Why efficiency matters, and how to get there.
Ashley Brissette, MD, MSc, FRCSC

Efficiency in the OR is important not only for utilization and case volume, but also for patient safety. As time of surgery increases, so may the risks of infection and complications. We also know that adverse events are diminished with increased surgical experience and overall surgical volume; therefore, it is important to operate as much as possible in order to continuously refine skills.
Create a Ritual
For me, my behavior in the OR has become a ritual. I attempt to perform my cataract surgeries with the exact same steps each time, making alterations only for case-specific requirements (eg, a posterior polar lens) that may require different techniques. A surgical mentor once told me, “First you get good. Then you get fast.” This adage could not hold more truth. Performing each step with precision and with efficiency of movement is achieved by performing the same steps of surgery in the same manner each and every time. I also try to make sure that the pre- and postoperative steps are the same. I prepare and drape in the same way, I put the bed at exactly hip height (this is ergonomically the most comfortable for me), and so on and so forth.
Optimize Your Teamwork
The team is so important to the flow in the OR as well, and this flow almost becomes a dance, with every team member performing his or her role precisely. Time in the OR is such an important part of our experience, and by simplifying all of the steps down to being done the exact same way each time, we have been able to achieve tremendous efficiency and safety in my OR.
Thinking through the entire surgical process can help you become faster—and better—in the OR.
Daniel H. Chang, MD

Providing high-quality care comes first, but achieving great outcomes in an efficient manner is also of utmost importance, particularly in a time of increasing expenses and declining reimbursements. When you look for ways to become more efficient, remember that your time in the eye is only a portion of the total time per case in cataract surgery—particularly for a small, one-room surgery center like mine. Remember, the clock doesn’t stop when the drape comes off.
TEAM MENTALITY
A desire to become faster should permeate one’s organization, and the key to becoming faster is teamwork. On any given surgery day, we have only seven staff members, one anesthetist, and one surgeon in our entire 1,236 ft2 facility. Each person has a clearly defined role, but each is also constantly looking to help others. At times, the anesthesiologist may wipe the surgical table while I change the bed sheet and the nurses move patients. Everybody is looking to pitch in, and we all do whatever it takes to keep the day moving efficiently. We try to eliminate choke points at any step or with any person so that the whole process moves forward smoothly.
POSITIONING THE PATIENT
Speed and efficiency in surgery come not from moving quickly, but in doing each step well the first time and setting things up for the next step. It’s getting the little things consistently right that optimizes efficiency. Making the incisions in just the right place, getting the capsulorhexis just right, taking advantage of both peristaltic and venturi fluidics at the right times are just a few key points.
The process begins with positioning the patient properly on the bed. One simple yet extremely important trick is to elevate the head of the bed by at least 15°, so that the operative eye is always the highest point of the body. My patients never lie flat in the OR. This means that patients with large chests and necks need even greater head elevation. By elevating the head of the bed, you not only improve ventilation, but you also reduce posterior pressure, improve exposure of the eye, and set up the rest of your case for success.
CONCLUSION
There is no a simple formula to becoming faster in the OR. The key to speed and efficiency is to have a mindset that is always searching for how to do things better, from where to place the preoperative prep gloves to how and when to place postoperative drops. Each surgeon can become faster when we build our team and work through optimizing each step of the whole surgery day. The best part is that, although it is important to be fast, optimizing efficiency typically results in both faster cases and better outcomes for our patients.
Increasing surgical volume requires strategy, planning, and flexibility to reengineer the system—often after several attempts.
Scott LaBorwit, MD

The key to increasing efficiency in the OR is for the surgeon to focus on making everything around him or her faster while doing everything during surgery in the same way, without rushing or speeding up. As my mentor told me, “Getting faster is what happens between your surgical steps.”
When I work with residents who look at the clock at the start of a case, I remind them: It took 60 years for this cataract to develop; let’s not worry about saving 3 or 5 minutes now.
If rushing doesn’t increase efficiency, what does? This article outlines some of the steps that my staff and I have taken to improve efficiency and boost surgical volume in our OR (see Top Tips to Create OR Efficiency).
Top Tips to Create OR Efficiency
1. Speed is created between surgical steps with strategic planning;
2. Staff involvement and buy-in is needed at all levels to assign tasks and create flow;
3. Train and delegate nonsurgical steps;
4. Minimize distractions and deviation from routines; and
5. Understand that flexibility and reengineering will be necessary.
Take a Field Trip
A first step you can take toward increasing your OR efficiency is to visit a surgery center that is doing significant volume. Make sure to take notes. You will see things that will work for you and other things that will not. Notice how effortless it seems for the staff to get through the day. No one is rushing, but each person has a specific job. Any effort to increase OR efficiency requires a team approach. Being able to explain to your staff the why of it creates their buy-in.
Allowing your staff to participate in developing a strategy is also critical to success. I always joke that I am the only one who gets to sit for the surgery, while everyone around me is running around getting us through the day.
Create and Delegate Routines
One way to achieve efficiency is to create an environment that allows the surgeon to begin operating within a minute of entering the OR and doing the time-out (Figure 1). To accomplish this goal in our OR, we have implemented several strategies outlined here.
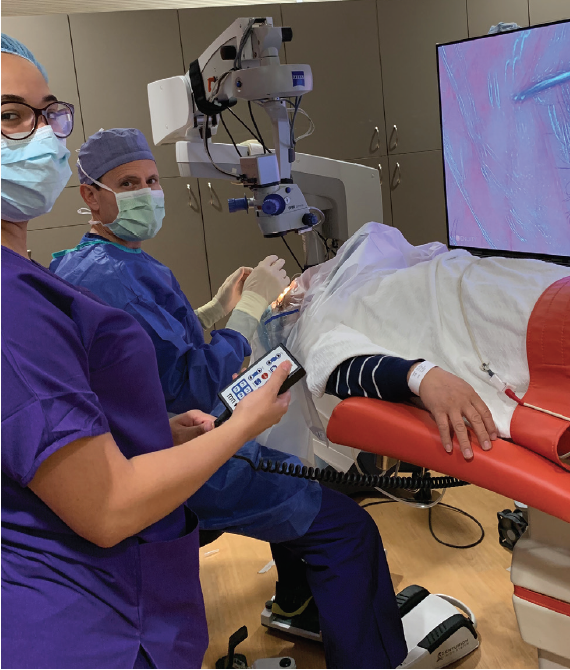
Figure 1. The surgeon should be able to start surgery within 1 minute of entering the OR. The floor is marked, the stretcher remote has memory to set the bed to the correct height, the circulating nurse has prepped the patient, and the scrub tech has draped the patient and placed the lid speculum.
In addition to marking the floor to line up the stretcher, I have operating chairs that have remote controls with saved settings. The nurses hit memory P3 on the remote so that, when I sit down, the patient’s head is always in a perfect position, and no time is needed to adjust the bed.
I now delegate tasks to the OR staff that I performed in the past. I train, delegate, and then supervise these nonsurgical steps. Because I am personally engaged in the training and reviewing of these steps, I am comfortable that they will be done correctly by my staff. Now the OR staff knows how to prepare the eye for surgery, drape the patient, and place the lid speculum. Additionally, during the prep they know to make certain that the top of the patient’s head is at the edge of the stretcher and that his or her chin is higher than the forehead.
Plan With Flexibility, Integrate Communication
Orchestrating the steps to keep the pace of surgery requires staff members to stay in touch with the surgical flow. When we use two ORs, we use a wireless doorbell placed in the hallway to alert the other OR to allow timing of the drape and lid speculum placement. The circulating nurse pushes the remote for the doorbell when the IOL is being placed in the eye, and this tells the other OR personnel that the surgeon should be entering their OR in about 3 minutes.
Communicating with your staff will flush out rough spots that are slowing down your day. For example, I noticed that the staff barely had time to get the cataract set out of the sterilizer and cool the phacoemulsification handpiece quickly to allow surgery to begin. This was stressful for the scrub technician, and also it was not ideal for the lifespan of the handpiece to have the quartz crystals cooling in water. I realized that, if we purchased a fourth sterilizer and a fifth cataract set, there would always be a set ready to use. The cost of purchasing these items would be offset over time by increased volume, and it would also be worthwhile not to have the staff stressed or rushing to set up.
I also try to wait until the end of the day to deconstruct problems with pace and flow. Meeting with the team at the end of a busy day helps us improve by allowing us to micromanage each person’s role for the next surgery day.
Another correction in staff roles occurred after the circulating nurse who was accompanying the patient to the recovery room reported having trouble getting back to the OR to set up for the next case. Once in the recovery room, the nurse would get sidetracked with questions or other distractions. Now, we have the anesthesia provider bring the patient to the recovery room alone instead of the nurse, because he or she is going in that direction anyway. On busy days, the nurse manager will help with breaks and help keep the day moving along.
We changed the role of staff members in other minor ways, too. For example, during room turnover, the instrument cleaning technician helps the circulating nurse by moving the footpedals into position. Little changes in delegating tasks such as these may save only 1 minute, but, after 37 cases in a day, those minutes add up.
Discussing issues with staff and creating specific roles encourages staff members to stay in their lanes and thereby creates efficiency.
Build on the Shoulders of Technology
Technological advances over time have allowed cataract surgery to become more predictable with fewer steps and more routine cases. Complications or challenges during surgery add time to the day and shift the staff members out of their routines. I use femtosecond laser technology in most of my cases, along with recent-vintage phacoemulsification machines that keep the anterior chamber formed and include refined phacoemulsification tips. I also use reengineered tools for cortex removal and preloaded IOLs.
These advances have combined to make cataract surgery an overall safer procedure. For example, in more than 1,800 cataract cases in 2019, there was only one vitrectomy and only one case requiring a pupil expander. A complication interrupts routine, and any change in surgical patterns slows down the day and challenges patient flow. Performing cataract surgery with predictable steps for the staff allows them to get into a groove.
It’s Not Always Right the First Time
Flexibility from the entire team to implement strategy is paramount in creating efficiency in the OR. When we were integrating femtosecond laser technology for cataract surgery, we met with key nurses, technicians, and anesthesia providers for strategy sessions. Moving soda cans simulating stretchers around on a break room table, we came up with a strategy that failed in the OR the next day. At the next meeting, we used the salt and pepper shakers—which worked out perfectly (Figure 2). In two ORs we are now able to perform 37 cases a day, including about 25 that are femtosecond laser-assisted.
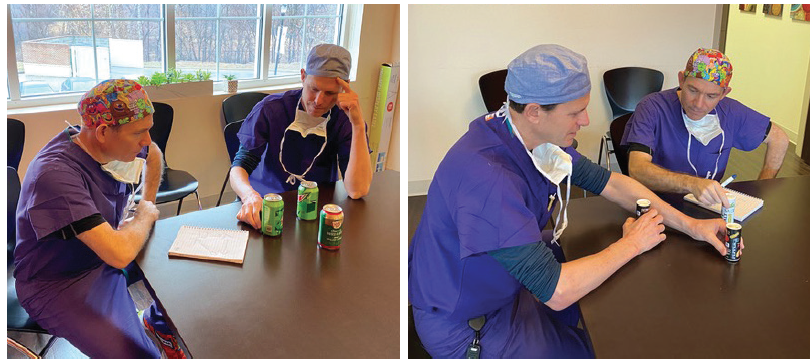
Figure 2. When Dr. LaBorwit and his team were figuring out patient flow for using a femtosecond laser with two ORs, they first used soda cans as stretchers to outline our plan. It didn’t work. After the failed experience, they used salt and pepper shakers and reworked the flow.
Warn your OR staff that it will take some time to get it right. One time, I didn’t tell the team in advance that a new stretcher was coming, and later that day I found it hidden in the patient bathroom so they wouldn’t have to work it into the busy day (Figure 3).

Figure 3. Prepare and communicate with staff. Dr. LaBorwit once forgot to tell the nursing staff that a new stretcher was coming. Because there was no plan in place, they hid it in the bathroom (without letting him know it came in) so that it wouldn’t disrupt the day.
Figures 1–3 courtesy of Scott LaBorwit, MD
The focus should be on surgery, with all details, concerns, and changes having been discussed before the start of the day. The surgeon should have all IOLs selected and sent to the surgical center at least 1 day before they will be used in surgery. The surgeon should also be able to stay on task, and office staff should know to interrupt the surgeon only in a true emergency. What may seem like just a minute’s interruption can add up over time and break the rhythm and focus of the day.
Another efficiency improvement occurred when the post-anesthesia care unit (PACU) changed the process for discharge after surgery. The discharge instructions are now reviewed with the patient during the preoperative period while the eye is dilating.
Also, the family member or guest accompanying the patient is brought to the recovery area before the patient comes out of surgery. This allows time to again go over the discharge instructions, and the patient can see a familiar smiling face as he or she comes out from surgery. This change allows the nurses in the PACU to better pace flow, and discharging patients has become more efficient.
Game Day, Game Face
Efficiency is created by using a team approach to analyze opportunities to improve workflow. It requires flexibility and the ability to learn and adapt. Efficiency should not come at the cost of rushing or stressing out.
All team members need to understand the reasons and goals for change and engage in the process in order to achieve success. Learning from others, then adapting and customizing these processes to make them fit in your own OR, maybe challenging at first, but over time the improvement is rewarding and the new becomes routine.
Finding opportunities to save time and money can benefit surgeons, staff members, and patients alike.
Steven M. Silverstein, MD, FACS

Achieving efficiency in the ambulatory surgery center (ASC) is not just important, it’s also fun. Whether we are solo owners, part of a physician-owned facility, or share-owners in a hospital or corporate program, being mindful of our every motion translates into time spent doing more cases per surgical block, getting back into clinic or other business responsibilities sooner, and conserving more quality time outside of the office.
Efficiency begins with the ergonomics of the facility. This can always be improved, so we mustn’t become complacent. Proper patient flow is of utmost importance from the time the patient checks in; through the preoperative period, the surgery, and the postoperative period; to the time the patient receives discharge instructions. Discharge should involve the fewest possible steps for both the staff and the patient. This shows the staff members that we value their time, and it minimizes the stress and strain on the patients, many of whom are elderly.
DO IT RIGHT
I had the opportunity to design and build our facility with the guidance of an expert in ASC ergonomics, and I also participated in the certification process. Working with an expert is essential. It can not only save time and money during the construction phase but also help to ensure that the facility is built to code. In this way, the facility can receive state and federal certification as quickly as possible, thus preventing extremely costly rebuilds to make the facility compliant with ASC and Medicare regulations. There are countless horror stories about the consequences of failed inspections, the expense of bringing an ASC up to code, and the lost revenue that this entails. Under the best of circumstances, an ASC does not begin earning money relative to debt service during the first year, so getting up and running as soon as possible is paramount.
CREATING EFFICIENCY
In the preoperative holding area, our patients are placed on motorized beds, some of which are specifically designed for a capacity of 700 pounds. Each one has its own electrocardiogram monitor that connects to the patient not by sticky pads and electrodes but by two or three large—and comfortable—alligator clips for the wrist and ankle that take just seconds to apply. Each bed also has its own oxygen tank with clean tubing and nasal prongs.
This bed is also the OR bed, so patients do not require transfer from one bed to another. Once the bed is in the OR, the oxygen is connected to a wall source. In the preoperative holding area, the patient receives three rounds of drops—antibiotics, a dilator cocktail, anesthetic drops, and lidocaine jelly—delivered by the nurse, while the nurse anesthetist is examining and reviewing medical history with the patient. If the patient is anxious or requires a retrobulbar or peribulbar block, the nurse anesthetist places 3 to 4 drops of sublingual midazolam (Versed, Pfizer) under the patient’s tongue. Most patients do not receive or require an intravenous (IV) line or heparin lock.
Giving the OR staff a heads-up based on your assessment in the clinic as to which patients may require IV sedation and/or a block also saves time and makes the surgical journey faster and smoother for both patient and staff. Corneal refractive surgery patients are comfortably seated in ASC-approved recliners rather than beds, making their stay both comfortable and easy, and they are typically walked into the OR by the accompanying nurse.
OR DESIGN AND LOGISTICS
First thing in the morning, our surgeons do a 5-minute scrub followed by use of an approved alcohol-based hand sterilizer, and that is the only scrub of the surgeon’s morning or afternoon. Between each case, the surgeon applies three squirts of the same hand sanitizer by holding his or her hand under a motion sensitive system that delivers it. The liquid then dries before the surgeon enters the OR for the next case.
The design and logistics of the OR relative to the scrub sink and dirty and clean rooms is also important. First, an efficient layout can save the surgeons and staff members steps, but also the distance from the clean room to the OR should be as short as possible to avoid contamination in the unsterile hallway. Some ASCs incorporate a clever system whereby the clean room sits between two ORs, and the clean instruments are simply passed through to the surgical suite via a window.
In our second ASC, we have two teams of nurses and scrubs. Near the end of each case, a separate team swoops into the room to turn it over while the surgeon signs all of the pretyped and approved orders, discharge instructions, operative report notes, and other paperwork. Meanwhile, the circulating nurse and nurse anesthetist are taking the just-completed patient to the postoperative area—which is set up in the same fashion as the preoperative area, with multiple bays—and bringing in the next patient while the scrub nurse is setting up the room for the next case.
ERGONOMICS
Ophthalmologists are quite prone to permanent orthopedic conditions due to the unnatural sitting positions we assume in clinic and in the OR. In fact, the AAO assembled a panel a number of years ago to address this issue at length.
It is important to use a comfortable seat. Look in the exhibition halls at the major meetings; there are always companies selling a variety of styles. Whatever seat you choose to use, make certain that the microscope oculars and your back, hand, and arm positions are proper and comfortable before starting a case.
DURING SURGERY
During surgery, it is important to use as few surgical steps as possible, only entering or exiting the eye for the next step. This cuts down on surgical time, lessens the risk of tissue damage, and lowers the risk of carrying organisms into the eye. The fewer steps and instruments used, the better. Be deliberate about each step.
To minimize instrument exchange, I use microincision cataract surgery (MICS) capsulorhexis forceps that I designed (Silverstein MICS capsulorhexis forceps, Bausch + Lomb). These long, slender forceps work through a normal-sized incision or a sub–2-mm incision without oar-locking. They are scored at 5.5 mm and 6 mm, so that the surgeon can determine the size of the capsulorhexis in vivo. They also have sharp, pointed, roughened tips to allow both puncture and easy grasping of the capsule without going in and out of the eye with first a cystotome needle and then a separate pair of forceps.
As another point of efficiency, I use a 2% hydroxypropyl methylcellulose OVD (OcuCoat, Bausch + Lomb) because it both protects the cornea and tissues of the anterior segment and coats the corneal surface. It also allows perfect visualization throughout the case without the need for constant squirting of balanced saline solution by the scrub technician. OcuCoat also comes in a full 1-cc syringe, so there is plenty of volume to get through the surgery without needing to open additional syringes, saving significant cost.
POSTOPERATIVE PERIOD
After surgery, the patient’s family or guests walk only a few steps from the check-in/waiting room to the patient education area for final postoperative instructions, and then each patient is wheeled to his or her car by a staff member.
Speaking of staff members, although the ASC maintains a core group of full-time nurses and staff, on particularly busy surgery days we share staff from our practice. This saves both the facility and the practice tens of thousands of dollars each year in salaries and benefits. Additionally, the high level of staff cross-training this practice requires leads to greater pride and job satisfaction among our motivated technicians who wish to have added responsibilities beyond patient workups in the clinic. It has also demonstrably contributed to staff retention by reducing boredom and burnout.
CONCLUSION
Thinking through efficiencies in your facility—even if you are hospital-based—can be enjoyable, satisfying, and profitable. In the end, it is not about speed for speed’s sake: The patient experience, safety, and superlative outcomes are our only priorities.
Our time has value, and improving efficiency in the ASC should be a priority for each of us. The result can lead to opportunities for additional productivity among staff and surgeons and can free you up to enjoy more time away from the OR.
Making a slight adjustment to our femtosecond laser settings cut surgery time by about 6 seconds and may have decreased the risk of suction loss.
Jonathan D. Solomon, MD

The linchpin for the femtosecond laser in cataract surgery is the delivery of arcuate incisions. This is the last step performed during the laser treatment, and, if suction fails or something else goes wrong during the laser application, astigmatism correction is lost and must be performed some other way, whether through manual arcuate incisions or use of a toric IOL.
When the surgeon steps on the pedal of the femtosecond laser, the suction turns on, docking occurs, and, as soon as all of the settings are confirmed, laser delivery begins. The typical order of events during femtosecond laser cataract surgery is capsulotomy, cataract fragmentation, and, finally, corneal treatments, which include the creation of the main and arcuate incisions.
The problem with this order of treatment is that, if the patient moves or something else causes suction to break, the corneal treatment will be lost. This means that arguably the most important part of the laser cataract procedure—for the purposes of billing and correction of refractive errors—is lost.
What We Changed
A few months ago, my practice had a run of several patients who, for whatever reason—movement of the head, fluid loss, or something else—had suction breaks occur. To try to avoid this, we changed the settings on our Lensar Laser System (Lensar) to, in essence, allow the laser to travel faster through the lens. We spread out the spot-line separation through the nucleus from the typical 20 to 50 μm.
This means that the femtosecond laser just blazes right through the cataract component of the procedure, cutting about 6 seconds off the procedure time. That may not sound like a whole lot of time; however, it took our average treatment time from 73 seconds down to 67 seconds.
For the surgeon, it can feel like an eternity waiting for the suction to stop during the laser procedure. You’re not doing anything other than holding your finger on a pedal or button. Cutting out those 6 seconds has allowed greater efficiency without having a noticeable impact on the actual treatments.
The change has thus far allowed us to avoid the dreaded suction loss, which in turn allowed us to deliver complete treatment to a greater number of patients.
Use of a sublingual sedative has increased my efficiency in the OR.
Russell Swan, MD

Surgeons should never rush a surgery, but we should strive to be as effective and efficient as possible for our patients. One question I often ask other surgeons when we discuss efficiency in the OR is whether the OR staff is waiting for the surgeon or the surgeon is waiting for the OR staff. The most important aspect of building efficiency, in my mind, is embracing a team approach and empowering members of the team to function at their highest level.
I use two ORs, so, ideally, when I finish surgery in one OR I move into the other OR for another surgery. While I am performing that surgery, the circulating nurse and scrub technician from the first OR know what needs to be done before I return for the next case. They place all postoperative drops for the patient whose surgery was just completed, clean the patient, transfer him or her to the PACU, clean the OR, prepare for the next case, bring the next patient back, prep the next patient’s eye, place the surgical drape and speculum, keep the patient’s eye wet, and prepare for a time-out the moment I walk into the room. This well-choreographed dance continues back and forth throughout the day and allows each patient to receive the extraordinary care he or she deserves, while also allowing me to serve as many patients as possible.
IV-FREE SEDATION
One of the biggest efficiency builders in our ASC that has been a win for patients and staff has been the use of a compounded, sublingual sedative, a midazolam, ketamine, and ondansetron melt (MKO Melt, ImprimisRx). This IV-free method of sedation eliminates one of the largest pain points of topical cataract surgery—insertion of the IV. The melts also provide a uniform, predictable level of sedation while avoiding the time and energy our staff used to spend getting the IV inserted into a fasting patient and removing it after the case. The early onset of the sedation allows the staff members to easily drape the patient prior to my arrival in the room.
OTHER TRICKS
I strongly believe in the power of video review, self study, and learning from others. A simple goal I have is to reduce the number of instrument handoffs that occur during surgery. Simple examples of this include placing a dispersive OVD and then using that cannula to stabilize the eye for creation of the main incision. Further, I love using capsulorhexis forceps (MicroSurgical Technologies) that allow me to puncture the capsule and then efficiently create the continuous curvilinear capsulorhexis.
Other surgical changes I have incorporated to increase efficiency include using a Wong pocket for corneal wound hydration1 and using a modified hydrodissection technique.
CONCLUSION
These simple changes have all come from carefully observing other surgeons and borrowing from their wisdom. I love visiting other surgeons, and I encourage others to commit to spending 1 day a year with another surgeon to see if there is anything you might learn and incorporate into your practice.
1. Wong MY. Tools & techniques: Using the Wong incision to improve the seal of a clear corneal incision. Eyeworld. June 2012. Available at https://www.eyeworld.org/article-using-the-wong-incision-to-improve–the-seal-of-a-clear-corneal-incision. Accessed February 27, 2020.




