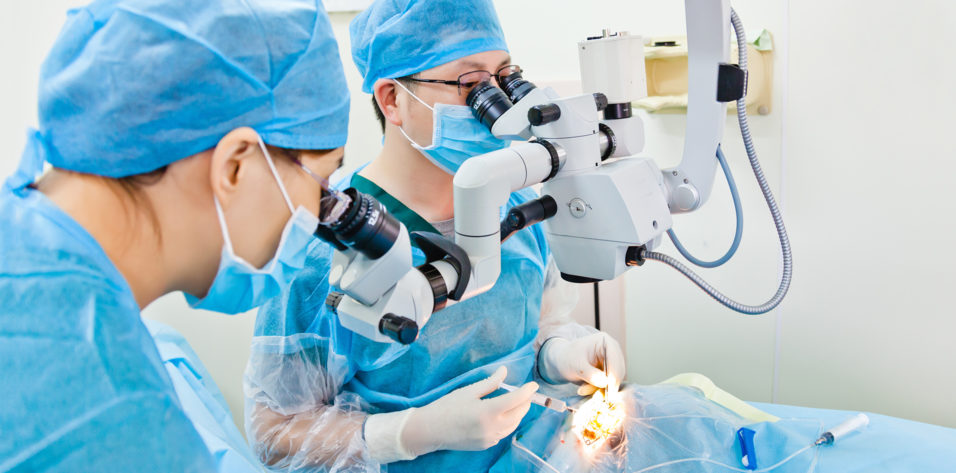
CRST recently spoke to Chief Medical Editor Robert J. Weinstock, MD, about practice efficiency and the use of physician extenders.
CRST: What are the options available to surgeons with regard to delegating parts of patients’ management to or sharing it with other care providers in the practice? Do you make use of optometrists and other physician extenders in ways beyond a more traditional model of shared care?
OPTOMETRIC CARE
Robert J. Weinstock, MD: Optometrists are the most common example of the use of physician extenders. The best use of ODs is a creative modeling unique to the surgeon’s practice’s situation, and optometrists have many opportunities to be involved in patients’ care. For example, an OD in an ophthalmic practice may be revenue producing in his or her own separate clinic on site or in a satellite office, nonrevenue producing seeing patients in the surgeons’ clinic or seeing postoperative patients inside the global period, or a combination of both. Some optometrists may be general eye care providers, and some are subspecialists; there are therefore different models depending the practice’s needs
At the Eye Institute of West Florida, we have eight optometrists in our practice. Most are general eye care providers; they perform routine care like eye exams for glasses and contacts, routine pediatric care, and routine yearly follow-ups for pseudophakic patients. These providers do not do many tests; rather, they refer patients needing a higher level of care to an MD subspecialist if they identify a disease process needing more subspecialized attention. General optometrists can conduct routine eye and contact lens examinations in phakic and pseudophakic patients. Although this is the most simplistic role of an optometrist, it is very valuable. In this model, the OD takes much of the burden off the surgeon in terms of seeing pseudophakic patients and patients with healthy eyes and only in need of a routine yearly exam. In addition, they also function as a “triage” or “urgent care eye clinic.” When patients called with a problem, we used to try to handle it over the phone because we were so busy. Now, we always offer them the choice to come in and be seen. If the OD can handle the situation, he or she may bill for the visit, or he or she can have the patient see an MD if needed.
CRST: The surgeons are then freed up to do the things only the surgeon can and should be doing.
Dr. Weinstock: Yes, optometrists’ providing routine care frees up the surgeon’s schedule so that he or she can see more surgical consults and handle more acute care situations. In my experience, that model of ODs providing general eye care can generate anywhere from $150,00 to more than $300,000 a year in revenue, depending on how busy they are
CRST: Typically, contact lens examinations are not covered by insurance the way a vision plan might cover a glasses examination, so would that be out of pocket for the patient?
Dr. Weinstock: It depends on the vision plan. For the optometrists we are talking about here, some of their services are insurance based, and some are cash pay. Let us assume that the average salary for an optometrist is somewhere between $90,000 and $120,000 and that they are assigned one technician. If that optometrist is bringing in roughly $180,000 or more, the arrangement can be profitable for the practice.
CRST In what other ways can this simple arrangement benefit the surgeon or the practice?
Dr. Weinstock: The practice can generate more income, because the surgeon has expanded room in the schedule to provide improved service and a superior experience to new patients or those who are having problems. The surgeon is not slammed with providing routine care.
CRST: How does the model look in a very busy subspecialized practice?
Dr. Weinstock: In our practice, we have another model as well. We have two very busy glaucoma surgeons and an optometrist who underwent a medical glaucoma fellowship with ophthalmologists at Bascom Palmer. The OD has a strong interest in medical glaucoma management, and she can now treat the patients who need routine glaucoma care. These are patients with mild to moderate, stable, open-angle glaucoma who do not currently need a surgical intervention, or maybe the patient has had surgery and requires routine follow-up visits (we check visual fields and pressures every 3 to 6 months). The fellowship-trained optometrist can do a more thorough examination than a general OD. Because of her additional training, she can perform additional testing as well: with the diagnosis of glaucoma, patients require periodic optic nerve imaging, nerve fiber layer analysis, visual fields, gonioscopy, etc. This optometrist can do what she enjoys, generate significant income, and take some of the burden off the glaucoma surgeons who are busy with more surgical and acute care situations.
CRST: Her salary would be higher than the general OD’s, but she can bill for a lot more.
Dr. Weinstock: Yes, the income she generates well supersedes her salary and the cost of an additional technician to help her. Because she is subspecialized and providing more in-depth exams and testing, she is adding billing and collections greater that what a comprehensive OD usually generates
CRST: Do you have other ODs with special interests in your practice?
Dr. Weinstock: Yes, we have an optometrist who is subspecialized in refractive surgical eye care, both pre- and postoperative treatment. She did a medical OD fellowship at Omni Eye Care in Atlanta, and then she did another fellowship with me in refractive corneal and lenticular surgery. She helps me immensely not only preoperatively but, more importantly, postoperatively. She monitors the patients and makes sure the outcomes are on target, she tracks the results, and she is responsible for biometry. I think of her as an outcome specialist, and she can flag patients who are not doing as well as they should. She can identify those who need enhancements, perform the appropriate testing, and treat minor postoperative issues. She ensures the patient sees me again if needed for an additional refractive procedure like a PRK or LASIK touchup or even a limbal relaxing incision with a laser or manually at the slit lamp. In addition, she follows up with the patients every year. It’s a very hands-on approach to make sure the refractive surgery patients (cornea and cataract) do not get lost to follow-up. It also adds to the patient’s experience at the practice, and we promote a “team approach” so that the patients always feel they have access to help if they need it.
CRST: That way, her practice grows year to year as the number of cataract surgeries that are done grows.
Dr. Weinstock: Exactly. Those surgical patients become routine, paying patients, so in that way, she is kind of a hybrid of the models we are discussing. Some of her time is spent doing nonrevenue-producing tasks, like seeing postoperative patients and running the biometry department, but that allows me to have more time to see new cataract consultations and spend more time in the OR. Some of her time is spent caring for postoperative patients who are outside of their postoperative period, which generates income. In this subspecialized yet hybrid income model, she may not actually cover her salary in terms of income production, but that is made up in the time she saves me and many intangible benefits that lead to great outcomes, great patient experiences, and practice growth.
THE OCULAR SURFACE
CRST: What about ocular surface disease? How do you handle that in your practice?
Dr. Weinstock: We employ a physician’s assistant (PA), and one of her roles is to treat and monitor patients with ocular surface disease (OSD) as well as to be a resource to our surgeons. If a preoperative cataract patient has OSD, it is the PA’s job to treat the patient before we do surgery. If a patient experiences OSD symptoms after surgery, the PA will manage him or her. She did a fellowship under our corneal specialist (Neel Desai, MD) to learn how to manage OSD. In addition, she can do minor procedures like punctal plugs, chalazions, foreign body removals, etc.
In trying to advance this aspect of the practice, we are also seeking an optometrist who has a real affinity for and advanced training in OSD. The key is to identify an OD, or even a PA or a nurse practitioner (NP), for that matter, who can fulfill a mini dry eye disease fellowship. For example, conferences offer intensive training on managing OSD patients, and there is a huge opportunity in most practices to have and market that type of specialist.
The caregiver needs to understand the disease process, know how to make a diagnosis with the proper point-of-care tests, and be an expert on managing patients with the condition. This is a ripe area for a practice to employ additional caregivers.
CRST: Are there other roles for a PA within an ophthalmic practice?
Dr. Weinstock: The PA also takes the history and performs physicals on patients, which are billable services. She can also assist in glaucoma, oculoplastic, and retinal surgery; there is an associated assistant fee for those services. Our PA represents a hybrid in terms of the various services she provides. Ideally, I think there is room for someone like her to manage OSD full time, but right now, she is wearing quite a few hats as a PA. An NP, for example, could fulfill those same roles. In addition, there are cosmetic services that our oculoplastic surgeon performs in which our PA is involved.
Theoretically, an NP or PA could do LipiFlow (TearScience) and intense pulsed light procedures. The advantage over an OD would be the scope of care. Under a doctor’s supervision, NPs and PAs are licensed and trained to do minor surgical procedures such as removing a chalazion, sutures, and foreign bodies; inserting punctal plugs; and executing a whole host of other minor ocular and skin procedures.
CRST: This sound like an attractive career path.
Dr. Weinstock: PAs and NPs would get little exposure to these procedures mentioned in traditional training. It would require them to come into a practice and train for a period of time. There is no question it is a big investment, but if a practice hired a PA and had him or her perform some of the minor procedures we discussed, and if the surgeons performed the complex procedures, the PA would be producing income right away. The surgeon could then carve out time for the PA to train under him or her, manage pre- and postoperative patients and OSD, and after a year or so, the PA could transition into those roles as well.
CRST: It is a big commitment but with a potentially huge upside.
Dr. Weinstock: That is right. It is not all about the letters following the provider’s name; it is about training, experience, and the scope of care.
CRST: Do you believe that the use of these alternative caregivers will become more common?
Dr. Weinstock: Clearly. Surgical demand will continue to rise, and the surgeon’s time pressures will increase. There will be more pressure on practices to have routine, basic care provided by ancillary care professionals. There will be a real push to find qualified people to help the surgeon care for the swelling volume of patients that need care. However, I still find that it is absolutely critical for the surgeon to examine and make a surgical recommendation to the patient prior to surgery. The decision to proceed with surgery and the discussion with the patient regarding the refractive goals, technology employed, and expectations is oftentimes the most challenging and important event in the delivery of great care.
CRST: There is also the move toward earlier surgical interventions and away from drugs that rely on patients’ compliance for efficacy.
Dr. Weinstock: Patients on medications need to be observed, too. Take something as simple as starting dry eye patients on Restasis (cyclosporine; Allergan) or Xiidra (lifitegrast; Shire); those patients may need a steroid as well. That requires seeing the patient again in 2 to 3 weeks and rechecking him or her and periodic visits. That is a prime role for another provider that will free the surgeon from having to perform that kind of a basic follow-up examination.
PATIENTS’ ACCEPTANCE
CRST: How do you explain to the patients whom they are seeing and why?
Dr. Weinstock: It does require education in the practice. Patients need to know upfront that they may not see the surgeon except at the consultation before surgery, for the surgery, and maybe once after, or maybe they will not see the surgeon again at all. We say to the patient, “If you do not see the surgeon, that is a good thing! It means you are doing well.” Then, it becomes a real positive when a patient only needs a quick follow-up check with another provider. They tend to wait longer in a busy surgeon’s practice than they would seeing a PA, NP, or OD. It also helps for the OD to meet the patient with the surgeon on the front end so it’s a familiar face seen postoperatively. This creates the team approach, continuity of care, and a great patient experience
CRST: So, you are providing better customer service. Plus, patients typically feel comfortable with PAs, NPs, and ODs, as they are used to that with their primary care visits.
USING FELLOWS
Dr. Weinstock: Using fellows in the practice also falls into this discussion. This is a very cost-effective and mutually beneficial way of providing added support for the patients in a surgical practice. There are many scenarios where this makes sense, such as 1-day postoperative visits, routine follow-up, or emergency visits where the patient should see an MD. A refractive surgery patient, for example, should receive high-quality care and an excellent experience. Fellows can quickly learn the surgeon’s preferences and enhance his or her efficiency. Certainly in the OR, especially if the surgeon uses femtosecond lasers, it is a huge benefit to have a fellow doing that part of the procedure so the surgeon can concentrate on the intraocular portion of cataract surgery. It is also great to have another set of eyes on the biometry and outcome targeting, which is an area where mistakes can be made if there aren’t checks and balances in place.
CRST: The fellow is getting invaluable experience and knowledge.
Dr. Weinstock: Exactly. Fellows are like any other ophthalmologists in the practice, but their salary is dramatically lower than if they were fully out of training. They can have full-fledged regular clinics as well, which produce income covering the cost of their fellowship salary.