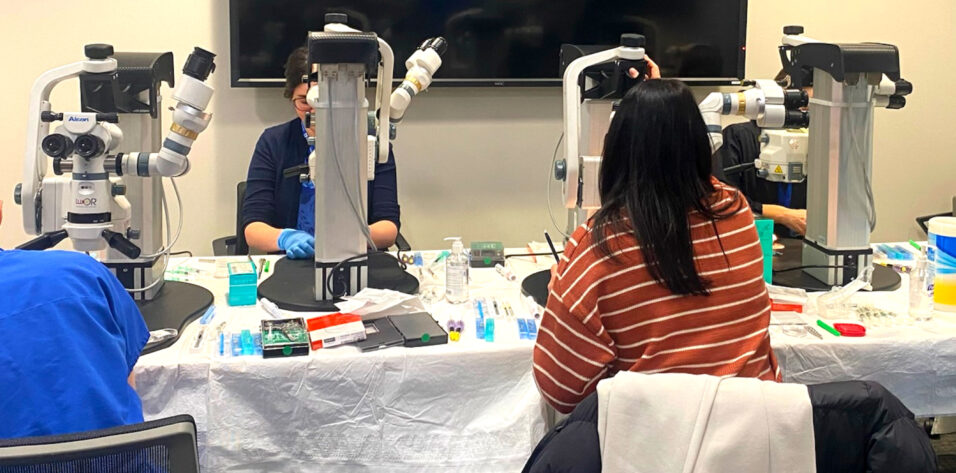
This February marked the annual Duke Cornea Fellows Course, spearheaded by Course Director Kourtney Houser, MD. For the 2nd year, current and incoming cornea fellows from across the country gathered in Durham, North Carolina, for an interactive forum that facilitated hands-on experience with advanced techniques in cornea and anterior segment surgery.
Didactic Segment
The main event kicked off with the convergence of more than 40 fellows in the exhibit hall at the Trent Semans Center for Health Education at Duke. The morning session was dedicated to a lecture series that covered key surgical concepts and techniques that would later be explored in the wet lab. The first section encompassed complex anterior segment surgery, with featured topics such as manual small-incision cataract surgery, secondary IOL implantation, iris repair, complex cataract surgery, and pars plana vitrectomy.
After a break to browse the exhibit hall and speak with industry representatives, attendees returned for the second didactic segment, which focused on corneal transplantation. Surgical videos illustrated step-by-step techniques as well as common pitfalls that may be encountered during endothelial keratoplasty, deep anterior lamellar keratoplasty, Boston keratoprosthesis placement, and limbal stem cell transplantation. The speakers, many of whom had graduated from fellowship within the past 5 years, provided insight into tackling some of the challenges that may present early in a cornea specialist’s career.
Wet Lab
The highly anticipated wet lab segment of the course consisted of a series of eight rotations, with an impressive array of 30 microscope workstations. Each station was proctored by a combination of attending surgeons, industry representatives, and local eye bank members. Attendees received plastic simulator eyes that traversed the stations with them and served as ideal models for practicing the Yamane technique and iris suturing without any mess. Miracles in Sight and CorneaGen generously provided donor corneal tissue to help attendees learn transplantation techniques in the most realistic manner possible. The opportunity to practice less commonly performed procedures such as pupilloplasty, manual small-incision cataract surgery, and IOL fixation in a relaxed environment made me feel much more likely to succeed in the OR going forward. Fortunately for me, I had more than one chance to attempt “the brave slash” at the deep anterior lamellar keratoplasty station put together by Eversight Vision.
The Opportunity to Build Community
This meeting provided a rare opportunity to unite as a cohort of fellows and to exchange ideas. Given the diversity of residency and fellowship training, it was interesting to reflect on where our individual experiences aligned or diverged. On a larger scale, moderated panel discussions revealed a range in management styles for various clinical questions, such as how long a postoperative endothelial keratoplasty patient ought to lie flat.
The course’s educational activities continued into the following day with the Controversies in Cornea and Cataract Surgery Conference, which was open to both trainees and attendings. Dr. Sonia Yoo’s excellent keynote lecture focused on the use of artificial intelligence in patients with corneal pathology. The other presenters covered a gamut of cataract, cornea, anterior segment, and ocular inflammatory disease topics. I look forward to attending this course next year as a full-fledged cornea fellow, and I hope to see many of my colleagues there!