The introduction of the EVO ICL lens (EVO) ushered in a new era for the ICL procedure. Now, it serves as a firstline option for patients with myopia and myopic astigmatism. Evidence has even shown the procedure to be an effective treatment for as low as -3.00 D of myopia.1 This article reviews proper patient selection and provides insight into what outcomes can be expected after EVO surgery.
PATIENT SELECTION AND EDUCATION
Patient selection. In my practice, we position EVO as a treatment offering in place of surface ablation procedures, although we still preform surface ablation where indicated. In the past, we might have offered the procedure only for those who were not good candidates for LASIK, such as those with troublesome corneas or high myopia (>-6.00 D). Now, however, we recommend EVO for a wider range of patients such as those with a stable refractive history and moderate myopia because the implant is removable by a doctor, setting the patient up for success in the future as the needs of their eyes may change. EVO is indicated for use in patients between 21 and 45 years of age with myopia or myopic astigmatism with spherical equivalent ranging from -3.00 to -20.00 D and cylinder from 1.00 to 4.00 D at the spectacle plane, and the internal anterior chamber depth (ACD) is at least 3.00 mm. EVO should not be used in patients with a true ACD of less than3.00 mm, an anterior chamber angle less than grade III, who are pregnant or nursing, are less than 21 years of age, who have moderate to severe glaucoma, or who do not meet the minimum endothelial cell density (ECD) in the directions for use.
EVO streamlines and enhances the patient experience, and therefore many patients become interested in the technology. We also prefer EVO for those with troublesome corneas and those at risk for keratoconus based on topography or epithelial mapping.
Introducing the procedure. Our email refractive consultation appointment reminders include a brief description of the services we offer with a hyperlink to our website. We encourage patients to review the EVO information on our website, most of which was provided by STAAR. The company provides excellent resources on the benefits and risks of surgery, including compelling testimonials from influencers such as Joe Jonas, of the Jonas Brothers band (click here).
Having EVO available in the United States is a game changer. It has made the conversations we have with our patients and our consultative process much simpler. Part of our advanced vision analysis is determining what’s the best fit for the patient in front of us. In the past when we talked about the multiple vision correction procedures that we offer, the discussion about ICL surgery was a little cumbersome because we had to explain the necessity for a preoperative peripheral iridotomy. Now with EVO, however, we explain that it takes about the same amount of time as LASIK but has numerous benefits unique to EVO, which is why this has become one of the most rapidly growing procedures that we offer. We tell them that it is removable by a doctor, allowing us to create vision for a lifetime and setting them up beautifully for the future. We also tell them several studies have demonstrated that postoperative vision is as good as or better than LASIK, which provides outstanding results.2 For all these reasons, our conversion rate has increased significantly since EVO became available.
SAME-DAY SURGERY
I prefer to approach EVO surgery as a same-day bilateral procedure, which we currently perform in an ambulatory surgery center. I don’t check the postoperative vault in the first eye before operating on the second eye because the vault at that time can appear to be greater than it actually is due to the timing of the assessment. The second eye is treated as an entirely new procedure with a separate sterile setup and medications and instrumentation from different manufactured lots to reduce the risk of endophthalmitis, consistent with same-day bilateral IOL surgery protocols.
On the day of surgery (between 1 and 6 hours after surgery) and at days 1 and 7, my practice checks visual acuity and IOP, and we assess the vault and centration of the lens. Postoperatively, the vault of EVO should be between 50% and 150% of the central corneal thickness (ie, 250–900 µm). If the vault falls outside this range, exchange or removal may be required only if the patient is experiencing visual symptoms (Figure 1).
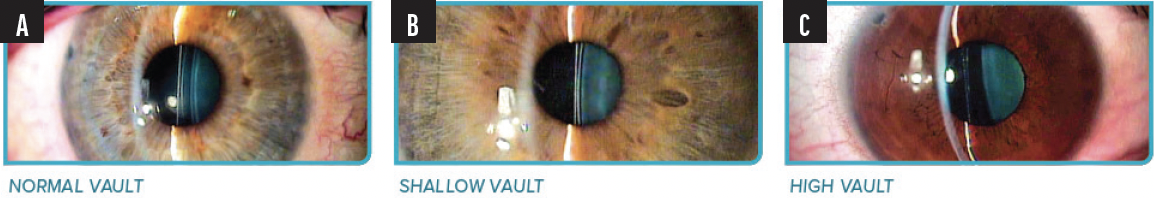
Figure 1. Normal (A), shallow (B), and high (C) vault after EVO surgery.
TYPICAL OUTCOMES
EVO can help patients achieve freedom from spectacles and glasses. Studies have shown that EVO achieves a high level of postoperative visual acuity, refractive predictability, and stability.3 In the published literature, 90.8% of 1,905 eyes achieved an accuracy within ±0.50 D, and 98.7% were within ±1.00 D up to 5 years after surgery. The uncorrected distance visual acuity was -0.02 logMAR. In the US FDA clinical trial of 619 eyes at 6-month follow-up,1 90.5% and 98.9%, respectively, were within ±0.50 and ±1.00 D of intended correction, and the efficacy index was 1.06. The efficacy index was defined as postoperative UCVA/preoperative CDVA. Regarding CDVA, most eyes (98.5%) were the same or better at 6 months postoperative, and about half (52.3%) gained one or more lines.3
EVO provides excellent visual stability. The US FDA clinical trial also showed excellent refractive and IOP stability at months 1, 3, and 6 postoperative (Figure 2). EVO also had high predictability across a large diopter range (Figure 3).
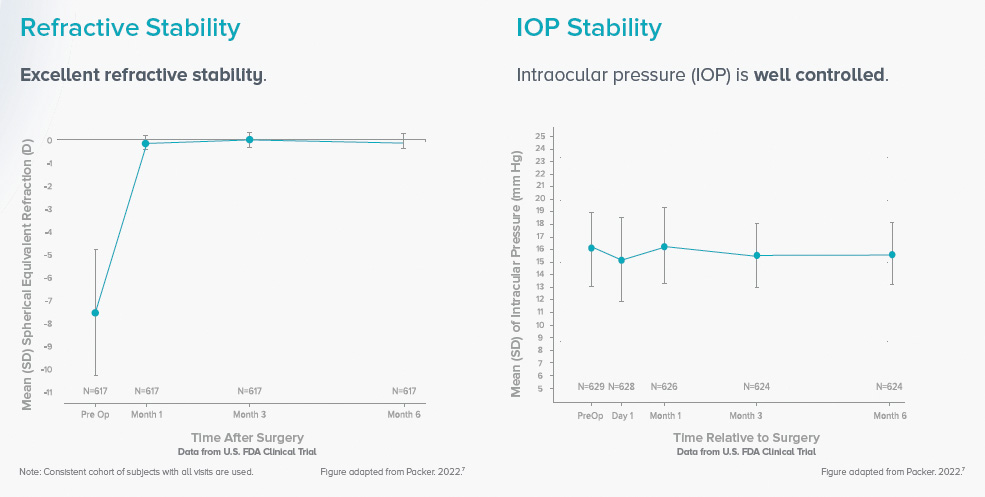
Figure 2. Refractive (A) and IOP (B) stability at 1, 3, and 6 months after EVO surgery. Figure 3. EVO has high predictability across a large diopter range.
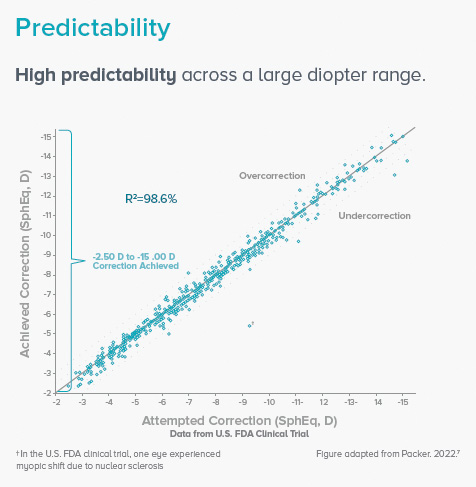
Figure 3. EVO has high predictability across a large diopter range.
Patients typically have excellent night vision with EVO. Studies have shown that there is significant improvement in mesopic contrast sensitivity with and without glare after EVO surgery4 with low induction of coma- and spherical-like and total higher-order aberrations.5 The rare potential for glare or halos is, however, always discussed with patients preoperatively.
EVO surgery is safe. The US FDA clinical trial confirmed that EVO has a reduced rate of anterior subcapsular cataract and pupillary block relative to earlier ICL models.1,3 Of course, all risks, benefits, and alternatives are always discussed with patients and documented.
EVO provides a quick visual recovery. Patients can expect quick visual recovery and may return to their daily activities the day after surgery. My patients are prescribed a mild steroid and antibiotic three or four times a day for 1 week.
Collectively, these outcomes point to a great potential for patients to experience these outcomes in the real-world setting.
CONCLUSION
Properly selecting patients, setting expectations, customizing the procedure, and using a meticulous surgical technique typically leads to an excellent outcome with EVO. Patients can expect the potential to achieve freedom from spectacles and glasses, stable effects, and excellent night vision.
1. Packer M. The EVO ICL for moderate myopia: results from the US FDA clinical trial. Clin Ophthalmol. 2022;16:3981-3991.
2. Sanders DR, Vukich JA. Comparison of implantable collamer lens (ICL) and laser-assisted in situ keratomileusis (LASIK) for low myopia. Cornea. 2003;22(4):324-31.
3. Packer M. The Implantable Collamer Lens with a central port: review of the literature. Clin Ophthalmol. 2018;12:2427-2438.
4. Martínez-Plaza E, López-Miguel A, López-de la Rosa A, et al. Effect of the EVO+ Visian phakic implantable collamer lens on visual performance and quality of vision and life. Am J Ophthalmol. 2021;226:117-125.
5. Igarashi A. Posterior chamber phakic IOLs vs. LASIK: Benefits and complications. Expert Review of Ophthalmology. 2019;14(1):43-52.

