Introduction
Accurate axial length (AL) measurements are an essential element to calculate the precise IOL power. Ever since the introduction of optical biometry, all biometers converted the optical path length to a geometric AL measurement using a Mean Group Refractive Index. A newer approach uses individual refractive indices to measure each segment of the eye, a method referred to as the Sum-of-Segments (SOS).
The SOS method sums up the geometric lengths of each segment in the eye to determine the AL. For each segment, a specific refractive index for conversion from the optical to geometric lengths is used (1.375 for the cornea, 1.336 for the aqueous and vitreous, and 1.41 for the lens). This approach is being utilized by the Argos biometer (Movu Inc.).
On the other hand, the older method applies a Mean Group Refractive Index equivalent to convert the optical into the geometrical AL. The following equation was introduced by Haigis et al1 for the first IOLMaster biometer: AL = (OPL/1.3549 - 1.3033) / 0.9571. Similar conversion equations are used in other SS-OCT biometers such as in IOLMaster 700 (ZEISS).
The question is, does the AL measurement method make a difference in IOL power calculations?
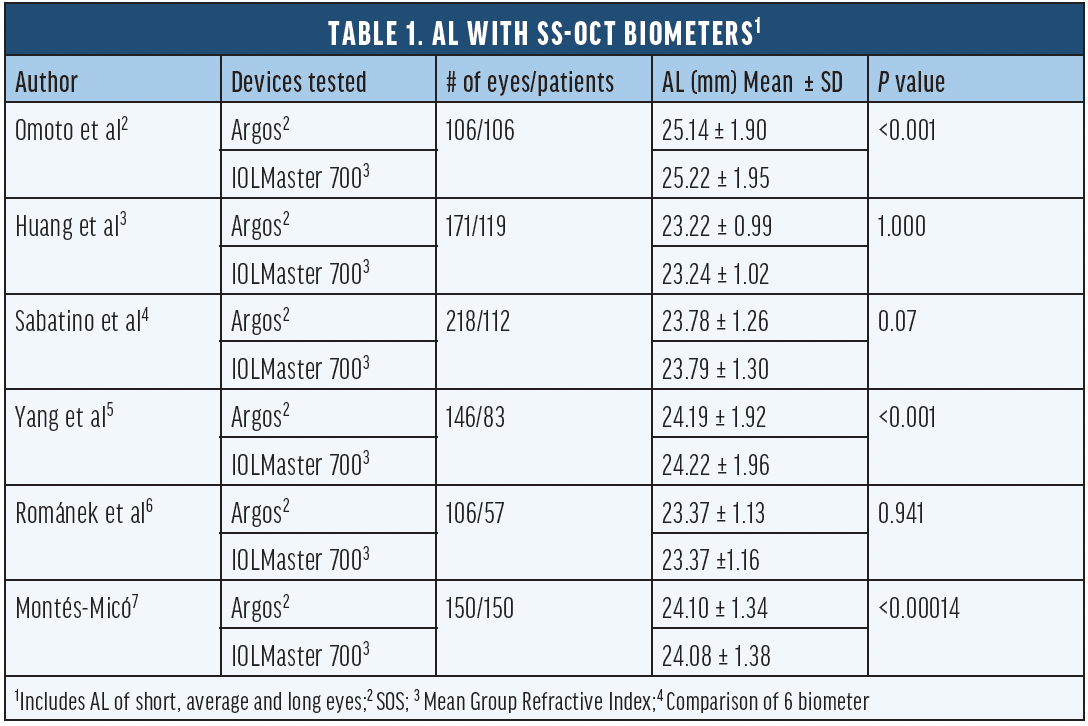
Several authors have compared SS-OCT biometers (Table 1). In about 50% of the reports, the AL was significantly different between biometers. Significant differences were detected when the AL exceeded an average of 24.08 mm, while no differences were found in eyes that ranged on average from 23.22 to 23.79 mm.
The impact on IOL power calculations
The SOS method may be particularly beneficial for eyes that are shorter or longer than average.8-10 Omoto et al2 reported that the IOLMaster 700 measured eyes significantly longer.2 The prediction error was not significantly impacted, although the percentage of eyes within 0.5 D was consistently higher with Argos in long eyes.2
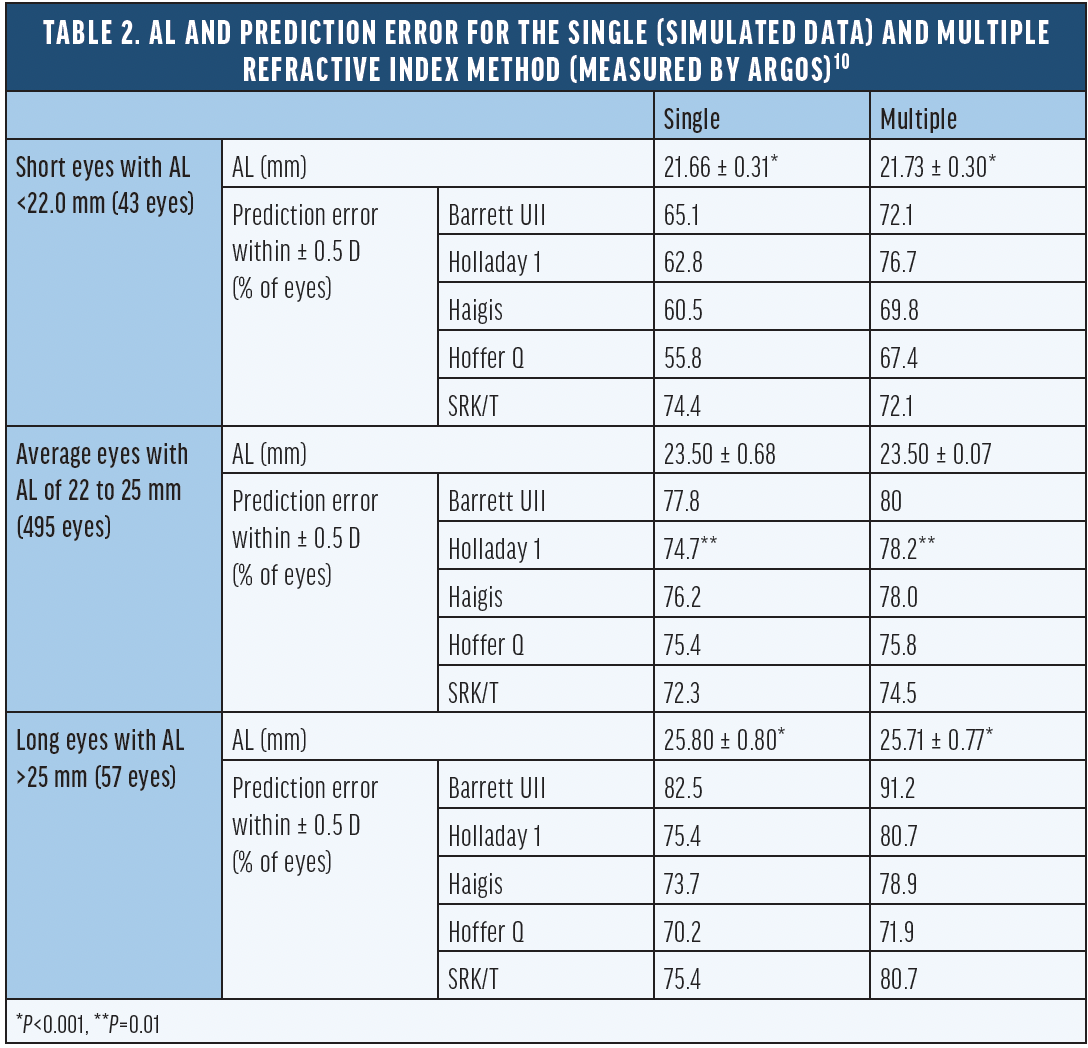
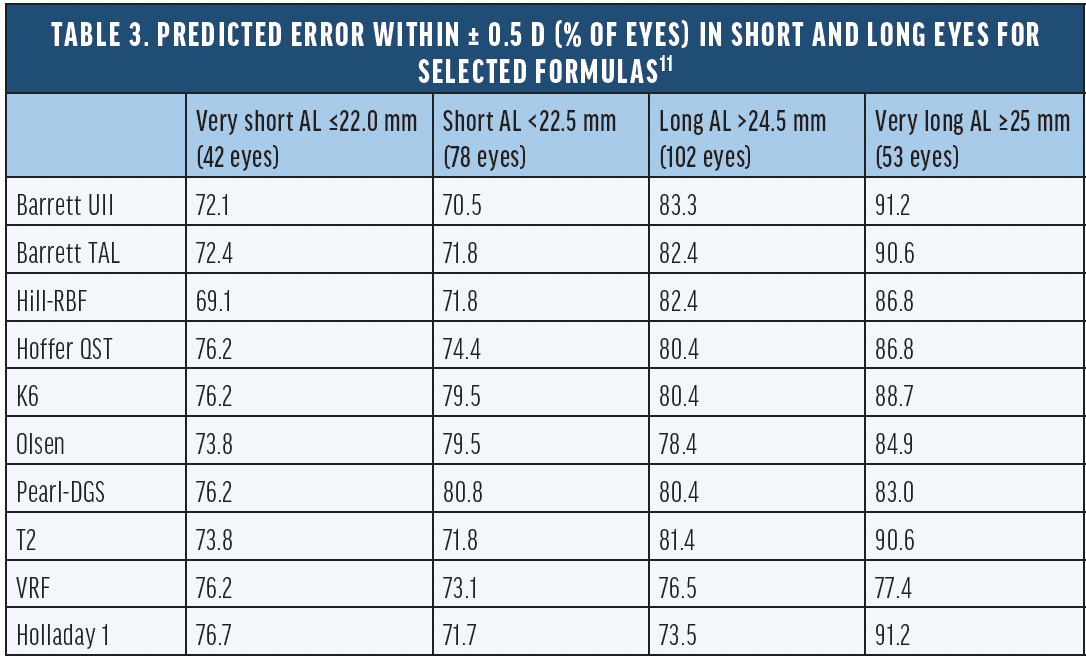
A large analysis performed by Shammas et al10 investigated the effect of AL determination based on the single refractive index and multiple refractive indices on IOL power calculations in short, average, and long eyes. The AL differed significantly in short and long eyes between methods, and the impact on IOL power calculations was small (Table 2). However, newer formulas may be impacted more significantly when using SOS, and the effect was investigated by calculating the expected residual refractions in a follow up study by Shammas et al.11 The analysis showed that newer formulas performed equal or better than the traditional formulas with the SOS biometry. For short and very short eyes, K6 and Pearl-DGS performed best, while in long and very long eyes, Barrett Universal II and Barrett True Axial Length provided the highest percentage of eyes within a predicted error within ± 0.5 D (Table 3).
Conclusion
AL determined with the Mean Group Refractive Index seems to produce measurements that are slightly shorter in short eyes and longer in long eyes. Depending on the length of the eye, some IOL power calculation formulas may provide better outcomes with the SOS method.
1. Haigis W, Lege B, Miller N, Schneider B. Comparison of immersion ultrasound biometry and partial coherence interferometry for intraocular lens calculation according to Haigis. Graefes Arch Clin Exp Ophthalmol. 2000;238(9):765-773.
2. Omoto MK, Torii H, Masui S, Ayaki M, Tsubota K, Negishi K. Ocular biometry and refractive outcomes using two swept-source optical coherence tomography-based biometers with segmental or equivalent refractive indices. Sci Rep. 2019;9(1):6557.
3. Huang J, Chen H, Li Y, et al. Comprehensive comparison of axial length measurement with three swept-source OCT-based biometers and partial coherence interferometry. J Refract Surg. 2019;35(2):115-120.
4. Sabatino F, Matarazzo F, Findl O, Maurino V. Comparative analysis of 2 swept-source optical coherence tomography biometers. J Cataract Refract Surg. 2019;45(8):1124-1129.
5. Yang CM, Lim DH, Kim HJ, Chung TY. Comparison of two swept-source optical coherence tomography biometers and a partial coherence interferometer. PLoS One. 2019;14(10):e0223114.
6. Romanek J, Slukova K. Comparison of optical biometers argos and iol master 700. Cesk Slov Oftalmol. 2021;77(6):295-299.
7. Montes-Mico R. Evaluation of 6 biometers based on different optical technologies. J Cataract Refract Surg. 2022l48(1):16-25.
8. Cooke DL, Cooke TL. A comparison of two methods to calculate axial length. J Cataract Refract Surg. 2019;45(3):284-292.
9. Wang L, Cao D, Weikert MP, Koch DD. Calculation of axial length using a single group refractive index versus using different refractive indices for each ocular degment: theoretical study and refractive outcomes. Ophthalmology. 2019;126(5):663-670.
10. Shammas HJ, Shammas MC, Jivrajka RV, Cooke DL, Potvin R. Effects on IOL power calculation and expected clinical outcomes of axial length measurements based on multiple vs single refractive indices. Clin Ophthalmol. 2020;14:1511-1519.
11. Shammas HJ, Taroni L, Pellegrini M, Shammas MC, Jivrajka RV. Accuracy of newer Iol power formulas in short and long eyes using sum-of-segments biometry. J Cataract Refract Surg. 2022.
Important Patient Information for ARGOS® Optical Biometer
Caution: Federal (USA) law restricts this device to the sale by or on the order of a physician.
Indication: ARGOS® is a non-invasive, noncontact biometer based on swept-source optical coherence tomography (SS-OCT). The device is intended to acquire ocular measurements as well as perform calculations to determine the appropriate intraocular lens (IOL) power and type for implantation during intraocular lens placement.
Intended Use: The Reference Image functionality is intended for use as a preoperative and postoperative image capture tool. It is intended for use by ophthalmologists, physicians, and other eye-care professionals and may only be used under the supervision of a physician.
Warnings / Precautions:
• Only properly trained personnel with experience may operate the device and control software and interpret the results.
• Factors that influence the measurement of patient’s eyes are listed in the User Manual (Table 1): pseudophakic eye, wearing contact lenses, fixation problem, cornea opacity, non-intact cornea, refractive surgery, blood in the vitreous humor, retinal detachment, keratoconus, asteroid hyalosis, ambient light in the room, and deformation of the corneal shape. Please consider the guidance provided in Table 1 when you encounter these factors.
• Optical Radiation - This device is equipped with a Class 1 laser light source.
Attention: Refer to the ARGOS® User Manual for a complete description of proper use and maintenance, optical and technical specifications, as well as a complete list of warnings and precautions.
© 2022 Alcon Inc. 09/22 US-ARB-2200109





