
Today’s 20- and 30-somethings, our potential refractive surgery patients, are constantly on the go. They learn about new technologies on social media and make decisions spontaneously, often based on friends’ experiences. Consequently, their experience is as important as their postoperative results.
I say this somewhat facetiously, but, in reality, visual outcomes with any of the refractive surgical procedures available in 2020 are outstanding. And millennials know that. Once they get past the fear of having surgery on their eyes, which, from an existential perspective includes fear of the experience, what distinguishes one procedure from the next is the experience itself. Let’s examine how the VisuMax femtosecond laser (Carl Zeiss Meditec, Figure 1) contributes to, in my opinion, the best refractive surgery experience currently available. This platform can be used to create the LASIK flap and to perform SMILE. During the SMILE procedure, the VisuMax is used to create a lenticule within the corneal stroma that is then removed through a small keyhole incision cut to the corneal surface (Figure 2).
Figure 1. The VisuMax 500-kHz femtosecond laser can be used for LASIK flaps and for SMILE.
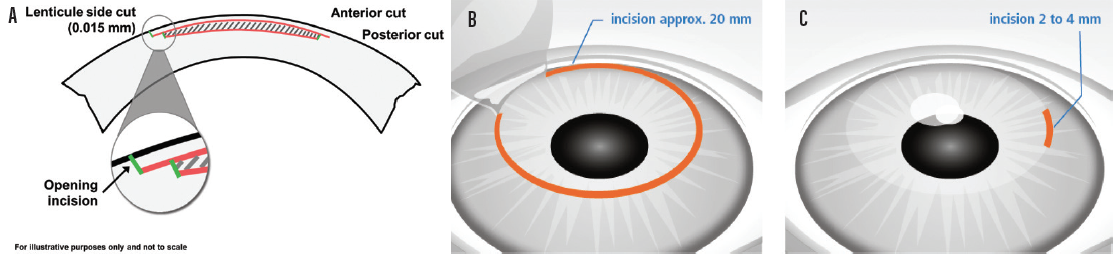
Figure 2. The lenticule, cut beneath the corneal surface, is accessed via a small surface keyhole incision (A). The LASIK flap extends for 300° and measures 20 mm (B), while the SMILE incision extends for only 60° and measures 4 mm (C).
Courtesy of Carl Zeiss Meditec
LASIK FLAP CREATION EXPERIENCE
A white eye. As we begin 2020, LASIK remains the most common and most popular refractive surgery procedure in the United States with the flap typically created using a femtosecond laser.1 Of the available femtosecond lasers, only one—the VisuMax—touches the cornea alone. Because its patient interface creates suction on the cornea without engaging the conjunctiva, there is no subconjunctival hemorrhage and the eye is white following the procedure.
How does this translate into a better patient experience? Immediately after surgery, family members are likely to remark, “The eyes don’t look like anything was done.”
Less pressure. The increase in pressure on the eye is relatively low with the VisuMax compared with other femtosecond laser suction mechanisms. Therefore, patients maintain vision throughout the procedure—a feature I find is much appreciated relative to the anxiety-producing blackout phase with high applanation pressure. Prior to acquiring the VisuMax in 2014, I had used another femtosecond laser for LASIK flap creation. When I released suction following flap creation, I was used to telling patients, “The worst is over.” Out of habit, I would say the same to patients after releasing suction with the VisuMax. The response from the patient was universally, “Really? Wow, that was nothing.”
Likewise, during my preoperative instructions, I changed from saying, “You will feel a fair amount of pressure on the eye and the vision will go dark,” to, “The green flashing light will get very clear at one point. I want you to look right at it. You will feel a light touch, like putting a contact lens in the eye.”
How does this translate into a better patient experience? Swapping the phrase “vision will go dark” for “light touch, like putting a contact lens in the eye” has had a noticeable effect on decreasing patients’ anxiety leading up to the procedure.
More comfortable. Because the VisuMax patient interface is relatively small (Figure 3), does not touch the conjunctiva, and does not require a separate suction ring, the surgeon needs to open the lid speculum less wide compared to other femtosecond lasers.

Figure 3. The patient interface contacts only the cornea, eliminating the possibility of subconjunctival hemorrhage.
Courtesy of Carl Zeiss Meditec
How does this translate into a better patient experience? Especially for patients with narrow palpebral fissures and those with deep-set eyes, minimizing lid speculum aperture significantly improves comfort and decreases anxiety.
SMILE EXPERIENCE
Growing volume, excellent results. I recently spent 3 weeks touring China with the AIER Eye Hospital Group, the largest eye care provider in the world. I gave patient education lectures in 10 cities, and I observed a volume of refractive surgery rarely, if ever, seen in the United States. The surgeons are humble yet incredibly experienced, and they are immersed in a population that is more than 80% myopic.
SMILE is becoming increasingly popular not just within the AIER Eye Hospital system but also within China as a whole. In 2018, SMILE represented 25% of all refractive procedures done within the AIER system, including all versions of LASIK, PRK, and phakic IOL implantation (personal communication with AIER).2 At one hospital in particular, Chengdu AIER Eye Hospital, SMILE accounted for 63% of all refractive procedures performed in 2018. The SMILE patient experience is likely contributing to the remarkable growth of the procedure in China.
As of December 2019, more than 2.5 million SMILE procedures have been performed worldwide. Visual outcomes and vision recovery are equivalent to LASIK, with 90% of patients achieving 20/20 or better UCVA on the first postoperative day (Figure 4).2
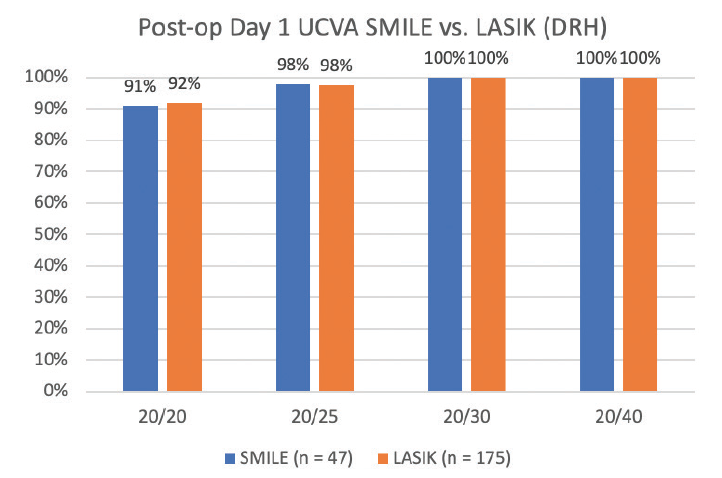
Figure 4. UCVA on postoperative day 1 for SMILE versus femtosecond LASIK.2
In one study, 100% of patients achieved 20/20 or better UCVA at 2 years after SMILE, compared to 93% for wavefront-guided LASIK. Further, 90% in the SMILE group achieved 20/15 or better, compared to 87% in the wavefront-guided LASIK group.3 With equivalent vision outcomes, what does SMILE bring to the table to challenge the magnificently successful LASIK? You guessed it: the patient experience. All the VisuMax patient experience features I just described for LASIK hold for SMILE as well. Additionally, SMILE is far and away the easiest procedure to go through from the patient’s perspective (see Watch It Now). I have found this to be true for four reasons.
A patient testimonial on undergoing SMILE at Dr. Hamilton’s practice.
Speed. In my hands, the average bilateral SMILE takes less than 8 minutes. For the surgeons I visited in China, who have typically performed at least 10,000 SMILE procedures, bilateral SMILE takes less than 5 minutes to complete.
How does this translate into a better patient experience? Patients are reassured in their decision when they realize that the procedure uses a single laser and will last less than 8 minutes for both eyes.
No sound, no smell. As experienced refractive surgeons, we barely notice the odor of the vaporized tissue and the sound of the excimer laser. Patients not only notice the sound and the smell, but often they come into the consult anxious about these issues. “My friend told me I’ll smell my flesh burning.” I respond by saying, “Oh no, we use a cool laser, there’s no burning involved. It smells a little like singed hair.” But with SMILE, these worries do not exist—no sound, no smell.
How does this translate into a better patient experience? SMILE is a kinder, gentler refractive surgical experience. Millennials, especially, appreciate learning that.
No flap. How many times have you repositioned a dislodged flap? After 16 years, I can count the number of times I’ve had to on one hand, maybe two. Even though it is rare, it is a source of anxiety for the patient. “Doc, does the flap heal?” “What if I get poked in the eye?” “I play competitive basketball.” “I’m into mixed martial arts.” “What about removing make-up?” “I’ve got an infant at home who loves to poke me in the eye.” Before SMILE, I would try to defuse such issues by telling patients, “In more than 10,000 surgeries, I’ve had to reposition a flap less than 10 times, and these patients have done well. You don’t need to lose sleep over it.” Now, with SMILE, I simply say, “There is no flap.” I can feel the patient’s instant relief.
How does this translate into a better patient experience? In reality, the flap is not an issue; perception is that it is, and perception is reality. Simply put, patients are relieved to know there is no flap in SMILE.
Fewer dry eye symptoms. Despite the incredible success of LASIK and the findings of the PROWL study,4 the perception remains that dry eye symptoms can worsen following LASIK and that, on rare occasions, these symptoms can last for years. It frustrates us as refractive surgeons because we know the literature does not support the notion that dry eye following LASIK is a major issue. In fact, in most situations, patients are more comfortable and experience less dry eye symptoms after LASIK than they did with contact lenses before the procedure.5 Unfortunately, this is yet another instance in which perception is reality. The concern over dry eye symptom exacerbation remains a barrier to entry for many potential refractive surgery candidates.
Enter SMILE. The scientific literature has shown that the negative impact on corneal sensation and dry eye symptoms is less and of a shorter duration with SMILE compared to LASIK (Figure 5). A meta-analysis of 11 studies and more than 1,100 eyes demonstrated better corneal sensitivity and longer tear breakup time at 1 and 6 months in patients who had SMILE versus those who had femtoesecond LASIK.6
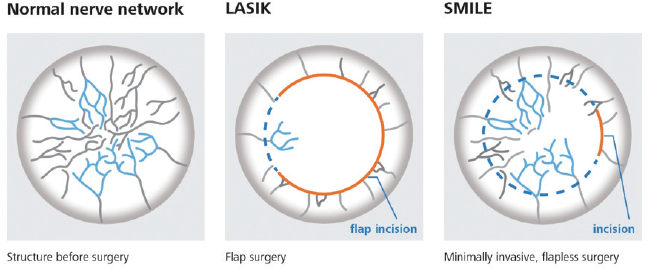
Figure 5. In LASIK flap creation, the subbasal corneal nerve plexus is severed for 270º (center). In SMILE, a 60º surface incision preserves significantly more corneal nerves, reducing the magnitude and duration of dry eye symptoms following surgery (right).
Courtesy of Carl Zeiss Meditec
How does this translate into a better patient experience? Millennials spend increasingly more time on cell phone, tablet, television, and video game screens. Dry eye is a major concern for them. Patients are reassured that, with SMILE, they are choosing the procedure that will have the shortest and smallest effect on their ocular surface and overall comfort.
CONCLUSION
We have at our disposal remarkable refractive surgery tools that can help to increase the confidence that we have in reliably delivering excellent outcomes and satisfying the majority of our patients. Fear remains the leading barrier to potential patients seeking out our services, however, and millennials desire a seamless, painless, quick procedure with minimal side effects. Whether it’s for LASIK flaps or SMILE, the VisuMax laser was designed to provide the most comfortable refractive surgery experience available. Enjoy its advantages!
1. Duffey RJ, Leaming D. 2015 U.S. ISRS Surgery Survey. www.duffeylaser.com Accessed December 6, 2019.
2. Chong JK, Nejad M, Nutkiewicz M, Hamilton DR. Comparing uncorrected visual acuity on postoperative day 1 following low versus high energy SMILE. Paper presented at: the 2019 European Society of Cataract and Refractive Surgery Annual Meeting; September 14-18, 2019; Paris.
3. Kobashi H, Kamiya K, Igarashi A, Takahashi M, Shimizu K. Two-year results of small incision lenticule extraction and wavefront-guided laser in situ keratomileusis for myopia. Acta Ophthalmol. 2018;96(2):e119-e126.
4. Eydelman M, Hilmantel G, Tarver ME, et al. Symptoms and satisfaction of patients in the patient-reported outcomes with laser in situ keratomileusis (PROWL) studies. JAMA Ophthalmol. 2017;135(1):13-22.
5. Sainz R, Hauser W. Treating dry eye disease with refractive surgery. Collaborative Eye. collaborativeeye.com/articles/sept-oct-18/treating-ded-with-refractive-surgery/. Accessed December 6, 2019.
6. Zhang Y, Shen Q, Jia Y, Zhou D, Zhou J. Clinical outcomes of SMILE and FS-LASIK used to treat myopia: a meta-analysis. J Refract Surg. 2016:32:256-265.




