
Visual acuity outcomes after cataract surgery are more precise than ever, and patients’ expectations are at an all-time high. This presents a challenge to surgeons, because more than a spherical equivalent result is necessary to meet these expectations.
AT A GLANCE
• Patients’ expectations are at an all-time high, and more than a spherical equivalent result is necessary to meet these expectations.
• The new Alcon Online Toric IOL Calculator can improve postoperative results and help surgeons meet patients’ expectations.
• The calculator has incorporated several important changes that make data entry easier, increase the accuracy of postoperative astigmatism prediction, and provide customizable and clear data printouts.
Preoperatively, the vast majority of patients have at least 0.75 D of astigmatism, and two-thirds of patients have between 0.75 and 1.50 D of corneal astigmatism. Because even small amounts of residual astigmatism will decrease visual acuity and quality of vision, accurate preoperative measurements and sophisticated planning for intraoperative management are key to providing excellent visual outcomes. The new Alcon Online Toric IOL Calculator is an important tool for improving postoperative results and meeting patients’ expectations. It is available at www.myalcon-toriccalc.com.
FEATURES
A key feature of the calculator is its incorporation of the Barrett toric algorithm for toric power calculation and axis determination. I have been using the Barrett formula for toric IOLs for the past 2 years and have seen a significant improvement in my refractive results, with less residual astigmatism and better UCVA postoperatively.
This formula theoretically accounts for posterior corneal astigmatism, it calculates a patient-specific effective lens position, and it recommends toric IOL powers with the least residual astigmatism. The formula is designed to improve preoperative refractive predictability by using a centroid value for surgically induced astigmatism (SIA). The centroid value takes into consideration the direction as well as the magnitude of SIA and is therefore a smaller value than has been traditionally used, given that values in opposing directions cancel each other out. The SIA centroid has less variability among surgeons compared with the mean or median values, and it is less sensitive to incision location, according to Warren Hill, MD.
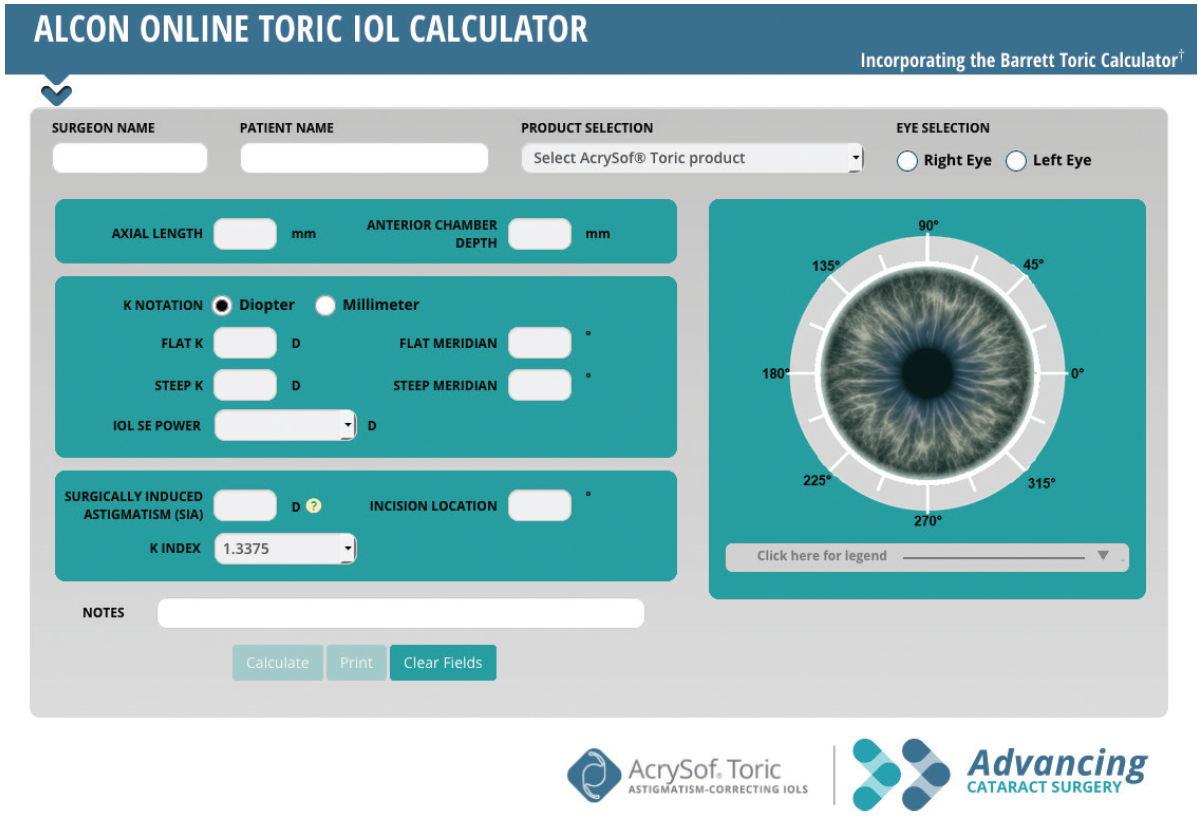
In a September 2016 email to CRST, Dr. Hill explained: “The problem with using a mean or a median value for surgically induced astigmatism is that there is significant variability from one patient to the next. This is because the cornea of each patient is different in terms of the radius, thickness, and rigidity. The incision location and size may also have an influence. If we create a 2-D plot of SIA for a series of patients of the magnitude and the orientation, this gives us a centroid value. For most surgeons, this value is something between 0.10 D and 0.12 D. I have a website for calculating surgically induced astigmatism with about 36,000 cases that have been entered by surgeons worldwide (SIA-calculator.com). When I do a centroid calculation for any of the 550 surgeons who have used this, I always get about the same number for a temporal, clear corneal incision: around 0.10 D. Graham Barrett has presented this at multiple meetings, and this is the reason why a centroid value for surgically induced astigmatism is used with his Barrett toric calculator.”
CUSTOMIZED CENTROID VALUES
Surgeons can calculate their own centroid values at Dr. Hill’s site and then plug those values into the formula for even greater accuracy. I use a centroid value that is specific for the type and size of incision made (laser vs manual), lens type, and left or right eye. The default value of 0.1 suggested on the Alcon website also works well in my experience. It is close to the specific calculated values I have for my SIA.
I have found the new online calculator to be easy to use, with its intuitive user interface and customizable printouts. Entering the required data into the appropriate cells of the online spreadsheet is straightforward. The data output includes a range of toric IOL recommendations with associated predicted residual astigmatism. The printout can be rotated to the appropriate orientation based on the surgeon’s operating preference—temporal versus superior—so that the data are easy to read during surgery.
LIMITATION
One limitation of the Alcon Online Toric IOL Calculator is that the IOL spherical equivalent power (not the astigmatic power) has to be entered manually and is not calculated by the online program, unlike the Barrett toric calculator that is available on the American Society of Cataract and Refractive Surgery’s website. The latter Barrett calculator determines both the spherical equivalent power and the toric power based on the data entered. With biometers that include the Barrett universal formula, such as the Lenstar (Haag-Streit), the base lens power can be calculated without additional data entry.
CONCLUSION
The new Alcon Online Toric IOL Calculator has incorporated several important changes that make data entry easier, increase the accuracy of postoperative astigmatism prediction, and provide customizable and clear data printouts. These features should help ophthalmologists to manage astigmatism with even greater predictability, a fundamental goal of modern refractive cataract surgery.




