
Multifocal IOLs have been a big part of our practice for the past 8-plus years. My colleagues and I were early adopters of and have increasingly become advocates of this IOL technology, as it has evolved to better serve our patients.
Following the Array lens (Abbott Medical Optics [AMO]), the first commercially successful multifocal IOLs were the Acrysof ReStor IOL +4.0 D (Alcon) and the ReZoom Multifocal (AMO). Although these lenses showed promise, they had drawbacks: distance vision was not perfect, reading in dim light could be problematic, and haloes could be distracting. Despite the compromises involved, many patients still enjoyed the benefits of simultaneous near and distance vision after cataract surgery. To be successful with these early lenses, however, my colleagues and I adopted the mantra to “underpromise and overdeliver.”
THE EVOLUTION
The next step in the evolution of multifocal IOLs was the aspheric AcrySof IQ Restor lens (Alcon), which was eventually offered with a lower (+3.00 D) add. Having a lens design that corrected for spherical aberration was a big improvement in terms of the image contrast. Then, the Tecnis Multifocal IOL (AMO) was introduced. With correction for both spherical aberration and chromatic aberration, in my experience, it produced crisper, high-quality distance vision. This lens was also more pupil independent than previous multifocal IOLs, making people with large pupils good candidates and allowing patients to enjoy their near vision even in dim light.1
As good as these lenses were, we still had to manage our patients’ expectations because of nighttime halos and deficits in intermediate vision.
LOW-ADD MULTIFOCAL IOLs
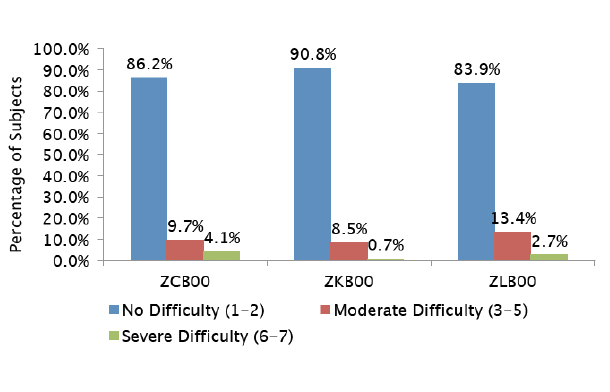
Figure 1. In the Tecnis low-add multifocal clinical trials, patient reports of difficulty with night vision were similar among the tested IOLs and the monofocal control.
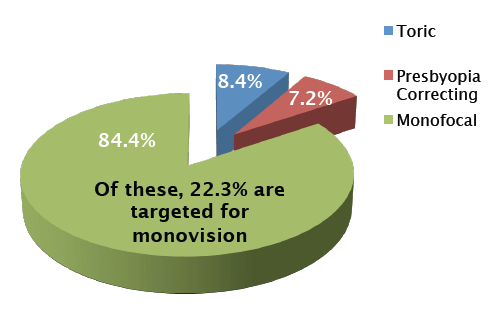
Figure 2. In our practice, 80% of patients get some form of refractive cataract surgery, and about 30% of all the lenses we implant are multifocal IOLs. This is well above the average of 7.2% and above the 15% that respondents to the 2014 ASCRS Clinical Survey4 indicated they expect to see in their practices within the next couple of years.
Both of the aforementioned problems have been addressed by the latest generation of low-add multifocal IOLs, including two on the Tecnis Multifocal platform (ZKB00 and ZLB00) and one on the AcrySof Restor platform (SN6AD2). I believe these lenses represent a major step forward.
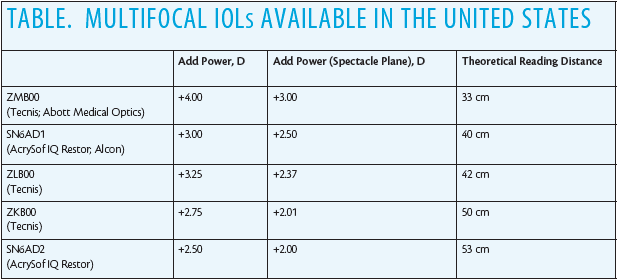
These lens options increase the number of patients who are good candidates for multifocal lenses by allowing physicians more options for selecting the best focal points (Table). In the past, it was not uncommon for me to have to dissuade a patient from choosing a multifocal IOL if he or she relied strongly on intermediate vision. For example, if the patient was an avid musician, I would spend time explaining how he or she would be able to read and drive but would likely have difficulty seeing the score on the music stand. The newest multifocals offer much better vision for intermediate tasks.
Perhaps the biggest myth I would like to dispel is that multifocality comes at a cost to distance vision. Although that might have been true with early lens designs, I do not believe it is the case now. In the clinical trials that led to FDA premarket approval of the lower-add Tecnis Multifocal and Acrysof ReStor models, there was no statistically significant difference in distance vision between patients with the tested multifocal IOLs and patients with their monofocal counterparts.1,2
Moreover, I am not asking patients to sacrifice good visual acuity at night anymore. All three new multifocal lenses have fewer diffractive rings than their higher-add predecessors, which means fewer and less noticeable nighttime halos.1,2
Newer-generation multifocal lenses perform well under nighttime contrast sensitivity testing. In the Tecnis low-add multifocal clinical trials, for example, patients’ reports of difficulty with night vision were similar among the tested IOLs and the monofocal control (Figure 1). Of the three lenses (ZCB00, ZKB00, and ZLB00), in fact, the monofocal had the highest rate of “severe difficulty” reported.3
PERSONAL EXPERIENCE
In our practice, patients’ satisfaction with low-add multifocal IOLs has been very high. The most frequently implanted lens now is the ZKB00, which surprised me.
Before the release of the ZLB00 (+3.25 D) and the ZKB00 (+2.75 D), I was an avid and satisfied user of the ZMB00 (+4.00 D). I began my transition by implanting the ZLB00 in the first eye, with the intention of having the option of either a ZKB00 or a ZMB00 in the fellow eye, depending on whether the near vision focal point of the first lens was too close or too far. Surprisingly, my patients did not request any adjustment, so my first 20 cases were all bilateral ZLB00 lenses. Satisfied with the ZLB00, I then experimented with the ZKB00 in an effort to minimize the potential for nighttime haloes. Now, I often start with the ZKB00, and although I sometimes combine it with a ZLB00 in the second eye, bilateral ZKB00 implants are the most common scenario. I expected patients would lose some desired reading vision, but that has not happened. Bilateral ZKB00 lenses seem to provide a very good functional balance of near, intermediate, and distance vision with the least amount of halos.
I also find the new lower-add IOLs to be quite forgiving. It is still important to optimize the ocular surface and hit the target refraction—good surgical protocols will always be important—but the lenses are more forgiving of small residual refractive error or ocular dryness in my experience. I also find them to be a far better option than surgical monovision for pseudophakic patients. When there are minor deviations from the intended refractive target, multifocal lenses allow the eyes to compensate for each other’s deficiencies. This is not possible with monovision, where refractive precision in each individual eye is more critical to patients’ satisfaction.
Two recent cases illustrate the wide range of patients who can benefit from multifocal IOLs. One of my first bilateral ZLB00 cases was a woman who had developed early cataracts. She had -18.00 D of myopia, had worn glasses since the fourth grade, and at the age of 50, had recently become presbyopic. After surgery, she is now plano and sees beautifully without spectacles at any distance. She reported that the experience has been life changing and that the resulting vision seemed very natural and fluid.
At the other end of the spectrum, I recently implanted multifocal IOLs in an elderly patient with mild dementia. I was initially skeptical that this nursing home-bound patient would benefit from the technology, but her daughter explained that, between her mother’s arthritis and dementia, she would often misplace or have trouble putting on her glasses. After surgery, her daughter noticed that her mother was more social and interactive.
MULTIFOCAL LENSES IN PRACTICE
In our practice, 80% of patients get some form of refractive cataract surgery, and about 30% of all the lenses we implant are multifocal IOLs. This is well above the average of 7.2% (Figure 2) and even above the 15% that respondents to the 2014 ASCRS Clinical Survey indicated they expect to see in their practices within the next couple of years.4
Demographics and geography certainly play a role, but I think any practice can be successful with multifocal IOLs by following these tips:
Do present the option to everybody, even if they are not candidates. Our patient education videos discuss laser cataract surgery and multifocal IOLs. If I have a patient with macular degeneration, I tell him or her why she is not a candidate. Patients have heard about this technology by doing online research or from friends. They appreciate knowing that these options were considered in their case and the reason why they will not be used. Also, those who are not candidates will be able to share information on the latest technology with their neighbors or family.
Do not assume patients cannot afford premium IOLs. I have heard countless times from my patients, “These are my eyes. What could be a more important investment?” Truly, patients will be looking through the lens every waking moment for the rest of their lives. Patients and their families will understand the value proposition and make the best decision for themselves. Do not make that decision for them.
Do not be intimidated or count yourself out if you do not have a femtosecond laser, intraoperative wavefront aberrometer, or other advanced technology. Although these tools are helpful, ophthalmologists can successfully become refractive cataract surgeons just by using the lates multifocal lenses in the appropriate patients.
Do start with the low-hanging fruit: patients with cataracts who have been dependent on glasses their whole life, who have little to no astigmatism, and who have no other ocular pathology.
CONCLUSION
The ability to see at near, far, and in between without glasses is clearly something patients want. In this sense, “conversion” is easy. What has not always been easy is meeting those expectations. Each iteration of multifocal IOLs has provided significant advantages, to the point that I do not think my colleagues and I need to underpromise anymore. With today’s technology, I have great confidence in being able to deliver the functional range and quality of vision that my patients want.
I expect the landscape will continue to get better with extended-range-of-vision lenses and, perhaps someday, adjustable lenses that let surgeons fine-tune lens power after implantation. Lower-add multifocal IOLs make this a great time right now, however, to be a multifocal IOL surgeon.
1. Tecnis Multifocal 1-Piece IOL, Models ZKB00 and ZLB00, and Tecnis Multifocal 1-Piece IOL, Model ZMB00 [package insert]. Santa Ana, CA: Abbott Medical Optics; 2014
2. FDA Summary of Safety and Effectiveness Data, AcrySof IQ Restor +2.5 D Multifocal Intraocular Lens, Model SV25T0. http://www.accessdata.fda.gov/scripts/cdrh/cfdocs/cfTopic/pma/pma.cfm?num=p040020s050. Accessed September 25, 2015.
3. FDA Summary of Safety and Effectiveness Data, Tecnis Multifocal 1-piece Intraocular Lens, Models ZKB00 and ZLB00. http://www.accessdata.fda.gov/scripts/cdrh/cfdocs/cfTopic/pma/pma.cfm?num=p980040s049. Accessed September 25, 2015.
4. Global Trends in Ophthalmology and the American Society of Cataract and Refractive Surgery. ASCRS Clinical Survey 2014. Published 2014. http://www.eyeworld.org/supplements/2014_ASCRS_clinical_survey.pdf. Accessed August 19, 2015.
5. Kretz FT, Gerl M, Gerl R, et al. Clinical evaluation of a new pupil independent diffractive multifocal intraocular lens with a +2.75 D near addition: a European multicentre study [published online ahead of print.]. Br J Ophthalmol. 2015. doi: 10.1136/bjophthalmol-2015-306811.
Paul C. Kang, MD
• partner at Eye Doctors of Washington in Chevy Chase, Maryland
• assistant clinical professor of ophthalmology at Georgetown University School of Medicine
• founder and current president of the Vanguard Ophthalmology Society
• pkang@edow.com
• financial disclosure: consultant to AMO, Alcon, and Allergan


