
By all indications, 2011 was starting off well. My practice was growing, my patients were happy, and I was enjoying life in the Ozarks with my lovely wife Debbie. There was plenty of promise and opportunity ahead. We had recently received a US Department of Defense (DoD) research grant to develop nanofiber drug delivery for the US military, which my team had been working very hard to secure. When I landed in Aspen, Colorado, in late February to deliver my first-ever Aspen Corneal Society lecture, I saw warm sun, fresh powder, and blue skies; I truly felt a great future lay ahead.
They say it happens so fast. It no doubt did, but for me, 7 years later, I still can remember most of the fall in full detail, frame by frame. I had decided to break off from my friends, all ophthalmologists and their families, and ski down to the hotel to prepare for my talk. I felt that it was truly earth-shattering information that had to be shared with the brightest in the cornea world. If I didn’t make this lecture perfect, how would they know how to rapidly detect adenovirus in their pink eye patients?
Against a chorus of Wimp! and One more run! I jumped on an easy blue cruiser called the Coffee Pot and headed for the hotel. I recall hearing a distinct rifle shot, then feeling white nuclear pain, while suddenly noticing that one ski was pointing downhill and the other was turned more than 90° and behind me. My last thought was, “This is no way to ski.”
As I woke up sliding headfirst on my back in a ski patrol toboggan, I immediately thought, “How humiliating!” Keeping a cool demeanor, I asked Stan the ski patrolman which run we were taking because I wanted to come back and ski it later. “You won’t be skiing this ever,” he said solemnly. I thought to myself, “This must be a bit more than a torn ACL.”
Dude, that is GNARLY
The ER doctor filled me in. I was found by an English couple, unconscious and hypotensive in fresh snow; apparently, I had been there for a while. The radiology technician put it bluntly: “Dude, that is a gnarly looking leg!” I was given an appointment to meet an orthopedic surgeon in the morning for urgent surgery, and no, I could not fly home and get it taken care of by the orthopedic surgeons at my familiar Mercy Clinic.
William B. Trattler, MD, came to the ER and gave me one of his shoes, and he hopped and I crutched on ice over to the meeting (Figure 1). Loaded with pain meds, I did in fact give my lecture on pink eye. We had a great meal, and everyone honored my need to be nil per os after midnight. Carlos Buznego, MD, was designated my bodyguard; he would get me to the hospital in the morning (Figure 2).

Figure 1. A sign made by William B. Trattler, MD, before he escorted Dr. Tauber to his lecture on pink eye.
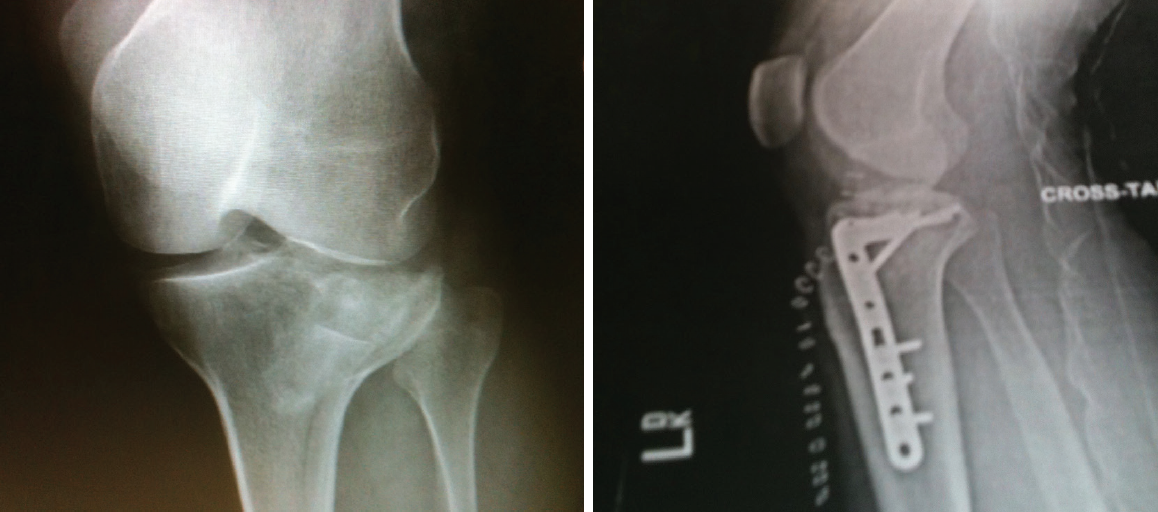
Figure 2. Pre- (left) and postoperative (right) x-rays of Dr. Tauber’s leg.
SWEET DREAMS, BUT …
As I drifted off to sleep my thoughts were simple: Surgery the next day, and I would soon be sitting by the fire with a nice brandy, a St. Bernard at my feet, surrounded by my friends who had arrived for the beginning of the American-European College of Ophthalmic Surgeons (AECOS) meeting.
It was not to happen. I woke up in the ICU with a fat embolism in my lung, trying to catch my breath despite 10 L/min of oxygen blowing into me like a windstorm. Panic set in as I realized that things were not going well.
No St. Bernard, no fireplace, no brandy. But I was surrounded by friends from the AECOS meeting. They came to visit at all times of the day and night, to the chagrin of the nursing staff. Fortunately, none of their aggressive suggestions for the constipation I was experiencing were undertaken by these lovely nurses.
The rules were laid out for me: Six months with zero weight bearing. I would need to learn how to get around my house, how to get in and out of a car, how to use the toilet (Figure 3). I was told physical therapy (PT) was crucial, but not to expect full recovery. Sadly, the ski patrolman was right.

Figure 3. Equipment arrives to help Dr. Tauber adjust to his new life.
BACK HOME AGAIN
I made it home to Springfield, Missouri, 5 days after surgery with the help of many friends. They arranged to get my gear, including my computer with the all-important pink eye lecture, home safely.
The look on Debbie’s face when I was dropped off at home that night said it all. How are we going to get through this? Why didn’t we buy a house with a full bathroom on the ground floor? Where was the disability policy?
I had spent 5 long days in Colorado preparing for this meeting with my wife, and I thought I had all the answers. With a brave face, she heard me mumble, “We got this, Debbie girl.”
That night I fell into a deep sleep in a chair in my home office, my wife sleeping upstairs with the dogs. I had no idea what I was doing or what was about to happen.
A LONG ROAD
Five months is a long time not to put your left foot on the ground. My body went through some shocking changes as my left leg quickly lost most of its muscle mass. I was rushed to the ER with a possible pulmonary embolism, which fortunately was ruled out. My abdomen became one big welt as I injected enoxaparin sodium (Lovenox; Sanofi-Aventis US) twice a day.
The mental challenge was worse. The OR nurse supervisor banned me from the OR because I couldn’t use crutches without being a risk to the patients, the staff, and myself. Trying to examine patients at the slit lamp with an indirect ophthalmoscope required two feet on the ground. Taking calls in a Level 1 trauma center was out of the question.
My life was altered. I was letting down patients and partners, my leg was melting away, and the twice-daily injections were torture. I couldn’t take a shower in the house because we had none on the ground floor. I was sleeping in a rented hospital bed and getting hosed off in the garage, which fortunately had hot water.
GETTING WITH THE PROGRAM
PT was painful and long. Early on, I hated PT. I watched nice little old ladies come and go every 6 weeks with their total knee replacements, smiling and ready to dance when therapy was over. Meanwhile I just watched and waited for my leg to mend.
Over time, however, I grew to cherish my time in PT (Figure 4). The staff members were incredibly dedicated and creative as they helped me to build up a leg that couldn’t touch the ground. I told them I wanted to try out for Dancing With the Stars in August, and they took it as a personal challenge.
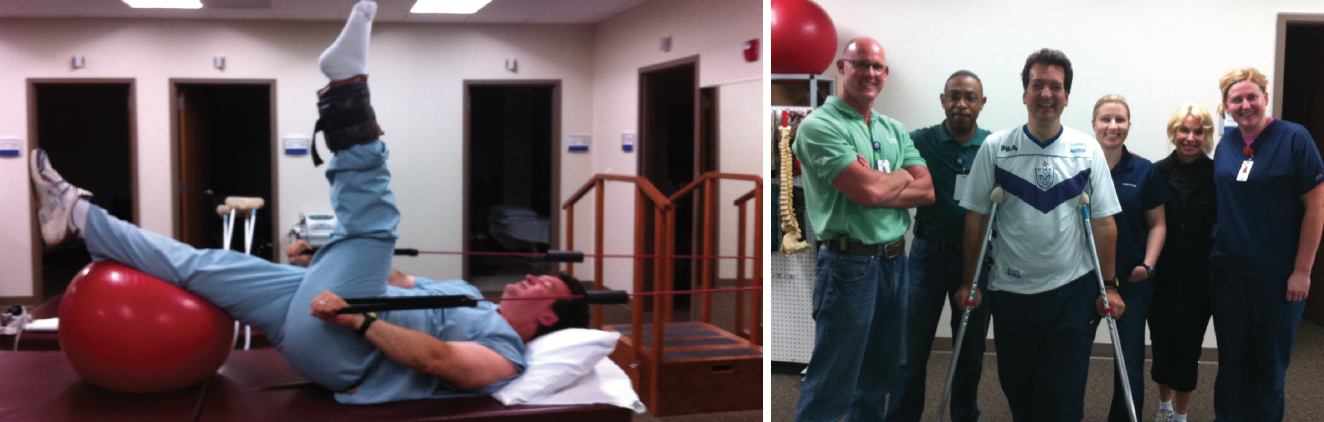
Figure 4. Photos of Dr. Tauber at rehab (left) and with PT staff (right).
At the end of PT sessions, while I was icing my leg, my optometrist, Alison L. Hood-Kirar, OD, would come in with stacks of charts and photos. She did a fantastic job managing our patients with corneal ulcers, failed grafts, glaucoma, and retinal issues. I began to look forward to these interactions with Dr. Hood, as she shared with me how she was managing our patients. She had great support from my brother, Joseph Tauber, MD, of the Tauber Eye Center in Kansas City, Missouri, and my dear friend Gregg J. Berdy, MD, FACS, of Ophthalmology Associates in St. Louis.
Not to be overlooked, there was a great shower at the end of each PT session. Within a month, I stopped crying in pain and anguish in the shower stall.
STAYING WITH IT
Without a schedule for clinic and surgery, it was easy to get bored. I learned that there are only four plot twists on Judge Judy.
I knew that, if I was going to make a comeback as a physician, it would require stimulating my brain, busting my ass in PT, and keeping myself relevant to my partners and to the field of ophthalmology. I vowed not to express to Debbie, my friends, and my family the despair, loneliness, and uncertainty I felt during this period. Somehow, I vowed, I would be strong.
It would not have been possible to remain current in ophthalmology without the friends who periodically checked in on me. I am grateful for my good friends Guy M. Kezirian, MD, MBA, FACS; Karl G. Stonecipher, MD; and Steven D. Vold, MD, who encouraged me with their late-night calls. They and others lifted my spirits and helped me develop a strategy to stay engaged in the profession.
A new eye organization, the Cornea, External Disease, and Refractive Society (CEDARS) was forming at the time, and the phone calls we made to discuss its formation were fun and full of promise. I also had the time and freedom to explore, with my partners and my colleagues around the world, the new concept of laser cataract surgery. It was during those quiet moments, while others were busy with their lives, that I developed the idea of Femto for All (see An Idea is Born below).
AN IDEA IS BORN
“ If a prudent, cautious beginning is made, there is every prospect of success.”
– Sister Catherine McAuley
In 2009, Douglas Katsev, MD, introduced me to the work of Zoltan Z. Nagy, MD, PhD, DSc, on laser cataract surgery. Needless to say, I was intrigued. With the blessing of James A. Gessler, MD, our section chair at Mercy Hospital Springfield, I began to pursue the use of the femtosecond laser in cataract surgery. In my work, I met Mark Forchette, who at the time was president and CEO of Optimedica (later acquired by Abbott Medical Optics; now Johnson & Johnson Vision). He introduced me to a formidable group of ophthalmologists in and around Sunnyvale, California, who were all interested in performing laser cataract surgery.
By the time I arrived in Aspen in 2011, we had developed a good fund of knowledge on the current state of the technology. Our group was eager to develop a realistic plan to participate in this arena, and we were excited about the technology and its possibilities to improve cataract surgery for our patients. But we also recognized the daunting financial burden that providing this care would entail.
I was deeply inspired by the passion of my partners to offer the best for our patients. Our administrators at Mercy did not reject the notion of laser cataract surgery, but they were skeptical that it could be offered.
While recovering from my skiing injury, I found myself with a little bit of extra time and headspace. Armed with the burgeoning science and the passion of our group and instilled with the mission and history of Sister Catherine McAuley, foundress of Mercy, I set out to find a way to offer femtosecond laser technology to all our patients. Many conversatations and visits with senior leaders at Optimedica and Abbott followed.
By the time of the AECOS summer meeting in Park City, Utah, we had devised a rudimentary model to offer the femtosecond laser to all our patients undergoing cataract surgery. This February marked 5 years since we started the Femto for All patients program. Our group is proud of the success and contributions we have made to our patients and our colleagues. Our relationship with our administrators and with Johnson & Johnson Vision and Carl Zeiss Meditec is strong, ethical, and full of promise.
The research grant kept me busy, and I looked forward to those teleconferences, the lab meetings with the cornea wound repair team, and the fantastic team at the DoD. We met all the proposed goals on time and on budget. I am proud of that work and the patents we received as a result.
Slowly, physical progress was also made. I could bend my knee, the compression hose came off, and, finally, my left foot touched the ground. Bradley H. Walz, MD, my orthopedist at Mercy, asked, “Do you want to try to walk?” Heck yes I did! That night I asked Debbie to walk with me and our dogs to the mailbox. Freedom was so sweet.
BACK TO WORK
By August, it was time to go back to work. Questions lingered. Would I remember how to do eye surgery, or had I lost my dexterity? Thankfully, I found that it was right there where I left it 6 months before. After a few nights practicing suturing and other skills in an empty OR, my confidence returned (Figures 5 and 6).

Figure 5. Dr. Tauber’s first day back in surgery after his skiing accident.

Figure 6. Dr. Tauber relaxing at home after a long day of surgery.
How sweet it was to return to the profession I loved. I never did get to audition for Dancing With the Stars, and I have not had the nerve to try downhill skiing again. Watching it today, televised from the PyeongChang 2018 Olympic Winter Games, brings pangs of jealousy, even though I was never gifted enough to ski at that level.
As I reflect on the journey, I am thankful that I am healthy and that I have the unconditional love of my beautiful wife (Figure 7) and can enjoy a robust and invigorating professional and personal life.

Figure 7. Dr. Tauber and his wife Debbie, hiking in Deer Valley during the 2011 AECOS summer meeting in Park City, Utah.
While skiing in February 2011, I shattered my leg doing something I had truly loved since I was 4 years old. It happened for a reason that I am still learning about. I have come out the other side much better off. Yet there are things I have learned from this debacle:
No. 1: The kindness of strangers is best appreciated while seated in a wheelchair. The 90-pound Ethiopian refugee who managed to wheel me and my gear through the Denver Airport will forever be remembered for her smile and good humor.
No. 2: You have been knocked down, not knocked out. You have family, friends, and colleagues who will root for you loudly and quietly. It is important that you do everything in your power not to let them down. I am very proud of the success of the Mercy Femto for All laser cataract program.
No. 3: Take the time to appreciate that your patients are praying for your recovery. I have kept each card that was sent to me (Figure 8).

Figure 8. A pile of cards and letters Dr. Tauber received from his patients.
No. 4: When the chips are down and you don’t know where to look for strength, search for your mentors. They will be there.




