In a society obsessed with appearances, red eyes have a lot of negative connotations, including inebriation, sleep deprivation, and various forms of addiction. Americans’ vanity or self-consciousness about their appearance has resulted in the availability of a plethora of over-the-counter (OTC) remedies promising white eyes, fast (Figure 1). Consumers buy these products at an alarming rate, with more than 15 million bottles sold in the United States each year.1
The problem with the available red eye-reducing eye drops is that they contain a decongestant as the active ingredient for vasoconstriction. Naphazoline, tetrahydrozoline, and phenylephrine have relatively short durations of action and require frequent dosing, 1 to 2 drops up to four times daily.2
Soparkar and colleagues reported in 1997 that misuse of these OTC eye drops can lead to chronic conjunctivitis.3 Their study of 137 eyes demonstrated that, over the course of a median 3-year use cycle, OTC decongestant eye drops can produce both acute and chronic conjunctivitis, which can take several weeks to resolve.3 It is also well known to eye care professionals that the long-term use of these whitening agents can have a rebound effect, causing vasodilation and actually making the redness worse for the user.3 Some experience rebound effects; others experience tachyphylaxis, a rapid decrease in response to a drug after use.1
REDNESS A SIGNAL
The reality is that inflammation causes redness. If the cause of the inflammation is not identified, the healthy tissues of the eye can be harmed.
Redness or hyperemia, to an eye care professional, is a key sign of inflammation. It is one of the five clinical symptoms of inflammation, along with pain, edema, heat, and loss of function. We must remember that, to the patients we serve, however, redness is just an inconvenience and one that mars their appearance. They want a quick, easy solution; they have jobs to go to, lives to live, and contact lenses to wear.

Figure 1. US consumers buy more than more than 15 million bottles of OTC eye drops.
Our society has been trained to self-medicate before seeking medical attention. The shelves of our grocery and drug stores are overflowing with self-treatment options. OTC remedies such as Clear Eyes (naphazoline; Prestige Brands) and Visine (tetrahydrozoline; McNeil) are often half the price of doctor-recommended drops such as Refresh Tears (carboxymethylcellulose sodium; Allergan), Systane (polyethylene glycol; Alcon), Genteal (hydroxypropylmethylcellulose; Alcon), etc. Many OTC allergy eye drops also contain a red eye reducer.
UNCOVERING THE CAUSE
Getting a patient with a red eye in the door for the initial examination can be the biggest hurdle. Many patients will already have used one or more OTC eye drops by the time they are in your chair. Uncovering and successfully treating the true cause of the redness can be a challenge, but when you do, you have earned a patient for life.
History is always the first step. A thorough history can uncover much about the patient and his or her symptoms before the examination begins. Questionnaires can help to expedite the intake process; the Ocular Surface Disease Index (OSDI) and Standard Patient Evaluation of Eye Dryness (SPEED) are two commonly used, validated questionnaires. Many doctors have a questionnaire specifically personalized for their patient base and their experience of risk factors leading to ocular discomfort. It is fine to use a customized survey, or more than one, but the advantage of using a validated survey is that results are reproducible. Repeating the questionnaire can aid in determining whether treatments are relieving symptoms.
Environmental Causes
Occupation plays a big role in ocular surface wellness. Some professions have a higher risk for ocular surface disease and chronic redness. Pilots and flight attendants spend much of their days in low-humidity environments. Truck drivers are in small cabs with airflow either from the vents or a window down.
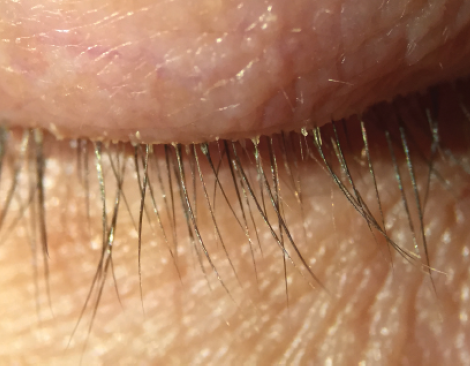
Figure 2. Many patients experience chronic inflammation and redness due to undiagnosed Demodex mites.
Despite decades of health warnings, many Americans continue to smoke cigarettes. The highest usage, 20.1%, is among people ages 25 to 44.4 Many states have legalized the medical use of marijuana. The smoke from either source is an ocular irritant. Little is known about the vapor from e-cigarettes, but this too is an irritant. Ask your smoking patients with which hand they hold their cigarette; often, the eye on that same side is the more symptomatic.
Alcohol consumption is another risk that should be discussed. Decreased tear breakup times have been noted with alcohol consumption compared with controls.5 Even hydration can be a cause. Many patients are likely in a chronic state of dehydration.
Ultraviolet light can be harmful to the eyes, causing the common condition of pinguecula. Patients with pinguecula often present for emergency examinationss, with the chief complaint of a “yellow bump” on the eye. This raised nodule appears on the conjunctiva in the nasal or temporal limbal area, the areas with most ultraviolet light exposure.6 Pingueculae can become inflamed due to surface dryness causing localized redness.
For many patients, applying makeup is a daily routine. Makeup products do not undergo FDA approval, and most are loaded with potential ocular irritants: pigments, dyes, and waxes, to name a few. These irritants are applied daily to the lid and lashes. Patients’ makeup removal process is another concern. If the makeup is not completely removed, the resins left behind encourage increased bacterial loads and possibly even Demodex growth.
Blink Rate
In the digital world, history should include how many hours the patient spends on digital devices daily: smartphones, tablets, computers, video games, e-readers, and now even smartwatches. Digital eyestrain is known to cause redness. Ask patients if they notice improvement of their redness on weekends or when they are on vacation.
Educate patients to follow the 20/20 rule: For every 20 minutes of screen time, take a 20-second break to focus at a distance and blink. Screen time reduces the blink rate, which leads to surface dryness and then redness. Blinking exercises help a great deal. Teach patients to open/shut/squeeze the lids for a count of 2 seconds/open and to repeat this process for 10 consecutive blinks at an hourly or even half-hourly interval.
Donald R. Korb, OD, has developed a smartphone app that patients can download for free (Donald Korb Blinking Exercise, available at iTunes.com) and set blinking reminders. This illustrates that sometimes the problem can also be a part of the solution.
This video shows makeup residue in the eye.
Contact Lenses
Inflammation associated with contact lens wear can be the result of mechanical trauma from a damaged lens or from a poorly fit lens. A tight-fitting contact lens that provides low oxygen flow can cause inflammation. Immunologic factors, introduced by poor cleaning and/or failure to replace lenses on a prescribed schedule, can also trigger a response.7
Medications
Treatments for ocular conditions can also be a cause of chronic redness. Glaucoma patients taking a prostaglandin analogue often have conjunctival hyperemia. Anecdotally, the incidence of this side effect has declined as lower concentrations with the same pressure-lowering ability but fewer unwanted side effects have been developed. Preservatives in prescription or OTC topical medications can also contribute to redness.
Chronic Causes
Examinations of the patient with a red eye should include a thorough evaluation for chronic ocular surface disease conditions: allergy, blepharitis, and dry eye disease (DED).
Start with the lids. Debris, specifically cylindrical debris, can suggest Demodex blepharitis. Grab your microscope and epilate a few lashes; it is amazing what is hiding in there. Since I started using a relatively inexpensive light-emitting diode microscope in my practice, I have found that many patients experience chronic inflammation and redness due to undiagnosed Demodex mites (Figure 2). In-office and at-home treatments are available to aid in reducing mite counts. Symptoms may be improved with tea tree oil-based products such as Cliradex (BioTissue) or an in-office treatment such as Oust Demodex Swabstix (OcuSoft).
Next, evaluate the palpebral conjunctiva, looking for papillary or follicular reaction. A papillary response is a common clinical finding for ocular allergies. Ask the patient if he or she has been formally tested for environmental allergies, and arrange for this testing if needed. Makeup or other localized allergens can also cause this type of response. A chronic follicular response can indicate toxic conjunctivitis from prolonged exposure to a preservative and/or active ingredients in OTC drops, especially if the drops have been abused.
Mucous fishing syndrome is another less common cause of chronic inflammation in patients. In this condition, the patient is bothered by ocular irritation and continuously and repetitively “fishes” for the foreign object, causing a large volume of tissue inflammation and mucous production.
Finally, evaluate the patient for DED with a slit-lamp examination and auxiliary testing when possible. Inflammation is an underlying cause of ocular surface disease, both aqueous-deficient and evaporative DED. All patients complaining of redness should have a thorough evaluation. Initiating proper treatment based on this examination will quell the inflammation and result in whiter eyes.
BE SKEPTICAL OF SURGICAL SOLUTIONS
Beware of eye-whitening surgeries, known as I-Brite or IsoWhite. Studies have found that removing the conjunctival tissue to whiten the eye carries the risk of delayed and serious complications, including impaired healing, infection, and scleral thinning.8
ON THE HORIZON
Bausch + Lomb is reportedly developing a product that may lead to faster, more effective, and longer-lasting treatment for ocular redness. This therapy will use a low dose of brimonidine tartrate to relieve ocular redness, a different mechanism of action from available products. There is little to no risk for rebound redness, according to the company. The biggest concern is for allergic reaction to the active ingredient. At the lower concentration, the risk for this seems to be low. The results have been dramatic. In patients at risk for angle closure, this is not a concern because brimonidine can constrict the pupil, unlike phenylephrine, which can cause pupillary dilation.
RAISING PUBLIC AWARENESS
Education is vital. Educate your community regarding the potential risks associated with OTC whitening agents and surgical procedures. Patients often seek advice from their local pharmacist; working with pharmacists may help get patients to your door sooner.
Educate patients of the importance of reducing screen time, drinking to stay hydrated, avoiding the sun and direct air flow when possible, and getting enough sleep. A healthy diet is also important.
Many patients may be motivated simply by vanity to reduce their ocular redness, but it is important they understand that simply masking the situation with drops is not the best approach. They could be masking an important symptom of a serious underlying problem. n
1. Abelson MB, Smith LM. Vasoconstrictors: myths and realities: the facts about how vasoconstrictors work and thoughts about mechanisms behind their purported negative side effects. Review of Ophthalmology. August 2012.
2. Bielory L, Katelaris CH, Lightman S, Maclerio RM. Treating the ocular component of allergic rhinoconjunctivitis and related eye disorders. Med Gen Med. 2007;9(3):35.
3. Soparkar CN, Wilhelmus KR, Koch DD, et al. Acute and chronic conjunctivitis duew to over-the-counter ophthalmic decongestants. Arch Ophthalmol. 1997;115(1):34-38.
4. Jamal A, Agaku IT, O’Connor E, et al. Current cigarette smoking among adults--United States, 2005-2013. MMWR Morb Mortal Wkly Rep. 2014;63(47):1108-1112.
5. Kim JH, Kim JH, Nam WH, et al. Oral alcohol administration disturbs tear film and ocular surface. Ophthalmology. 2012;119(5):965-971.
6. Panchapakesan J, Hourihan F, Mitchell P. Prevalence of pterygium and pinguecula: the Blue Mountains Eye Study. Aust N Z J Ophthalmol. 1998;26(suppl1):S2-5.
7. Suchecki JK, Donshik P, Ehlers WH. Contact lens complications. Ophthalmol Clin North Am. 2003;16(3):471-484.
8. Vo RC, Stafeeva K, Aldave AJ, et al. Complications related to a cosmetic eye-whitening procedure. Am J Ophthalmol. 2014;158(5):967-973.
Leslie E. O’Dell, OD
• director of the Dry Eye Center at Wheatlyn Eye Care, York, Pennsylvania
• helpmydryeyes@gmail.com; www.twitter.com/helpmydryeyes
• Financial disclosure: None acknowledged