A promising scleral solution to presbyopia demonstrates positive early results.

By Frank A. Bucci Jr, MD
As an investigator in the clinical trial of the VisAbility Micro-Insert System (ReFocus Group), I have had the opportunity to treat more than 35 patients with this innovative new approach to correcting presbyopia. If early results are replicated in the larger clinical trial, I think the technology will be a promising addition to surgeons’ armamentarium.
EARLY RESULTS
During the procedure, four microinserts are implanted in the sclera, outside the visual axis (Figures 1 and 2). Observation of 360 patients enrolled at 13 clinical trial sites in the United States is ongoing, with results expected this year. Prior to the final data set, my fellow investigators and I were able to look at the results from an early sample of 10 consecutive cases from two surgeons (Y. Ralph Chu, MD, and me). The FDA permitted analysis specifically of the sixth through fifteenth cases for a total of 40 eyes of 20 patients.
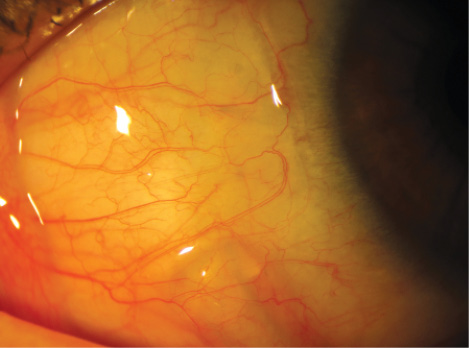
Figure 1. Side view of the VisAbility microinsert in vivo.
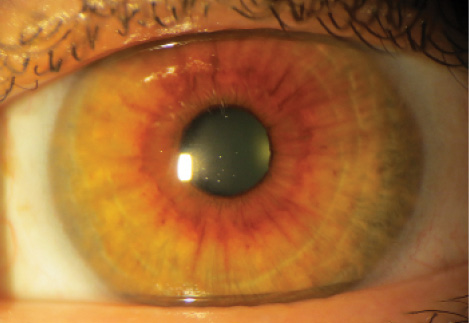
Figure 2. On primary gaze, the scleral microinserts are nearly invisible.
To be considered for this clinical trial, patients had to be 45 to 60 years old and have a nearly emmetropic manifest refractive spherical equivalent (MRSE; +0.50 to -0.75 D), with no ocular pathology or history of ocular surgery.
The average age of the 20 patients was 52.1 years (range, 46-58). Sixty percent were male. The mean MRSE was +0.184 D (range, +0.50 to -0.50 D) at baseline, with a near visual acuity of 20/62.4 monocularly and 20/50.1 binocularly.
Distance vision was unaffected by the microinsert procedure. Twelve months postoperatively, there was essentially no change (0.00 ±0.25 D) in MRSE from baseline (Figure 3).
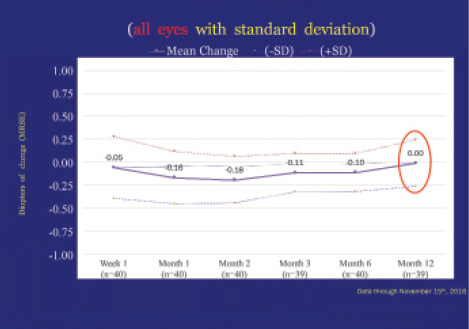
Figure 3. Mean MRSE was unchanged from baseline to 12 months in eyes undergoing the procedure.
Patients’ near vision was tested at the FDA-mandated distance of 40 cm, which is a comfortable reading distance for most people. At 12 months, all patients had a bilateral near UCVA of J3 (20/40) or better; 95% saw J2 (20/32) or better; and 90% saw J1 (20/25) or better (Figure 4). Impressively, even when we assessed monocular distance-corrected near visual acuity in primary eyes only, 100% were J3 or better, and 95% were J2 or better.
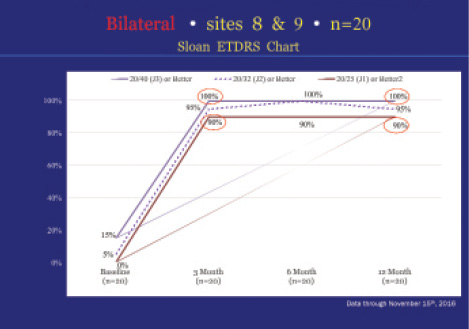
Figure 4. Near UCVA results were excellent, with all patients seeing J3 or better at 12 months in an early, two-site analysis.
We are finding that patients’ near vision continues to improve over time. For example, the minimum add required to achieve optimal distance-corrected near visual acuity in the two-site analysis was 1.65 D at baseline. Six months after the procedure, it was 0.63 D, and by 12 months, it was 0.46 D. When I saw my last three patients for their 1-year follow-up examinations, they could all see J1 uncorrected.
My patients report a high level of satisfaction with the microinsert procedure. They seem to experience a visual rejuvenation with a continuous range of vision and no drop-off in between focal points.
A NEW TYPE OF SURGERY
Although the mechanism of action is not fully understood, the current thinking is that the microinserts increase tension on the zonules, changing the position of the lens with accommodative effort. Going into the study, therefore, my expectation was that the procedure might work better in younger patients who had more accommodative ability, but I have not personally found that to be the case. My 60-year-old patients seem to do just as well as the 45-year-olds. I do encourage patients not to use their reading glasses at all postoperatively, because my sense is they will have better results from the procedure with accommodative effort over time.
The procedure is not technically difficult, but because it is quite different from other refractive surgeries, there is a learning curve. First, the surgeon recesses the conjunctiva at the corneal limbus. There will be conjunctival bleeding, but my fellow investigators and I purposely did not use cautery so as to maintain the architecture of the sclera.



Figure 5. The system includes a docking station (Top), scleratome (Middle), and four two-piece PMMA microinserts (Bottom).
The docking station (Figure 5A) “locks” with four-point fixation. A spring-loaded scleratome (Figure 5B) then docks into position and is used to create four 4 × 1.1-mm lamellar scleral tunnels at the oblique quadrants of the eye. The tunnels are precisely positioned 4 mm from the limbus and 400 µm deep. A two-piece PMMA microinsert (Figure 5C) is then guided into each tunnel. Finally, the two pieces are locked together; a tiny flange on the end keeps the microinsert from migrating once it is positioned in the sclera (see video below). After all the microinserts are in place, the surgeon reapproximates and secures the conjunctiva. Tisseel surgical glue (Baxter Healthcare) may be used to maintain hemostasis.
View an animation of the procedure.
As with other refractive procedures, postoperative medications include 1 to 2 weeks of a topical antibiotic and steroid. Treatment with the steroid may be extended if needed for the patient’s comfort and control of hyperemia. My fellow investigators and I also aggressively treat dry eye disease with artificial tears, oral omega-3 supplements, and punctal occlusion.
ADDING TO THE ARMAMENTARIUM
Refractive surgeons have been looking for the perfect solution to presbyopia for a long time. Compared with other approaches, the VisAbility Micro-Insert System has a number of advantages. As an extraocular procedure performed outside the visual axis, it avoids the most serious risk associated with lenticular surgery (endophthalmitis) as well as the sight-threatening complications that have been associated with some iterations of corneal inlays, including corneal melts and central haze.1,2 In the case of microinserts, postoperative steroids are used primarily for the patient’s comfort and are not needed to modulate the healing response.
The microinsert procedure is bilateral, so it has no negative impact on depth perception, light transmission, or binocularity. In addition, patients have the advantage of excellent near and distance acuity in each eye. Moreover, the procedure preserves the cornea and lens for future surgery, if needed. To date, the microinserts have not been associated with nighttime dysphotopsia; nor is there reason to think they would be, because they are not in the visual axis. Reversibility of the procedure is another advantage, although I have not yet removed any of the devices myself.
1. Whitman J, Dougherty PJ, Parkhurst GD, et al. Treatment of presbyopia in emmetropes using a shape-changing corneal inlay. Ophthalmology. 2016;123(3):466-475.
2. Wu EI-H. Review of corneal inlays for presbyopia. Adv Ophthalmol Optom. 2017;2(1):355-365.
It should soon become clear if scleral expansion surgery has a role in presbyopia correction.

By John F. Doane, MD
Interest in any modality for resolving presbyopia’s symptoms should be considered in relation to the many surgical approaches that have been tried, including monovision LASIK and PRK, presbyopic LASIK (multifocal laser ablation), paracentral corneal collagen shrinkage (laser thermal keratoplasty and conductive keratoplasty), femtosecond laser central steepening (Intracor; Technolas Perfect Vision; not FDA approved), corneal inlays (Kamra [AcuFocus], Raindrop Near Vision Inlay [ReVision Optics], Presbia Flexivue Microlens [Presbia; not FDA approved]), and pseudophakic IOLs (monovision, accommodating, extended-depth-of-focus, and multifocal IOLs). All of these have met with limited acceptance by patients and surgeons, and some techniques have been abandoned.
Researchers have studied scleral surgery to ameliorate presbyopia’s symptoms for several decades. Thornton and Fukasaku spearheaded early efforts,1,2 and others have evaluated the theory, surgery, and accommodative effects of the technique.3-7 Nevertheless, today, several questions have yet to be answered.
WHAT IS THE MECHANISM OF ACTION?
Schachar postulated that an anatomic mechanism can be taken advantage of by altering the relationship of the peripheral crystalline lens to the equatorial zonules.3 The Schachar theory states that the equatorial zonules tighten to cause accommodation. In contrast, the Helmholtz theory holds that, during accommodation, contracture of the ciliary muscle fibers shrinks the ciliary body, relaxing the zonules and rounding the lens.8 Proposed in 1855 and published in 1909, the latter has been the more widely accepted theory since the turn of the 20th century. The goal of scleral expansion is to facilitate a return of the natural mechanism of accommodation, whatever that may be.
DOES SCLERAL EXPANSION SURGERY WORK?
The answer to this question depends on patients’ subjective reports and objective measurements of accommodative amplitude and near vision reading with distance correction in place. To date, the reports have been mixed.1-7
If the results are good, is it clear if true crystalline lens accommodation is occurring, or are pseudoaccommodative effects at play? Three studies evaluating scleral expansion surgery without segment placement have found no improvement in accommodation, and the authors of one of these studies asked, if scleral expansion surgery does not work without the placement of expansion bands, why would it work with them?5-7
WILL THE RESULTS LAST?
Presbyopia is a progressive process, with most accommodative loss occurring by age 65. Without a controlled analysis at the 3-, 5-, and 10-year marks, it is impossible to determine unequivocally if scleral expansion surgery will have a lasting effect.
CAN THE TECHNIQUE BE COMMERCIALLY VIABLE IN THE LARGER REFRACTIVE SURGERY MARKET?
It is one thing to perform surgery in an FDA trial and quite another to stimulate interest in a large swath of refractive surgeons and patients. Stable long-term results would likely determine the commercial viability of scleral expansion with segment insertion.
Years ago, keratomileusis in situ lost out to IOLs as the solution for aphakia. Two descendants of keratomileusis in situ, LASIK and small-incision lenticule extraction or SMILE, however, arose from earlier concepts and have been successfully adopted worldwide. Could there be a place for scleral expansion surgery as the cure of presbyopia? Ophthalmologists should know in the next several years.
1. Thornton SP. Anterior ciliary sclerotomy (ACS), a procedure to reverse presbyopia. In: Sher NA, ed. Surgery for Hyperopia and Presbyopia. Williams & Wilkins: Baltimore; 1997:33-36.
2. Fukasaku H, Marron JA. Anterior ciliary sclerotomy with silicone expansion plug implantation: effect on presbyopia and intraocular pressure. Int Ophthalmol Clin. 2001;41(2):133-141.
3. Schachar RA. Cause and treatment of presbyopia with a method for increasing the amplitude of accommodation. Ann Ophthalmol. 1992;24(12):445-447, 452.
4. Glasser A, Kaufman PL. The mechanism of accommodation in primates. Ophthalmology. 1999;106(5):863-872.
5. Mathews S. Scleral expansion surgery does not restore accommodation in human presbyopia. Ophthalmology. 1999;106(5):873-877.
6. Ostrin LA, Kasthurirangan S, Glasser A. Evaluation of a satisfied bilateral scleral expansion band patient. J Cataract Refract Surg. 2004;30(7):1445-1453.
7. Hamilton DR, Davidorf JM, Maloney RK. Anterior ciliary sclerotomy for treatment of presbyopia: a prospective controlled study. Ophthalmology. 2002;109(11):1970-1976; discussion 1976-1977.
8. von Helmholtz HH. Mechanism of accommodation. In: Southall JPC, ed. Helmholtz’s Treatise on Physiological Optics. New York: Dover; 1962.




