Ophthalmologists and optometrists rely on their own training and skill to help patients achieve their best visual function. They rely on administrators to develop practice structure and provide staff direction. And they rely on ophthalmic technicians to do just about everything else. A help-wanted ad on the job search engine Indeed for an experienced ophthalmic technician described the role this way:
Provides a variety of preliminary ocular assessment activities including obtaining a complete and accurate medical history; visual acuity and stereo testing; lensometry; motility; applanation tonometry; diagnostic testing including but not limited to visual field, OCT, topography, fluorescein angiography/fundus photos; and pupillary assessment. Increasingly complex patient procedures may also be assigned as determined by level of proficiency and experience.
Responsibilities of the ophthalmic technician will undoubtedly differ depending on practice size and specialty and on the level of experience of the technician; however, the commonality is that technicians act as care extenders—allowing eye care providers to focus specifically on the tasks defined by their scope of practice. The result, when executed effectively, is increased efficiency for the entire practice.
GREATER VERSATILITY
“Physicians can become a limiting factor for a practice in terms of how many patients they can see and the amount of patients to whom we can provide health care,” said Arsen Grigoryan, MBA, Director of Operations for Harvard Eye Associates in Orange County, California. “Our team of 30 ophthalmic assistants, comprising technicians and scribes, is utilized to prevent this from happening. We categorize technicians and scribes as ophthalmic assistants because it allows us greater versatility; they can be cross-trained and help out across the clinic.”

Figure 1. Harvard Eye Associates staff of ophthalmic technicians, led by Arsen Grigoryan, MBA (front row, second from right).
At Harvard Eye Associates (Figure 1), a large multispecialty practice with 10 ophthalmologists and three optometrists, workup technicians are primarily responsible for gathering preliminary information from patients, such as chief complaint, history, and review of systems. They also conduct tests including preliminary manifest refraction and IOP checks. If the patient needs additional testing, he or she is taken to a diagnostic area that is staffed by a dedicated diagnostic technician.
“This is where we have put additional efficiencies into place,” Mr. Grigoryan explained. “The workup technician can hand the patient off to the diagnostic technician and return to another patient, rather than creating a bottleneck waiting for a particular machine to be available.” (Editor's note: For more on avoiding patient bottlenecks and improving patient flow, see Improving Patient Flow, by David I. Geffen, OD, FAAO.)
Once the patient is in the exam room, a scribe further streamlines the process for the physician. “We want our doctors interfacing with the patient as much as possible,” Mr. Grigoryan said. “While the scribe keys in the findings, the doctor is able to maintain eye contact and provide premium treatment, and the patients are made to feel comfortable because they know they have the doctor's full attention.”
At Harvard Eye, two workup technicians and one scribe are usually assigned to each ophthalmologist and one workup technician and one scribe to each optometrist. “When deciding how many technicians we need, patient volume is one factor, but we also look at the type of workup that needs to be conducted,” Mr. Grigoryan said. “For instance, when working with an ophthalmologist, ophthalmic assistants typically conduct preliminary manifest refractions, dilate pupils, and check pressures, and we recognize that each of those tests takes up additional time.”
Newly hired ophthalmic technicians often have no more education than a high school diploma, but they are immersed in on-the-job training and encouraged to become certified. “We take pride in providing a robust training system for our staff,” Mr. Grigoryan said. “We also encourage our staff to get their certified ophthalmic assistant [COA] certification. And, whether or not they have their COA, we require them to have an ophthalmic scribe certification before we allow them to input anything into the electronic health record.”
When he or she is hired with no prior experience, he explained, they undergo 2 months of intensive in-house training. “Our most senior and seasoned ophthalmic assistant is responsible for teaching the new hire. They start off with a literature portion learning about what ophthalmology is, then move on to anatomy, and that is followed by pathology lessons. After that, they graduate to the technical aspects of the job, and then we work on making sure they are interfacing with the patients in a way that reflects well on us,” he said.
MORE FACE TIME
Patti Barkey, COE, OCS, a certified ophthalmic executive, ophthalmic coding specialist, and the CEO of Bowden Eye & Associates in Jacksonville, Florida, is an example of a professional who started out as an ophthalmic assistant and then gained experience and earned certifications while working at just about every job available in an ophthalmic practice. Today, she applies that background as Director of Operations for a flourishing practice that employs about 30 ophthalmic technicians (Figure 2).

Figure 2. The Bowden Eye & Associates technicians enjoy a team-building exercise.
“Our best technicians are those who have already been scribes, and our goal is to have them all cross-trained,” Ms. Barkey said. At Bowden Eye, in addition to transcribing the doctor’s findings into the electronic health record, the scribe also “fills the room, opens the records, presents the patient to the doctor, and then facilitates the visit, so the doctor can move on quicker,” she explained. “They can also facilitate the medication lists for the patient and give patients instructions after the doctor leaves the room, but the main function of the scribe is to give the physician more face time with the patient.”
Technicians at Bowden Eye are also responsible for anticipating the physician’s needs and doing everything they can to ensure that the doctor has all of the diagnostics at hand to enable him or her to diagnose and determine treatment for the patient. “In our practice, the primary goal of the lead technician and the technicians on that team is to do everything possible to make each patient experience a smooth transition to the physician,” Ms. Barkey said, adding that some physicians prefer to control the entire patient experience and others give their technicians the agency to prepare and educate the patient.
“The most productive practices are those where the physicians lean on technicians as extenders,” she said. “I drive this point home by reminding our physicians that they should only do what is required of them in the scope of their license. For instance, if the physician’s license does not require him or her to do refractions, then someone else needs to do that for them. If we want to create flow and efficiency—which is a must in today's marketplace—we need to empower and trust our technicians and scribes and counselors to enhance that patient experience.”
SURGICAL DUTIES, TOO
The role of the tech can be different—and possibly even more rigorous—at a practice dedicated solely to LASIK, according to Ann Speer, Practice Administrator at Coleman Vision, a solo practice headed by Stephen C. Coleman, MD, in Albuquerque, New Mexico (Figure 3). “Because we only do LASIK, our techs have a huge role,” she said. “They not only take the patients’ measurements and perform topography and refract the patients, they also prepare them for surgery and educate them on what is going to happen during the surgery. Our techs also call the patient after surgery and then again a week later to check on them,” she said. “They really build a rapport with our patients, which makes Dr. Coleman’s life easier.”

Figure 3. Coleman Vision ophthalmic techs and Practice Administrator Ann Speer (second from right) enjoy a Kentucky Derby–themed event during a New Mexico Optometric Association meeting.
The techs at Coleman Vision have an effective and discreet way of conveying helpful information about patients to Dr. Coleman. “If the patient is apprehensive about the surgery or may be a bit difficult to deal with, or if there is anything that is slightly off the grid, the techs prepare him before he sees the patient,” she said. “If you have a good team of techs who respect the doctor, your practice runs so much smoother.”
Most practices have a mix of techs at various levels of experience; some are certified, others not. “It’s great if a new tech coming on board is certified and has extensive experience, but honestly we prefer to train our techs for customer service and patient care, and then they learn as they go.” Ms. Speer said. “The bottom line is that I would rather hire a person who is kind, hardworking, and able to present a professional manner rather than someone who is trained and knows the numbers. They can learn the technical things on the job, but the other stuff—they either have it or they don’t.”
SURGICAL SCHEDULING AND MORE
At Horizon Eye Care in Southern New Jersey, about 20 technicians are paired with nine physicians across six locations (Figure 4). Practice Administrator Suzanne D. Bruno, MBA, said the role of the technician at her practice varies according to physician preferences, but generally techs provide preoperative instructions, educate patients about IOL options, perform biometry with the »IOLMaster (Carl Zeiss Meditec), and field questions pre- and postoperatively.

Figure 4. Two Horizon Eye Care techs flank optometrist Sara Shkalim, OD.
A key responsibility of Horizon’s techs is ensuring that surgery days are efficiently booked. “The techs do not handle general appointment scheduling, but they do handle surgery scheduling. Our techs make sure that the physicians’ blocked surgery time is fully booked, which is really important as far as efficiency goes,” Ms. Bruno said. “Other responsibilities are physician-dependent. For instance, some techs are asked to make sure that whatever testing is required by the physician is done and interpreted and available to the physician, so that when he or she gets to the operating room there are no loose ends and no surprises.”
Another major role of the technician at Horizon is medication management. “We get thousands of phone calls from representatives at pharmacies and prescription management companies such as CareMark, saying the patient isn’t covered for this or that, and asking if something else can be prescribed. Our techs handle resolution of those inquiries, with physician input. Drug management is a huge part of their job.”
That duty is handled by administrative or back-office personnel in some practices, Ms. Bruno said, but relegating drug management calls to the technician support team is more efficient. “In our experience, the techs understand drug interaction much more than somebody in an administrative area would, so the issue gets resolved more quickly and completely for the patient.”
NUMBERS BASED ON VOLUME
At Horizon, techs are teamed with physicians based on patient volume. If the physician has 25 patients on his or her schedule, one tech is assigned. Those with 25 to 45 patients booked get a second, and those with 45 to 50 patients get a third. If the physician is a surgeon, four techs are on his or her team, and yet more for a retina surgeon. The best technicians can handle volume with ease, Ms. Bruno said, and at Horizon they are compensated better than general medical technicians.
Of the 20 techs on staff there, about 15 have been there for 5 or more years, she said; however, this is not typical. Some administrators interviewed for this article said a high rate of tech turnover is a widespread problem (see Slowing Down the Tech Turnstile). In some cases, techs leave to pursue professional careers, in others competitors target senior level techs and lure them away with better pay or perks, and in still other cases, according to Ms. Bruno, the best technicians are wooed by ophthalmic industry vendors.
Slowing Down the Tech Turnstile
A high rate of turnover among ophthalmic technicians is not universal, but it is a widespread phenomenon. Ophthalmic administrators cite rapid turnover as a source of inefficiency and revenue loss. According to the job search engine Indeed, the typical tenure for an ophthalmic technician at a practice is 1 to 3 years. Ophthalmic administrators interviewed for this article said causes for the tech turnstile effect include inadequate remuneration, inconsistent work schedules, poaching of high-level techs by practice competitors and industry vendors, and burnout.
The administrators quoted in the main article shared the following tips for tech staff retention:
- Be generous with time off. Ophthalmic technicians who work for several different physicians must work the same hours as those physicians, and often that means a different set of hours daily. The inconsistency makes having a life outside of work challenging. Recognizing that techs have family responsibilities, hobbies, and other obligations is important. Be generous in granting time off for their children’s school events or sports activities and allow them the time they request to participate in a nonwork-related passion. This flexibility pays the practice back in better work performance and greater loyalty.
- Pay for ophthalmic technicians to become certified. Ophthalmic technicians are exposed to a wealth of information and experience that typically eludes those who do not pursue higher education. As they expand their horizons on the job, they gain confidence and consider moving on to bigger and better things. Pay for them to become certified; compensate them for attendance at medical meetings that will fortify their knowledge base and make them even more valuable to the practice.
- Understand that your competitors, and even your ophthalmic industry vendors, are sizing up your techs for possible employment. Make sure the practice environment is one where they want to be, not one they want to escape. Encourage participation in staff social outings; surprise them with rewards such as gift cards for local eateries or coffee shops. If you don’t, your competitors will be happy to.
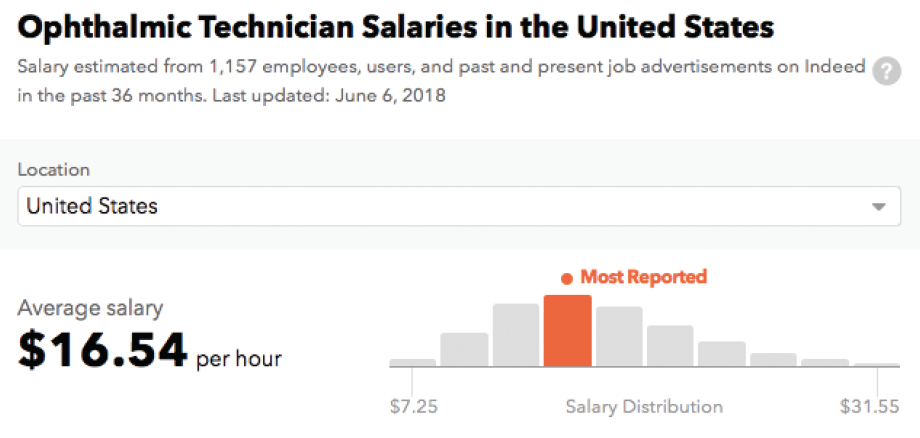
Figure. A salary survey indicated that US ophthalmic technicians earn an average annual income of $33,000.
(Source: Indeed)
- Pay good ophthalmic technicians appropriately for the work they do. According to Indeed, the average salary for an ophthalmic technician in the United States is $16.54 per hour. That totals about $33,000 annually (Figure). This figure is based on 1,157 salaries submitted anonymously by ophthalmic technician employees and users and collected from job advertisements on Indeed throughout a 3-year period. Without these care extenders, the number of patients a physician can bill for in a typical day decreases dramatically. The best technicians have initiative and drive and consider this their career; they should be compensated as career-level professionals, not worker bees.
“It’s a highly technical job, and, after they realize that they are capable of doing these highly skilled activities, such as performing OCTs, using the IOLMaster, and performing visual fields, they often develop an interest in medicine and science, and a lot of them move on to additional training, such as going to nursing school. Some of our techs have even moved on to go to optometry school,” Ms. Bruno said.
TRUST THE PROCESS
“Physicians need to trust management and the training process,” Ms. Barkey said. “Techs leave, new techs need to be trained, and techs need to be rotated so they can be cross-trained. Physicians need to appreciate the big picture: We want every employee to have a foundation of general knowledge throughout the practice. Just like physicians have a standard of care, all care extenders must have a shared standard of knowledge for the practice to operate efficiently.”




