
Building and owning an ambulatory surgery center (ASC) is arguably the single most important financial investment I have made in my career. Having my own ASC has given me direct control of how things are run, boosted my efficiency, and helped me achieve a better work-life balance.
PERSONAL JOURNEY
My father founded The Eye Institute of West Florida in 1974 in Largo, Florida. Over the course of about 50 years, the practice has expanded to include four additional locations. In 2003, we built a 30,000–square foot practice with an 8,000–square foot ASC on the second floor and a clinic on the first floor in Largo, Florida. The project was a game changer. Having a one-stop shop for our patients grew our practice in a way we could never have imagined.
We decided to replicate the model at a second location, St. Petersburg. We bought the office about 20 years ago, and the top floor sat empty while we built our first ASC. The practice is located only 12 miles away from our Clearwater location, but most patients don’t want to travel out of St. Petersburg for their surgery. Patient convenience becomes a huge factor in decision-making for ASCs, and we are looking to open a third in our Tampa location in the future.
CONSIDERATIONS
If you are thinking about building a new ASC or purchasing an existing one, consider six main points.
No. 1: Patient care. There is no question about the safety of an ASC and the outcomes that can be delivered to patients in the setting.
No. 2: Proximity. The ASC should be located close to your practice. Having it attached or directly next to your practice is ideal because patients are already comfortable with the setting. A location within or near your practice can also alleviate staffing burdens.
No. 3: Surgical volume. There is a push toward facilities for office-based surgery (OBS). I agree the setting has benefits, but oftentimes OBS suites are one or two rooms within a practice. This might not help ophthalmologists handle increases in surgical volume. Alternatively, an ASC can be built to scale. Find out how long it will take to recoup your costs and what types of providers will be in the ASC.
No. 4: Size and cost. The size of an ASC can be anywhere from 4,500 square feet (one or two surgery rooms) to 10,000 square feet (four or five surgery rooms). The sweet spot for a cataract surgeon who performs about 750 cataract surgeries or 250 laser procedures is probably two or three surgery rooms. Before breaking ground, visit other ASCs and bring a tape measure. I was surprised to see just how spacious a 6,500–square foot facility is. We probably could have gotten away with something smaller, and the size arguably reduces efficiency slightly. Each class B surgery room (ie, the indicated class for surgical procedures) is between 250 and 300 square feet.
The build-out cost has increased tremendously over the years. In Florida, it is currently about $350 to $500 per square foot. Surgical equipment costs about $750,000 to $1 million for two ORs. I recommend keeping the ORs simple. In our first ASC, we added built-in cabinets, which cost a lot of money. It is more cost-effective to buy simple cabinets and other storage units that can be wheeled between areas in the ASC.
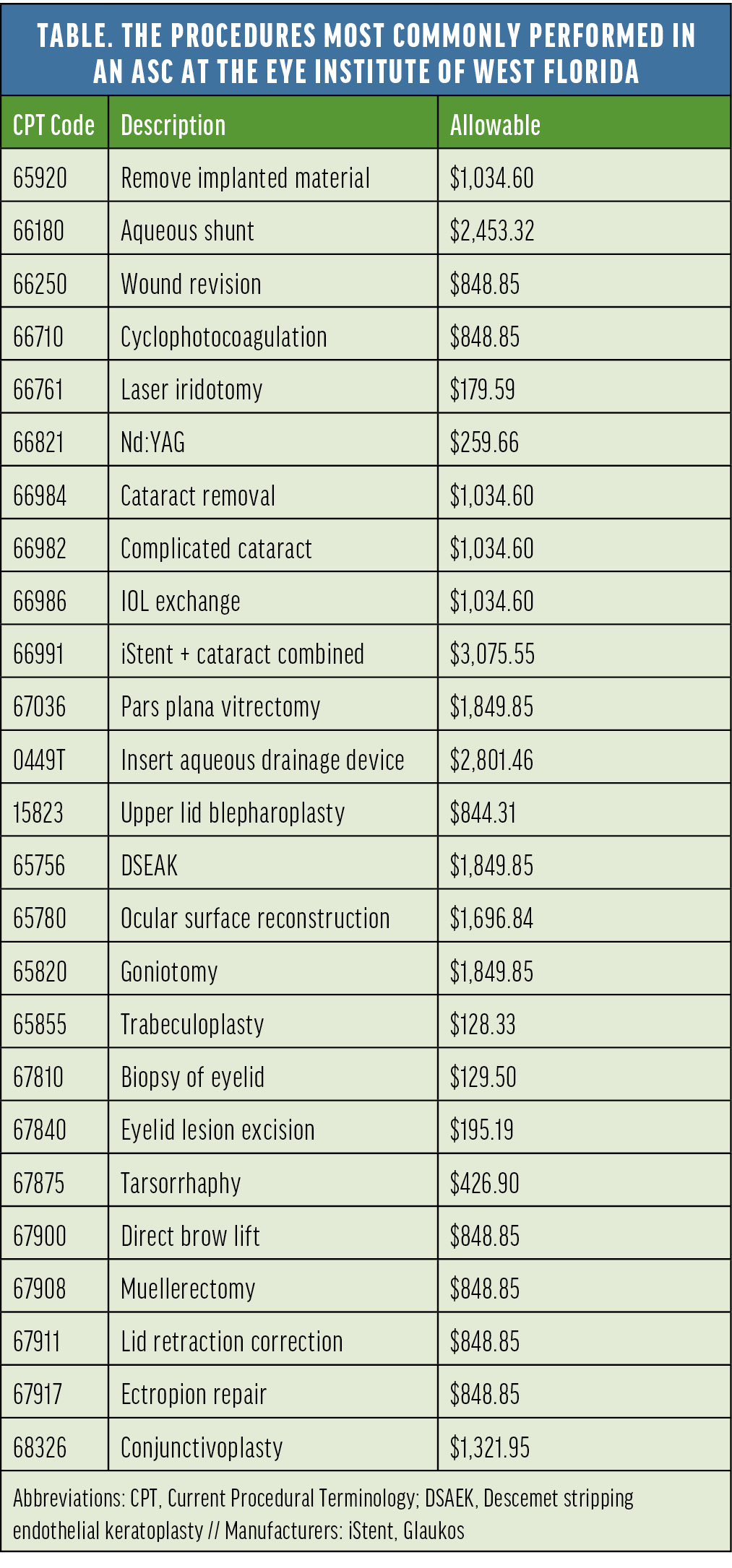
No. 5: Services offered. The Table lists the anterior segment procedures most commonly performed in our ASCs. These procedures are generally supported well by reimbursement if they are billed and coded properly and cost-effective equipment is used. Depending on the services you offer, an ASC can help you get in and out of surgery quickly yet efficiently so you can get back to the clinic. This is especially important for retina surgeons and those who perform laser procedures such as refractive surgery and certain glaucoma procedures.
No. 6: Layout. Our newest ASC in St. Petersburg is built on the second story above our freestanding clinic, which we have been growing for 20 years. It has three operating rooms, one of which has a femtosecond laser, and is designed to handle two surgeons working simultaneously as we grow. We put a lot of time into developing the layout to maximize workflow efficiency (Figure). The large pre- and postoperative area has four bays on each side. This is critical for efficiency and throughput and can allow a busy refractive surgeon to do eight cases per hour.
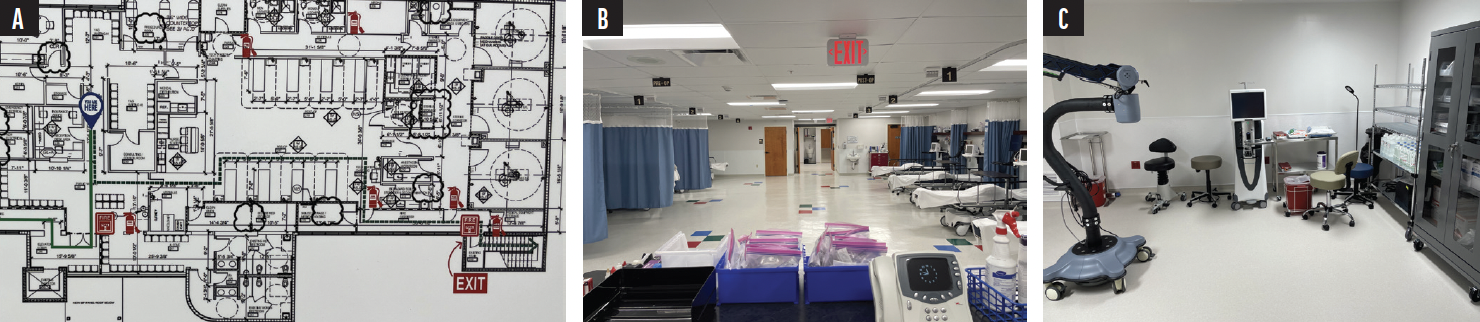
Figure. The blueprint for one of Dr. Weinstock’s ASCs (A). The pre- and postoperative areas (B) and the OR (C).
LOGISTICS
According to the CMS, an ASC and another entity such as an adjacent physician’s office cannot mix functions or operations in any common spaces during concurrent or overlapping hours of operation. For example, the same waiting room may not be used for patients in the ASC and clinic, and the same lasers may not be used for clinic and surgery center patients.
The CMS regulations permit two different Medicare-participating ASCs to use the same physical space as long as they are temporally separated and are not using the ASC at the same time. Theoretically, then, it is possible to rent your ASC in partnership with another clinic as long as both practices do not use the facility at the same time.
Conclusion
Owning an ASC can be a viable financial investment. It can be an important and practical move for ophthalmologists navigating a landscape of increasing surgical demand. In the future, I believe that OBS suites and ASCs will coexist in different formats, but for my practice, we have chosen to focus on building ASCs. They are a safe environment where we can treat patients in a guaranteed, well-proven, stable, and compliant way.




