

Presbyopia is profoundly frustrating for patients. This age-related condition manifests as a progressive loss of accommodation that impairs their near and intermediate visual acuity. Patients may strain to read and may experience intermittently blurry distance vision due to accommodative spasm. They also find themselves increasingly reliant on optical aids and other work-arounds to perform everyday tasks—challenges that can substantially erode their quality of life.
Refractive lens exchange (RLE) has emerged as a highly effective intervention for the majority of suitable presbyopic patients. The procedure can substantially reduce the spectacle dependence of appropriately selected candidates and enhance their visual function across all distances.
In our practice, RLE consistently yields high patient satisfaction rates. The procedure not only corrects presbyopia, but it also preempts future cataract development, making RLE a comprehensive, long-term solution.
There is, however, a presbyopic gray zone inhabited by patients who have excellent corrected distance visual acuity, no cataracts, and increasing difficulty with their near visual acuity. Achieving optimal outcomes in these individuals requires meticulous patient selection, a thorough preoperative evaluation, and precise expectation alignment. Unlike cataract surgery, which typically delivers unequivocal visual gains by removing an opacified crystalline lens, RLE replaces a functional (albeit aging) lens with an IOL, thereby introducing potential optical trade-offs. Nonetheless, with contemporary IOL technologies, including multifocal and extended depth of focus (EDOF) designs, RLE performs remarkably well for most patients.
In our experience, the key to success in the presbyopic gray zone is to prioritize functional improvements, such as seamless transitions between distance, intermediate, and near vision. Framing RLE as a way to enhance patients’ quality of life rather than as a panacea can transform potentially challenging cases into reliably rewarding ones.
PATIENT SELECTION
Ideal Candidates
Presbyopic patients with hyperopia or high myopia are ideal candidates for RLE. Their preoperative dependence on optical correction at multiple distances predisposes them to immediately appreciate postoperative gains in image quality and overall spectacle independence.
The Gray Zone
We have found that RLE can be successful in the presbyopic gray zone with targeted counseling and personalized planning (Figure 1).
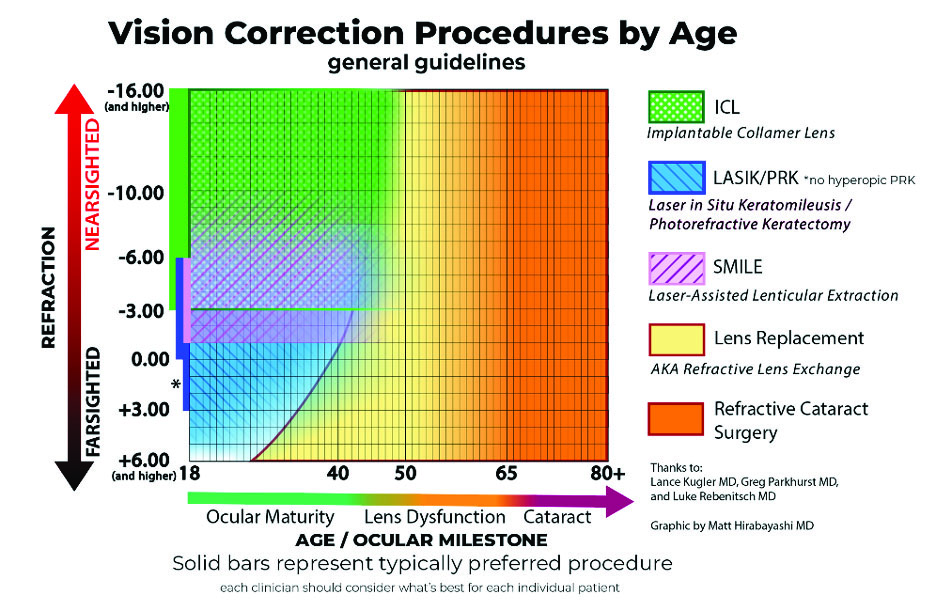
Figure 1. Visual guide for vision correction procedures by age and refraction. Reproduced with permission from Hirabayashi M et al.1

Figure 2. Intraoperative photograph of a multifocal IOL in situ.
Low myopia. Presbyopic patients with low myopia often underappreciate their uncorrected near visual acuity until the effect of improving their uncorrected distance visual acuity is demonstrated. Advanced technology IOLs are designed to optimize overall visual performance by balancing distance clarity with functional near vision. During counseling, we emphasize that, although near vision dynamics may shift postoperatively, the net gain in spectacle independence can outweigh this adjustment for motivated patients.
Emmetropic presbyopia. Patients who present with 20/20 uncorrected distance visual acuity and seek RLE solely to correct their presbyopia can be challenging to manage. In our experience, these patients thrive when we emphasize realistic functional endpoints preoperatively.
Younger patients. Individuals in their early 40s whose presbyopia is mild and whose crystalline lenses retain some flexibility are generally better served by alternatives to RLE. We have found that a blended vision strategy with procedures such as LASIK, keratorefractive lenticule extraction, and phakic IOL implantation can mitigate presbyopic symptoms while preserving accommodation. RLE can be reserved for when their presbyopia advances or cataracts develop.
OCULAR HEALTH AND HISTORY: ENSURING A SOLID FOUNDATION
Preoperative optimization of the ocular surface is imperative for successful RLE. Comorbid age-related conditions such as dry eye disease, Salzmann nodular degeneration, and epithelial basement membrane dystrophy can compromise both biometric accuracy and postoperative visual quality.
Irregular astigmatism, prior radial keratotomy, macular pathology, and glaucoma necessitate careful IOL selection or, in some instances, alternative refractive strategies. A comprehensive anterior and posterior segment evaluation is essential. We often avoid multifocal optics in these patients; monofocal and EDOF IOLs are more tolerant and help minimize dysphotopsias.
EXPECTATION MANAGEMENT: THE CORNERSTONE OF SUCCESS
Expectation management remains the main determinant of RLE success in the presbyopic gray zone. We discuss the potential trade-offs of current technologies at length and frame the goals of surgery around targeted reductions in spectacle dependence. We emphasize to patients that their UCVA will not be perfect at every distance. One practical technique we use is to ask patients, “In what situations do glasses hinder you most?” Their answers help us tailor preoperative counseling and set realistic expectations.
We also strive to normalize transient glare, halos, and the occasional need for low-powered readers in dim lighting conditions as expectations after rather than complications of presbyopia-correcting IOL implantation. We often say, “Multifocal IOLs maximize spectacle independence. Most patients achieve this the majority of the time, though specific scenarios like reading small text or low-light tasks might benefit from adjuncts like extra illumination or minimal magnification.” This transparency builds trust and facilitates neural adaptation.
Additionally, we have found personality assessments to be invaluable. The brains of flexible patients typically adapt readily to visual changes. In contrast, perfectionists, analytical engineers, and individuals who fixate on minor imperfections merit extended chair time or a deferral if their expectations remain unrealistic. For the latter group, recommending alternatives can prevent dissatisfaction and preserve rapport.
Finally, we routinely offer loose lens simulations to gauge patient tolerance and preferences.
ENHANCEMENT STRATEGIES: PROACTIVE PLANNING
Even with state-of-the-art biometry formulas and diagnostics, refractive surprises can occur. For this reason, we preoperatively discuss enhancement procedures as routine components of the refractive journey. Strategies include laser vision correction, piggyback IOL implantation for residual refractive error, and IOL exchanges in certain situations.
Reassuring patients that enhancements reflect our commitment to excellence is essential. We regularly tell them, “We will optimize your vision to support you throughout the process.” This mindset helps normalize refinements and sustain a high level of satisfaction when enhancements are needed.
An AI language model (ChatGPT 5.2, OpenAI) was used to assist with language editing. All content was reviewed, verified, and revised by the authors, who assume full responsibility for the accuracy and integrity of the manuscript. The AI tool was not used for data analysis, interpretation, or drawing scientific conclusions.
1. Hirabayashi M, Nasser T, Parkhurst G. Vision Correction: Introduction to Modern Refractive Surgery. 2nd ed. KDP; 2025.




