
Cataract surgery in children differs in many ways from cataract surgery in adults. Pediatric eyes are growing and often have congenital anatomic abnormalities such as persistent fetal vasculature or dense posterior capsular plaque associated with vitreolenticular interface abnormalities.
Posterior optic capture for pediatric cataract surgery has a considerable history, reaching back to the 1990s. Recently there has been renewed interest in the use of posterior optic capture in patients aged 7 months to 7 years because the technique may allow surgeons to forgo the planned anterior vitrectomy that is currently commonly performed at the time of IOL implantation.
RENEWED INTEREST
In 2017, Vasavada and colleagues published the 1-year results of a single-center prospective randomized controlled clinical trial comparing in-the-bag IOL implantation, posterior capsulotomy, and anterior vitrectomy to posterior optic capture of the IOL in a posterior continuous curvilinear capsulorhexis (PCCC) without vitrectomy.1 The study included 61 children, and cataract surgery was performed at an average age of 16 months.
Both groups did well, with only one eye undergoing a reoperation for a secondary membrane. In five eyes in the optic capture group (16%), optic capture was attempted but could not be achieved. The investigators demonstrated that, in this cohort of children aged 4 to 41 months, it was possible to achieve a clear visual axis without anterior vitrectomy when the optic of a three-piece IOL was captured through a properly sized PCCC.
A LONG HISTORY
In the mid-1990s, Gimbel was the first to champion posterior optic capture with posterior capsulorhexis as a way to prevent opacification of the visual axis in children without having to resort to anterior vitrectomy.2 Shortly thereafter, others studied the technique and concluded that posterior optic capture failed to prevent visual axis opacification (VAO) in young children unless it was combined with anterior vitrectomy.3 One frequently cited study, in fact, concluded that posterior optic capture in children increased inflammatory sequelae.4
These early studies were conducted using rigid PMMA IOLs. In the current era of acrylic IOLs, optic capture in children is mostly used in combination with anterior vitrectomy as a way to stabilize and center an IOL that needs to be placed in the sulcus. The optic is captured through both anterior and posterior capsulorhexes.
BAG-IN-THE-LENS
Tassignon and colleagues developed the bag-in-the-lens concept in the early years of this century.5 Their IOL design uses the principles of optic capture. The Bag-in-the-Lens IOL (Morcher; not FDA approved) has been used in children with great success. It requires creation of a precise anterior capsulorhexis and matching PCCC. The combined anterior and posterior capsular remnants are placed between the flanges of the IOL.
A recent publication by Van Looveren et al reported results with the lens in 64 pediatric cataract cases, in which all but one IOL were successfully implanted.6 In 35 of the 64 eyes, anterior vitreolenticular interface dysgenesis made the PCCC especially challenging and resulted in detectable breaks in the anterior hyaloid membrane. The investigators concluded that, when children have evidence of persistent fetal vasculature or posterior capsular plaque, an anterior vitrectomy may be needed; in most cases, however, the bag-in-the-lens technique allows the anterior and posterior capsular edges to fuse, preventing VAO even in young children and even when planned anterior vitrectomy is not performed.
PEDIATRIC CATARACT SURGERY IS DIFFERENT
Many aspects of pediatric posterior capsule management are different from the technique in adult cataract surgery. There is rapid opacification, fibrosis, and thickening of the posterior capsule in young children after cataract surgery when the posterior capsule is left intact. For that reason, primary posterior capsulectomy and planned anterior vitrectomy are commonly performed in children who are not old enough to sit still for an Nd:YAG laser capsulotomy.
Posterior capsulotomy and vitrectomy in children are often performed through the pars plana after the IOL is placed in the bag and all OVD has been removed. Alternatively, the anterior approach also works well. Although planned anterior vitrectomy in children is incredibly safe, and retinal detachment and cystoid macular edema are rarely seen in these children, avoiding vitrectomy has some appeal, especially if recurrent VAO can still be avoided.
There are also reasons to want to avoid laser capsulotomy in pediatric eyes. Because the vitreous in children has not yet undergone liquefaction, debris from a laser capsulotomy can remain suspended in the vitreous and block the visual axis. In addition, larger amounts of laser energy are often needed when performing Nd:YAG laser capsulotomy in children. As a result, pediatric surgeons today are more commonly performing manual primary PCCC without vitrectomy, even in patients in the second decade of life and into early adulthood. In these older children, the visual axis remains clear after PCCC without posterior optic capture, so it is unclear whether optic capture would add significantly to the effectiveness of the surgery in the second decade of life.
CONCLUSION
When cataract surgery is performed in the first 7 months of life, studies have shown a clear benefit to leaving the infant aphakic and performing planned anterior vitrectomy. Secondary IOL placement is often done at age 4 to 7 years, at which time the IOL can often be placed in the capsular bag. For cataract surgery from age 7 months to 7 years, an IOL is usually placed in the capsular bag primarily, in combination with posterior capsulectomy and anterior vitrectomy. In children older than 7 years, primary PCCC without vitrectomy works well, even without posterior optic capture, and VAO is very rare.
Beyond the uses described herein, there are exciting possibilities for utilizing optic capture for children in the future. For infants in whom IOL implantation is necessary, primarily because of the unavailability of contact lenses or aphakic glasses, a three-piece IOL placed in the sulcus and captured through both anterior and posterior capsulectomies can allow the capsules to fuse in a way similar to when the infant is left aphakic (Figure). This would reduce the incidence of cortical reproliferation reaching the visual axis, which is the most common indication for reoperation when an IOL is implanted in the first 6 months of a patient’s life. Anterior vitrectomy may still be needed in these children because persistent fetal vasculature and capsular plaques occur in nearly all of them.
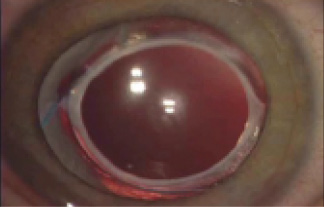
Figure. Appearance of the eye 4 years after IOL implantation. When the patient was 2 months old, a three-piece IOL was placed in the ciliary sulcus, with optic capture through both anterior and posterior capsulotomies. Anterior vitrectomy was performed at the time of surgery.
The posterior optic capture technique of Gimbel, as modified by Vasavada and others, is best utilized as a hyaloid-sparing technique in children aged 7 months to 7 years, in whom planned pars plana vitrectomy and posterior capsulectomy are commonly done now. We hope to gain access to the Bag-In-The-Lens IOL in the United States soon because this technology may also have unique applications in children after infancy.
Editor’s note: The use of IOLs in children is off-label.
1. Vasavada AR, Vasavada V, Shah SK, et al. Postoperative outcomes of intraocular lens implantation in the bag versus posterior optic capture in pediatric cataract surgery. J Cataract Refract Surg. 2017;43:1177-1183.
2. Gimbel HV. Posterior capsulorhexis with optic capture in pediatric cataract and intraocular lens surgery. Ophthalmology. 1996;103:1871-1875.
3. Koch DD, Kohnen T. Retrospective comparison of techniques to prevent secondary cataract formation after posterior chamber intraocular lens implantation in infants and children. J Cataract Refract Surg. 1997;23:657-663.
4. Vasavada AR, Trivedi RH. Role of optic capture in congenital cataract and intraocular lens surgery in children. J Cataract Refract Surg. 2000;26:824-831.
5. Tassignon MJ, De Groot V, Vrensen GF. Bag-in-the-lens implantation of intraocular lenses. J Cataract Refract Surg. 2002;28(7):1182-1188.
6. Looveren JV, Vael A, Ideler N, et al. Influence of the vitreolenticular interface in pediatric cataract surgery. J Cataract Refract Surg. 2018;44:1203-1210.




