hd-for-teaching-and-training.
2. Wallace RB. The 45 degree tilt: improvement in surgical ergonomics. J Cataract Refract Surg. 1999;25:174-176.
3. Marx JL, Wertz FD, Dhimitri KC. Work-related musculoskeletal disorders in ophthalmologists. Techniques in
Ophthalmology. 2005;3(1):54-61.
4. Kent C. Will ophthalmology cripple you? Review of Ophthalmology. Published October 2011.
http://www.reviewofophthalmology.com/content/i/1650/c/30458/. Accessed November 10, 2014.
Mark Packer, MD, CPI
• president of Mark Packer MD Consulting and the medical director of Boulder Eyes in Boulder, Colorado
• mark@markpackerconsulting.com
• consultant to and holds equity in TrueVision Systems


