CASE PRESENTATION
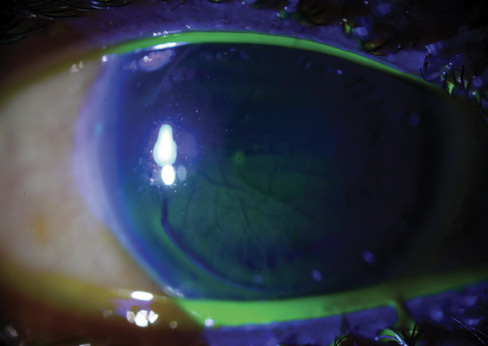
Figure 1. Macrostriae and a large inferior gutter in the left eye.
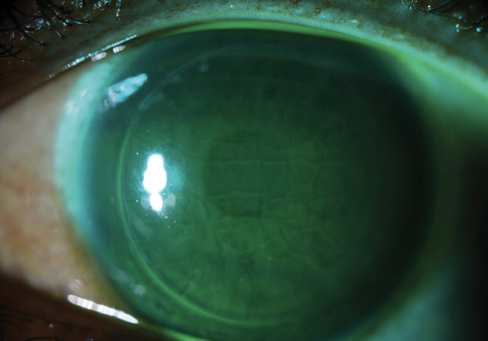
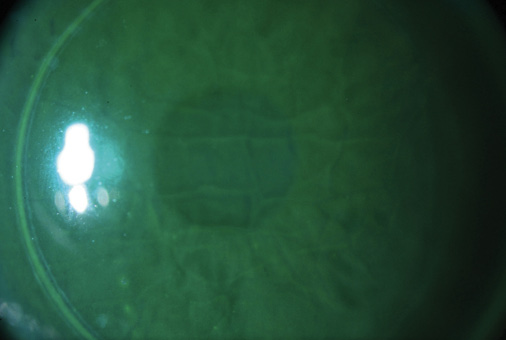
Figure 2. Fluorescein highlights the extent of flap striae (top, bottom) in the left eye.
— Section Editor Alan N. Carlson, MD

Jorge L. Alió, MD, PhD, FEBOphth
In cases such as this one, especially if the macrostriae appear a couple of weeks after surgery or if the patient is referred to me at that point, I relift the flap and administer drops of deionized, hypotonic, distilled water to the stromal face of the LASIK flap until it curves like a papyrus scroll. The change signals that edema is stretching the collagen fibers to the point at which the natural elasticity of Bowman membrane makes the edges of the elevated flap curve. Not only does hyperhydration of the flap stroma loosen the collagen fibers, which retract and thus create the folding, but it also partially detaches the epithelium that is partly responsible for the macrostriae. Next, I reposition the flap and gently flatten it with a rounded cannula by rubbing the tissue from the hinge to the opposite side. The striae will still be visible as I place a bandage contact lens. The patient is then discharged and scheduled for a follow-up visit in 48 hours. He or she is advised to expect blurry vision from flap edema during the first 7 to 10 days after surgery. The contact lens remains in place for at least 1 week because the flap may be loose while edema persists. The patient uses a steroid and an antibiotic drop for 7 days or until the bandage contact lens is removed. He or she uses a hyaluronic acid lubricant for a month or more after surgery.
I have used this technique in hundreds of cases and have never seen a relapse or complication.1 In 99% of cases, the approach will eliminate the folds, and I have found it effective for macrostriae that have been present for up to 1 year. Beyond that duration, especially if I detect epithelial ingrowth along with striae, I prefer to place seven radial sutures in order to keep the flap well attached and to avoid a recurrence of both striae and epithelial ingrowth. In such cases, I leave the sutures and contact lens in place for 10 days to encourage appropriate attachment of the flap to the stromal bed and to avoid recurrent epithelial ingrowth through the previous fistula.

Louis Probst, MD
The history of this case is unusual. Although macrostriae can develop in one eye after LASIK, its occurrence in both eyes is rare. To have two subsequent unsuccessful treatments of the macrostriae in both eyes is also very rare. After performing only refractive surgical procedures for more than 20 years, I have never found myself in this situation. Five months after surgery, the cracked-glass appearance resembles the sequelae of grade 4 diffuse lamellar keratitis. A second potential source of this outcome could be extremely thin LASIK flaps; a third could be the repeated lift attempts without sufficient flap smoothing. Regardless of the etiology, the outcome is so atypical as to require caution.
My approach would be the same no matter the source of the macrostriae. I would wait for refractive stability. If the refractive outcome had not improved, I would perform transepithelial phototherapeutic keratectomy and PRK on one eye at a time. The surface transepithelial phototherapeutic keratectomy treatment would smooth the corneal irregularities, which should improve the patient’s BCVA. PRK should improve his UCVA. I would not try to lift the flaps because they have likely scarred down from diffuse lamellar keratitis and previous lifts, because they may be thin and fragile, and because the risk of epithelial ingrowth after a fourth procedure would be extremely high. Depending on the corneal topography, I would consider using topography-guided PRK to address any irregularities. Finally, I would administer 0.02% mitomycin C for a full minute following the laser treatment to address the risk of haze after multiple procedures. I would proceed with surgery on the second eye only after a satisfactory outcome had been achieved in the first.

Rick Wolfe, FRACS, FRANZCO
In this case, the large striae visible in negative fluorescein staining are associated with a gap at the flap’s edge, which the epithelium has not completely filled. It is clear that the macrostriae will not resolve unless the gap is eliminated.
The usual strategies for smoothing the flap have not worked, and epithelial damage has presumably led to epithelial ingrowth. I would treat the worse eye first and suture the flap under the laser microscope. The procedure can be an ordeal for both the patient and the surgeon, so peribulbar anesthesia and sedation are options.
I would make multiple radial marks for alignment of the flap and the suture. I would lift the flap while keeping the epithelium intact. After carefully moving a rim of epithelium filling the gap back off the bed, I would administer a few drops of water for injection to the underside of the flap. Next, I would tighten a 360º antitorque suture and bury the knot. Flap mobility is a challenge. Although I have not used it, Mackool’s technique of progressive flap lifting might be of help.2 The sutures would remain in place for at least 3 weeks, after which the patient’s residual refractive error could be corrected in the usual way.
Prevention is most important. I have seen reports that a meticulous positioning technique is integral to preventing striae, but I think that is the problem rather than the solution. Edema and manipulation of the flap after bed adhesion are possibly responsible for striae. The flap needs minimal brief interface irrigation, followed by accurate positioning of marks. The speculum may then be removed. The surgeon should perform a slit-lamp examination and immediately attend to any problems.

What I Did: Alan N. Carlson, MD
I appreciate the diversity in treatment options offered by three of the most experienced LASIK surgeons in the world. My therapeutic approach was most similar to that recommended by Dr. Wolfe. I treated the patient’s left eye. I surgically lifted the flap under the microscope, debrided the epithelium covering the large gutter, and sutured the flap (Figure 3). My preference for these procedures is a 10-0 black nylon suture on a TG160-4 needle. The fine needle makes burying the knot difficult, so I have patients wear a bandage soft contact lens (usually with an 8.8-mm base curve) for a few days. In this particular case, the epithelium sloughed off spontaneously during suturing, and I was careful to keep it from becoming trapped under the flap. I find that placing the first suture farthest from the hinge—with subsequent sutures sequentially closer to the hinge—optimizes the tension for proper redistribution of tissue. I generally remove the sutures 2 to 3 weeks after surgery in these cases.
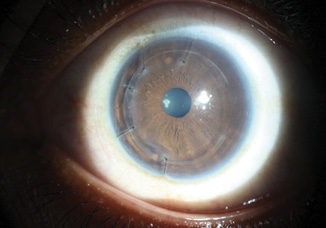
Figure 3. Sutured LASIK flap with bandage soft contact lens.
Although this patient is still healing, he is already completely comfortable and has crisp 20/20+ UCVA. He is still deciding whether he wants to undergo surgical correction of his contralateral eye, the visual quality of which is only moderately debilitating.
1. Steinert RF, Alio del Barrio JL. Prevention and management of flap striae after LASIK. In: Alio JL, Azar DT, eds. Management of Complications in Refractive Surgery. 2nd ed. Cham, Switzerland: Springer International; 2018:75-82.
2. Mackool RJ, Monsanto VR. Sequential lift and suture technique for post-LASIK corneal striae. J Cataract Refract Surg. 2003;29(4):785-787.




