
Many patients with symptomatic presbyopia do not fit cleanly into traditional diagnostic categories, including the dysfunctional lens syndrome classification system.1 These patients may report subtle complaints or less common quality-of-life frustrations, and some may not mention symptoms unless asked directly. Asthenopia is a symptom that has an evolving role in these less typical presentations, beyond age-related declines in near vision. Notably, whether volunteered or elicited, these complaints are often reported in younger, prepresbyopic patients.
A classic example is the younger individuals with moderate to high hyperopia. With an appropriate workup, cycloplegic refraction often reveals clinically meaningful latent hyperopia. When asked specifically about eye strain or fatigue at the end of the day, many patients acknowledge the symptom—sometimes with visible relief—because it may be the first time they have discussed it.
In this setting, asthenopia is primarily accommodative. A younger hyperopic patient must accommodate to see clearly at distance, often by using a substantial portion of accommodative effort. When the patient shifts to near work, the additional accommodative demand may exceed the remaining reserve, contributing to difficulty with reading vision. After sustained accommodative overuse—particularly with prolonged computer work—patients may report eye fatigue. Figure 1 may help visualize this mechanism. Figure 2 shows how age-related loss of accommodation can unmask latent hyperopia, contributing to asthenopia and presbyopic symptoms.
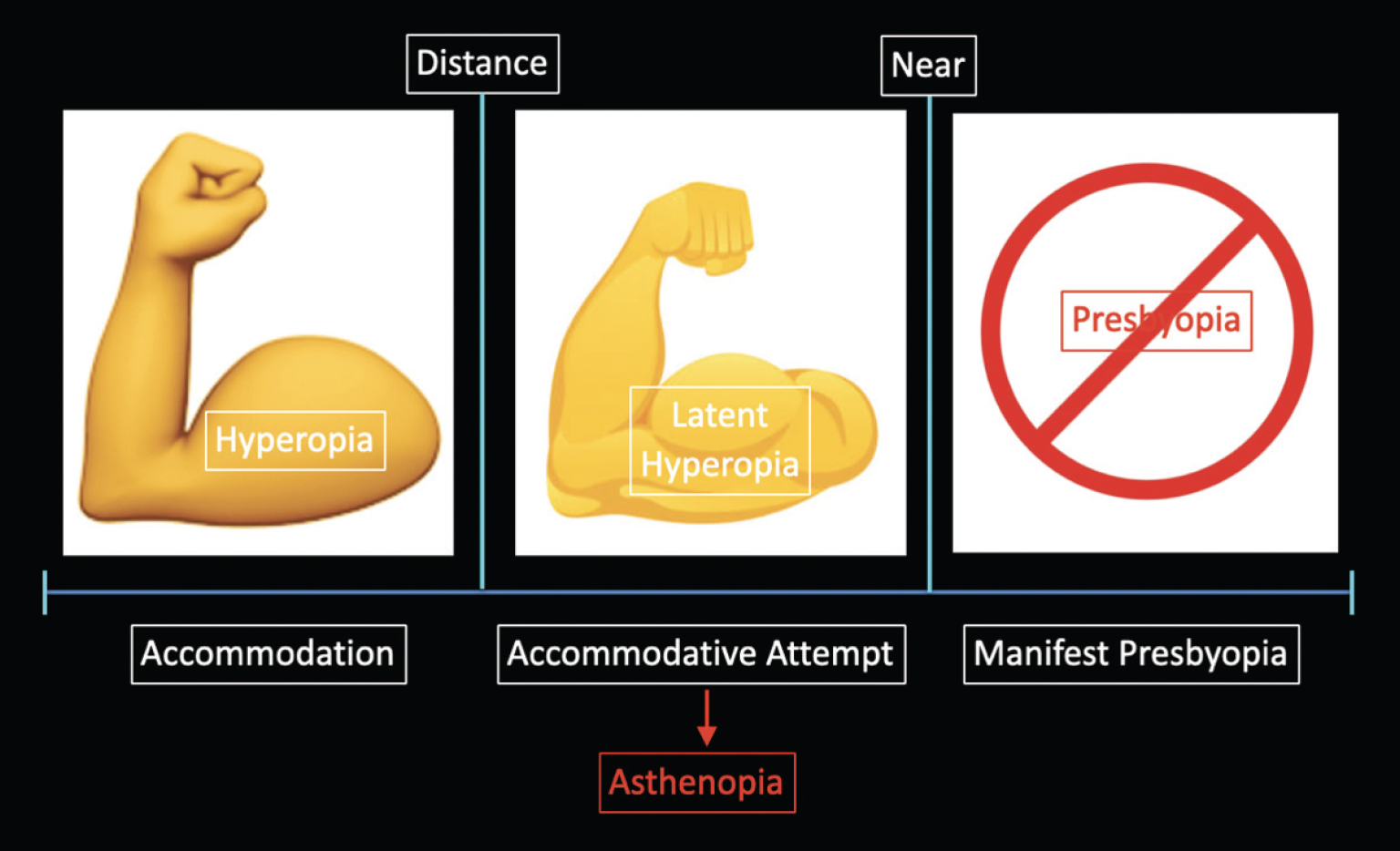
Figure 1. Latent hyperopia increases accommodative demand, reducing reserve and contributing to asthenopia and earlier presbyopic symptoms.

Figure 2. Manifest versus latent hyperopia: age-related loss of accommodation can unmask latent hyperopia, leading to asthenopia and presbyopia.
With that context, I turn to the “what”: the most appropriate solution for the younger patient with latent hyperopia who presents for surgical vision correction. Many of these patients are intolerant of either contact lenses or high-plus spectacles.
In this edition’s editorial, I explore the concept of earlier intervention with lens-based procedures. In parallel with advances in diagnostics and more reliable refractive lens exchange workflows—including laser-assisted steps, improved presbyopia-correcting IOL technology, and in-office procedures—many practices have become more comfortable offering earlier lens-based intervention for symptomatic presbyopia. The clinical question is increasingly less “Is intervention premature?” and more “Relative to what threshold of dysfunction—and over what time horizon?”
Figure 3 places latent hyperopia within the dysfunctional lens syndrome framework and highlights the lens–ciliary body complex as a driver of symptoms—context that informs the cornea-versus-lens decision.
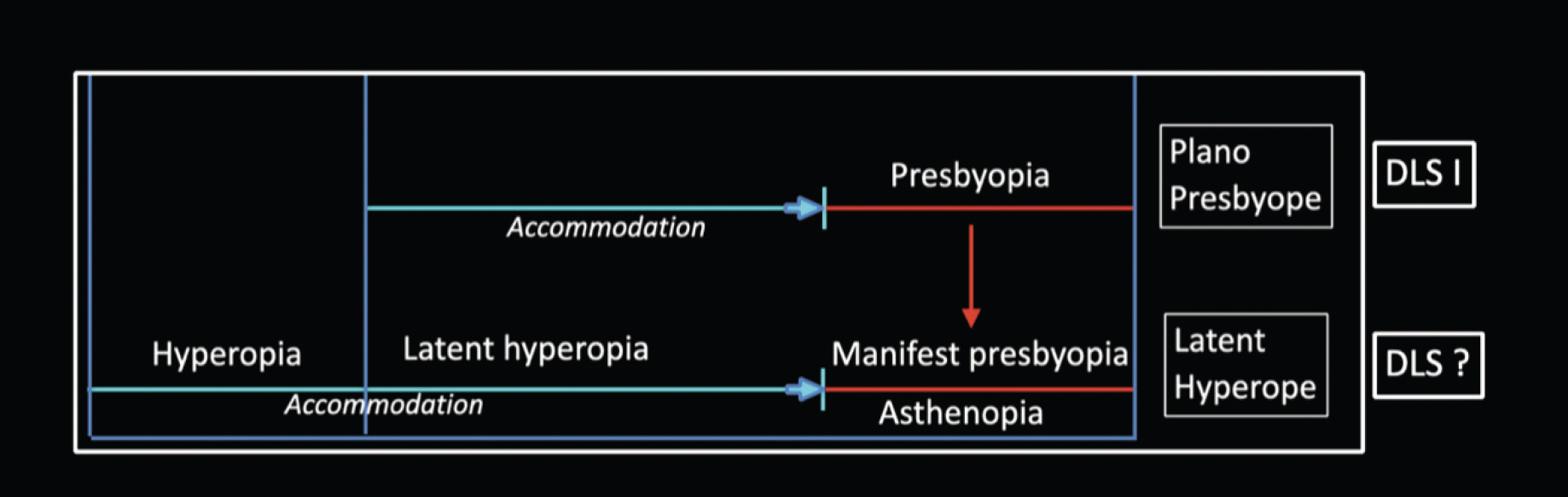
Figure 3. Latent hyperopia within dysfunctional lens syndrome, emphasizing the lens–ciliary body complex as a driver of symptoms.
THE CORE DECISION: THE CORNEA OR THE LENS
LASIK remains an option for select individuals, but long-term refractive stability can be limited in many hyperopic individuals. Hyperopic ablations may regress, and that regression can overlap with progressive loss of accommodation over time—what William F. Wiley, MD, has described as a two-hit process: postoperative epithelial remodeling and refractive regression on one axis, with progressive accommodative decline on the other.
Additionally, the hyperprolate optical profile after hyperopic LASIK can induce clinically meaningful negative spherical aberration when treating higher degrees of hyperopia, particularly when latent hyperopia is included in the treatment plan. These corneal changes may influence subsequent lens-based options; specifically, a hyperprolate corneal profile may reduce opportunities for presbyopia-correcting IOL strategies later.
BINOCULARITY DRIVES PERFORMANCE— AND SURGICAL PLANNING
In my practice, patients tend to achieve the highest satisfaction with binocularity. Binocular summation may improve both quantity and quality of vision (ie, Snellen visual acuity and contrast sensitivity function) when compared with anisometropia. I have also found patient satisfaction to be higher with immediately sequential bilateral procedures when appropriate.
In select individuals presenting for vision correction—particularly those intolerant of contact lenses—I have increasingly moved to immediately sequential bilateral refractive lens exchange with a presbyopia-correcting IOL as the primary intervention.
COUNSELING AND CONSENT
These clinical scenarios are decided case by case and require careful discussion of risks and benefits, thorough informed consent, and documentation. In my practice, multiple visits are often scheduled, and patients are encouraged to bring family members to support decision-making. In my experience, lens-based procedures have been a more refractively durable solution for this potential phenotype of lens dysfunction: latent hyperopia.
1. Waring GO IV, Rocha KM. Characterization of the dysfunctional lens syndrome and a review of the literature. Curr Ophthalmol Rep. 2018;6(4):249-255.




