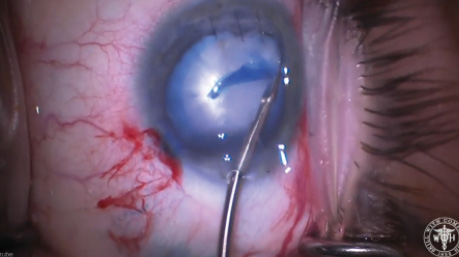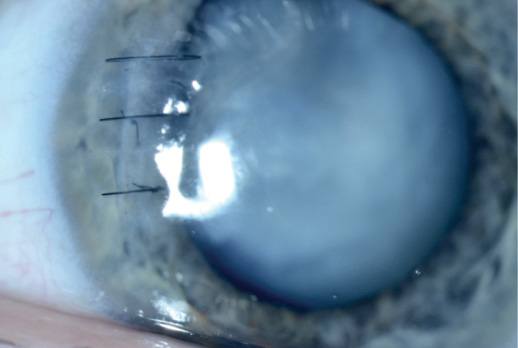
Figure 1. Corneal sutures and a white cataract.
—Case prepared by Brandon D. Ayres, MD.
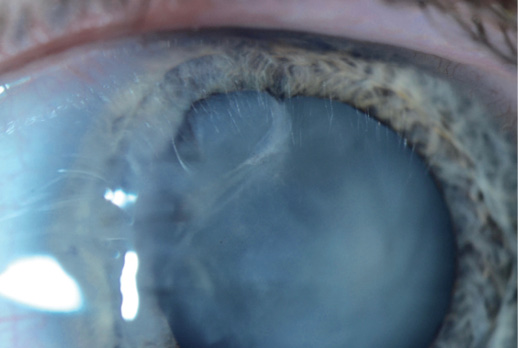
Figure 2. Slight irregularity in the iris contour and a violated anterior capsule.
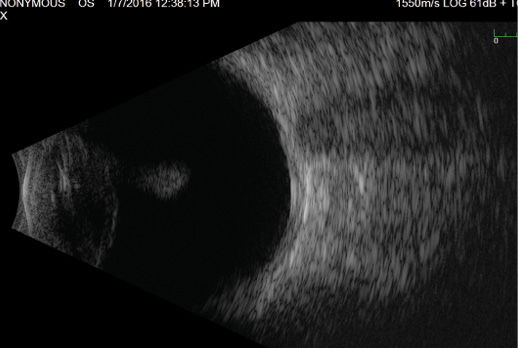
Figure 3. B-scan ultrasonography of the patient’s left eye shows a normal posterior pole but confirms violation of the posterior capsule of the lens, with debris posterior to the lens.


ASHA BALAKRISHNAN, MD, AND D. MICHAEL COLVARD, MD
In the absence of profound zonular instability, we would proceed with cataract extraction using an anterior approach. Placing iris hooks along the superonasal iris and staining the capsule with trypan blue (VisionBlue; Dutch Ophthalmic USA) would maximize visualization of the extent of the anterior capsular tear. A cohesive ophthalmic viscosurgical device (OVD) or soft-shell approach and decompression of the lens by needle aspiration would reduce the risk of capsulorhexis run-outs or extension of the preexisting tear. If the anterior capsular tear does not extend posteriorly, we would incorporate it within the capsulorhexis flap and use capsular hooks for focal zonular weakness. Given the posterior capsular defect, we would favor hydrodelineation without hydrodissection. We would attempt to identify the posterior rent as early as possible and place a dispersive OVD through the tear to discourage vitreous prolapse during lens removal.
Because of the patient’s age, the cataract may be soft and amenable to aspiration. If not, we would perform phacoemulsification, viscodissection, epinuclear removal, and bimanual I/A. A lower bottle height and vacuum level would minimize chamber fluctuation. After completing the anterior vitrectomy, we would consider creating a posterior capsulotomy in the area of the defect, depending on its size, for optimal stability of the IOL-capsular bag complex. Owing to the patient’s history of trauma, we would insert a posterior chamber IOL (PCIOL) with a capsular tension ring and place capsular tension segments as needed. A three-piece IOL could be implanted in the sulcus if the posterior capsule is unstable. In the event that the anterior and posterior capsules are not suitable to support an IOL, we would place an iris- or sclera-fixated secondary IOL at a later time.

NICOLE R. FRAM, MD
Fortunately, an intraocular foreign body was ruled out in this case, and the corneal laceration appears to be outside the visual axis. Eyes such as this one require a systematic approach that will allow the ophthalmologist to turn an unpredictable presentation into a planned surgical outcome.
The first step is proper biometry and IOL calculations. If the corneal topography is regular centrally, the ophthalmologist can proceed with cataract surgery and feel relatively comfortable about the reliability of IOL calculations. If the cornea is highly irregular, however, the patient must be informed that he or she will need to wear a contact lens postoperatively to obtain BCVA. In this case, the corneal laceration appears to be peripheral, and it is unlikely the patient will need a penetrating keratoplasty in combination with cataract surgery. An immersion A-scan can thus be obtained to accurately measure axial length, because optical biometry cannot penetrate a white cataract. The axial length can be entered into a biometry device so that IOL power can be determined. Although it would be ideal for all corneal sutures to be removed prior to measurements, cataract surgery may need to take place imminently because of increasing inflammation. A combined procedure with a retina colleague should be planned, because the B-scan reveals violation of the posterior capsule and lenticular debris in the posterior pole.
The surgeon can begin by intracamerally instilling preservative-free triamcinolone and balanced salt solution diluted 1:4 to help visualize potential vitreous prolapse into the anterior chamber. After the vitreous is cleared, the anterior capsule should be stained with trypan blue to visualize the extent and location of the anterior capsular violation. Of note, the surgeon could contemplate performing a laser capsulotomy if the posterior capsule is intact, the central cornea is clear, and the anterior capsular violation is central to the planned capsulotomy. If a continuous curvilinear capsulorhexis (CCC) cannot be completed and removal of the cataract from an anterior approach is not possible, then a pars plana lensectomy could be performed, followed by scleral fixation of a secondary PCIOL. Fixation could be accomplished with a suture (Gore-Tex CV-8 thread on a ttc-9 needle [W.L. Gore & Associates; off-label use] or 9–O polypropylene on a CIF-4 needle [Ethicon]) or intrasclerally. The choice of secondary PCIOL depends on the surgeon’s skill set and familiarity with the procedure. If the corneal endothelium is healthy and there are no anticipated procedures requiring gas/air, then suturing an Akreos AO60 PCIOL (Bausch + Lomb) with four-point scleral fixation is reasonable. Alternatively, intrascleral fixation can be performed using a SofPort LI61AO (Bausch + Lomb) or EC-3 PCIOL (Aaren Scientific, Zeiss). I would avoid iris suture fixation, because the previous injury traumatized the iris.
After fixation of the secondary IOL, iris repair can be performed using 10–O polypropylene on a CIF-4 needle (Ethicon) or PC-7 needle (Alcon). The surgeon should evaluate the extent of iris damage prior to suturing by using intracameral agents such as acetylcholine (Miochol-E; Bausch + Lomb) and carbachol (Miostat; Alcon). Intracameral agents will help the ophthalmologist to assess the status of the remaining pupillary sphincter tone and tissue available for repair. To avoid iatrogenic damage during pupilloplasty, a careful evaluation for traumatic iridodialysis will be necessary prior to initiating a pupillary cerclage or closure (Figures 4 and 5). The ideal postoperative pupillary opening to maintain so as to allow for a proper retinal evaluation is 3.5 to 4 mm.
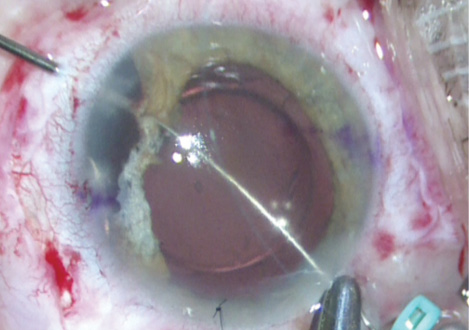
Figure 4. Iridodialysis repair using a double-armed 10–O polypropylene suture (STC-6 needle [Ethicon]) docked into a 25-gauge needle 1.5 mm posterior to the limbus after the performance of a conjunctival peritomy.
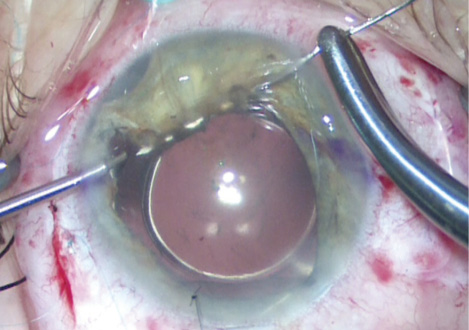
Figure 5. Pupillary cerclage using a 10–O polypropylene suture (CIF-4 needle) docked into a 27-gauge cannula.
Scleral suture fixation can result in early hypotony and vitreous hemorrhage in the immediate postoperative period. It is therefore important to monitor patients carefully and collaborate with retina colleagues.

SUMIT “SAM” GARG, MD
Based on the history and Figures 1 and 2, this patient has a traumatic cataract with pupillary damage superonasally. Accurately determining IOL power can be a challenge in such cases, because the corneal sutures will affect the keratometry readings, and I would assume that typical biometers will not be able to determine an accurate axial length, given the hydrated character of this cataract. Normally, I remove corneal sutures and wait a few weeks for the cornea to stabilize prior to proceeding, but I would not wait as long in this case, given the violation of the anterior and posterior capsules. I would remove the sutures and perform an A-scan along with measurements using the IOLMaster (Carl Zeiss Meditec) to help select the correct IOL. Moreover, assuming that both of his eyes were similar prior to the trauma, I would rely on the IOLMaster measurements of his right eye to help choose the appropriate IOL (with a slightly myopic goal to allow for easier laser vision correction in the future).
I would favor a combined case with a retina colleague, given the posterior capsular violation. I would consider performing a laser capsulotomy and would use a platform that has a liquid interface to prevent pressure on his recently repaired corneal wound. After staining the capsule with trypan blue dye, I would keep the anterior chamber pressurized throughout surgery in an effort to avoid extension of the capsular violation. In light of the patient’s age and rapidly developed cataract, I would avoid hydrodissection and would aspirate out the hydrated nucleus and cortex. Next, a pars plana vitrectomy (PPV) would be performed to clean up the fragments already present in the vitreous cavity. Depending on the status of the capsule, I would place a three-piece IOL either in the bag (preferred) or the sulcus. In case the bag is completely compromised, I would be prepared to scleral tunnel fixate a three-piece IOL. Lastly, I would perform a pupilloplasty to make sure that no edge of the IOL was exposed and to normalize the pupil’s shape.


CYNTHIA MATOSSIAN, MD, AND SEBASTIAN LESNIAK, MD
Because the outcome of complex repairs is not always predictable, it is important to set realistic expectations for patients from the beginning.
We would attempt to remove the sutures from the corneal laceration repair if the wound is stable so as to get the best approximation of keratometry readings prior to cataract extraction. Next, we would schedule the case with a retina surgeon to combine cataract extraction and IOL implantation with a PPV. Given that the posterior capsule is open, the risk of vitreous presentation and dropped nuclear fragments is high.
If we were able to create an anterior CCC with the aid of trypan blue, we would implant a three-piece IOL in the bag along with a capsular tension ring. If the violation of the anterior capsule is such that a CCC cannot be created, then a three-piece sulcus lens could be used if the anterior capsule provided enough support; otherwise, a three-piece sclera-glued IOL or sclera-sutured IOL such as the Akreos AO60 IOL or the CZ70BD lens (Alcon) would have to be considered. Because a vitrectomy is planned, the PPV incisions could be used for the sclera-sutured IOL. Given that this is a traumatic cataract, zonular compromise is likely, and a sclera-sutured IOL may be the best long-term option.
The corneal scarring appears to be near the limbus and outside the visual axis. Any resultant irregular astigmatism could be corrected with a rigid gas permeable contact lens.

WHAT I DID: BRANDON D. AYRES, MD
The patient was scheduled for cataract removal with anterior vitrectomy and iris repair. Given the known violation of the posterior capsule, a retina surgeon was on standby in the event that I was not able to manage the lens from an anterior approach. Keratometry readings from the right eye were used as a substitute for the left eye for IOL measurements.
My first concern was making the capsulorhexis in an eye with a violated anterior capsule. I decided to start the CCC in the area of capsular violation by using a pair of microscissors. I encountered several areas of capsular fibrosis during creation of the CCC, making the step more challenging, but ultimately, I was able to start and finish the tear at the location of the initial violation.
Removing the lenticular material was surprisingly easy. All that was necessary was bimanual I/A; no phacoemulsification was needed. I removed the lenticular and cortical material surrounding the area of the posterior capsular perforation last to prevent vitreous prolapse. Using a dispersive OVD, I observed no vitreous prolapse during lens removal or cortical cleanup.
Upon close inspection, a violation of the posterior capsule was clear, with fibrosis surrounding the area of perforation. I carefully positioned a single-piece acrylic IOL in the capsular bag and made sure the haptics were completely within intact capsule.
I instilled a miotic agent to reduce the pupil’s size and performed a small iridoplasty using 10–O Prolene to repair a small iris defect caused by the nail injury. Then, I administered triamcinolone (Triesence; Alcon) in the anterior chamber and performed a small vitrectomy to make sure no vitreous had inadvertently prolapsed during the case. The corneal sutures were removed at the conclusion of the case.
In summary, I was able to safely extract a traumatic cataract and place a PCIOL in the capsular bag in a patient with known anterior and posterior capsular violation. No vitreous was encountered intraoperatively, and no lenticular material was lost to the posterior segment of the eye.
Section Editor Lisa Brothers Arbisser, MD
• emeritus position at Eye Surgeons Associates, the Iowa and Illinois Quad Cities
• adjunct associate professor, John A. Moran Eye Center, University of Utah, Salt Lake City
Section Editor Brandon D. Ayres, MD
• surgeon on the Cornea Service, Wills Eye Hospital, Philadelphia
• (484) 434-2700; bayres@willseye.org
• financial disclosure: consultant to and speaker for Alcon and Bausch + Lomb
Section Editor Audrey R. Talley Rostov, MD
• private practice with Northwest Eye Surgeons, Seattle
• SightLife global partner
Asha Balakrishnan, MD
• cataract, cornea, and refractive surgeon at Colvard-Kandavel Eye Center, Encino, California
• (818) 906-2929; sabalakrishnan.md@gmail.com; Twitter @AshaBalaMD
• financial interest: none acknowledged
D. Michael Colvard, MD
• clinical professor of ophthalmology, Keck School of Medicine, University of Southern California, Los Angeles
• director, Colvard-Kandavel Eye Center, Encino, California
• (818) 906-2929; mike@mcolvard.com
• financial interest: none acknowledged
Nicole R. Fram, MD
• private practice, Advanced Vision Care, Los Angeles
• clinical instructor of ophthalmology, Jules Stein Eye Institute, University of California, Los Angeles
• (310) 229-1220; nicfram@yahoo.com
• financial disclosure: consultant/advisor to and lecturer for Alcon; lecturer for Bausch + Lomb
Sumit “Sam” Garg, MD
• vice chair of clinical ophthalmology; medical director; director of technology; and associate professor of cataract, corneal, and refractive surgery at the Gavin Herbert Eye Institute, University of California, Irvine
• gargs@icu.edu
• financial disclosure: consultant to and speaker for Abbott Medical Optics
Sebastian Lesniak, MD
• in practice with Matossian Eye Associates, with locations in Pennington and Hamilton, New Jersey, and Doylestown, Pennsylvania
• slesniak@matossianeye.com
• financial interest: none acknowledged
Cynthia Matossian, MD
• owner, founder, and chief medical officer, Matossian Eye Associates, with locations in Pennington and Hamilton, New Jersey, and Doylestown, Pennsylvania
• clinical instructor, Department of Ophthalmology, School of Medicine of Temple University, Philadelphia
• cmatossian@matossianeye.com
• financial interest: none acknowledged