
Three-Year Longitudinal Survey Comparing Visual Satisfaction With LASIK and Contact Lenses
Price MO, Price DA, Bucci F, et al1
Abstract
This study reframed the assessment of patients’ satisfaction with LASIK by prospectively comparing a cohort of LASIK patients with a control group that chose to continue wearing contact lenses. The study enrolled 1,800 participants at 20 private medical practices across the United States: 39% composed the contact lens control group, 45% wore contacts at baseline and underwent LASIK, and 16% wore glasses at baseline and had LASIK. Most of the contact lens wearers had used the modality successfully for at least 5 years. Participants completed self-administered web-based surveys at baseline and at 1, 2, and 3 years. The study was funded by the nonprofit Cornea Research Foundation of America and the participating physicians with no industry support or involvement.
AT A GLANCE
• A prospective, 3-year, multicenter study involving 1,800 participants compared LASIK results with those of a control group that continued to wear contact lenses. The investigators found that LASIK resulted in higher satisfaction, improved the ease of driving at night, and reduced visual symptoms. Dry eye symptoms did not increase after LASIK among former contact lens wearers but did among former glasses wearers, suggesting this group may need more intensive dry eye management. The rate of eye infection, corneal ulcers, and abrasions was significantly lower every year after LASIK versus after continued contact lens wear.
• A pair of prospective studies in military and civilian populations evaluated patients’ satisfaction and visual symptoms 1, 3, and 6 months after LASIK. Patients’ satisfaction with LASIK was high, and visual symptoms improved after the procedure compared to baseline. Some individuals with no visual symptoms preoperatively reported symptoms postoperatively, however, and a few were dissatisfied. The Ocular Surface Disease Index score improved at 3 and 6 months after LASIK relative to baseline.
• Self-administered, web-based surveys may become the new standard for evaluating satisfaction and visual symptoms after refractive surgery.
Compared to continued contact lens use, LASIK improved the ease of driving at night, reduced the risk of eye infections, and did not significantly increase dry eye symptoms. Satisfaction levels with LASIK consistently exceeded those with contact lenses.
Patients’ strong agreement with recommending a current method of vision correction to a close friend or family member was considered indicative of their satisfaction. In the contact lens control group, the proportion of participants who strongly agreed that they would recommend contacts declined from 63% at baseline to 54% at year 3 (Figure 1). This decrease occurred despite the substantial contact lens discontinuation rate (14% over 3 years) by those presumably the least satisfied, which dropped their responses out of subsequent satisfaction calculations. The proportions of patients who strongly agreed that they would recommend LASIK were consistently higher throughout the 3-year follow-up period, both among participants who had previously worn contacts (84%-88%) and those who had previously worn glasses (77%-80%; Figure 1). At every time point, between 1% and 2% did not recommend their current method of vision correction in both the LASIK and the contact lens control groups.
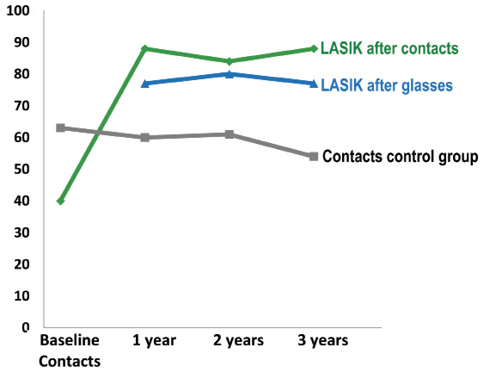
Figure 1. Proportion (percentage) that strongly recommends current method of vision correction.
LASIK significantly reduced difficulties with driving at night as well as nighttime visual disturbances, both for former contact lens wearers and former glasses users (Figure 2). The proportion that reported no difficulty with driving at night remained substantially lower every year in the contact lens control group.
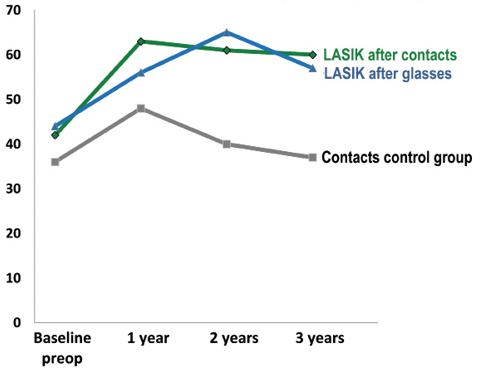
Figure 2. Proportion (percentage) with no difficulty driving at night.
The proportion of participants with no dry eye disease (DED) was consistently low in the contact lens control group (29%-34%), and no significant decline was seen after LASIK compared with baseline contact lens wear (Figure 3). Among former glasses wearers, however, the proportion without DED decreased from 51% at baseline to 28% 1 year after LASIK, with a subsequent improvement to 42% at 3 years (Figure 3). Those who wore glasses at baseline were older on average than the contact lens wearers. Also, 74% of former glasses wearers said that they had tried contact lenses, and DED was the most common reason given for quitting.
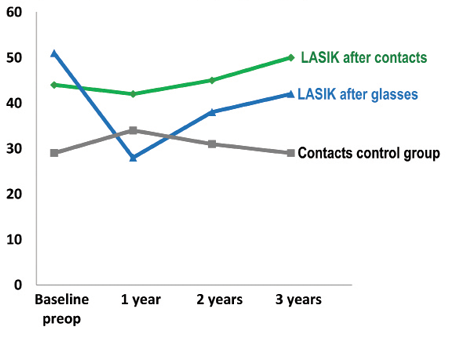
Figure 3. Proportion (percentage) with no DED.
The self-reported rates of eye infection, ulcer, and abrasion were more than twice as high each year in the group that continued to wear contact lenses compared with the group that underwent LASIK.
DISCUSSION
This research focused on what patients care about when evaluating vision correction options. Compared with those who chose to continue wearing contact lenses, the participants who elected to undergo LASIK reported substantially higher satisfaction with their vision, improved ease of night driving, and reduced levels of visual disturbance.
The investigators found that DED symptoms were common among contact lens wearers, with no increased prevalence 1 to 3 years after LASIK. The findings suggest that glasses wearers represent a group that needs more intense preoperative and postoperative management of DED.
Infectious keratitis is a well-recognized problem with contact lenses, particularly with overnight use. The substantial reduction in eye infection, ulcers, and abrasions after LASIK represents an important safety advantage.
Symptoms and Satisfaction of Patients in the Patient-Reported Outcomes With Laser in Situ Keratomileusis (PROWL) Studies
Eydelman M, Hilmantel G, Tarver ME, et al2
Abstract
Eydelman and colleagues reported results from the FDA-sponsored PROWL studies. PROWL-1 enrolled 262 active-duty Navy personnel monitored for 6 months after LASIK, and PROWL-2 enrolled 312 civilians observed for 3 months.
Participants completed self-administered web-based surveys. The baseline PROWL-1 and 2 surveys had 161 and 154 questions, respectively, whereas the postoperative surveys had 129 and 112 questions, respectively. A companion publication described the design and testing of the survey instruments, which included eight new visual symptom questions, the National Eye Institute Refractive Error Quality of Life instrument and Visual Function Questionnaire, and the Ocular Surface Disease Index.3 An interesting finding was that patients were more likely to report ocular symptoms with an online questionnaire than to a health care professional.
The investigators found that visual symptoms and dissatisfaction with vision were common preoperatively. Most participants were satisfied after LASIK. The mean satisfaction ratings at 3 months were 92.9 and 90.6 (on a 100-point scale) in PROWL-1 and 2, respectively, and 93.1 at 6 months in PROWL-1. Dissatisfaction rates were 1% and 2% at 3 months for PROWL-1 and 2 and 2% at 6 months in PROWL-1, with no retreatments performed during the study.
The overall prevalence of visual symptoms decreased after LASIK. Among participants who reported no visual symptoms at baseline, 43% to 46% reported a new symptom at follow-up, whereas a larger number of participants who reported symptoms at baseline either experienced improvement or reported no symptoms after LASIK.
The Ocular Surface Disease Index scores improved postoperatively at the 3- and 6-month exams compared with the baseline preoperative level. A little over 25% of those with normal scores developed abnormality, but this was more than offset by those whose abnormal scores improved.
DISCUSSION
As in the first study addressed in this article,1 the PROWL studies did not specify patients’ care or the types of devices that could be used for LASIK; they only required that enrollment and treatment be consistent with device labeling. Thus, the results were not limited to a specific LASIK platform but were instead more broadly representative of the standard of care at the time of enrollment.
The PROWL studies showed that LASIK produced excellent outcomes and high levels of satisfaction among patients. The number of dissatisfied patients was small. Interestingly, a weak correlation was detected between the preoperative depression/anxiety score and the level of satisfaction 6 months after LASIK.
The PROWL findings were consistent with a review of the clinical outcomes of LASIK published between 2008 and 2015. Sandoval and colleagues reviewed 97 relevant articles (representing 67,893 treated eyes) and concluded, “Modern results support the safety, efficacy, and patient satisfaction of the procedure.”4
1. Price MO, Price DA, Bucci FA, et al. Three-year longitudinal survey comparing visual satisfaction with LASIK and contact lenses. Ophthalmology. 2016;123:1659-1666.
2. Eydelman M, Hilmantel G, Tarver ME, et al. Symptoms and satisfaction of patients in the patient-reported outcomes with laser in situ keratomileusis (PROWL) studies. JAMA Ophthalmol. 2017;135(1):13-22.
3. Hays RD, Tarver ME, Spritzer KL, et al. Assessment of the psychometric properties of a questionnaire assessing patient-reported outcomes with laser in situ keratomileusis (PROWL). JAMA Ophthalmol. 2017;135(1):3-12.
4. Sandoval HP, Donnenfeld ED, Kohnen T, et al. Modern laser in situ keratomileusis outcomes. J Cataract Refract Surg. 2016;42:1224-1234.




