Key Takeaways
- Dry eye disease management starts by identifying the dominant mechanism through symptom assessment, targeted ocular surface examination, and focused testing rather than treating DED as a single entity. Specifying the pathology found on examination guides therapy more precisely than relying on the umbrella diagnosis alone.
- Improved ocular surface signs do not rule out nerve-mediated ocular pain when symptoms persist. Reassessment should evaluate peripheral, central, and autonomic nerve dysfunction, especially in autoimmune disease, migraine, fibromyalgia, postsurgical pain, or when symptoms appear disproportionate to surface findings.
- Mixed dry eye and ocular pain often require multimodal, mechanism-targeted management rather than a single intervention. An individually acceptable Goldilocks state is reached through the right combination of topical therapies, systemic medications, devices, and patient education, with time and stepwise adjustment.

Dry eye disease (DED) is not a single condition but rather a spectrum of symptoms and signs arising from multiple, often overlapping mechanisms. A treatment that works well for one patient may offer little benefit—or may be inappropriate—for another. This variability became more relevant with the US FDA approval of a growing number of therapies under the broad label of DED.
For clinicians, the challenge is not simply choosing from an expanding list of therapies but also determining which mechanism is most relevant for a given patient and selecting treatment accordingly. A mechanism-based approach to DED management begins with careful attention to the history, examination, and targeted testing. This article uses a case example to illustrate how I apply this framework in everyday practice.
CASE PRESENTATION
A 55-year-old White woman was referred for a DED evaluation. She described episodic ocular itching and burning that began during her time in the US Army and gradually progressed to chronic daily symptoms. Despite instilling artificial tears more than eight times daily, she experienced little meaningful relief.
Her medical history was notable for chronic knee and neck pain, migraine, dry mouth, Hashimoto thyroiditis without evidence of thyroid eye disease, and Ehlers-Danlos syndrome.
DEFINING THE DOMINANT MECHANISM
A systematic symptom assessment is a critical first step in DED management. Standard questionnaires can help clarify symptom domains. For example, the 5-Item Dry Eye Questionnaire focuses on dryness, discomfort, and tearing, whereas the Ocular Surface Disease Index captures pain, light sensitivity, wind sensitivity, visual disturbance, and functional limitations. Notably, the Ocular Surface Disease Index does not ask about dryness specifically despite this survey’s widespread use in dry eye populations.
In addition to subjective questionnaires, I ask patients to rate their ocular pain independent of symptom descriptors. In this case, on a scale of 10, the patient rated her pain a six at the visit and an eight at its worst during the prior week.
The examination begins as soon as I enter the room. I pay particular attention to dermatologic findings and anatomic features that could influence the individual’s ocular symptoms. This patient had facial rosacea, but her eyelid anatomy, blink rate, and lid position were normal (Figure 1).
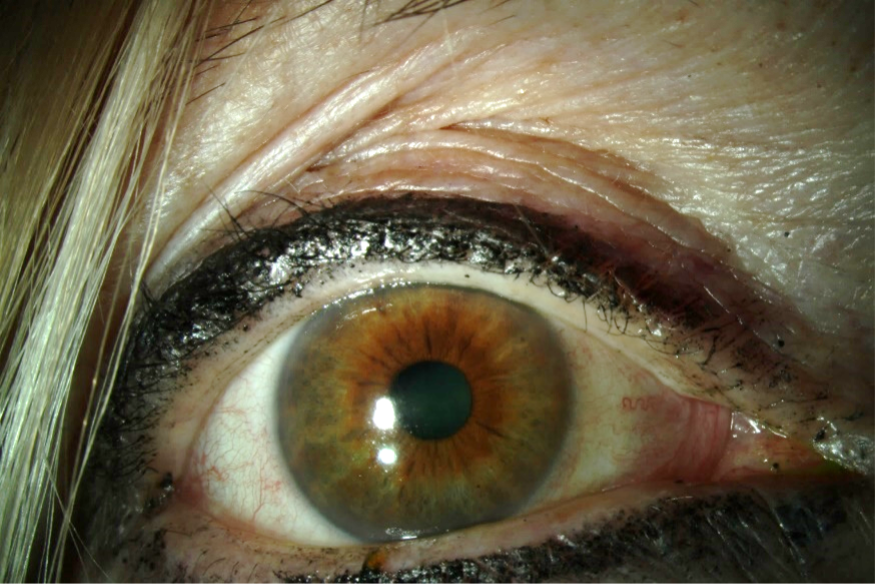
Figure 1. External photograph showing facial rosacea with otherwise normal eyelid anatomy.
Point-of-care testing can provide additional context. In this case, InflammaDry (QuidelOrtho) testing for matrix metalloproteinase-9 showed only a faint pink stripe, suggesting minimal active ocular surface inflammation (Figure 2). A focused but comprehensive ocular surface examination revealed several findings consistent with meibomian gland dysfunction, including poor meibum quality and lid margin vascularity, as well as epithelial disruption and reduced tear production on Schirmer testing at 3 mm in each eye.

Figure 2. InflammaDry showing a faint positive pink line, consistent with minimal active ocular surface inflammation based on qualitative matrix metalloproteinase-9 detection.
These findings supported a diagnosis of aqueous-deficient DED with coexisting rosacea-associated meibomian gland dysfunction. Given the low tear production, serologic testing was pursued. Although classic Sjögren antibodies (SSA and SSB) were negative, antibodies directed against lacrimal and salivary gland proteins—sometimes referred to as early Sjögren markers—were present. Although these markers are not predictive of future Sjögren syndrome development, their presence led me to suspect an immune-mediated contribution to the patient’s DED symptoms and signs.
TREATMENT AND REASSESSMENT
Immunomodulatory therapy was initiated. As is often my practice, a sequential trial was conducted of T-cell-directed therapies—three cyclosporine formulations and lifitegrast (Xiidra, Novartis)—to identify the option that was best tolerated by and most effective for the patient. In my experience, some patients clearly prefer cyclosporine-based therapy, others prefer lifitegrast, and still others tolerate neither.1 I cannot reliably predict these preferences in advance, which underscores the need for better diagnostic biomarkers.
In this case, immunomodulatory treatment led to a clear improvement in objective signs. Tear production normalized to more than 10 mm, and epithelial integrity improved. The patient’s symptoms, however, persisted. This disconnect highlights a critical clinical reality: findings on examination do not always correspond directly to the mechanisms causing symptoms.
WHEN SIGNS IMPROVE BUT SYMPTOMS PERSIST
Persistent symptoms despite an improvement in ocular surface parameters suggest an alternative or additional mechanism, most commonly nerve-mediated pain. This scenario is particularly common in patients with autoimmune disease, chronic pain conditions, or migraine, which is itself a chronic pain disorder. For that reason, an assessment of corneal and periocular nerve function is a routine part of my examination.
This patient had classic neuropathic symptoms, including ocular burning and sensitivity to light and wind. I use the Neuropathic Pain Symptom Inventory modified for the Eye,2 but focused questioning can often provide similar insight. Corneal sensitivity testing with a cotton wisp demonstrated asymmetry, with hyperesthesia in the right eye and normal sensation in the left. A topical anesthetic challenge reduced the patient’s pain from a five to a three on a scale of 10 in each eye, indicating partial relief but persistent pain. Palpation of the periocular skin did not elicit cutaneous allodynia (sensitivity to light touch).
The findings were consistent with a mixed pain phenotype, with evidence of peripheral nerve hypersensitivity and a likely nonocular, potentially central, contribution to pain, as suggested by persistent symptoms despite topical anesthesia.
A LAYERED MANAGEMENT PLAN
Management shifted accordingly. When nerve dysfunction contributes to ocular pain, patient education becomes essential because there is rarely a single immediate solution. Improvement typically requires time, combination therapy, and stepwise refinement.
Given the evidence of peripheral nerve involvement, therapy with autologous serum tears was initiated at a 20% concentration and later increased to 40%, administered four to six times daily. The patient reported partial but insufficient improvement. Several peripheral nerve–targeted therapies—including insulin, nerve growth factor, transient receptor potential vanilloid 1 antagonists, and ChemR23 agonists—are currently under investigation and may expand future treatment options.
To address potential central contributors, oral neuromodulation was introduced with low-dose naltrexone, titrated from 2 to 4.5 mg nightly. Treatment further improved but did not fully control the patient’s symptoms. Autonomic testing revealed both symptoms and objective evidence of dysautonomia, prompting initiation of vagal nerve stimulation. I also recommended she wear FL-41 tinted lenses to reduce her light sensitivity and address her migraine-associated photophobia.
Ultimately, the patient achieved adequate relief with a multimodal regimen that included autologous serum tears 40% instilled six times daily, preservative-free artificial tears instilled as needed, twice-daily lid hygiene, low-dose naltrexone 4.5 mg administered nightly, the use of a vagal nerve stimulator, FL-41 tinted lens wear, and active engagement in understanding the mechanisms underlying her symptoms. In real-world practice, access to care, out-of-pocket costs, and treatment burden can shape which treatment combinations are feasible.
CONCLUSION
This case example illustrates several principles central to a mechanism-based approach to managing DED and ocular pain:
- First, the term DED should be used thoughtfully. Whenever possible, the specific pathology identified on examination should be described in lieu of the umbrella label.
- Second, identifiable abnormalities should be treated, and the patient should be reassessed if DED signs improve without a parallel improvement in symptoms.
- Third, peripheral, central, and autonomic nerve dysfunction warrant consideration, particularly in patients with autoimmune disease, migraine, fibromyalgia, postsurgical pain, or a symptom burden that appears disproportionate to surface findings.
- Finally, most patients can reach an individually acceptable Goldilocks state through the right combination of topical therapies, systemic medications, devices, and education, but time and adjustment are often required.
Better diagnostic algorithms and biomarkers are clearly needed to distinguish inflammatory, nociceptive, and neuropathic drivers more precisely. Progress in this area could allow clinicians and patients to develop effective, personalized treatment strategies with less trial and error.
1. Locatelli EVT, Acuna KA, Betz J, Tovar AA, Galor A. Comparison of subjective responses to cyclosporine 0.05% versus lifitegrast 5.0% in individuals with dry eye disease. Cornea. 2024;43(1):88-94.
2. Farhangi M, et al. Modification of the Neuropathic Pain Symptom Inventory for use in eye pain (NPSI-Eye). Pain. 2019;160(7):1541-1550.




