CASE PRESENTATION
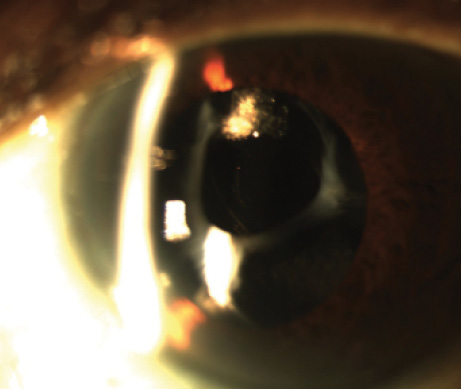
Figure. Superior-temporal decentration of a three-piece silicone IOL and anterior capsular phimosis.
—Case prepared by Audrey Talley Rostov, MD.

KENDALL DONALDSON, MD, MS
From the figure, it is difficult to assess the degree of decentration, the IOL’s stability and tilt, and the chronicity of the problem. It sounds as if the patient’s symptoms are acute, but from the figure, the condition looks relatively chronic. It would be nice to have a better image and to obtain old records that predate the onset of her symptoms to compare and correlate with the clinical appearance. This would better elucidate if the symptoms are associated with the anterior capsular phimosis, the IOL’s decentration, or both.
Anterior capsular phimosis is relatively straightforward to treat with an Nd:YAG laser by creating relaxing incisions in the anterior capsule or by using the laser to remove segments of the opacified anterior capsule, which may impinge on the line of sight or cause the lens to tilt.
If a decentered lens is found to be the culprit but the problem is mild, such that the optic is still fully covering the visual axis, the patient could be treated with an alteration in refraction. In more extreme cases associated with a significant shift of the entire bag-IOL apparatus, the complex can be used as a scaffold for resuturing. A three-piece IOL can be fixated in any of three ways, depending on the surgeon’s preferred technique: iris fixation (10–O Prolene [Ethicon]), glued IOL through scleral tunnels, or sutured IOL with scleral flaps using 10–O Prolene or CV-8 Gore-Tex fixation (W.L. Gore & Associates) with rotated sutures. All three techniques are reasonable and could be considered based on the surgeon’s experience.
The fibrotic capsule (possibly with a dense Soemmering’s ring or even a capsular tension ring) supporting the IOL can be salvaged, and the fibrotic material may be used to aid in fixation for scleral suturing. In these cases, I prefer a CV-8 Gore-Tex suture to the sclera or a 10–O Prolene suture to the iris. For scleral suturing, after a conjunctival peritomy, the Gore-Tex suture can be passed through 23-gauge sclerotomies (3 mm apart) using a 25-gauge microforceps. The suture can then be tied externally and turned to bury the knot. With 10–O Prolene iris fixation, a Siepser sliding knot technique can be used to secure the lens to the iris. Alternatively, a handshake technique (popularized by Amar Agarwal, MD) could be used to externalize the haptics and pass them through scleral tunnels to be secured by fibrin glue beneath a scleral flap. Surgeons are fortunate to have several different options to effectively handle complicated cases such as this one while avoiding IOL explantation and even vitrectomy in many instances.

PRIYA NARANG, MS
The three factors that would guide treatment are the presence of monoocular subjective diplopia, the good visual status, and the fibrosed anterior capsule with a decentered IOL. Initially, I would prefer to perform an Nd:YAG laser capsulotomy, create radial relaxing incisions around the margin of anterior capsular phimosis, and assess whether or not the release of adhesions helped to center the IOL and eventually resolve the complaint of diplopia. If Nd:YAG laser treatment did not help, then a surgical maneuver with cutting down of fibrotic adhesions around the anterior capsular fibrotic stricture could be tried with the help of microscissors. This would alleviate the contractile forces on the IOL, leading to its decentration. Afterward, I would reassess the decentration of the capsular bag and IOL. At this stage, I would not contemplate putting a capsular fixation device in the bag, because the capsular margin is already compromised and it might be difficult to create enough space in the capsular bag.
Watch it Now
Priya Narang, MS, shows her approach to another case of a decentered three-piece IOL associated with a break in the posterior capsule.
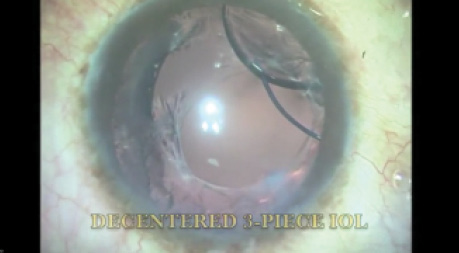
Rafael Catañeda Diez, MD, uses a single knot to repair a subluxated IOL-capsular tension ring complex.
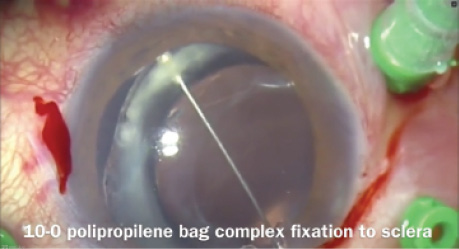
Michael Klufas, MD, and Pradeep Prasad, MD, demonstrate fixating an Akreos AO60 lens to the sclera using a Gore-Tex suture.
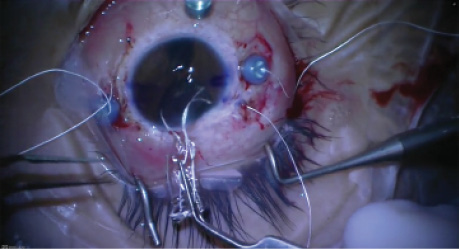
I would consider glued intrascleral fixation of the IOL (glued IOL) for this case (see Dr. Narang’s video in Watch It Now). A three-piece lens is already present in the eye, and I would take advantage of this clinical scenario. I would make two partial-thickness scleral flaps 180º opposite to each other and introduce infusion in the eye. After making a sclerotomy beneath the scleral flaps, I would introduce a glued IOL forceps from one sclerotomy site and hold the entire bag-IOL complex. I would then introduce a vitrectomy cutter from the other sclerotomy site, perform a thorough vitrectomy around the IOL, and cut down all fibrotic adhesions. Next, I would remove the vitrector, introduce another glued IOL forceps, and externalize the haptics of the three-piece IOL from the sclerotomy sites followed by intrascleral tuck and fibrin glue application to seal the flaps. Using the same IOL would ensure and continue the advantage of a closed-chamber approach.

KARL STONECIPHER, MD
First, I would try to find a copy of the original surgical records, which might or might not help me to determine the original surgeon’s experience. Unfortunately, in many of these cases, I find a standard dictation despite evidence of intraoperative surgical issues. Often in such situations, I will contact the surgeon directly and ask him or her to pull the chart and let me know of any issues that could help me deal with the case.
Next, I would discuss with the patient the options of trying to recenter this lens versus replace it. I would explain that many decisions may be made intraoperatively but that I will address the options in the informed consent and document the discussions in the chart. Intraoperatively, I would first try to stabilize the capsular bag-IOL complex by scleral fixation with a double-armed suture of either Prolene or Gore-Tex material. In cases such as this one, a strategically placed suture can often recenter and stabilize the lens in a good position. Rafael Catañeda Diez, MD, demonstrates an alternative approach in a more difficult case on Eyetube.net (see Watch It Now).
If suturing proved difficult, I would try to viscodissect the lens and prolapse it into the anterior chamber after placing a tamponade of viscoelastic behind the IOL itself in the case of posterior capsular compromise. In my experience, it is possible to manipulate these silicone lenses with care even after 9 years. If I could sulcus fixate the lens with good positioning, I would leave it in the sulcus and execute a classic McCannel suture to fixate the IOL to the iris superiorly so as to give me confidence that the IOL would stay where I placed it. At a later date, I could deal with the residual capsular bag in the visual axis via an Nd:YAG laser capsulotomy using the Ultra Q Reflex (Ellex). I believe this laser provides me with the best ability to tailor my treatment to the patient.
If neither of the options I have described seemed feasible, then I would remove the lens from the eye, replace it with an Akreos AO60 lens (Bausch + Lomb), and rely on Gore-Tex sutures and sulcus fixation using the residual capsular bag for support (see Drs. Klufas and Prasad’s video in Watch It Now). Based on how the eye looked after fixation, I might or might not perform a pars plana vitrectomy to remove residual capsular bag in order to open the visual axis. I would hope, by this point, that vitreous had not presented as an intraoperative challenge, and again, I could use the Ultra Q Reflex laser postoperatively to clear the optical pathway at a later date as needed.
I like to operate on patients such as this one early in the day and to check them 3 to 4 hours after surgery to confirm stability of the lens and evaluate the IOP, because residual viscoelastic can be an issue. I also increase my standard postoperative drug regimen to quell inflammation.




