Many ophthalmologists establish settings on a phaco machine when they first start using it and never look back. Just as we surgeons are always refining power calculations, instruments, and techniques, it behooves all of us to reevaluate our phaco settings regularly if we wish to deliver the best possible outcomes in cataract surgery.
I had tweaked my setting several times in the past, but I recently realized some time had passed since I last evaluated them. A good rule of thumb is that, if you cannot remember when you last adjusted your settings, it has been too long!
Some of us may intuitively understand the physics of phaco fluidics and easily adjust our own settings. The rest of us are fortunate to have phaco experts readily available in the form of manufacturers’ representatives. These individuals not only know the technology they represent very well, but they have also observed dozens or even hundreds of surgeons using the device and can use the experiences of many to help other surgeons.
When I sought assistance for my WhiteStar Signature System’s (Abbott Medical Optics) fluidics and power settings, it was not because I was dissatisfied with the device or with my technique. Rather, I wanted to make sure I was using the best possible settings to achieve the optimal surgical outcomes for my patients. As a result of that meeting, I made a number of improvements to my phaco settings.
MY TECHNIQUE AND SETTINGS
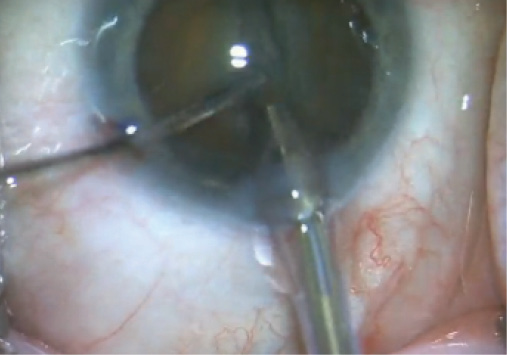
My preferred technique for nuclear disassembly is a supracapsular flip-and-slice technique that minimizes my need to maneuver inside the eye. In brief, I hydroprolapse the nucleus out of the capsular bag, then slice through it as I flip the lens toward me with a smooth spatula. This technique is described more fully in my article from the October 2013 issue of CRST, “The Flip-and-Slice Technique Is Safe and Efficient,” and on Eyetube (eyetube.net/?v=edigu).
I have three preestablished programs on the WhiteStar System for different types of nuclei: standard, dense, and slow motion. I use the slow-motion program when I need to be extra cautious, such as for patients with zonulopathy, zonular dialysis, pseudoexfoliation syndrome, or other situations in which I want to proceed slowly. I usually start cases in the standard mode unless I know in advance that the cataract is unusually dense or comorbidities warrant a slower approach. Perhaps surprisingly, given the relatively congested East Coast location of my practice, I do see a broad variety of lens types, including many brunescent and black cataracts.
THE UPDATE PROCESS
After working with my phaco representative, I modified the settings for all three programs (Table). The phaco representative visited my surgery center to observe my technique on the WhiteStar Signature System during a full morning of cases. Afterward, we implemented changes to improve my efficiency and keep the fluidics in the anterior chamber even more stable.
I used the new settings for about 1 month to understand the nuances of how the device was performing in all types of cases and situations. After that, the representative returned for some final tweaks based on my feedback. Overall, I was surprised at how many changes we made to what I thought were already satisfactory settings. In general, my new settings rely more on peristaltic ultrasound for the dense and slow-motion cases, but I use venturi for standard cases and for a portion of the I/A in all cases. One of the elements of the WhiteStar phaco system that I particularly like is the ability to use both pump styles within a single case so that I can minimize the disadvantages and maximize the benefits of each pump for my technique.
CONCLUSION
Although I provide my updated settings here for educational purposes (Table), the process of establishing and modifying settings is highly individualized and will vary based on each surgeon’s techniques. The adjustments I made were subtle but, taken together, have made me a more efficient surgeon. Nuclear disassembly goes faster—but not recklessly fast—and I have noted that the anterior chamber is more stable. Change is never easy, but when it enables me to capitalize on others’ expertise to provide safer surgery and better outcomes for my patients, it is certainly worthwhile. n
Click to view larger image in new tab
Cynthia Matossian, MD
• founder and CEO of Matossian Eye Associates in Doylestown, Pennsylvania, with additional locations in New Jersey
• clinical instructor, Department of Ophthalmology, School of Medicine of Temple University, Philadelphia
• cmatossian@matossianeye.com
• financial interest: consultant to Abbott Medical Optics