In the formal classification, micro-invasive glaucoma surgery (MIGS) devices are defined by five criteria: (1) use of an ab interno approach; (2) minimal trauma to the target tissue with negligible disruption of normal anatomy and physiology; (3) at least modest efficacy; (4) high safety profile; and (5) rapid patient recovery with minimal impact on their quality of life.1 Since this definition was introduced, several devices and surgeries have broadened the offerings in the MIGS category, and thereby broadened the definition. For example, in some MIGS procedures, the surgeon excises at least a portion of the trabecular meshwork (TM) tissue, with the idea that removing diseased tissue should facilitate improved flow mechanics. Such procedures raise several questions: are they indeed “minimally traumatic to the target tissue,” as the formal definition requires? Do goniotomies fall under a separate category compared to trabeculotomy, and as to the latter, is there a difference between removing tissue for 90° versus 180°? More fundamentally, are these procedures desirable options in the armamentarium of glaucoma treatment options if they obviate future options that would otherwise be targeted at the removed tissue?
Ultimately, the pursuit of formal definitions may be more of an academic exercise. Nevertheless, new MIGS devices have added to, and have not necessarily replaced, the options available to the practitioner. In our view, the variety of MIGS devices offers greater ability to personalize the care of each patient. In that context, options for TM removal do not need to fit any sort of definition if the more important question is whether the risk-benefit profile makes sense for the individual patient and whether they preclude future options. Certainly, some forms of glaucoma, such as juvenile or angle-closure glaucoma, might benefit from TM removal, and so it is important to recognize a role for these procedures.
As the above illustrates, clinicians are able to ask a different set of questions than they historically may have with a treatment paradigm that started with drops, moved to laser, and considered invasive surgery as a last resort. MIGS has facilitated the laudable goal of early intervention, with the mindset of performing the best procedure for the patient today with an eye to what future steps may be warranted. As clinicians approach the prospect of individualizing the care of glaucoma patients, an understanding of the relevant data can help guide decision-making. As well, to be truly successful in this regard, clinicians may be challenged to rethink their conventional definitions of a successful outcome.
Mechanisms of Action
One way to differentiate among MIGS devices is according to where in the aqueous drainage pathway it has an effect. Emerging evidence in the glaucoma literature has expanded the understanding of aqueous flow dynamics. Although a majority of resistance in primary open-angle glaucoma (POAG) occurs in the TM, the juxtacanalicular region and the Schlemm canal (SC) are also important potential areas of blockages.2 Moreover, these anatomic structures function within the conventional outflow pathway. Recent evidence highlights the important role of collector channels in directing flow to the distal drainage system, ultimately terminating in the episcleral venous system.3

Collectively, an evolved understanding of aqueous flow dynamics demonstrate that the entire system is complex, and each component has a function in physiologic flow. Therefore, MIGS options which address multiple potential sources of resistance may offer a distinct advantage. To this point, the trimodal mechanism of action associated with Hydrus Microstent (Alcon LLC; Fort Worth, TX; USA) is notable: the Hydrus Microstent (1) directs aqueous to bypass the TM through the inlet of the device to allow fluid to pass from the anterior chamber into the SC; (2) scaffolds the SC to provide permanent patency in the canal to prevent SC collapse, despite IOP elevation and augment flow; and (3) maintains patency across a 90° span of the canal, providing access to multiple collector channels over time.4 The device is engineered with a slight contour to match the curvature of the SC and with three open windows along its 8-mm length that face the anterior chamber for unobstructed collector channel access.5 The latter is a significant consideration, as complete blockages/herniations or collapse of the SC that block the ostia of the collector channels are present in about 50% of eyes with POAG.6
There may be an additional aspect to consider after successful implantation of a Hydrus device. Mechanically opening a portion of the canal and scaffolding it open over time potentially restores physiologic function within the aqueous drainage pathway. Moreover, if there is a collapse in the SC, bypassing the canal vis-à-vis a focal stent may be insufficient to undo the collapse.7 Intuitively, opening and maintaining the patency of SC for 90° are additive to TM bypass in assuring aqueous drainage.
As reviewed in other parts of this supplement, these mechanisms and benefits appear to contribute to better outcomes compared to cataract surgery (CS) alone (see Reviewing HORIZON 2- and 5-Year Outcomes). While separating the effects of MIGS and CS on IOP response postoperatively is complicated, there is evidence accumulating from major clinical trials to support that MIGS devices have an additive effect on IOP lowering.5,8,9 For example, the IOP-lowering effect of CS alone was similar in the comparison groups in each of the COMPASS, HYDRUS II, and HORIZON trials, and deemed greater in each group being studied with a MIGS device.5,8,9 Consistently better IOP response should tell us something. As well, MIGS devices appear to deliver more durable IOP reduction: in the Hydrus II Study, mean diurnal washed-out IOP in the Hydrus plus CS group was slightly lower when compared to the CS alone group at 12 months, and then the IOP rebounded at 24 months in the CS group (Figure 1).5
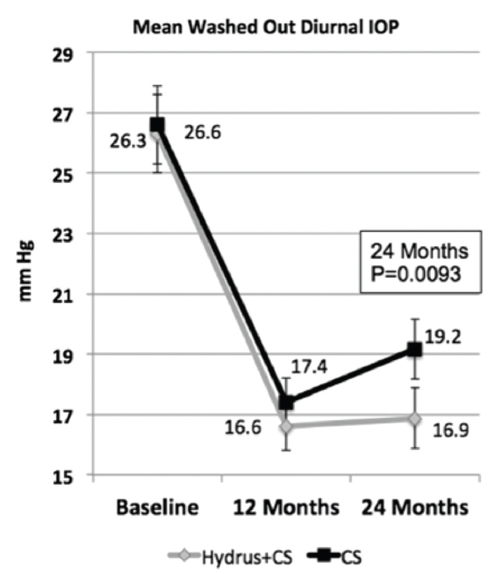
Figure 1. The IOP rebounded at 24 months in the CS group in the Hydrus II study.
However, a singular focus on IOP may paint an incomplete picture when judging outcomes after MIGS surgery. As demonstrated in the HORIZON trial, compared to CS alone, Hydrus plus CS resulted in a higher percentage of patients on zero medications at 2 and 5 years and a significant reduction in the need for invasive secondary surgical interventions (SSI), in addition to greater-magnitude reduction in IOP at 2 and 5 years.9-11
Differentiating the Data
The decision-making process in POAG is inherently different for each ophthalmologist, but it is safe to say we are all working from the same library of MIGS studies. A question we must answer is how to compare outcomes from one study to another, and ultimately between one device or surgery and another, so that we can make the best decision for each individual patient.
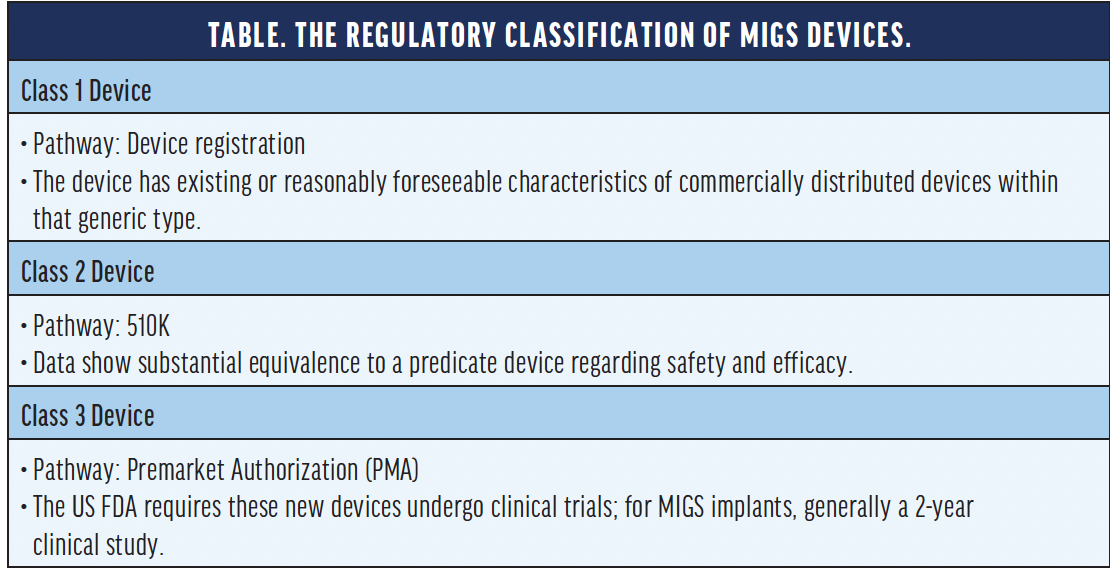
Although the various MIGS devices and surgeries belong to the same category, the regulatory pathway each one followed is different. Some nonimplantable MIGS devices are classified as Class 1 or 2 devices, whereas implantable MIGS devices require the full premarket approval process associated with Class 3 devices (Table). The distinction may be a factor when considering the evidence associated with a particular device: data requirements for Class 1 or 2 devices may not include clinical data or may be limited to 1 year. If clinical data exist, they will not be of the rigor required for Class 3 devices. As well, with respect to Class 2 devices, the selected predicate devices may be variable; furthermore, Class 3 MIGS devices must be implanted in conjunction with CS.

As clinicians, we want to feel confident in the quality of the data from a clinical trial, and here again is something we see in the HORIZON trial. From our perspective, these are unprecedented data in the context of a 5-year study by design for MIGS implant devices. In brief, the HORIZON trial had a 2-year pivotal phase with the primary endpoint being the percentage of patients with a reduction of at least 20% in mean washed-out diurnal IOP from baseline. The study met this endpoint, and several secondary endpoints also favored the use of Hydrus Microstent plus CS versus CS alone. In years 3-5 of the study, which retained a large majority (80%) of enrollees, patients were followed to assess safety and for monitoring efficacy outcomes; however, medication washout was not continued beyond 24 months. This second phase of the study demonstrated continued durability in the IOP response, while also providing insights into the impact of MIGS on the clinical disease course relative to CS alone.
The findings from the study on their own demonstrate the benefits of this particular MIGS device. Yet, the fact that they come from a study which enrolled patients both in the United States and from outside the United States, and which was able to retain 80% of patients through 5 years, adds additional merit. We note, as well, that the demographics of the study population are similar to what the average US glaucoma specialist sees in clinical practice, making it that much easier to see our own patients in the data.12

What it All Means
Fundamentally, MIGS challenges the definition of a successful postoperative outcome in the sense that it asks clinicians to reconsider the goals, objectives, and endpoints of surgery. The safety data from major trials show us that MIGS devices are appropriate for use earlier in the disease continuum, thereby providing long-term, durable control of IOP, the only known modifiable risk factor in POAG.9-11 Based on what we have learned from HORIZON, we can also have conversations with patients about how medications are affecting their daily lives and whether they have cost concerns, because we have data that show us a unique ability to reduce or eliminate drop burden by using a Hydrus device at the time of CS. Individualizing the approach to POAG while considering the impact on quality of life has long been held as the ideal in glaucoma management. Ultimately, these data from HORIZON show us that we are getting closer to that goal.
1. Saheb H, Ahmed II. Micro-invasive glaucoma surgery: current perspectives and future directions. Curr Opin Ophthalmol. 2012;23(2):96-104.
2. Johnson M. What controls aqueous humour outflow resistance? Exp Eye Res. 2006;82(4):545-557.
3. Goel M, Picciani RG, Lee RK, Bhattacharya SK. Aqueous humor dynamics: a review. Open Ophthalmol J. 2010;4:52-59.
4. HYDRUS Microstent [instructions for use]. Irvine, CA: Alcon Vision LLC; September 2021 (United States).
5. Pfeiffer N, Garcia-Feijoo J, Martinez-de-la-Casa JM, et al. A randomized trial of a schlemm’s canal microstent with phacoemulsification for reducing intraocular pressure in open-angle glaucoma. Ophthalmology. 2015;122(7):1283-1293.
6. Gong H, Johnstone M, et al. Poster #115 American Glaucoma Society, New York 2012.
7. Allingham RR, de Kater AW, Ethier CR. Schlemm’s canal and primary open angle glaucoma: correlation between Schlemm’s canal dimensions and outflow facility. Exp Eye Res. 1996;62(1):101-109.
8. Vold S, Ahmed II, Craven ER, et al; CyPass Study Group. Two-Year COMPASS Trial Results: supraciliary microstenting with phacoemulsification in patients with open-angle glaucoma and cataracts. Ophthalmology. 2016;123(10):2103-2112.
9. Samuelson TW, Chang DF, Marquis R, et al; HORIZON Investigators. A schlemm canal microstent for intraocular pressure reduction in primary open-angle glaucoma and cataract: The HORIZON Study. Ophthalmology. 2019;126(1):29-37.
10. Ahmed IIK, Rhee DJ, Jones J, et al; HORIZON Investigators. Three-year findings of the HORIZON Trial: a schlemm canal microstent for pressure reduction in primary open-angle glaucoma and cataract. Ophthalmology. 2021;128(6):857-865.
11. Ahmed IIK, De Francesco T, Rhee D, et al; HORIZON Investigators. Long-term outcomes from the HORIZON Randomized Trial for a schlemm’s canal microstent in combination cataract and glaucoma surgery. Ophthalmology. 2022;129(7):742-751.
12. Marketscope. 2021 Glaucoma Surgical Device Market Report: Global Analysis
for 2020 to 2026, July, 2021. Available at: https://www.market-scope.com/pages/reports/267/2021-glaucoma-surgical-device-market-report.



