The Hydrus® Microstent is indicated for adult patients with mild to moderate primary open-angle glaucoma (POAG) in conjunction with cataract surgery.
Introduction
As a category, Minimally Invasive Glaucoma Surgery (MIGS) procedures and devices have been shown to represent a less invasive alternative to traditional incisional glaucoma surgeries,1 thus making them suitable for use early in the natural course of the disease. The hypothesis underlying the “early recognition, early intervention” paradigm is that managing with a MIGS early on may help reduce IOP and topical medication burden for patients.
The HORIZON Study is the largest MIGS pivotal trial to date, enrolling 556 patients globally and was continuous to 5 years. The Hydrus Microstent® (Alcon) is the only MIGS device to show long-term safety and effectiveness outcomes from a pivotal trial at 5 years, including a high proportion of medication-free patients and a low rate of subsequent incisional surgeries to manage IOP.2-4 What exactly these data mean for real-world practice, and how they might inform how MIGS are used in the clinic, remains an important question to answer.
Here, Nathan M. Radcliffe, MD, of Mount Sinai School of Medicine, New York, and I. Paul Singh, MD, of the Eye Centers of Racine and Kenosha, Wisconsin, explore some of the key findings from the HORIZON Trial, the largest and longest duration pivotal trial of a MIGS device to date. Over the course of their discussion, they explore how these data shape and transform the management of POAG, as well as what they may teach us about the MIGS category as a whole.
What have we learned from the HORIZON trial through 5 years of follow-up?
Nathan M. Radcliffe, MD: If we take a step back and look at the HORIZON Trial from inception to the present, it has proven to be a rich dataset that has informed the way we treat POAG—not only in terms of how we use the Hydrus® Microstent, but also more generally in our thinking about the entire MIGS category. The topline takeaway from this study is that Hydrus plus cataract surgery was superior to cataract surgery alone in the percentage of patients with ≥ 20% reduction in unmedicated modified diurnal IOP (MDIOP) at 2 years, the study’s primary endpoint, which became the basis for gaining an indication from the US Food and Drug Administration (FDA).2 With the 3 and 5-year data, there is additional evidence of a durable effect (Figure 1).4

For the clinician, these data should provide confidence that for appropriate patients implanted with the Hydrus® Microstent, there is a good chance of lowering their IOP and reducing medication burden.
Some of the study’s other outcomes at the 5-year timepoint support our intervening with a device early in the disease process: there was a greater than 50% relative reduction in invasive Secondary Surgical Interventions (SSI)* compared to cataract surgery only at 5 years (2.4% Hydrus + cataract surgery vs. 5.3% cataract surgery alone), and a high medication-free rate at every time point.
HORIZON: Fast Facts
- Largest MIGS pivotal trial to date
- Global study: 38 sites, 9 countries, 556 patients randomized (331 US; 225 OUS)
- Five years of continuous follow up with 80% retention at year 5 (Hydrus: 83.5% [308/369]; Control: and 71.7% [134/187])4
To me, both of those endpoints highlight the advantages associated with opening up Schlemm’s canal and maintaining its patency long-term.

I. Paul Singh, MD: I agree. It’s so important to remember that being medication-free in this study meant that the elevated IOP was managed off drops: those patients didn’t need medication to maintain their individual target pressures. That’s a huge win for the patient in terms of convenience: it obviates the issues around medication compliance, and we know from other studies that achieving low and stable pressure is a key goal in managing patients with glaucoma.5,6 And so, what the data from HORIZON tell me is that when we use Hydrus, we are able to provide a durable long-term benefit in regards to lowering eye pressure and drop burden for most patients.
The design of the HORIZON Study exceeded the typical requirements for a pivotal trial. There are a couple of unique aspects of the study supporting the robustness of the data. First of all, the study enrolled patients from sites both inside and outside the United States, which is unique among glaucoma studies. The diversity supports that this data is representative of the general patient population. Second, with more than 550 patients, it was the largest pivotal trial in MIGS; the large ‘n’ (sample size) speaks to the robustness of the data. Third, patients were followed out to 5 years, which is noteworthy on its own, but to have 80% retention in a long-term study is truly impressive. All of those are reasons that most likely contributed to why the Hydrus® Microstent received a quality of clinical data rating of ‘moderate quality, strong recommendation,’ the highest rating given among all MIGS, in the 2020 AAO Primary Open-Angle Glaucoma Preferred Practice Pattern guidelines.7
Dr. Radcliffe: You really cannot argue with the quality of the data coming out of HORIZON. We’ve been promised so-called ‘game-changing data’ before, but this feels a little different. We know that IOP is the only known modifiable risk factor for glaucoma. The number of patients, the duration of follow-up, the 80% retention rate at 5 years, durable safety and efficacy… this truly has rewritten what we know and can say about MIGS.
At the 5-year follow-up, 66% of patients in the Hydrus group were medication-free versus 46% in the Control group; and 73% of patients on one medication preoperatively were medication-free versus 48% in the Control group. Why is medication-free status important for patients in the real word?
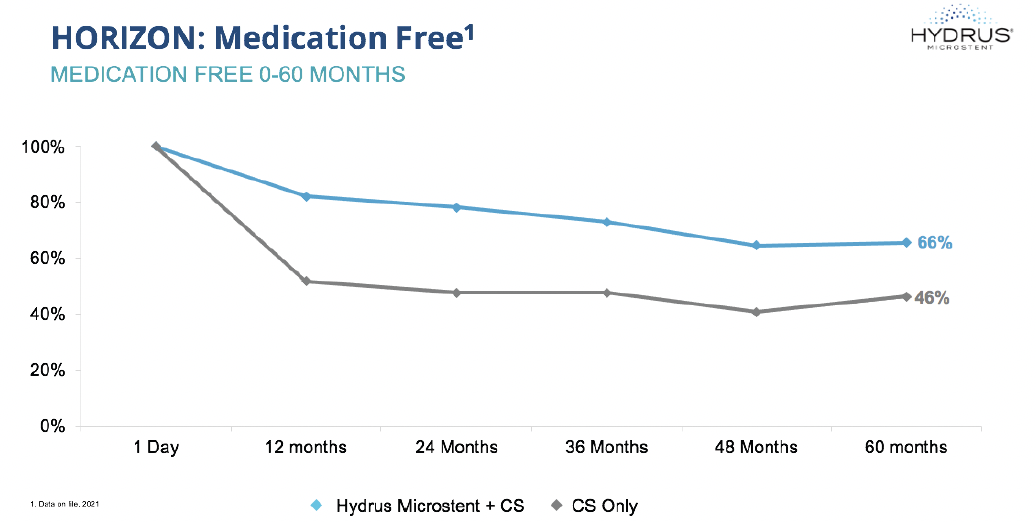
Figure 1. Medication-free rates for the Hydrus + cataract surgery and cataract surgery alone groups at Year 5.
Dr. Radcliffe: My takeaway is that a little more than half the patients in the study were on one medication at baseline, which is almost the same distribution we see among patients in the clinic.8 And so, we get a little insight into the prognosis for the population of patients we see in clinical practice, specifically about the eyes with mild POAG. Historically, we may have delayed intervention a bit for those patients while they were on medication, because if their pressure remains out of control, the next step is to think about a trabeculectomy or drainage device. The safety profile of MIGS changes that; it is amenable to use in earlier-stage disease—and what HORIZON really shows is the benefits of treating glaucoma early. In the Hydrus® Microstent plus cataract surgery group, 3 out of 4 patients on one drop at baseline—ostensibly with mild glaucoma—remained medication-free after 5 years. That is a durable benefit being provided to our patients.
Dr. Singh: Any medication, no matter how perfect it is, will be associated with side effects, and that is certainly true in glaucoma. The adverse event profiles associated with the drops we use to control glaucoma are well-known. But the potential for side effects is only one factor in the complex milieu of medication non-compliance. Our patients experience cost and access issues; they forget to take their drops; and even when they do take them, the actual instillation can be challenging. When we really step back and think about it, all of these factors affect the quality of the patient’s life. If we can do something that eases that burden, it’s a huge win.
Through 5 years, there was a greater than 50% relative reduction in invasive SSI* compared to cataract surgery only at 5 years (2.4% in Hydrus vs 5.3% in CS only). What does this finding mean to you?
Dr. Singh: When I see that a number of patients with mild disease wound up needing an SSI, the message to me is, ‘don’t get complacent.’ HORIZON provided clear evidence that placing a scaffold to maintain the patency of Schlemm’s canal has a significant long-term benefit. I think the benefits we see with Hydrus® Microstent have something to do with restoring the eye’s physiologic outflow by bypassing the trabecular meshwork and dilating Schlemm’s canal, spanning roughly 90°. This should also have a benefit in regard to addressing pressure fluctuations.
Dr. Radcliffe: The cataract-only arm of HORIZON teaches us something very important about the disease. A number of patients with mild disease in both groups required invasive SSI, and there was no way to predict which patients would go on to that fate. This reminds us that POAG is a very serious disease and that it should be treated early. The myth that patients will do fine without intervention can lead to too many people going on to require invasive glaucoma surgery.
I was a monitor for the HORIZON study, so I got to see the charts of patients who went on to need an incisional SSI. Why were they getting surgery? Because their glaucoma was progressing, and you have to ask yourself why that is. Although the eyes in these two groups achieved similar target IOP, there was a greater than 50% relative reduction in the need for incisional SSI* for those who received the Hydrus® Microstent plus cataract surgery compared to those who underwent cataract surgery alone (2.4% in Hydrus vs 5.3% in CS only). We may not be able to say yet with certainty the specific reason, but it highlights why stents are an important part of treating certain types of glaucoma.

What have we learned about the safety of the Hydrus® Microstent from the HORIZON study?
Dr. Radcliffe: It is encouraging to see a MIGS device with long-term safety data from a pivotal trial at 5-years (Table). There was a higher incidence of peripheral anterior synechiae (PAS) in the Microstent group, but that doesn’t necessarily mean worse outcomes. In fact, at 2 years, there was no significant impact in terms of IOP reduction (p = 0.08) for those patients with obstructive PAS.4 There was also no sequelae associated with PAS or any other potential safety concern throughout the study. In regard to endothelial cell loss, the Microstent group showed a slightly greater reduction in endothelial cell count in the immediate postoperative period (3 months), but after the first follow-up and out to 5 years, the rate of progression between both groups remained relatively stable (Figure 2).4
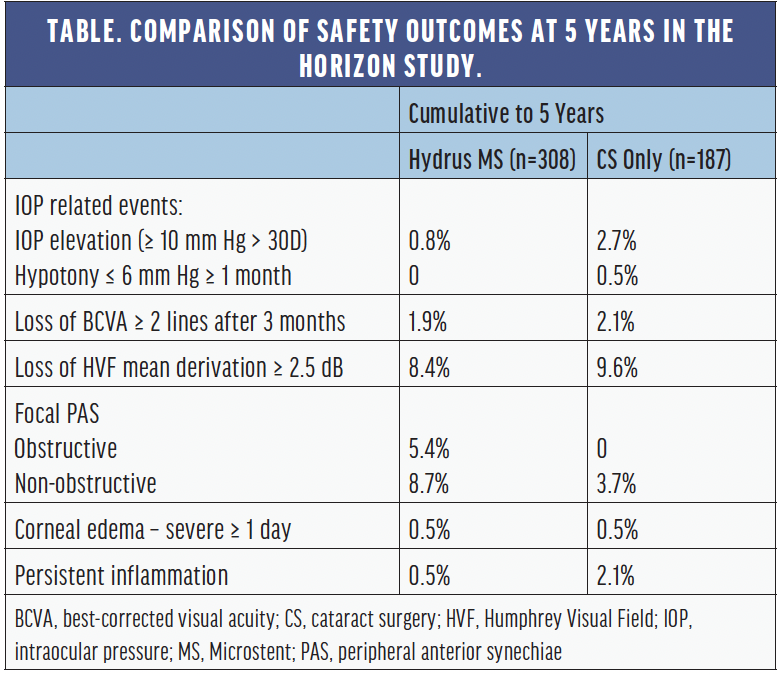
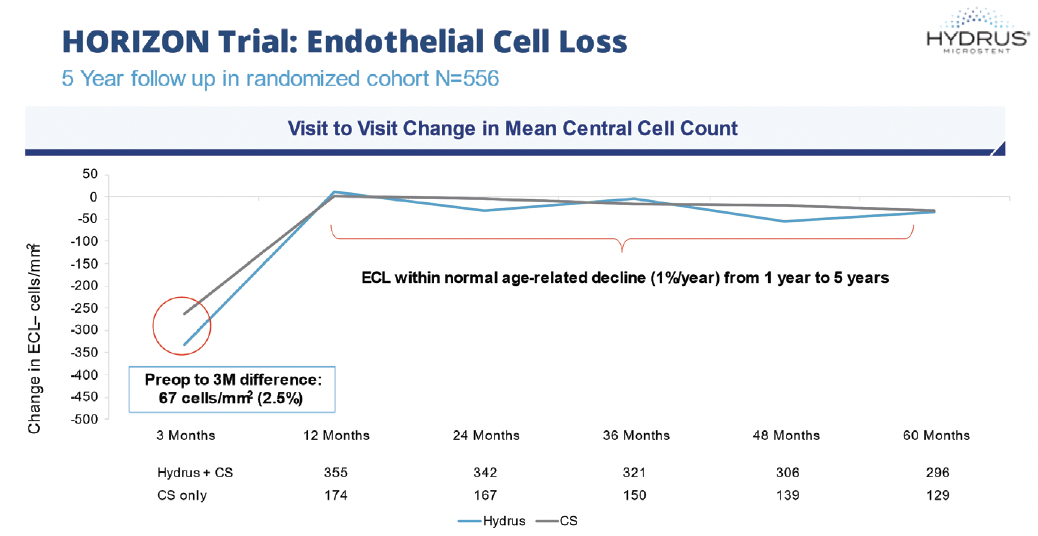
Figure 2. Endothelial cell density in the HORIZON Study: intergroup differences and rates of endothelial cell loss were not statistically significant at any time point.4
Dr. Singh: We talked earlier about what large, randomized trials mean for the MIGS category. Well, this is it: the safety data from the HORIZON trial reinforce what we long believed to be true about the relative safety of these procedures. Specific to the Hydrus® Microstent, we can have a little more confidence, because its safety has been established through 5 years of follow-up in the HORIZON study. In fact, the Hydrus® Microstent is the only MIGS with 5-year pivotal data referenced in its labeling, which wouldn’t be there unless it passed the scrutiny of the FDA.
How do the outcomes from HORIZON shape your clinical decision-making? How do these data impact how you treat patients in the real world?
Dr. Singh: When I see a cataract patient who is also on drops for mild to moderate POAG, I know Hydrus may be a great option because it works on multiple areas of resistance, bypassing TM, holding the canal open, and gaining access to 90° of the distal system. I can now say confidently that this treatment option is likely to have a long-term impact on patients treated with Hydrus—including mean IOP reduction and the potential to eliminate drops—because we have data to back it up.4 The data confirm patients do progress, and even a mild patient can progress within 5 years to needing an incisional glaucoma surgery if they are not adequately controlled. Reducing IOP is important but reducing the drop burden is as well. The HORIZON study has now shown that achieving both is possible.4 For me, a glaucoma patient undergoing cataract surgery on medications is going to be getting some type of MIGS procedure. We now have to find reasons to exclude a patient rather than finding the ‘right’ patient for MIGS.
Dr. Radcliffe: I think that is a reasonable approach based on the cumulative evidence from HORIZON. The study’s 2-year data led to the FDA approval of the Hydrus® Microstent, so it was certainly subjected to rigorous clinical testing.2 At 5 years, we now see evidence of long-term safety as well as efficacy when looking at measures such as medication free rates and the occurrence of incisional SSIs.4 The real essence of the interventional mindset is finding solutions for our patients that do a good job of lowering eye pressure and reducing medication burden. The objective of MIGS is to address each of these goals. And with that mindset, the clinician’s judgement becomes that much more important in deciding the best option for each patient. At the same time, the decision to offer a MIGS device like Hydrus can be made with greater confidence with the data we now have from HORIZON.
*SSI=Secondary Surgical Intervention. Includes: trabeculectomy, tube shunt, gel stent, ECP/TSCP, non-penetrating. (9/369 Hydrus and 10/187 CS)
1. Pereira ICF, van de Wijdeven R, Wyss HM, et al. Conventional glaucoma implants and the new MIGS devices: a comprehensive review of current options and future directions. Eye (Lond). 2021;35(12):3202-3221.
2. Samuelson TW, Chang DF, Marquis R, et al; HORIZON Investigators. A schlemm canal microstent for intraocular pressure reduction in primary open-angle glaucoma and cataract: The HORIZON Study. Ophthalmology. 2019;126(1):29-37.
3. Ahmed IIK, Rhee DJ, Jones J, et al; HORIZON Investigators. Three-year findings of the HORIZON Trial: a schlemm canal microstent for pressure reduction in primary open-angle glaucoma and cataract. Ophthalmology. 2021;128(6):857-865.
4. Ahmed IIK, De Francesco T, Rhee D, et al; HORIZON Investigators. Long-term outcomes from the HORIZON Randomized Trial for a schlemm’s canal microstent in combination cataract and glaucoma surgery. Ophthalmology. 2022;129(7):742-751.
5. Musch DC, Gillespie BW, Niziol LM, Lichter PR, Varma R; CIGTS Study Group. Intraocular pressure control and long-term visual field loss in the Collaborative Initial Glaucoma Treatment Study. Ophthalmology. 2011;118(9):1766-73.
6. The Advanced Glaucoma Intervention Study (AGIS): 7. The relationship between control of intraocular pressure and visual field deterioration .The AGIS Investigators. Am J Ophthalmol. 2000 Oct;130(4):429-40.
7. Gedde SJ, Vinod K, Wright MW, et al. Primary Open-Angle Glaucoma Preferred Practice Pattern®. Ophthalmology. 2021;128(1):PP71-P150.
8. Marketscope. 2021 Glaucoma Surgical Device Market Report: Global Analysis for 2020 to 2026, July, 2021. Available at: https://www.market-scope.com/pages/reports/267/2021-glaucoma-surgical-device-market-report.
IMPORTANT PRODUCT INFORMATION
CAUTION: Federal law restricts this device to sale by or on the order of a physician.
INDICATIONS FOR USE: The Hydrus Microstent is indicated for use in conjunction with cataract surgery for the reduction of intraocular pressure (IOP) in adult patients with mild to moderate primary open-angle glaucoma (POAG).
CONTRAINDICATIONS: The Hydrus Microstent is contraindicated under the following circumstances or conditions: (1) In eyes with angle closure glaucoma; and (2) In eyes with traumatic, malignant, uveitic, or neovascular glaucoma or discernible congenital anomalies of the anterior chamber (AC) angle.
WARNINGS: Clear media for adequate visualization is required. Conditions such as corneal haze, corneal opacity or other conditions may inhibit gonioscopic view of the intended implant location. Gonioscopy should be performed prior to surgery to exclude congenital anomalies of the angle, peripheral anterior synechiae (PAS), angle closure, rubeosis and any other angle abnormalities that could lead to improper placement of the stent and pose a hazard. The surgeon should monitor the patient postoperatively for proper maintenance of intraocular pressure. The surgeon should periodically monitor the status of the microstent with gonioscopy to assess for the development of PAS, obstruction of the inlet, migration, or device-iris or device-cornea touch. The Hydrus Microstent is intended for implantation in conjunction with cataract surgery, which may impact corneal health. Therefore, caution is indicated in eyes with evidence of corneal compromise or with risk factors for corneal compromise following cataract surgery. Prior to implantation, patients with history of allergic reactions to nitonal, nickel or titanium should be counseled on the materials contained in the device, as well as potential for allergy/hypersensitivity to these materials.
PRECAUTIONS: If excessive resistance is encountered during the insertion of the microstent at any time during the procedure, discontinue use of the device. The safety and effectiveness of use of more than a single Hydrus Microstent has not been established. The safety and effectiveness of the Hydrus Microstent has not been established as an alternative to the primary treatment of glaucoma with medications, in patients 21 years or younger, eyes with significant prior trauma, eyes with abnormal anterior segment, eyes with chronic inflammation, eyes with glaucoma associated with vascular disorders, eyes with preexisting pseudophakia, eyes with pseudoexfoliative or pigmentary glaucoma, and when implantation is without concomitant cataract surgery with IOL implantation. Please see a complete list of Precautions in the Instructions for use.
ADVERSE EVENTS: The most frequently reported finding in the randomized pivotal trial was peripheral anterior synechiae (PAS), with the cumulative rate at 5 years (14.6% vs 3.7% for cataract surgery alone). Other Hydrus postoperative adverse events reported at 5 years included partial or complete device obstruction (8.4%) and device malposition (1.4%). Additionally, there were no new reports of persistent anterior uveitis (2/369, 0.5% at 2 years) from 2 to 5 years postoperative. There were no reports of explanted Hydrus implants over the 5-year follow-up. For additional adverse event information, please refer to the Instructions for Use.
MRI INFORMATION: The Hydrus Microstent is MR-Conditional meaning that the device is safe for use in a specified MR environment under specified conditions.
Please see the Instructions for Use for complete product information.





