Staying Positive With the U Curve
An experienced ophthalmologist shares pearls for staying optimistic through the ups and downs of life and career.

BY THOMAS A. OETTING, MD
THE U CURVE
Have you heard about the U curve (Figure)? This economic concept, describing a U-shaped relationship between happiness and age, gives me great solace. The concept of the U curve has been described in various economic and social science journals over the past 20 years.1-3 The concept is based on data from a variety of surveys on well-being, and it seems to transcend time and culture.
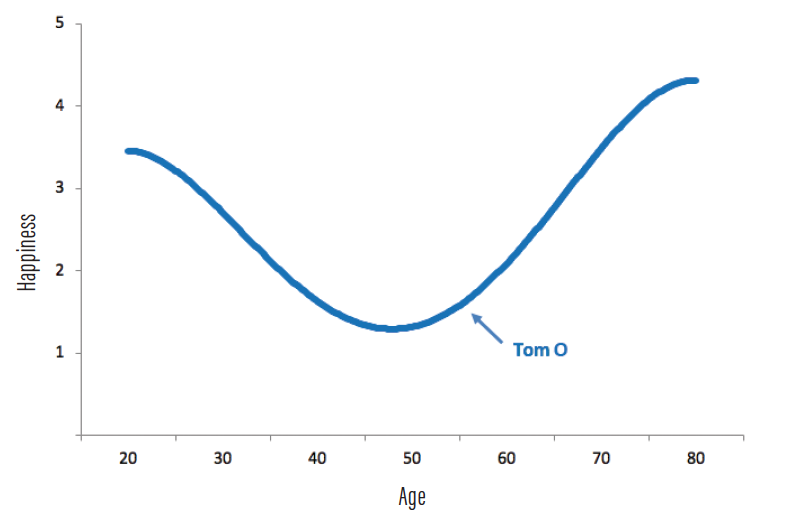
Figure. The U curve representing happiness relative to age in human life.
Courtesy of Thomas A. Oetting, MD
Basically, these data suggest that we start off happy at a young age, and our happiness decreases over time, reaching a nadir when we are about 50 years old. But here’s the great news: After this age, our happiness shoots back up and may even exceed that of our youth.
I love that the U curve reveals how we all feel during the craziest part of most of our lives, as we slip down that curve from 30 to 50 years old. I know that this is not a universal experience, but the U shape really resonates with me. And the idea of the U curve shows that we are not alone if we feel stressed during this phase of life. We are likely juggling too much, and our expectations are likely too high during this 30-to-50-year age range. People have been sold, as I was a few years ago, on the idea that we could be great parents, great spouses, great doctors, and great friends, all at the same time and all while remaining thin and athletic. How’s that working for you?
LEARNING FROM THE DOWNS
The U curve projects optimism. As you slide down the curve during your 30s and 40s, just know that good times most likely lie ahead. Don’t go out and buy a sports car or have an affair in search of happiness. Just remember that, statistically, good times are coming. Also keep in mind that this slide down the happiness curve during your 30-to-50-year-old phase provides experiences that will help you learn to balance and to figure out what is really important to you. It’s the junior high school of adulthood.
The good news for me is that I am on the happier side of that 50-year nadir of the U curve. I realize where I fit in the world, and I am not stressed out by the day-to-day issues of emails, clinical ups and downs, and the drama of my world of make-believe here in Iowa City. I know my place in life. I know that I can’t do it all, and I know how to say, “No, but thanks for asking.” I realize that relationships are the most fun parts of our lives and sustain us more than research papers or money ever will.
A NOTE TO YOUNG OPHTHALMOLOGISTS
My advice to wonderful young ophthalmologists such as Ashley Brissette, MD, MSc, FRCSC, is to keep charging but give yourself a break if you get a little down or find that you can’t do it all. The good part of the U curve will come around for you soon enough.
1. Blanchflower, DG, Oswald AJ. Is well-being U-shaped over the life cycle? Soc Sci Med. 2008;66(8):1733-1749.
2. Clark AE, Oswald AJ. The curved relationship between subjective well-being and age. 2006. HAL open access journal. https://halshs.archives-ouvertes.fr/halshs-00590404/document. Accessed August 16, 2019.
3. Graham C, Pozuelo JR. Happiness, stress, and age: how the U curve varies across people and places. J Popul Econ. 2017;30:225-264.
Work-Life Balance and Burnout
Physician burnout from a young ophthalmologist’s perspective.

BY ASHLEY BRISSETTE, MD, MSC, FRCSC
Physician burnout from a young ophthalmologist’s perspective.
As a millennial, I am well aware that my generation has been pegged as a group that places a high value on work-life balance. Older generations may even believe that our desire for work-life balance means that we do not want to work as hard as our predecessors. However, I would argue that millennials have a strong desire to work hard, but we also realize that success at work should not come at the expense of our personal health and happiness.
BURNOUT
The term burnout has become synonymous with practicing medicine. Burnout can occur when a physician’s workload increases and the stresses of the job start to outweigh the benefits. Due to the nature of our work, ophthalmologists may be less prone to burnout than physicians in other medical specialties. We are not, however, immune to it. Burnout affects not only the physical body, as a result of late hours on call, answering emails and phone calls, or finishing electronic medical records well past our clinic hours; it can also affect our emotional well-being.
We all start our ophthalmology careers with a singular goal: to improve vision and promote the health of our patients. Along the way toward reaching this goal, we are exposed to job stressors, including surgical or medical complications, administrative duties, electronic medical records, and reimbursements. In the end, we may be spending more time focusing on these than taking care of the people in need of our services.
We can become cynical and/or lose our capacity for empathy if burnout is not addressed. I think that the physicians of my generation understand the importance of being committed to this profession while at the same time making sure we are physically and emotionally supported.
PREVENTING BURNOUT
There are a few strategies I use to prevent burnout in this profession. My biggest tip is to create a sense of community. I attend many conferences, which has allowed me to foster friendships and mentors within ophthalmology. I also make sure to reach out to colleagues when I have tough questions about patient care or am having a difficult day and looking for advice on how to approach a complex problem. In fact, use of social media has made it extremely easy to reach out to other ophthalmologists and to interact with surgeons around the world. It is also important to have a way to check in with your personal well-being, whether through hobbies, religion, therapy, journaling, or whatever it is that may help you, is important.
Lastly, my strongest recommendation is to make time for physical exercise. We know it helps to improve not just physical health, but also mental health, so making the time to exercise should be a priority. We need to take care of ourselves first if we are going to be able to take care of our patients.
POSITIVE CHANGES
Attention to work-life balance in our specialty is growing, and more doctors are moving toward work-life integration. Some conferences I have recently attended have encouraged participants to bring their families and have also provided child care. I think these are positive changes that will help keep us all happy and healthy in ophthalmology.




