Improving UCVA in Toric IOL Patients
Measure accurately, and make sure the IOL stays where you put it.
Eric D. Donnenfeld, MD

The largest rate-limiting step for improving UCVA in patients undergoing refractive cataract surgery is the treatment of preexisting and surgically induced astigmatism. For this reason, toric IOLs offer an easy solution for surgeons who wish to improve outcomes in their refractive cataract surgery patients.
Based on the current literature, approximately 50% of cataract patients have 1.00 D or more of preexisting corneal astigmatism and could therefore benefit from a toric IOL.1 Toric IOLs have almost no contraindications. They can benefit patients with epiretinal membranes, glaucoma, macular degeneration, and other ocular pathologies. The only exceptions are that they are contraindicated in patients with irregular corneas in which the axis of cylinder cannot be determined and in patients who wear gas permeable or scleral contact lenses.
In our practice, we have developed several pearls for increasing the accuracy of improving UCVA in our toric IOL patients. These can be divided into two steps.
- Step No. 1: Measure correctly. Accurately and correctly measure the magnitude and axis of preoperative corneal cylinder.
- Step No. 2: Place correctly. Implant the IOL at the correct axis and then make as certain as possible that the IOL stays at the correct axis.
MEASURE CORRECTLY
Determining the correct magnitude and axis of the cylinder depends on using multiple sources of information. We perform automated keratometry, topography, and keratometry with the IOLMaster 700 (Carl Zeiss Meditec) or the Lenstar LS 900 (Haag-Streit). The magnitude is best managed by using the keratometry reading from the IOLMaster or Lenstar. The axis is best determined by looking at the topography and drawing a straight line through the bowtie (Figure 1) rather than using simulated keratometry.
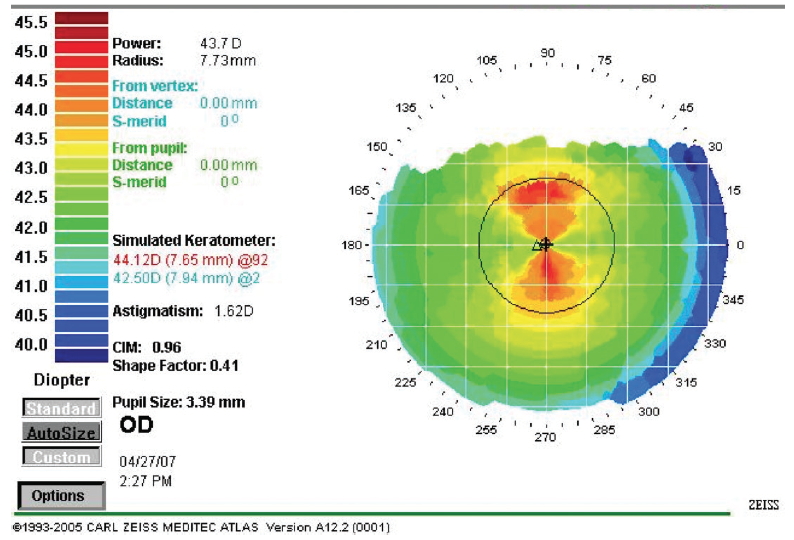
Figure 1. A straight line can be drawn through a topography image to determine the correct axis of cylinder for toric IOL implantation.
Additionally, estimating posterior keratometry can help to improve refractive results with the Barrett formula. And now that the IOLMaster 700 employs swept-source OCT and the Barrett Total K formula, we can provide a real-time measurement of the posterior corneal surface to further improve toric IOL outcomes.
PLACE CORRECTLY
Intraoperatively, I follow my basic cataract surgery technique. The placement of the toric IOL on the correct axis is of paramount importance. Preoperative marking should be done with the patient sitting up to avoid marking the wrong axis due to cyclotorsion.
When I am performing laser cataract surgery, I use the femtosecond laser to mark the cornea at the correct axis. A small intrastromal incision made with the laser serves to designate the toric axis. I have also used intraoperative aberrometry successfully for this purpose, but my go-to axis marker is an intraocular guidance system such as Callisto eye (Carl Zeiss Meditec; Figure 2) or the Verion Image Guided System (Alcon).
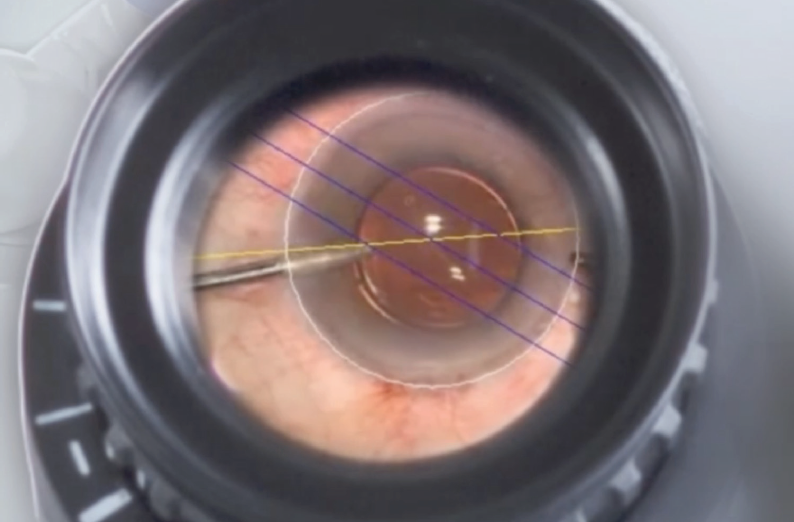
Figure 2. Graphical overlays generated by the Callisto system, seen here through the operating microscope, demonstrate the axis of astigmatism in this eye.
Courtesy of Eric D. Donnenfeld, MD
Several intraoperative pearls can be helpful in toric IOL surgery. One is not to vacuum the posterior surface of the anterior capsule; this allows better adhesion of the IOL to the capsular bag.
With the Tecnis Toric II IOL (Johnson & Johnson Vision), introduced late last year, I have found that the IOL stays exactly where it is placed. (Editors’ note: For more on the Tecnis Toric II and other new in IOL technologies available in the United States, see “Newcomers,” on pg 46). Therefore, I no longer place the IOL 15° clockwise from the intended axis, as I used to do, but rather leave it exactly at the correct axis before removing the OVD.
Another trick I have developed is that I press on the IOL with the angle of the I/A tip to hold the IOL in place while I remove the OVD, and then I tilt the IOL to place the I/A tip under the IOL to remove residual OVD from the capsular bag.
Finally, I leave the eye relatively soft, with IOP of around 10 to 20 mm Hg, to avoid expanding the capsular bag, and I ask patients to avoid eye rubbing and exercise for 1 week. These steps help to ensure that the IOL stays where I put it.
CONCLUSION
Toric IOLs are tremendously underutilized. They can be useful for almost any cataract patient with preexisting cylinder. The surgical pearls I have outlined here are simple and easily adopted. Toric IOLs can be of great benefit to many of our patients undergoing cataract surgery.
1. Anderson DF, Dhariwal M, Bouchet C, Keith MS. Global prevalence and economic and humanistic burden of astigmatism in cataract patients: a systematic literature review. Clin Ophthalmol. 2018;12:439-452.
Pre- and Intraoperative Planning Are Crucial
Prepare the corneal surface, and have a backup plan for axis alignment.
Detlef Holland, MD

In our daily routine, we are using an increasing number of multifocal and toric IOLs. This is a result of cataract surgery patients being better informed preoperatively regarding their options for receiving different types of IOLs. With toric IOLs, as with multifocal IOLs, it is important to have a good quality system in place for pre- and intraoperative care in order to achieve the best outcomes for our patients.
PREOPERATIVE
The preoperative process starts with the correct diagnostics performed by a well-educated staff. Sometimes, it can be challenging to acquire good biometry and topography measurements in patients with, for example, dry eye disease (DED) or small lid margins. In especially difficult cases, our optometrists focus on achieving reliable and comparable results. If the results of astigmatism and axis measurements are inconsistent, we always perform another measurement at a second appointment and recommend that the patient uses artificial tears in the meantime.
If DED or blepharitis is severe, we treat these conditions aggressively in order to improve the ocular surface and ensure accurate biometry results. We have experienced good results with the treatment of meibomian gland dysfunction using devices such as the Eye-Light (Topcon, not available in the United States) and Tixel (Swissmed, not available in the United States).
We always explain to patients that it is better to invest a little more time and treat the eyes in advance of surgery for better results, and patients generally understand this reasoning. If reliable diagnostic results are achieved, it is possible to plan the best treatment and select the best IOL.
We use toric designs for both monofocal and multifocal IOLs in eyes with 0.75 D of astigmatism or more. Further, we always select the highest toric amount that is recommended by biometry, even if a slight overcorrection of the astigmatism is predicted, because in our postoperative analysis we have seen no relevant overcorrections to date.
It is important to educate patients preoperatively that rotation or misalignment of the toric IOL is possible, which may necessitate a secondary intervention. The occurrence of rotation or misalignment is, however, rare.
INTRAOPERATIVE
We have not yet invested in a microscope-based axis alignment system, but we expect to do so soon. For now, we use the self-leveling RoboMarker (Surgilūm) for preoperative marking, which yields precise results.
When we perform laser cataract surgery, the IntelliAxis marking performed by the Lensar Laser System (Lensar), together with its integrated cyclotorsion compensation, offers the best way to perform toric IOL implantation in our hands (Figure 3). Still, in all my toric IOL laser cataract surgery patients, I perform an ink mark with the RoboMarker in addition to the IntelliAxis marking. This requires a little more time in the OR, but it means I always have a safe option for lens positioning if the cyclotorsion control of the IntelliAxis system does not work.

Figure 3. The IntelliAxis system creates axis marking within the laser capsulotomy.
Another advantage of the IntelliAxis marking is that it allows perfect postoperative assessment of the lens position in relation to the planned axis. If, at follow-up, the lens is no longer parallel to the marks in the capsulotomy, I know that a rotation has occurred postoperatively.
When manual capsulotomy is performed, achieving the perfect size is important. If the diameter is too large, without a good overlap of the capsule over the optic, this may lead to IOL rotation and poor postoperative results. In these cases, we always implant a capsular tension ring along with the IOL to increase the contact of the capsule with the IOL surface. We believe that, especially in myopic eyes, patients benefit from this because it reduces the ability of the lens to rotate.
The toric IOL model we use most often is a plate-haptic design, which has high rotational stability. Another good toric design is the Precizon toric (Ophtec). The lens’ transitional conic toric surface provides compensation for some degree of misalignment, leading to good results even if the lens is not perfectly aligned to the target axis (Figure 4).
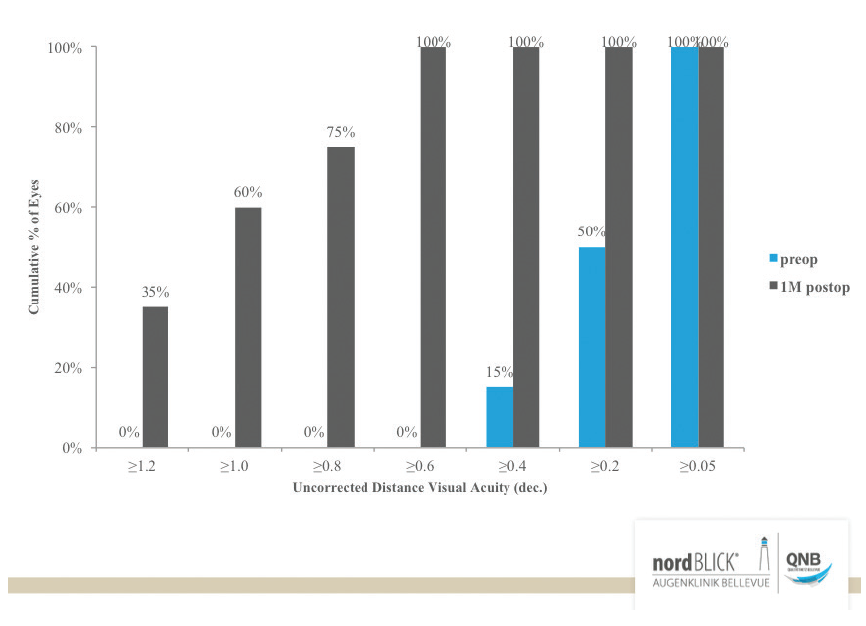
Figure 4. Results at 1 month postoperative with the Precizon toric IOL in 30 eyes.
Courtesy of Detlef Holland, MD
CONCLUSION
Using these strategies, we have seen good results in our toric patients and a small number of secondary interventions for IOL rotation.
How to Select the Best Lens and Nail the Refractive Goal
It’s all about optimizing the ocular surface preoperatively, properly positioning the toric IOL intraoperatively, and knowing how to manage residual astigmatism postoperatively.
Kourtney Houser, MD

The correction of even low levels of astigmatism at the time of cataract surgery can provide patients with improved image quality and overall satisfaction with their postoperative vision. In modern cataract surgery, toric IOLs have great potential to help surgeons grow their refractive cataract surgery practice.
In this article, I outline some of the factors I take into consideration specifically for patients who are interested in astigmatism correction at the time of cataract surgery with a toric IOL.
OPTIMIZE AND TREAT THE SURFACE
Achieving great outcomes for patients undergoing cataract or lens-based refractive surgery, no matter what type of IOL is to be used, begins with optimizing the ocular surface. Common surface abnormalities include dry eye with a poor tear film, corneal erosions, anterior basement membrane dystrophy, and Salzmann nodules. These conditions, if present, often require treatment before reliable biometry and topography can be obtained.
Left untreated, ocular surface abnormalities create irregular astigmatism and can artifactually increase or decrease the true amount of corneal astigmatism. This is of particular concern in patients who are candidates for toric IOLs. Any patient with dry eye causing corneal erosions centrally should be treated aggressively before proceeding with surgery. This can be accomplished with a combination of pulse-dosed steroid drops to speed improvement, artificial tears, topical immunomodulatory therapy, and meibomian gland treatment, if indicated.
Similarly, anterior basement membrane dystrophy or Salzmann nodules located in the central 3 mm of the cornea and causing irregular astigmatism in this area can mask underlying astigmatism, exaggerate its magnitude, or skew the axis of the underlying cornea. These corneal irregularities can be easily removed with superficial keratectomy, and then more representative biometry and topography can be obtained after 4 to 6 weeks to allow ocular surface stabilization.
NAILING THE CALCULATION
Once accurate biometry and topography are obtained, I evaluate the magnitude and axis of astigmatism, also considering the patient’s habitual and manifest refraction. I always take posterior corneal astigmatism into consideration in my lens selection; this is imperative to ensure accurate treatment of total corneal astigmatism. Accounting for posterior corneal astigmatism is simpler now than it used to be. Modern online calculators such as the Barrett Toric Calculator and the Alcon Online Toric IOL Calculator now incorporate posterior corneal astigmatism, as do nomograms such as the Baylor Toric IOL Nomogram, which is my preferred guide.
New technologies such as the femtosecond laser, intraoperative aberrometry, and microscope-integrated alignment tools have made intraoperative toric IOL positioning much easier than before. Many of these options eliminate the need for preoperative marking. Depending on what technology is available in your surgery center or clinic, however, manual marking may still be necessary. Accurate, predictable results can be obtained with manual marking.
CONSIDERATIONS FOR SURGERY
I prefer to manually mark the limbus at the 3 and 9 clock positions with the patient upright. I find that femtosecond laser–assisted surgery is often helpful to ensure a perfectly centered and round capsulotomy. Additionally, orientation marks can be placed with the laser to assist in intraoperative alignment. I use the LenSx Laser (Alcon) to place small intrastromal alignment marks on the axis of my desired toric alignment to aid in intraoperative positioning of the IOL.
Otherwise, I perform cataract surgery as I routinely do, ensuring that I thoroughly polish the anterior and posterior capsules after cortical removal. For eyes with long axial lengths (> 26 mm), I also place a capsular tension ring before IOL implantation to minimize postoperative rotation.
I use bimanual irrigation and aspiration to thoroughly remove the OVD from the anterior chamber, including from behind the lens. I then use a Sinskey hook with the irrigation infusion handpiece to rotate the lens to the desired axis (Figure 5). After removing the Sinskey hook but before removing the irrigation handpiece from the eye, I hydrate the second paracentesis (Figure 6). This helps to prevent chamber collapse and rotation of the IOL after the infusion is removed.
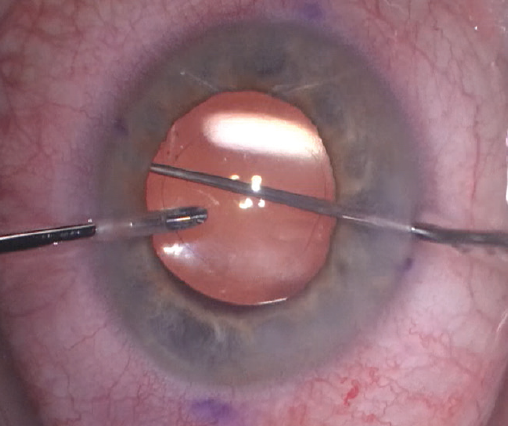
Figure 5. The irrigation handpiece and the Sinskey hook are used at the haptic-optic junction to rotate the toric IOL.
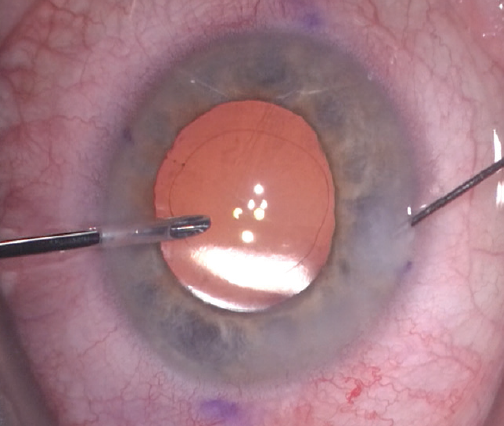
Figure 6. The second paracentesis wound is hydrated before the irrigation handpiece is removed from the eye.
Courtesy of Kourtney Houser, MD
I prefer to leave the eye slightly more firm than I do in standard cases, and I instruct patients to minimize their activities and avoid significant movement for the first 24 hours after surgery in an attempt to minimize postoperative IOL rotation.
POSTOPERATIVE MANAGEMENT
Equally important as proper selection and positioning of the toric IOL is knowing how to manage postoperative residual astigmatism. The Toric Results Analyzer, developed by John P. Berdahl, MD, and David R. Hardten, MD, is an essential tool to determine whether IOL rotation would sufficiently correct the error—and, if so, how much rotation is needed—or whether IOL exchange or a corneal refractive procedure would be superior.
CONCLUSION
For patients who are interested in astigmatism correction at the time of cataract surgery, the best strategy in my hands is a toric IOL. Optimizing the ocular surface, considering patients’ habitual and manifest refraction and posterior corneal astigmatism when making the lens selection, taking extra steps in surgery to help prevent rotation of the IOL, and instructing patients to minimize their activities on the day after surgery all go a long way in achieving successful outcomes with toric IOLs.
Mastering Toric IOLs
The four things that have helped me the most.
Stephen V. Scoper, MD

Successfully incorporating toric IOLs into your refractive cataract surgery practice takes patience, but it is achievable for those surgeons willing to take time to learn the nuances of these lenses. In my experience implanting thousands of toric IOLs, I have found the following four pearls to be the most helpful pieces of advice in achieving excellent outcomes.
Pearl No. 1: Hit your spherical equivalent. >There are two things you must accomplish when implanting a toric IOL: (1) eliminate the astigmatism and (2) hit the spherical equivalent. Therefore, the way I see it, before you can achieve good results with toric IOLs, you must be able to achieve good results with standard monofocal IOLs. This includes routinely hitting the best spherical equivalent and consistently achieving the target refraction to within ±0.50 D. The same is true for toric IOLs. You can select the toric lens power properly and implant the lens beautifully, but if you do not hit your spherical equivalent, the patient will be unhappy postoperatively.
Pearl No. 2: Get an accurate measurement of corneal astigmatism. >The measurement of corneal astigmatism is one of the most important elements involved in calculating the power of the toric IOL. Rather than simply relying on just one keratometer to measure corneal power, I like to use at least two methods of astigmatism measurement. For instance, I use the Lenstar (Haag-Streit) for keratometry (K) readings and, in addition, the Cassini (Cassini Technologies) and OPD-Scan (Nidek) for K readings and topography. When the K readings from all three devices are the same or very similar, it gives me confidence that I have an accurate measurement of corneal astigmatism.
Pearl No. 3: Have a good understanding of posterior corneal astigmatism. >Today’s topographers and keratometers generally measure the anterior surface of the cornea. But we now know that some astigmatism is also present on the posterior cornea. Therefore, in order to account for the total corneal astigmatism in our measurements, we must subtract or add the posterior corneal astigmatism to the anterior corneal astigmatism.
There are two ways to do that. The first way is by using modern lens formulas that include algorithms to calculate the posterior corneal astigmatism. A commonly used modern formula is the Barrett Toric Calculator.
The second way is by physically measuring the posterior cornea. Devices such as the Cassini and the Galilei (Ziemer Ophthalmic Systems) take separate measurements of the anterior and posterior corneal astigmatism and then algebraically add the two numbers together to calculate the total corneal astigmatism. When that objective measurement and the outcome from the Barrett Toric Calculator look about the same, I know I’ve nailed the astigmatism. Sometimes, the Cassini will show much more astigmatism than the Barrett Toric Calculator, however. In those cases, I usually go with the Cassini.
Pearl No. 4: Place the toric lens in the appropriate axis. >There are several ways to accomplish correct positioning of toric IOLs. I prefer to use the Lensar Laser System to create finger-like tabs on the axis of the plus cylinder. Retroillumination photography there shows me exactly where to place the toric IOL, and the iris registration corrects for head tilt or cyclorotation. Postoperatively, at the slit lamp, I can see if the toric lens is still aligned with the tabs or if it has rotated out of position. This is especially useful in cases in which residual astigmatism is present.
Other automated systems for toric IOL placement include the Verion Image Guided System and Callisto eye. Of course, standard ink marks placed on the cornea can also be used to guide toric IOL placement.
CONCLUSION
Obtaining good results with toric IOLs starts with mastering outcomes with standard monofocal IOLs, including hitting the spherical equivalent and consistently achieving the intended refraction to within ±0.50 D. Once this is achieved, and by following the four tips outlined in my contribution as well as the tips outlined in the contributions from the other authors, most surgeons can enjoy success with toric IOL technologies.




