
Cataract surgery lowers IOP in patients with angle-closure glaucoma (ACG) at every phase of the disease—after an acute attack, in chronic angle closure, when ACG is stable or unstable, and even in eyes with clear lenses.1-7 Because of the growing body of evidence supporting these findings, cataract surgery has gained widespread acceptance as a valuable intervention for ACG.
ANATOMIC CONSIDERATIONS
The anatomy of eyes with angle closure supports a therapeutic role for lens removal. Angle closure occurs in shorter eyes with shallower anterior chambers. The increasing thickness of the aging lens may also contribute to a progressive narrowing of the angle. Although laser iridotomy widens the anterior chamber angle, some iridotrabecular contact persists in most patients, and angle closure may progress despite a patent iridectomy. Performing cataract surgery may anatomically improve angle closure more profoundly than an iridotomy, because removing the lens mass causes a greater deepening of the chamber and opening of the angle, which could reduce—or even eliminate—the risk of blindness, both from an acute attack as well as a chronic increase in IOP.
CATARACT SURGERY: ALONE AND in combination
Cataract surgery has been found to be a more effective treatment for an attack of acute primary angle closure (APAC) than laser iridotomy.1 Lam et al randomized patients with APAC to either early phacoemulsification or laser iridotomy after the attack was successfully treated with medications. Compared with the eyes that underwent iridotomy, those treated with phacoemulsification experienced dramatically fewer IOP elevations, had lower mean IOPs, required fewer medications, and had deeper angles following lens removal (Figures 1 and 2). The authors concluded that, in APAC eyes presenting with an IOP greater than 55 mm Hg, phacoemulsification was a “definitive treatment” for preventing subsequent IOP elevations.1
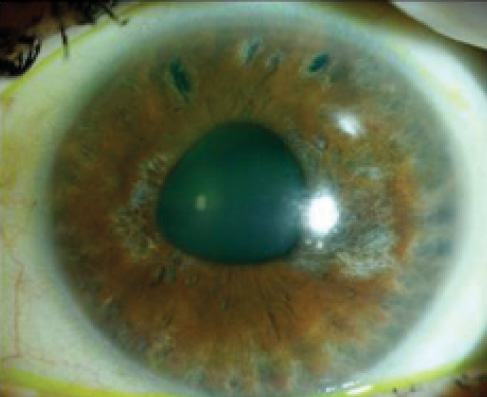
Figure 1. After an attack of ACG, there is a cataract and an irregular pupil.
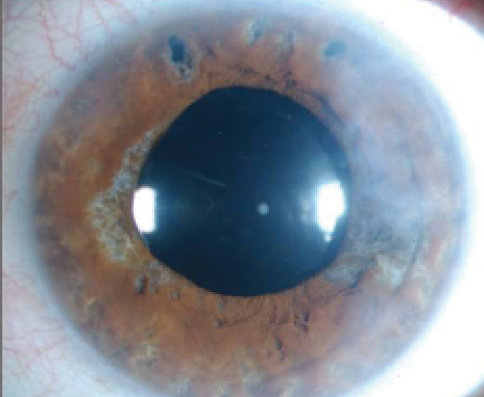
Figure 2. After cataract surgery on the same eye, the visual axis is clear, but the iris atrophy cannot be reversed.
Cataract surgery alone has also been compared to combined phacotrabeculectomy for treating chronic ACG in eyes with IOPs that were both controlled and uncontrolled.2,3 Phacoemulsification alone reduced IOP in both groups as well as the number of medications required for pressure control. In the medically uncontrolled eyes, the IOP was reduced by nearly 8 mm Hg with phacoemulsification alone, and the effect lasted for the 2 years of the study.3 Control of the glaucoma as defined in the study was achieved in more than 90% of patients in both treatment groups.
The phacotrabeculectomy group had a higher complication rate than for cataract surgery alone. Two patients lost central visual acuity despite adequate IOP control (“snuff out”), and two others lost vision from progressive optic atrophy. The authors concluded that phacoemulsification alone is a “viable surgical alternative” to combined phacotrabeculectomy whether or not the IOP before surgery is controlled.3 Although adding the trabeculectomy achieved a slightly lower IOP, the investigators preferred phacoemulsification alone because of the decreased complication rate.
These studies found that 14.8% of patients with uncontrolled IOP and 2.9% of patients with controlled IOP eventually required a trabeculectomy.
Clear Lens Extraction
The argument favoring cataract surgery as a treatment for ACG may be applied to clear lens extraction (CLE).5 If the anterior segment anatomy is the problem, removing a clear lens should have the same positive effects as removing a cloudy lens. The success of lens removal alone in angle closure may depend on the extent of permanent or appositional angle closure and the potential for reversibility. The angle’s appearance may not correlate with the severity of the glaucoma or the potential for reversibility. Therefore, predicting which ACG patients will benefit from lens removal—whether clear or cataractous—remains uncertain.
CLE is highly controversial. My colleagues and I recently published a series of three cases demonstrating the value of CLE as an alternative to a trabeculectomy.7 Two patients underwent cataract surgery alone, and one-third underwent combined lens removal and goniosynechialysis (GSL). All three patients experienced a marked improvement in IOP and were able to avoid undergoing a trabeculectomy and its serious risks. Two patients had been treated with four medications—and still had unacceptable IOPs—but were able to discontinue all medications after the surgery.
GSL can be combined with CLE and may help reduce the IOP,8 but there are no controlled studies proving that GSL improves the reduction in IOP over cataract surgery alone. It is impossible to know whether the GSL helped this patient.
CONCLUSION
Ophthalmologists’ appreciation of the value of cataract surgery in patients with ACG has grown recently. In the past, recommending cataract surgery alone to an angle-closure patient with uncontrolled IOP—even in the presence of a visually significant lens opacity—would have been controversial. Today, avoiding a trabeculectomy in these patients is an accepted practice. The current debate is over what to do for patients with uncontrolled IOP and nearly clear lenses and also what degree of angle closure is necessary for lens removal to have a therapeutic effect. That said, lens extraction alone should be recommended for any angle-closure patient with a visually significant cataract and should be seriously considered as an alternative to filtering surgery in patients with uncontrolled IOP.
1. Lam DS, Leung DY, Leung DY, et al. Randomized trial of early phacoemulsification versus peripheral iridotomy to prevent intraocular pressure rise after acute primary angle closure. Ophthalmology. 2008;115:1134-1140.
2. Tham CC, Kwon YY, Leung DY, et al. Chronic angle-closure glaucoma with cataract. Ophthalmology. 2008;115:2167-2173.
3. Tham CC, Kwong YY, Leung DY, et al. Phacoemulsification versus combined phacotrabeculectomy in medically uncontrolled chronic angle closure glaucoma with cataracts. Ophthalmology. 2009;116:725-731.
4. Tham CC, Kwong YY, Baig N, et al. Phacoemulsification versus trabeculectomy in medically uncontrolled chronic angle-closure glaucoma without cataract. Ophthalmology. 2013;120:62-67.
5. Brown RH, Zhong L, Lynch MG. Lens-based glaucoma surgery: using cataract surgery to reduce intraocular pressure. J Cataract Refract Surg. 2014; 40:1255-1262.
6. Brown RH, Zhong L, Whitman AL, et al. Reduced intraocular pressure after cataract surgery in patients with narrow angles and chronic angle-closure glaucoma. J Cataract Refract Surg. 2014;40:1610–1614.
7. Brown RH, Zhong L, Lynch MG. Clear lens extraction as treatment for uncontrolled primary angle-closure glaucoma. J Cataract Refract Surg. 2014;40:840-841.
8. Harasymowycz PJ, Papamatheakis DG, Ahmed I, et al. Phacoemulsification and goniosynechialysis in the management of unresponsive primary angle closure. J Glaucoma. 2005;14:186-189.
Reay H. Brown, MD
• in practice with Atlanta Ophthalmology Associates in Atlanta
• (404) 237-4368; reaymary@comcast.net
• financial interest: none acknowledged


