
Although the vast majority of corneal refractive surgery patients are satisfied with their outcomes, those who seek refinement through additional procedures can present challenges. I would argue that every secondary refractive procedure should be considered a complex case. These patients will have increased expectations, because their first procedure was not completely successful. Moreover, these individuals may be responsible for the additional cost of the secondary procedure, but surgery will often be less predictable because of their altered cornea.
AT A GLANCE
• Despite the seemingly benign nature of enhancements after radial keratotomy or LASIK, these procedures are actually much more challenging than primary laser vision correction (LVC).
• Any signs of corneal instability, either before or after the primary corneal procedure, are a contraindication for further LVC unless it is performed after corneal collagen cross-linking.
• A LASIK enhancement after radial keratotomy runs the risk of fragmenting the flap during its manipulation or of vertical gas breakthrough when a femtosecond laser is used. PRK is thus a safer and simpler option.
• For post-LASIK enhancements, determining the target refraction can be difficult, because these eyes will have increased spherical aberration from the initial LVC procedure. The author recommends performing the minimal amount of myopic or hyperopic correction in order to avoid overtreatment.
All secondary procedures should be approached with vigilance. It is important to review the preoperative topography and tomography scans whenever possible to ensure there were no signs of corneal instability. Prior to the secondary laser vision correction (LVC) procedure, patients should exhibit refractive stability for at least 3 to 6 months.
In some cases, nonsurgical options may be the best choice. Although this article focuses on the LVC of postoperative refractive errors, other procedures may be more appropriate in specific situations. For example, intraocular surgery may better address a large spherical error, particularly if the patient is presbyopic. If the spherical equivalent is close to zero, corneal relaxing incisions are another refractive option. Any signs of corneal instability, either before or after the primary corneal procedure, are a contraindication for further LVC unless it is performed after corneal collagen cross-linking.
RADIAL KERATOTOMY
LVC after radial keratotomy (RK) typically presents a number of challenges. These patients have usually undergone a steady hyperopic shift that has left them with iatrogenic hyperopia. Oftentimes, they have coexisting hyperopic astigmatism because of asymmetric RK incisions. After RK, patients frequently experience diurnal fluctuations in their refractive error, with significantly flatter corneas in the morning.1 The magnitude of the diurnal fluctuation of their refraction must therefore be measured with early and late-day refractions. Then, it is important to conduct a contact lens trial of the target refraction, which can often be coordinated through the patient’s optometrist.
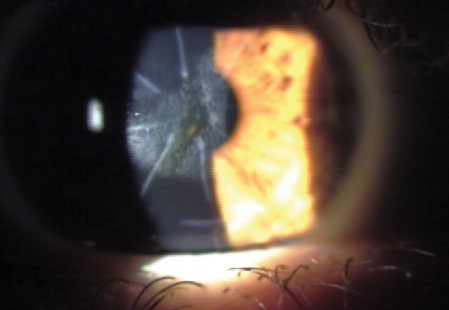
Figure 1. Previous RK with a residual refractive error is often best treated with PRK. Mitomycin C (MMC) should be used to avoid the postoperative haze seen here.
Although LASIK has been described after RK,2-4 it runs the risk of fragmenting the flap during its manipulation or of vertical gas breakthrough when a femtosecond laser is used. PRK is thus a safer and simpler option. During the procedure, the surgeon can remove the epithelium via phototherapeutic keratectomy, the application of alcohol, or an Amoils brush (Innovative Excimer Solutions). Transepithelial phototherapeutic keratectomy ablates approximately 50 µm of epithelium prior to the refractive correction. Alcohol can be used in various concentrations and times; I apply 100% alcohol for 10 seconds. I also find the Amoils brush effective for epithelial removal, particularly with primary PRK, because the instrument preserves healthy peripheral epithelium, which allows for faster recovery. In PRK enhancement procedures, I apply 100% alcohol for 10 seconds and then use the Amoils brush. The latter must be applied lightly so as not to open the RK incisions, but I find this approach provides a smoother bed than manual epithelial removal. After completing the excimer laser treatment, I administer mitomycin C 0.02% for at least 12 seconds (Figure 1).
LASIK
Post-LASIK patients’ desire for perfection is understandable, but it is also the reason that preoperative counselling on the risks and benefits of very small enhancements is critical, particularly for presbyopic patients who are slightly myopic. In these cases, contact lens trials can be invaluable, because they demonstrate the patient’s increased need for reading glasses after the enhancement. Determining the target refraction is challenging, because these eyes will have increased spherical aberration from the initial LVC procedure. I recommend performing the minimal amount of myopic or hyperopic correction in order to avoid overtreatment. The refractive correction needs to be adjusted so that the ablation depth corresponds with the size of the spherical equivalent refraction by about 16 µm per diopter to avoid an overcorrection.
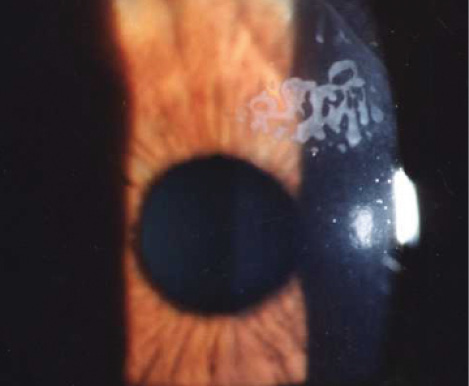
Figure 2. Epithelial ingrowth is not an uncommon complication after a flap-lift enhancement and can become recurrent.
There are several surgical approaches to LASIK enhancements. Although flap-lift procedures are usually an effective and safe option, the incidence of epithelial ingrowth increases with the duration of the postoperative period and can occasionally become a persistent problem (Figure 2).5 Laser side-cut enhancements and recutting the corneal flap offer a speedy recovery, but they can also be complicated by epithelial ingrowth as well as flap fragmentation if the second cut inadvertently intersects the primary cut. To avoid these issues, I have elected to perform PRK enhancement procedures for all of my post-LASIK patients. The epithelium can be removed with the same techniques described for post-RK PRK. I apply MMC 0.02% for at least 12 seconds to minimize postoperative haze.
CONCLUSION
Despite the seemingly benign nature of post-RK and post-LASIK enhancements, these procedures are actually much more challenging than primary LVC. Careful attention to preoperative counseling, surgical planning, and technique will help to ensure a successful outcome. n
1. MacRae S, Rich L, Phillips D, Bedrossian R. Diurnal variation in vision after radial keratotomy. Am J Ophthalmol. 1989;107(3):262-267.
2. Perente I, Utine CA, Cakir H, Yilmaz OF. Complicated flap creation with femtosecond laser after radial keratotomy. Cornea. 2007;26(9):1138-1140.
3. Leccisotti A, Fields SV. Femtosecond-assisted laser in situ keratomileusis for consecutive hyperopia after radial keratotomy. J Cataract Refract Surg. 2015;41(8):1594-1601.
4. Sinha R, Sharma N, Ahuja R, et al. Laser in-situ keratomileusis for refractive error following radial keratotomy. Indian J Ophthalmol. 2011;59(4):283-286.
5. Rapuano CJ. Management of epithelial ingrowth after laser in situ keratomileusis on a tertiary care cornea service. Cornea. 2010;29(3):307-313.
Louis Probst, MD
• national medical director, TLC Laser Eye Centers in Chicago; Madison, Wisconsin; Greenville, South Carolina; Tampa, Florida; and Cedar Rapids, Iowa
• (708) 562-2020


