INTROduction
MIGS has changed the landscape of surgical glaucoma so intensely that, particularly for newly minted glaucoma specialists, it may be difficult to remember the dynamics of pre-MIGS glaucoma practice. Still, the MIGS era is a new one, and developments that improve our ability to operate precisely and efficiently continue to propel us forward.
Adequate visualization of the angle is fundamental to MIGS, and yet many surgeons struggle to fully visualize the angle with their nondominant hand while still performing an elegant procedure. The release of GONIO ready® (OCULUS Surgical), a single-use gonioscopy system, which can be attached to your microscope, could address this challenge: GONIO ready® may not only improve our ability to see where we operate, but will also allow true bimanual MIGS to be performed.
My colleagues and I sat down for a roundtable discussion at AAO 2022 in Chicago to review the importance of visualization, discuss the limitations of available technology, and speculate how bimanual surgery could improve MIGS procedures. The second part of our discussion will appear in a forthcoming issue of Glaucoma Today and Cataract & Refractive Surgery Today.
—Iqbal “Ike” K. Ahmed, MD, FRCSC
Dr. Ahmed: Clear visualization is key to successful MIGS procedures, yet our current viewing systems have significant shortcomings. What are the biggest unmet needs in visualization for glaucoma specialists using MIGS?
Paul Harasymowycz, MD: When it comes to MIGS, if you can’t see the angle, you can’t operate. Pristine visualization comprises both magnification and a wide view of the angle, and acquiring both can be a challenge. Further, surgical instruments are sometimes impeded by the gonio prism that we use to visualize the angle, creating a frustrating scenario where we struggle to reach the very anatomy we have successfully visualized.
Ticiana De Francesco, MD: At first, one might assume that specific placement of a MIGS device or a unique surgical technique are the most challenging parts of completing a MIGS procedure. Actually, acquiring and maintaining a proper gonioscopic view from the angle is the most difficult part of many MIGS surgeries.
Leonard K. Seibold, MD: Control and consistency are major hurdles when it comes to MIGS. You might have a great view when you start a case, only to find that perspective compromised when the patient’s head or eye moves. Patients who cannot fixate present a challenge that we have not yet found a sufficient way to address.
Edward Yung, MD: Adding to this is the challenge of having to use one of our hands to visualize the angle and the other to perform surgery. This leaves us without a way to control unexpected movements. If we had a free hand to reposition a patient’s head and improve visualization, then some of these problems might not be so intrusive.
Dr. Ahmed: There are a handful of visualization systems available to surgeons placing MIGS devices. I’d like to hear from the panelists about their preferred approaches, as well as the limits of those approaches.
Ahmad Aref, MD, MBA: I’ve tried various stabilizing gonio prisms, but they often got in the way of the incision. For this reason, I use a handheld direct approach with a Swan-Jacob lens (Ocular Instruments) in approximately 95% of my cases. This approach is conducive to various MIGS procedures and does not interfere with instrumentation. Visualization of the extents of the angle can be difficult with a Swan-Jacob lens, and safely treating the extent of the nasal angle remains a challenge.
The Swan-Jacob lens is best used in experienced hands. Rotation of a prism, in order to maximize view of the nasal angle, by novice users may result in seepage of OVDs and increased corneal pressure, sometimes leading to view distortions or hemorrhage. For training purposes, Swan-Jacob lenses are limited.
Dr. Seibold: Like Dr. Aref, I use the Swan-Jacob lens in a vast majority of my cases. It allows me to make microadjustments, which become easier with experience. I have tried hands-free disposable lenses. They are nice in theory—as the name suggests, you’ll have a free hand during surgery—but I find myself adjusting them with my finger during surgery, which means I’ve merely swapped a hand for a finger, which is hardly an improvement. They’re simple and easy to use, but they’re limited in application.
Dr. Yung: The hands-free lenses Dr. Seibold described interfere with a smooth surgery. I find myself repeatedly tapping these hands-free lenses to the point that the patient’s eye is forced to endure a series of microadjustments. At that point, I’d rather just use a Swan-Jacob lens. Indirect lenses offer an advantage for some procedures (eg, goniosynechialysis, Xen gel stent implantation [AbbVie/Allergan]), but I otherwise almost always utilize a direct viewing system.
Dr. Ahmed: How comfortable are you with single-mirror viewing systems?
Dr. De Francesco: I have found it challenging to use single-mirror goniolens as I must be mindful that I am indeed moving to the correct direction (and not the opposite direction) with instruments during surgery. I feel more comfortable using a double-mirror goniolens.
Dr. Aref: I agree that visual inversion makes angle work difficult with a single-lens viewing platform. Single-mirror platforms have a role in ophthalmology, but use during MIGS may not be one of them.
Dr. Ahmed: The GONIO ready® is a single-use microscope-integrated gonioscopy system that allows truly bimanual surgery during MIGS (Figure). What are some of the potential benefits to a hands-free visualization system?
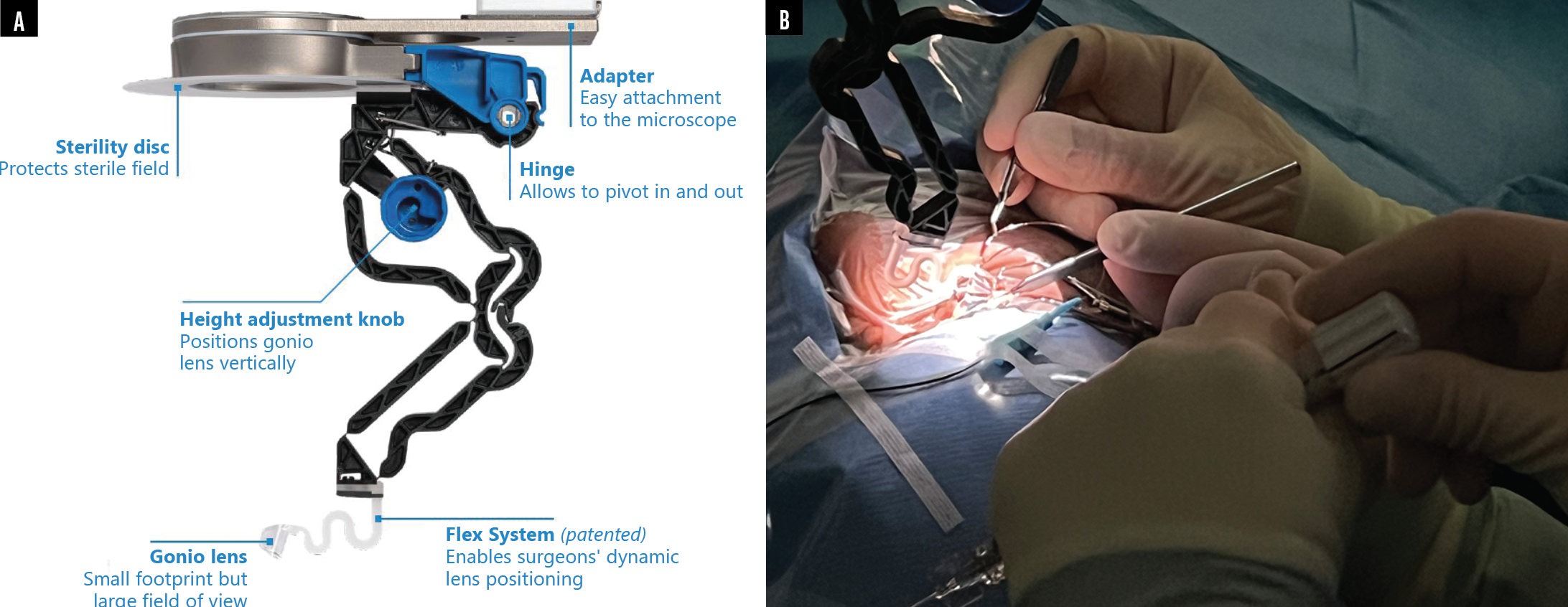
Figure. The design of the GONIO ready® single-use microscope-integrated gonioscopy system (A) allows glaucoma surgeons to improve visualization of the angle during MIGS and perform true bimanual MIGS procedures. The GONIO ready® attaches to the surgeon’s microscope, offers a large field of view, and allows dynamic lens positioning (B).
Dr. De Francesco: My ability to manage complications would be enhanced by having my nondominant hand free. Imagine if bleeding were to occur while performing a gonioscopy-assisted transluminal trabeculotomy. With my current visualization system, I need to withdraw my gonio lens and inject OVD into the anterior chamber. If my nondominant hand was free, I could inject OVD through the paracentesis while still keeping my angle view. This would make my procedure more efficient and allow me to control intraoperative bleeding better.
Dr. Harasymowycz: It may be easy to overlook, but it’s worth pointing out that having your second hand free to adjust a patient’s head would be a major improvement over our current approach.
Dr. Seibold: If one of our hands is occupied by a visualization system, we are limited in how much we can control our surgical instrument. It comes down to a simple principal: we are surgeons, and we’d prefer to have two hands on a device than only one hand—and we would always rather focus our hands on surgical placement rather than on a visualization system.









