
Complementing Strengths
By Mark Kontos, MD
There was a time when there were no optometrists working at Empire Eye Physicians. Looking back now, that seems like another world, one we would never consider going back to. Optometry has become an integral and indispensable part of who we are as a practice. It was not always that way, but as our practice and eye care have evolved over the past 20 years, it is a fact today.
In the late 1980s, our practice decided to work more closely with optometry in the comanagement of cataract patients. Several local optometrists with whom we were exploring working recommended that we hire an optometrist to help manage the care of patients and to act as a liaison between the community optometrists and our practice. We involved them in the hiring process to make sure we found a good fit. Our cataract practice grew rapidly, and the optometrist we hired, Frank Galizia, OD, soon became an experienced medical optometrist who worked closely with our referring doctors. He quickly became the local expert on cataract surgery and helped educate the optometric community on the postoperative care of cataract patients.
Dr. Galizia’s role expanded to include organizing continuing education for local optometrists through our office and refining the comanagement process. He was also the practice ombudsman, handling issues that would inevitably arise on occasion. All of this allowed my partner and me to focus on what we loved to do most: surgery. In a short time, the practice doubled and then tripled its surgical volume. This never would have been possible without bringing an optometrist on board.
AT A GLANCE
• The growth of refractive surgery correlated with the expanding role of optometrists in several ophthalmic practices is profiled herein.
• Combining optometric and ophthalmic expertise can increase productivity in an eye care practice and enable greater contributions to the field at large.
• Dedication to growing and maintaining relationships between ophthalmologists and optometrists is a worthwhile investment for practices, staff members, and patients alike.
The role of optometrists in our practice became even more crucial with the rapid growth of LASIK in the 1990s. Dr. Galizia was deeply involved in the development of our refractive surgery practice and referral network. He learned with us which patients were good LASIK candidates and picked up all of the ins and outs of postoperative care and the management of complications. Again, he was the key educator of the local optometric community. We became one of the leading refractive surgery practices in the Pacific Northwest, largely due to the efforts of our optometrist.
Fast forward to the present, and we have continued to expand the roles of our optometrists, Casey Claypool, OD, and Alicia Heaton, OD. They work closely with our referring doctors to help strengthen our referral networks. They organize all of our continuing education programs throughout the year and help develop our marketing programs. They have become key opinion leaders and speak at meetings locally and nationally. Clinically, their roles have continued to grow, and now our optometrists conduct most routine care visits and the majority of postoperative care. Our practice has also built a robust ocular surface disease clinic run entirely by our optometrists (Figure). Our collagen cross-linking practice and specialty contact lens program also rely heavily on them. All of this allows the ophthalmologists the luxury of primarily seeing patients with significant pathology or those needing surgery.
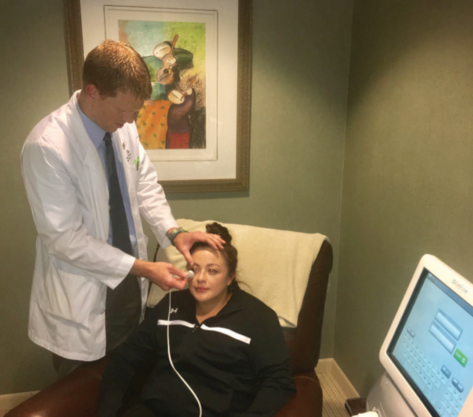
Figure. Dr. Claypool performs intense pulsed light therapy at Empire Eye Physicians.
Going forward, it seems that practices that have successfully integrated optometry will be better able to thrive in what is sure to continue to be a challenging environment. For our practice, employing optometrists has been rewarding both professionally and financially. Optometrists have become an integral part of who we are as a practice. In the future, there is no doubt that optometry will play an ever-increasing role in our continued growth.
An Uncommon Partnership


By Edoardo Ligabue, MD, and Cristina Giordano, OD
Our professional relationship began 20 years ago, around the time of the birth of refractive surgery. Over the years, we have been able to combine our respective medical and surgical skills (E.L.) and optical physics knowledge (C.G.) to achieve winning results. We have also always upheld the belief that a successful partnership between an ophthalmologist and an optometrist must be based on trust and respect. This collaboration has brought us success in various areas throughout our working history and has enabled us to keep patients’ satisfaction and the growth of our practice in sharp focus.
We started working together in 1996, when corneal topography was introduced. Around this time, we coauthored our first publication, an article on the corneal map of the Orbscan II (Bausch + Lomb). Later, as studies of aberrometry emerged, we began implementing aberrometric evaluation into our practice. This was our first step into the challenging and evolving arena of premium IOL surgery.
Our first aberrometer was the OPD-Scan II (Nidek). We started to evaluate the aberrometric map after our first implantation of an aspheric IOL in cataract surgery. In November 2007, we coauthored an article on interpreting aberrometric measurements in cataract surgery using dynamic skiascopy to evaluate visual quality after aspheric and multifocal IOL implantation.1 After this experience, we both started to speak at international meetings, where we presented papers and communications concerning the optical proprieties of premium IOLs, patient selection, and proper pre- and postoperative examination. In our experience, the partnership between a surgeon and an optometrist who is an expert in optics allows the surgeon to better understand how an IOL works and, overall, is valuable in determining a solution for patients who complain of low visual quality, photic phenomena, or unexpected results.
Our shared interests and efforts also include accommodating IOLs. We were able to work with Nidek to develop a module that could be used to evaluate changes in optical aberration during the accommodative process. Using the accommodative module in the OPD-Scan II, we conducted a study of the Crystalens HD (Bausch + Lomb) and presented several talks on our experience with and observations of this lens.2,3 With the introduction of toric IOLs into our clinical practice, cataract surgery became a refractive procedure, wherein our combined knowledge and experience were further beneficial in conducting valuable research and achieving optimal results.4,5
Over the years, our clinical practice evolved to the point at which we felt we needed to upgrade our technology. We were performing refractive surgery with the Allegretto Wave Eye-Q (Alcon) and felt we needed to incorporate laser technology into our refractive cataract surgery as well. In September 2012, we introduced the use of the Victus femtosecond laser (Bausch + Lomb) for cataract surgery, with Dr. Ligabue as the surgeon and Dr. Giordano as the key operator (Figure 1). The femtosecond laser allows us to obtain a capsulorhexis perfect in centration, diameter, and circularity; to create different fragmentation patterns; and to use little or no ultrasound energy. IOL positioning with the laser is precise in terms of centration, stability, and the avoidance of tilt.
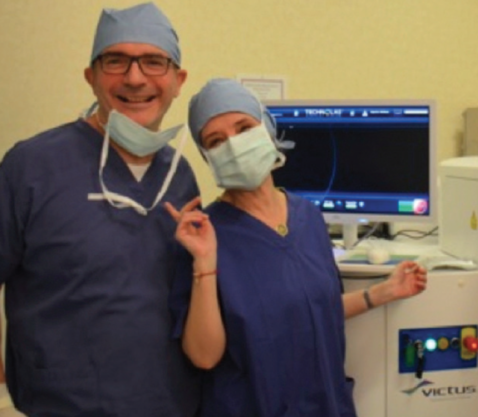
Figure 1. Drs. Ligabue and Giordano in the laser room.
In our opinion, the introduction of another technology, real-time optical coherence tomography, has made cataract surgery even safer. We have also been able to introduce the use of this software for corneal procedures such as LASIK, intrastromal corneal ring segments, and multiple types of corneal transplantation.
In addition to upgrading our cataract procedures, we felt we needed to improve the effectiveness and reliability of femtosecond laser programming. We set out to create a nomogram to determine correct energy levels for laser capsulotomy and lens fragmentation. Based on evaluation of the anterior corneal surface gradient map, the software calculates the average of all sections for change in axial curvature from the center to the periphery; we select the data, and the nomogram determines the correct energy needed to obtain a free-floating capsulotomy. At the same time, we evaluate the change in refractive index by analyzing the densitometry of the nucleus using a Scheimpflug camera. We insert the percentage value in the nomogram to select the correct fragmentation energy. This nomogram is another example of the strength of combining ophthalmic and optometric knowledge.
Today, premium cataract surgery requires superior results in terms of refractive error and visual quality. The modern patient’s expectations are high, so strong cooperation between surgeon and staff throughout the pre-, intra-, and postoperative periods is crucial. We have organized a diagnostic platform with the most useful tools for refractive, cataract, and corneal surgery, all connected to the laser room; this way, the surgeon can review a printout of the patient’s examination before a femtosecond laser procedure. For toric IOL implantation, having these tools connected to the laser room allows the key operator (C.G.) to select the femtosecond laser parameters and to meet with the surgeon (E.L.) to evaluate the corneal markings for axis orientation of the laser incisions (Figure 2). In the postoperative phase, the surgeon’s final evaluation of the patient is fed into the nomogram calculation to improve the preoperative process and surgical procedure.
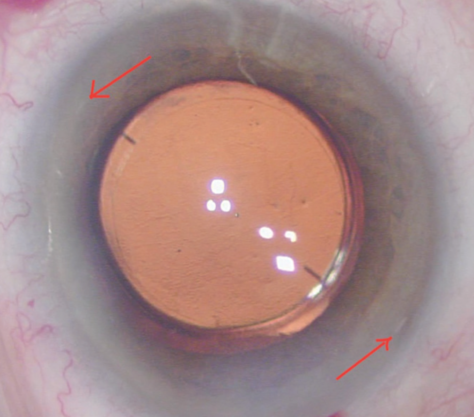
Figure 2. Femtosecond laser corneal limbal reference for toric IOL alignment.
In Italy, collaboration between ophthalmologists and optometrists is uncommon, because Italian regulation assigns the role of assistant in ophthalmology to the orthoptic graduate. Our successful experience demonstrates that this collaboration can, in fact, serve to promote productivity and enhance patients;=’ care.
1. Ligabue EA, Giordano C. Interpretation of aberrometry measurements in cataract surgery. J Refract Surg. 2007;23:S996-S1004.
2. Ligabue EA, Giordano C. Aberrometrical evaluation after Crystalens HD implant. Paper presented at: 14th ESCRS Winter Meeting; February 12-14, 2010; Budapest, Hungary.
3. Ligabue EA, Giordano C. Visual performance with Crystalens HD. Paper presented at: XXVIII Congress of the ESCRS; September 4-8, 2010; Paris.
4. Mencucci R. Preliminary results after toric IOLs implant. Paper presented at: the XXIX Congress of the ESCRS; September 17-21, 2011; Vienna, Austria.
5. Mencucci R, Giordano C, Favuzza E, et al. Astigmatism correction with toric intraocular lenses: wavefront aberrometry and quality of life. Br J Ophthalmol. 2013;97(5):578-582.

Pillars of Success
By Jason Schmit, OD
Vance Thompson Vision is an integrated ophthalmology and optometry practice with locations in Sioux Falls, South Dakota, and Fargo, North Dakota. We specialize in laser vision correction, cataract surgery, and corneal procedures, and we have clinics focused on glaucoma, oculoplastics, and research. We also have a large dry eye practice integrated into our business model. Our practice is primarily driven by our optometric comanagement network and word-of-mouth experiences through patient-to-patient interactions. We do some direct-to-consumer marketing through social media sites, television, and direct mail. The key to our success is outlined under our three pillars: (1) invest in the world’s best technology, (2) create a fantastic patient experience, and (3) do the right thing (Figure).

Figure. The three pillars of success at Vance Thompson Vision.
We have four ophthalmologists and five optometrists in the practice. As one of these optometrists, my role is to see every patient as the primary eye care doctor and to determine the surgical plan, whether it be for cataract surgery, laser vision correction, or eyelid procedures.
For cataract surgery patients, I determine whether standard or laser-assisted surgery is to be performed, the type of IOL to be implanted, whether astigmatic correction is needed, and what postoperative drop management (standard drops or drop-a-day option) is called for. Once I complete the surgical plan, the surgeon then comes in to meet the patient, review the surgical plan, and sign off on the chart. I also see most of the postoperative cataract patients at their day 1 visit, and the patients are then released back to their referring optometrist.
Our laser vision correction model is similar. I see all patients preoperatively and determine whether they are good candidates for surgery, which procedure is best (LASIK, PRK, phakic IOL, etc.), which technology is best (standard, wavefront-guided, wavefront-optimized), whether we will target a plano result in both eyes or monovision, and any other surgical variations. Patients are seen postoperatively by the referring optometrist.
Our oculoplastics clinic is run in a similar way. I see patients first to determine whether blepharoplasty, ptosis surgery, eyebrow correction, lateral tarsal strip, or some other surgical alignment of the eyelids is needed. The surgeon then meets the patients, agrees with or amends the decision, and signs off on the surgical plan.
Basically, our ophthalmology-optometry model accomplishes three things: (1) our optometrists get to practice at the highest level of their capabilities; (2) our surgeons get to spend most of their time doing what they enjoy most: surgery; (3) and our patients get the best of everything (ie, two doctors aligned in the surgical decision management of each case).
I am in constant communication with my surgeon, with a focus on our annual business and growth objectives. I get to see new pathology patients; manage dry eye patients; and help teach medical fellows, optometry students, and referring optometrists while they are in our clinic observing or completing their clinical rotations or programs. The surgeons can focus on surgery, strategic planning around the business, and other business ventures and consulting opportunities. Our business model also allows the surgeons more personal time outside of the clinic while maintaining annual growth of the practice.
We are heavily driven by optometric referrals, so we spend an enormous amount of time dedicated to creating and maintaining these relationships. Communication is everything. We send dictated letters to referring doctors for all patient visits. We have a dedicated person committed to optometric practice relations. We schedule weekly practice visits for optometrists, to be accompanied by one of our Vance Thompson Vision doctors, whether an optometrist or ophthalmologist. We also send quarterly newsletters and have developed an optometric portal to our website focused on clinical information that applies to our practice. We sponsor, through our foundation, an annual 2-day optometric practice symposium attended by more than 300 optometrists and staff members, focused on learning and enhancing doctor-to-doctor relationships.
Under our third pillar, doing the right thing, we also focus on our people. We invest in training and education to help improve the knowledge base of our team. We empower team members to make the best decision for any given patient on a daily basis, even if some financial outlay is required to make things right.
We have a monthly staff fun day, where we all might go sledding together, go to a baseball game, or meet at the office after work for a family Easter celebration or an October Halloween party. We work hard and respect each other, but we play hard, too. Attention to culture comes first. Without good people who love their jobs, nothing else can happen.
This is how we have become successful: we are caring, fun, committed, and egalitarian.




