Key Takeaways
- Excisional goniotomy has become a mainstay of contemporary interventional glaucoma care.
- An understanding of the evolution of goniotomy provides context for why angle-based procedures have become a cornerstone of contemporary interventional glaucoma care.
- The devices currently available are designed for use through a clear corneal incision, facilitating seamless integration into phaco workflows or use as a standalone procedure.
When I was in residency in the late 1990s, I was taught that goniotomy was reserved for pediatric glaucoma and that the procedure did not work well in adult patients. For the Ophthalmic Knowledge Assessment Program, my peers and I also memorized that the juxtacanalicular trabecular meshwork was the path of highest resistance in glaucoma. I, like many others, never challenged the contradiction. Thankfully, Malik Y. Kahook, MD, and others not only challenged the status quo but also pioneered the microinvasive goniotomy procedures that are widely used today.
Tal Raviv, MD



Glaucoma treatment is no longer confined to subspecialty care or late-stage disease. Advances in visualization, instrumentation, and surgical philosophy have transformed angle surgery into a practical, efficient, and increasingly familiar part of the cataract OR. Understanding how goniotomy evolved provides context for why angle-based procedures have become a cornerstone of contemporary interventional glaucoma care.
A BRIEF HISTORY OF GONIOSCOPY
The term gonioscopy was first documented in 1898, when the Greek ophthalmologist Alexios Trantas described visualization of the iridocorneal angle through scleral depression combined with indirect ophthalmoscopy.1 Interest in gonioscopy expanded rapidly in the early 1920s, largely thanks to Austrian ophthalmologist and artist Maximilian Salzmann, who recognized that the total internal reflection of the cornea could be overcome by using a convex contact lens, enabling consistent visualization of angle anatomy and pathology.2,3 This discovery laid the foundation for modern gonioscopy and fundamentally reshaped the diagnostic and therapeutic approach to glaucoma.
In that same decade, early slit-lamp technology was introduced, and convex contact lenses were refined to allow direct angle visualization.1-3 Building on these advances, Dr. Otto Barkan formalized modern goniotomy techniques, primarily for congenital glaucoma. Using a Koeppe lens and a slit lamp, Dr. Barkan developed an ab interno approach to incise the trabecular meshwork with a knife under direct visualization.4 He hypothesized that congenital glaucoma resulted from an embryonic membrane overlying the trabecular meshwork, a theory later disproven.3,4 By the early 1950s, the juxtacanalicular trabecular meshwork was identified as the principal site of aqueous outflow resistance.5 Nonetheless, Dr. Barkan’s central concept—bypassing or removing trabecular meshwork resistance to improve aqueous outflow—became foundational to modern MIGS.
FROM BYPASS TO PRECISION: THE RISE OF MIGS
For much of the 20th century, adult glaucoma surgery centered on invasive surgeries, including trabeculectomy and tube shunts, that were designed to bypass the trabecular meshwork entirely. Although effective, these surgeries are associated with significant risks, intensive postoperative care, and variable predictability—factors that limit their appeal for the treatment of mild to moderate disease.
The early 2000s marked a paradigm shift with the emergence of MIGS. These procedures aim to improve safety, reproducibility, and efficiency while targeting the eye’s natural outflow pathway.6 For cataract surgeons in particular, MIGS expands the opportunity to address glaucoma at the time of cataract surgery, reshaping glaucoma treatment algorithms from medication first to earlier surgical intervention.
REIMAGINING GONIOTOMY FOR ADULT EYES
Dr. Barkan’s goniotomy was revolutionary, but early attempts to apply the technique in adults had limited success.5 Histopathologic studies revealed collateral tissue damage caused by blunt or nonspecific instruments ill-suited to the delicate anatomy of the trabecular meshwork and Schlemm canal.7
Technological innovation in the early 2000s reignited interest in the procedure. The Trabectome (MicroSurgical Technology) was the first modern MIGS device designed for ab interno removal of the trabecular meshwork. Using electrocautery with integrated irrigation and aspiration, the Trabectome enabled controlled ablation of trabecular meshwork tissue while maintaining chamber stability and visualization.8 This marked a critical step in transitioning goniotomy from a concept to a reproducible procedure.
PURPOSE-BUILT PRECISION
Kahook Dual Blade
The Kahook Dual Blade (KDB) was developed by one of the authors (M.Y.K.) in collaboration with New World Medical. Introduced in 2015, the KDB is the first US FDA-registered goniotomy blade.
Unlike traditional goniotomy tools that incise the trabecular meshwork, the KDB was designed to excise a continuous strip of diseased tissue. The device’s pointed tip and ramp elevate the trabecular meshwork and place it on tension, while dual blades remove the tissue cleanly, creating direct access to Schlemm canal without residual leaflets. The tapered sides and rounded heel of the device allow smooth advancement across multiple clock hours of tissue with minimal disruption to adjacent structures.7
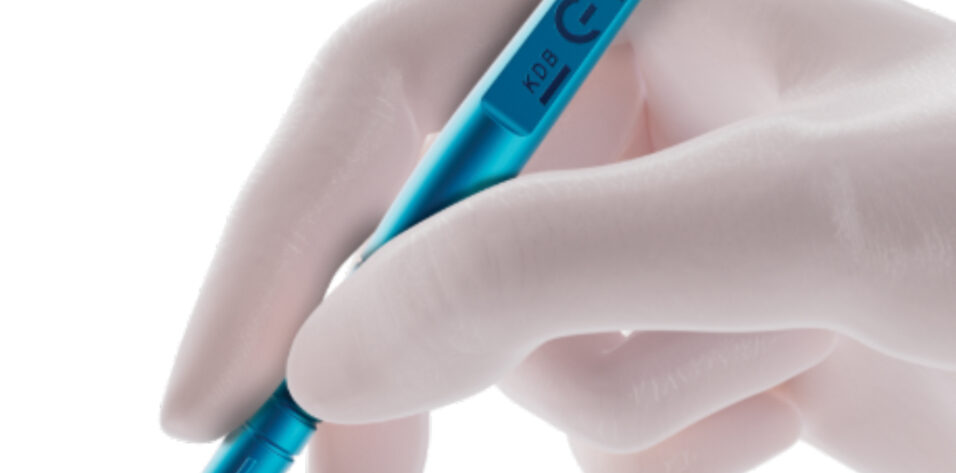
Since the KDB’s introduction, its design has evolved. The most recent iteration, the KDB Glide (New World Medical; Figure), refines the original excisional goniotomy concept with enhancements intended to facilitate smoother device advancement and improve control during tissue engagement. These incremental design updates reflect a broader maturation of goniotomy as a reproducible, purpose-built procedure suited for adult eyes.

Figure. KDB Glide.
Additional Options
Since the KDB’s introduction, several other MIGS devices have been specifically developed—or adapted—to provide additional ways to perform a goniotomy. The iTrack (Nova Eye Medical) was originally designed to deliver an OVD into the canal using an ab externo approach. Later, however, the device was adapted for ab interno cannulation of the canal and pulled out to perform a 360º goniotomy, a procedure termed gonioscopy-assisted transluminal trabeculotomy. A later modification of this technique utilizes a polypropylene suture to accomplish the same procedure.
The Omni Surgical System (Sight Sciences) was designed to deliver a microcatheter around 180º of Schlemm canal via a clear corneal incision and can then be used to tear through the trabecular meshwork. Later, the Sion Surgical Instrument (Sight Sciences) was developed as a goniotomy device with a bladeless design and tissue collection window.
In 2025, the Via360 Surgical System (New World Medical) received US FDA 510(k) clearance for the delivery of controlled amounts of an OVD around 360º of Schlemm canal. The device can be used for goniotomy when the catheter is pulled through. The Streamline Surgical System (New World Medical) also delivers an OVD during ophthalmic surgery and is commonly used for canaloplasty. The system, however, also features a separate class 1 exempt function for cutting trabecular meshwork tissue, which allows goniotomy to be performed independently of OVD delivery.
Relevance
Of particular relevance for cataract surgeons, all of these devices are designed for use through a clear corneal incision, facilitating seamless integration into phaco workflows or use as a standalone procedure. This provides an opportunity to align intervention with surgeon preference and to tailor treatment to the individual patient.
CONCLUSION
Excisional goniotomy has become a mainstay of contemporary interventional glaucoma care, particularly for surgeons seeking effective options that align with today’s cataract surgery environment. Nevertheless, glaucoma remains a leading cause of irreversible vision loss worldwide. Continued innovation in angle-based surgery is essential to improving patients’ access to safe, high-quality glaucoma care and supporting long-term outcomes.
1. Dellaporta A. Historical notes on gonioscopy. Surv Ophthalmol. 1975;20(2):137-149.
2. Alward WLM. A history of gonioscopy. Optom Vis Sci. 2011;88(1):29-35.
3. Barkan M. On the genesis of glaucoma. Am J Ophthalmol. 1936;19(3):209-215.
4. Barkan M. Technic of goniotomy for congenital glaucoma. Arch Ophthalmol. 1949;41(1):65-82.
5. Johnson MMJ, Douglas H. How does nonpenetrating glaucoma surgery work? Aqueous outflow resistance and glaucoma surgery. J Glaucoma. 2001;10(1):55-67.
6. Chan PPM, Larson MD, Dickerson JE Jr, et al. Minimally invasive glaucoma surgery: latest developments and future challenges. Asia Pac J Ophthalmol (Phila). 2023;12(6):537-564.
7. Ammar DA, Seibold LK, Kahook MY. Preclinical investigation of goniotomy using four different techniques. Clin Ophthalmol. 2020;14:3519-3525.
8. Francis BA, See RF, Rao NA, Minckler DS, Baerveldt G. Ab interno trabeculectomy: development of a novel device (Trabectome) and surgery for open-angle glaucoma. J Glaucoma. 2006;15(1):68-73.