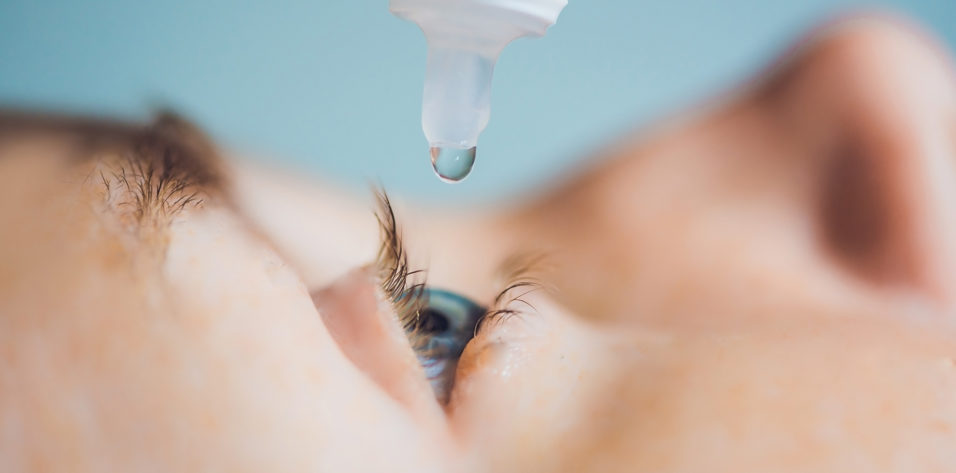
In my opinion, there is nothing more challenging and disruptive to the workflow of a refractive cataract surgery practice than a patient who has dry eyes. Several years ago, I was optimistic about the potential of novel diagnostic equipment and techniques to help manage ocular surface disease (OSD). I had hoped these products would allow me to efficiently and effectively treat dry eye patients on my own, but I feel as though the dry eye market has become oversaturated.
There are now many diagnostic tests and approaches to treatment that a physician must consider: tear osmolarity, the inflammatory marker matrix metalloproteinase-9, Schirmer testing, tear breakup time, corneal aethesiometry, intense pulsed light therapy, different types of artificial tear drops, punctal plugs, and many more. At the 2018 Annual Meeting of the AAO in Chicago, I saw no fewer than 10 new devices or treatment modalities for OSD.
Thankfully there has been some help to navigate these myriad treatment options with the Cornea, External Disease, and Refractive Society (CEDARS) algorithm, the Tear Film and Ocular Surface Society Dry Eye Workshop II (TFOS DEWS II) report,1 and the ASCRS algorithm. However, many providers I talk to seem to have their own magic formulas to manage dry eye patients that continue to evolve and change. This may be due to the fact that many physicians have too little time and energy to research, purchase, and integrate new approaches into their practices. Most of us are so busy with our current preferences that there is little motivation to take on this burden.
My practice has been struggling for years to create a dry eye center of excellence. Our surgeons are too busy to add in this layer of patient care, and our optometrists are equally overwhelmed from performing routine eye care and comanaging surgical patients. Thus far, our most successful effort has been through the hiring of a physician assistant (PA). Our PA has undergone informal training through observation and hands-on assistance of doctors in our practice. She truly enjoys this aspect of patient care and runs a specialized clinic for the management of OSD. However, there is still only one of her to treat a rapidly growing population of patients that needs her help.
Is it time for a new subspecialty in our field? Perhaps the only way to manage the growing population of patients with OSD is to develop a more formal training and fellowship educational process that will attract providers who have a true interest and desire to care for these challenging patients. There is a niche group of ophthalmologists who have embraced this aspect of patient care, have formalized testing and procedures, and have learned to deliver world-class care. They have focused the majority of their time and clinical operations on OSD and in doing so have experienced tremendous satisfaction and financial success.
Much like the evolving space and subspecialty of refractive cataract surgery, OSD will hopefully move in a similar direction through fellowships, mentorships, formalization, and benchmarking. A 1-year cornea fellowship is no longer an adequate amount of time to acquire all of the knowledge and skills necessary for these rapidly expanding niches. Next year at the annual AAO meeting, I hope to interview not only residents for my refractive fellowship, but also candidates for a full-time fellowship-trained OSD expert.
Robert J. Weinstock, MD | Chief Medical Editor
1. Craig JP, Nicholas KK, Akpek EK, et al. TFOS DEWS II definition and classification report. Ocul Surf. 2017;15(3):276-283.