



Cataract surgery has evolved rapidly, transitioning from simple removal of the cloudy lens to the provision of increased spectacle independence. The past decade is full of significant milestones, such as the introduction of femtosecond laser technology in 2011, enhanced astigmatism correction with laser arcuate incisions and toric IOLs, the introduction of extended depth of focus lenses in 2017, and the FDA approval of the Light Adjustable Lens (RxSight) in 2017. These and other developments have expanded surgical options to the benefit of both patients and surgeons and allowed greater customization of the procedure and its outcomes.
IOL selection, however, has become increasingly complex. Surgeons must now take the patient’s personality, occupation, hobbies, aspirations, and daily visual requirements into account. The choice of IOL can profoundly affect the recipient’s life. Patient dissatisfaction may necessitate further intervention.
For these reasons, considerable time must be devoted to patient education before surgery. Postoperatively, the ocular surface may require refinement, patients may need time for neural adaptation, and additional refractive procedures may be necessary to optimize results.
The increasing complexity of IOL selection and an escalation in patients’ expectations led us to evaluate the workload presented by premium cataract surgery.
STUDY METHODOLOGY
Our open-label, multicenter, comparative study retrospectively analyzed the case records of cataract surgery patients who underwent the bilateral implantation of either a presbyopia-correcting IOL (n = 177) or a standard monofocal IOL (n = 177). Outcome measures included the total time patients spent in the office, the number and average duration of visits, and the number of procedures and diagnostic tests conducted during the first postoperative year. These outcome measures were further evaluated by comparing data from the first 90 and subsequent 275 days postoperatively. The goal was to gain insight into the additional care requirements often associated with premium cataract surgery that can extend beyond the typical 90-day postoperative global period.
THE EXTENDED CARE SPECTRUM
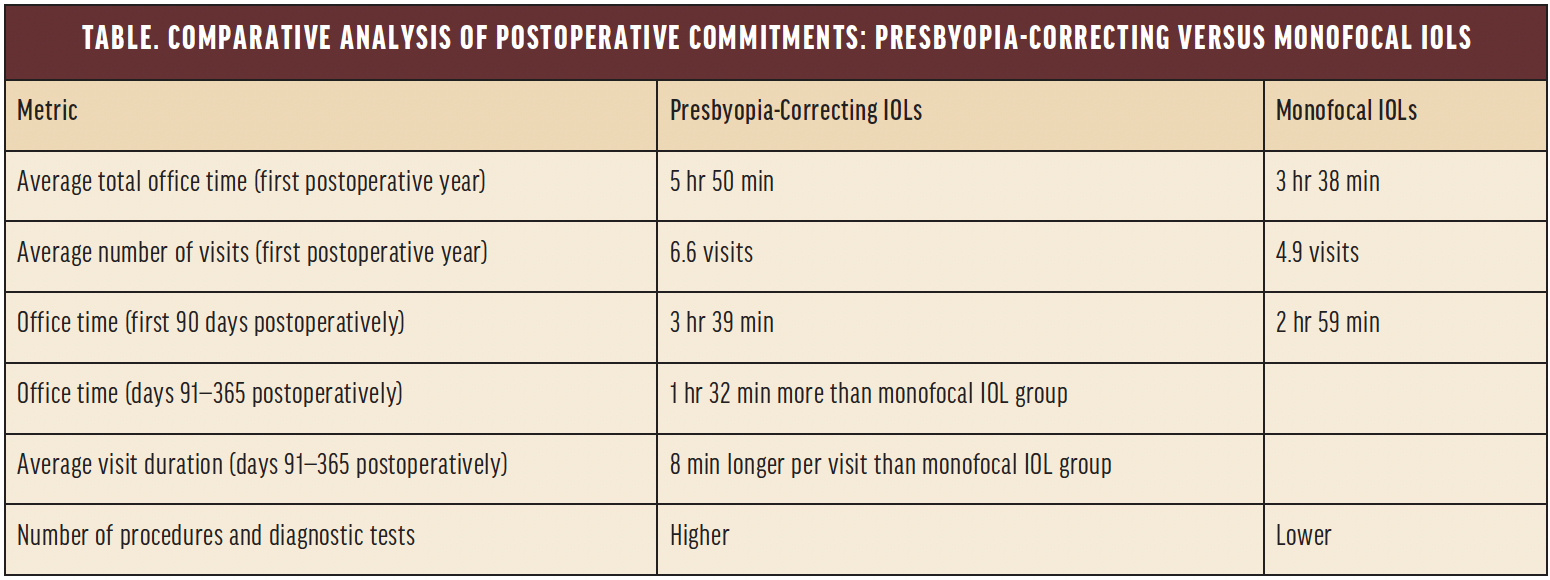
Postoperative care demands. During the first postoperative year, patients in the presbyopia-correcting IOL group spent an average of 5 hours and 50 minutes (±3 hours and 35 minutes) in a total of 6.6 ±2.9 visits compared to 3 hours and 38 minutes (±1 hour and 36 minutes) in 4.9 ±1.6 visits for the monofocal IOL group (P < .001; Table). In the initial 90-day period, the presbyopia-correcting IOL group required approximately 40 more minutes in the office than the monofocal IOL group (3:39 ±1:38 hours vs 2:59 ±1:13 hours; P < .001). From postoperative days 91 to 365, the amount of in-office time was 1 hour and 32 minutes longer for the presbyopia-correcting IOL group (P < .001), and the average visit duration was 8 minutes longer (P = .002) than for the monofocal IOL group. A greater number of procedures and diagnostic tests (P ≤ .001) were performed for the presbyopia-correcting IOL compared to the monofocal IOL group.
Pre- and intraoperative considerations. Whereas our study focused on the postoperative period, Oshika and colleagues explored the preoperative period.1 They found that patients slated for multifocal IOL implantation required 64 minutes of chair time during the preoperative cataract surgery consultation compared to 32 minutes for those receiving monofocal IOLs.
The implantation of presbyopia-correcting IOLs can involve extra intraoperative tasks, such as femtosecond laser treatment, precise centration of the IOL on the visual axis, alignment to the toric axis, and intraoperative aberrometry. Our analysis did not quantify the impact of pre- and intraoperative tasks on the workload associated with presbyopia-correcting IOLs.
Patient satisfaction and visual phenomena. Presbyopia-correcting IOLs often sacrifice quality of vision to some degree in order to extend the patient’s range of vision. Individuals who receive the lenses are at increased risk of experiencing visual phenomena such as glare, halos, and blurred vision.2-5
In a study of 74 eyes of 49 patients who reported dissatisfaction after multifocal IOL implantation at the Bascom Palmer Eye Institute,4 the predominant issues leading to a consultation were ocular surface disease and residual refractive errors. Addressing these issues often demands additional postoperative visits and time. Residual refractive errors can reduce visual quality and increase the incidence of visual phenomena, including glare and halos. Additional procedures such as corneal refractive surgery or an IOL exchange may be required.
IMPLICATIONS FOR PRACTICE
Our study supports the hypothesis that patients receiving presbyopia-correcting IOLs require significantly more clinical time, diagnostic testing, and postoperative procedures than those who receive a standard monofocal IOL. Given these findings, we believe it is imperative that additional physician compensation for these extended services be considered.
1. Oshika T, Bissen-Miyajima H, Nonaka T. Comparison of preoperative chair time between monofocal and multifocal intraocular lenses. J Cataract Refract Surg. 2022;48(5):632-633.
2. Woodward MA, Randleman JB, Stulting RD. Dissatisfaction after multifocal intraocular lens implantation. J Cataract Refract Surg. 2009;35(6):992-997.
3. Abdelghany AA, Alio JL. Surgical options for correction of refractive error following cataract surgery. Eye Vis (Lond). 2014;1:2.
4. Gibbons A, Ali TK, Waren DP, Donaldson KE. Causes and correction of dissatisfaction after implantation of presbyopia-correcting intraocular lenses. Clin Ophthalmol. 2016;10:1965-1970.
5. Mamalis N. Complications of multifocal intraocular lenses: What have we learned? J Cataract Refract Surg. 2021;47(10):1256-1257.




