In this article, members of CRST‘s editorial board share their choices of the best this year had to offer. Because this article went to press before 2016 began, any developments from its last weeks are not included. Even so, the panel had plenty of material.
IOL Power Calculations
Philadelphia surgeon Richard Tipperman drew his pick from a presentation by Douglas Koch, MD, of a series of challenging IOL power calculations at the 2015 meeting of the American Society of Cataract and Refractive Surgeons (ASCRS).1 Dr. Tipperman singled out the case of a patient with high hyperopia for whom “almost all of the IOL power formulas predicted different strength implants. One of the points Dr. Koch made is that, for patients with an anterior chamber depth [ACD] of less than 2.6 mm, the surgical refractive result can be unpredictable because of issues with effective lens position. Although I had seen this clinically on occasion, I [had] never codified and [drawn] this conclusion and association with [a] shallow ACD.”
Dr. Tipperman continued, “As a result of Dr. Koch’s insight, I now counsel my patients with shallow ACDs (< 2.6 mm) in a very similar fashion to how one would counsel a postrefractive surgery patient requiring cataract surgery.”
IOL FIXATION
Kenneth A. Beckman, MD, of Westerville, Ohio, also focused on IOLs. “My choice for best surgical pearl was a tip I received from Brandon Ayers, MD, for suturing posterior chamber IOLs,” he said. “In the past, I preferred to use IOLs with an eyelet in the haptic for suturing, but these are not as readily available as before. I have tried suturing in IOLs without the eyelet in the haptic, but this is not as easy as it was with the eyelet. Brandon showed me a technique for suturing in the Akreos lens [Bausch + Lomb], which is a one-piece, four-haptic lens. Each of the haptics has an eyelet, which allows for easy suturing. His technique is very straightforward.” To view the technique, visit http://bit.ly/1k7cRyn.
Cathleen M. McCabe, MD, of Sarasota, Florida, also nominated a suturing technique involving this IOL. She favored how John Berdahl, MD, sews the AO60 model to the sclera. In particular, Dr. McCabe has found the pearl valuable in eyes that lack capsular support, especially those with dislocated IOL-capsular bag complexes in which sewing the original lens is not feasible. “I have been able to adapt the technique to preload the suture through the haptic and then in the cartridge so that a small incision size is maintained,” she remarked.
Also from Sarasota, William J. Lahners, MD, voted for expanded uses of the Hoffman pocket, as presented in an episode of the Video Journal of Cataract and Refractive Surgery posted this year on Eyetube.net.2 Dr. Hoffman “originally described the technique several years ago for recentering dislocated IOLs using a limbal pocket dissected posteriorly,” Dr. Lahners noted. “This novel technique of scleral fixation is unique in that it spares the conjunctiva from any dissection, and in the current video, Dr. Hoffman expands the use of the pocket to secondary IOL implantation, ring segments, and even iridodialysis repair.”
GONIOSYNECHIALYSIS
Lisa Brothers Arbisser, MD, of Davenport, Iowa, nominated advice given by Ike Ahmed, MD, during their discussion of a trauma case early this year. “Don’t fail to perform goniosynechialysis along with cataract surgery for patients with angle-closure glaucoma or peripheral anterior synechiae,” she said. “This is a simple maneuver, which can be done blindly or with visualization through intraoperative gonioscopy. Though viscodissection can sometimes be successful, simply grasping the peripheral iris with an intraocular forceps and pulling centrally most efficiently exposes closed areas of trabeculum. It is not uncommon for this manipulation to result in better IOP control postoperatively.”

CORTICAL REMOVAL
In the opinion of Marguerite McDonald, MD, of Rockville Centre, New York, the year’s best pearl came from Russell Fumuso, MD, a prominent high-volume cataract surgeon on Long Island. He developed the Fumuso cortical hydration technique for laser cataract surgery, she said, because cortical removal is noticeably more difficult than with standard phacoemulsification. It turns out, Dr. McDonald added, that the technique also works well with standard phacoemulsification.
“The tip of the cannula is not placed under the edge of the capsule during hydrodissection; it is placed just central to it but in the same plane so that the fluid jet goes just under the capsular edge (as usual) but also creates a jagged ‘cliff’ or plane between the nucleus and the cortex,” she explained. “The nucleus will spin freely, and the cortex will have been hydrated into many fluffy strings that are much easier to remove later during irrigation/aspiration. It is important to cut back on aspiration (from 25 to 20 mL/min) with this technique to slow everything down ever so slightly” in order to reduce the risk of rupturing the posterior capsule.
CORRECTING PRESBYOPIA
The quest for a better solution to presbyopia continues, and four panelists’ picks focus on this area of ophthalmology. Chief Medical Editor Steven J. Dell, MD, looked to the future when he chose a tip from Gustavo Tamayo, MD, on a population for whom to consider the Symfony IOL (Abbott Medical Optics; not FDA approved). Dr. Dell said he learned that the lens is well suited to patients with a history of corneal refractive surgery. “While this IOL physically resembles a multifocal, it is in fact not a multifocal,” he explained. “Instead, the lens offers an extended depth of focus without significant loss of contrast sensitivity. The extended depth of focus minimizes the impact of a small refractive target miss, while offering better near vision than a conventional IOL.”3
William I. Bond, MD, of Pekin, Illinois, kept his sights on the patient when he nominated a pearl from George O. Waring IV, MD: the key concept of dysfunctional lens syndrome is that, after the age of 55, the crystalline [lens] is a blank slate on which to write presbyopic correction and desired refractive goals—often simultaneously. “I believe this leads to the proper consideration of what patients really want,” Dr. Bond remarked.
Northeast of Dr. Bond in Lake Villa, Illinois, Mitchell A. Jackson, MD, selected a tip he received from two colleagues, Dr. Waring and Jeffery Machat, MD. The advice pertained to using the objective scatter index (OSI) on the AcuTarget HD (Visiometrics) to help determine whether a patient should undergo a corneal procedure (eg, LASIK, PRK, corneal inlay) or a lens-based procedure to treat presbyopia. Dr. Jackson explained, “Low light scatter or low OSI suggests good optical clarity and only a low-grade dysfunctional lens syndrome (stage 1 or 2), as established by Dr. Waring. High light scatter or high OSI suggests [a] poor quality of vision, either from true cataract formation or a poor ocular surface.”
Los Angeles surgeon Kevin M. Miller nominated the description by John Vukich, MD, of how to use recently FDA-approved software for the iFS laser (Abbott Medical Optics) to create pockets for the placement of corneal inlays.4 “These pockets should be much better than LASIK flaps for planning the depth of placement and centration of these devices with respect to the pupil, both of which are critical to their function,” Dr. Miller stated.
SURGICAL PLANNING
Y. Ralph Chu, MD, of Edina, Minnesota, was impressed when James Schumer, MD, demonstrated how he uses the TrueVision 3D Visualization and Guidance System (TrueVision Systems) in conjunction with the Victus femtosecond laser (Bausch + Lomb).5 “Not only was this interesting from the perspective of protecting the longevity of the surgeon (up to 70% of surgeons over [age] 50 have some type of neck issue6,7),” Dr. Chu said, but he was also intrigued by how the TrueVision system’s integration with the Cassini (i-Optics) helped to guide the alignment of toric IOLs and limbal relaxing incisions. Dr. Chu anticipates that further integration of preoperative diagnostic tools to provide real-time information in the OR will improve surgical outcomes in the future.
PUPILLARY EXPANSION
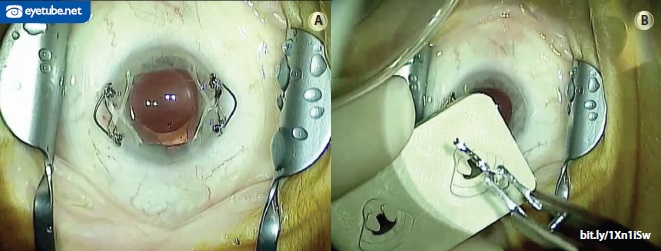
The sheer number of products and techniques for dealing with a small pupil during cataract surgery indicates the importance of this challenge, and innovation continues. P. Dee G. Stephenson, MD, of Venice, Florida, selected a technique to expand a small pupil with the APX 200 (APX Ophthalmology) demonstrated by Dr. Jackson (Figure 1). A user of the device now herself, Dr. Stephenson said, “It is faster and easier than any I have used. It requires two stab incisions. It expands the pupil to a trapezoidal shape, making it so easy to see and do your cataract surgery maneuvers without interference, and you don’t have to operate over the device. [The expander is] easy to remove and [causes] no harm to the iris. One size fits all.”
CATARACT SURGERY AFTER RADIAL KERATOTOMY
Cynthia Matossian, MD, of Doylestown, Pennsylvania, favored advice contained in a 2015 installment of CRST‘s “Cataract Surgery Complex Case Management” column.8 The article presented the case of a 63-year-old woman with unstable vision due to previous radial keratotomy who was contact lens intolerant. Of the many tips offered in the piece, Dr. Matossian highlighted the recommendation to be sure that such patients’ expectations are realistic.
REFRACTIVE ENHANCEMENTS
“We have learned a great deal about reactive epithelial hyperplasia after refractive surgery and have begun to take this into consideration for surface ablation enhancements,” commented Dr. Waring. He voted for a suggestion by William Wiley, MD, to “use intraoperative aberrometry after epithelial removal to determine the true refractive power of the cornea [after] epithelial debridement to help refine these treatments.”
PTERYGIUM
David A. Goldman, MD, of Palm Beach Gardens, Florida, selected a modification by William Trattler, MD, of the Anduze technique for the removal of pterygia with direct injection of mitomycin C and light cautery.9 “It makes surgery quick [and] safe, and the outcomes are outstanding,” Dr. Goldman said.
SKIN CARE
According to Chief Medical Editor Robert J. Weinstock, MD, the year’s best surgical pearl came from Luther Fry, MD, during the Caribbean Eye Meeting. Said Dr. Weinstock, “He described a technique of placing K-Y Jelly [Reckitt Benckler] on the patient’s forehead and cheek prior to placing the drape. This avoids the severe pain and skin damage that occur when peeling off the drape at the end of the case. Although [Dr. Fry] had been doing this for years, it was the first I had heard of it.” Dr. Weinstock stated that this pearl has greatly improved his patients’ experience.
LASER CATARACT SURGERY
Plenty of cataract surgeons have not invested in a femtosecond laser, and debate on laser versus manual techniques continues. It is therefore not surprising that Dr. Dell would single out the long-awaited results of the European Society of Cataract and Refractive Surgery’s study of laser cataract surgery (FLACS ESCRS Study), presented by Peter Barry, MD, at the XXXIII Congress of the ESCRS.10 According to Dr. Dell, investigators compared more than 2,800 eyes undergoing laser cataract surgery with rigorously matched controls from the European Registry of Quality Outcomes for Cataract and Refractive Surgery. They found that the overall complication rate and incidence of lost lines of vision were significantly higher in the laser versus the control group. According to Dr. Dell, these data show that, “while tremendous strides have been made with femto, there is still significant room for improvement.” For Prof. Barry’s own account of the study he presented, watch the interview at http://eyetube.net/?v=ulomi.
Dr. Chu was impressed by research in this field by Wendell Scott, MD.11 “He showed that, with increased spot spacing vertically, there were fewer irregularities [in the laser capsulotomy] and that he was able to perform a sub-1-second capsulotomy,” Dr. Chu commented. “This is exciting because we were able to be the first in the United States to replicate this using a different laser platform [Victus]. We found similar results and are conducting a clinical evaluation of this technique on our platform and hope to present this in the near future.”
CORRECTING PRESBYOPIA
Presbyopia was the most popular area of research among the panelists. Dr. Arbisser nominated a study showing that crossed monovision (dominant eye for near vs distance) is as effective a method as conventional monovision in pseudophakia.12 “The mean anisometropia was -1.39 D, and [the investigators] used [a] sighting dominance test preoperatively,” Dr. Arbisser said. “This definitively vindicates what I have found to be a successful strategy for thousands of cases over decades. After discussion of all options, when patients choose emmetropia, I operate [on] the eye with the worse cataract first for distance regardless of dominance. Assuming the goal is achieved, the patient can now understand [his or her] presbyopia, be shown what -1.25 D offers in focal distance, and have the option of aiming for the second eye to be intermediate versus distance corrected. Caution must be taken, however, in patients who have a lifelong experience with monovision not to switch eyes or those with very strong eye dominance and poor binocularity.” Dr. Arbisser added that work by Fuxiang Zhang, MD, to which she contributed supports these findings (unpublished data, 2015).
Impressed by its promise for the future, both Dr. Jackson and Dr. Waring voted for a computer-animated model of accommodation and presbyopia described by Daniel Goldberg, MD.13 “[It] has shed new light on a complex process involving previously poorly documented anatomic structures such as vitreous zones and capsule ligaments,” Dr. Waring remarked. Added Dr. Jackson, “[The model] demonstrates the extralenticular structures of accommodation moving in synchrony. [It] will pave the way on how industry will create accommodating IOLs in the future and help technologies invoking the scleral space for presbyopia therapy.”
Dr. Miller selected CRST‘s summary of the Kamra’s (AcuFocus) clinical trial, which included tips for the corneal inlay’s implantation and removal.14 “Physicians and patients in the United States have fallen behind the rest of the world with respect to access to new medical devices,” he remarked. “The reason is rigorous safety and efficacy mandates promulgated by the Food and Drug Administration. Finally, however, the first corneal inlay has cleared the phase 3 hurdle.”
IOL POWER CALCULATIONS
As with his pick for the best surgical pearl, Dr. Tipperman again went with the area of IOL power calculations. Specifically, he selected research presented by Graham Barrett, MD.15
“In recent years, ophthalmologists have become aware of the contribution of ‘posterior corneal astigmatism’ to the final refractive result achieved when performing cataract surgery with toric IOLs,” Dr. Tipperman stated. “In this paper, Dr. Barrett compared his toric IOL calculator (which is available on the ASCRS website) to several other common methods, including the Alcon Toric Calculator, the Baylor Nomogram, the Holladay calculator, and the Pentacam Comprehensive Eye Scanner [Oculus Surgical]. The paper demonstrated that the Barrett Toric Calculator would leave the greatest percentage of patients within ±0.50 D of their intended target refraction.”
According to Los Angeles surgeon Uday Devgan, “the absolutely most groundbreaking development in IOL calculations is the concept of a ‘super surface’ and ‘super formula’ to increase … accuracy. This will revolutionize the way we do IOL calculations.”16

ENDOPHTHALMITIS
Dr. Matossian selected what she called an informative installment of CRST‘s “The Literature” column that summarized a study by Nentwich and colleagues on endophthalmitis after cataract surgery.17,18 “To date, there are no approved standards for intracameral or transzonular antibiotics at the end of cataract surgery in the United States,” Dr. Matossian said. “I look forward to having guidelines as more studies review endophthalmitis rates post intracameral or transzonular antibiotic delivery.”
CORNEA
Dr. Lahners nominated a presentation at the World Cornea Congress VII in April by Shigeru Kinoshita, MD, PhD. Dr. Kinoshita described the use of injected cultivated corneal endothelial cells from a donor cornea into a patient with end-stage endothelial disease such as Fuchs dystrophy or pseudophakic bullous keratopathy, Dr. Lahners said. “The technique combines a suspension of approximately 1 million cultivated corneal endothelial cells and Rho kinase inhibitors,” he continued. “This procedure is not only much less invasive than current techniques such as Descemet stripping automated endothelial keratoplasty and Descemet membrane endothelial keratoplasty, but through cell cultures, a single donor can provide enough cells for over 200 patients.”
Dr. Lahners provided further details: “In his presentation, [Dr. Kinoshita] described the use of the technique in 11 patients, one of which started with a BCVA of 20/400 and a corneal thickness of 778 µm. This patient improved to a BCVA [of] 20/20 and a thickness of 525 µm postinjection. This is truly amazing research and promises to completely revolutionize the future of transplantation for endothelial diseases. I have been telling my patients with early Fuchs dystrophy for years that transplantation techniques have improved vastly in the last 10 years from penetrating keratoplasty to Descemet stripping automated endothelial keratoplasty/Descemet membrane endothelial keratoplasty, and one day, we will probably just be able to inject new cells into the eye. It looks like we are rapidly closing in on this day!”
In Dr. Bond’s estimation, William Trattler, MD, presented the year’s best review when he covered the history of corneal collagen cross-linking in the United States, including the procedure he performed on his own young daughter.19
REFRACTIVE SURGERY
Dr. McDonald selected 3-year data on small-incision lenticule extraction (SMILE; Carl Zeiss Meditec).20 More than 80,000 SMILE procedures have been performed worldwide, she said. “The clinical trial data are impressive, better than most refractive surgeons would have predicted,” she added. “It appears that SMILE will join our refractive armamentarium in the United States, after it is FDA approved.”
GLAUCOMA
Microinvasive glaucoma surgery may be a hot topic at cataract and refractive surgery meetings, but Richard Mackool, MD, of Astoria, New York, went with research on therapeutics. He selected an “elegant study [that] provided electroretinographic evidence that the use of citicoline eye drops [was] effective in improving retinal function and neural conduction along the visual pathways in open-angle glaucoma. The improved function was demonstrated to be reversible upon discontinuation of the drug. This information may lead to the development of a new class of antiglaucoma medications that does not lower IOP but nonetheless protects the eye from damage by possibly improving microcirculation to the retina and/or optic nerve.”21
LOW-ADD MULTIFOCAL IOLs
With five votes, low-add multifocal IOLs were the top choice of CRST‘s panel for the technology of the year. In 2015, Abbott Medical Optics released 2.75 D and 3.25 D models of its Tecnis Multifocal IOL (ZKB00 and ZLB00, respectively), and Alcon brought the AcrySof IQ Restor +2.5 D IOL to market. These additions to the +4.00 D models of both lenses and the +3.00 D version of the AcrySof IQ Restor give surgeons a wide range of add powers from which to choose. That flexibility “greatly improves our ability to customize lens choices to the patient’s needs, goals, and health of the eye,” commented Dr. McCabe. “Having more choices improves our ability to balance the strengths and weaknesses of each type of lens so that we best meet patients’ expectations. I always assess the performance of the first lens implanted to adjust, if necessary, the choice for the second eye.”
Speaking specifically about the ZKB00 and ZLB00, Dr. Dell remarked, “These low-add multifocal IOLs feature a reading zone that corresponds more closely to the visual needs of our patients. The original version of the Tecnis Multifocal IOL forced patients to read too closely for comfort in many cases, and computer vision was a significant problem. Having the ability to titrate the reading zone with the patient’s habitual reading distance has changed our practice pattern. These two new lenses also offer improved quality of vision over prior multifocals. Perhaps the best overall indicator of patients’ acceptance of these lenses comes from the FDA trial leading to their approval, where 94% of ZLB00 and 97% of ZKB00 recipients would select the same IOL again if they had to do it over again.22 These are the best numbers for patient satisfaction with a multifocal that I’ve ever seen.”
In Dr. Matossian’s experience, patients are far less likely to report problems with glare and halos with the low-add models of the Tecnis Multifocal. “The intermediate vision is excellent for computer monitors, e-tablets, and seeing the dashboard or GPS system while driving without compromising the distance vision,” she said. “The near vision is very good; in myopes, I mix and match by using the ZKB00 with the +2.75 D add in the dominant eye and the ZLB00 with the +3.25 D add in the nondominant eye for excellent near vision.” For hyperopic patients, Dr. Matossian implants the ZKB00 bilaterally.
Dr. Waring reported that he and his colleagues routinely implant the ZKB00 bilaterally. “We begin with the dominant eye first in the event the patient desires more near, in which case we will mix and match with the ZLB00,” he said.
According to Dr. Mackool, for all practical purposes, the distance acuity provided by the AcrySof IQ Restor +2.5 D IOL “is equal to that of an aspheric monofocal IOL. The importance of this simply cannot be overemphasized.” In addition, he said, “virtually every patient who receives this IOL will have better intermediate and near vision than they would have achieved with an aspheric monofocal lens.” He continued, “Were it not for the small possibility of troublesome postoperative glare and halo, I would readily confer the title of ‘no downside’ upon this lens. In our practice, many risk-averse patients are now candidates for multifocal IOL implantation because of the availability of the AcrySof IQ Restor +2.5 D IOL.”
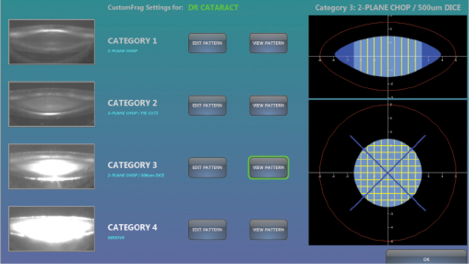
Figure 2. The Lensar Laser System with Streamline automatically categorizes cataract density and then performs
the preselected pattern for the appropriate cataract hardness.
LASER CATARACT SOFTWARE UPGRADE
Coming in a close second in the technology category was the Streamline upgrade to the Lensar Laser System (Lensar), nominated by four panelists (Figure 2). Remarked Dr. Lahners, “This update allows for automated analysis of the lens density and programmable [customized] fragmentation solutions. It also seamlessly allows for detailed and innovative arcuate incision planning using iris registration to compensate for cyclotorsion and more precise placement. This system integrates with the Cassini via a Wi-Fi connection for maximum efficiency and reduction in potential transcription errors. The Lensar Laser System has always proven itself to be efficient and intelligent; with Streamline, it takes the automation concept to a new level.”
Dr. Weinstock stated that the upgrade has had a real effect on his patients’ outcomes and that it has optimized his phaco technique. For Dr. Stephenson, the most important change is “the automatic fragmentation patterns based on the density of the cataract imaging, which allows the [laser] energy to be as efficient as possible and decreases the amount of phaco power needed. … In the grades 1 and 2 category, zero phaco power is needed; only aspiration is needed, which is healthier for the cornea, and the outcomes have been impressive.”
In Dr. Jackson’s estimation, the introduction of this technology “has paved the way for a true ‘hands-free’ approach to modern-day refractive cataract surgery.”

INTRAOPERATIVE ABERROMETRY
Dr. Tipperman also chose technology that helps him to analyze data for cataract surgery—VerifEye+ for the ORA System (Alcon). He and his colleagues incorporated intraoperative aberrometry using this system in 2015, and he said that they and the nursing staff have been pleased with its ease of use thus far. “By incorporating the alignment and capture screens into a ‘heads-up’ display on the microscope’s oculars, the process of data acquisition is much easier,” he commented. “Additionally, changes in the software have allowed the data acquisition and processing to be much faster so that 40 measurements are taken in 10 seconds.” Dr. Tipperman highlighted a poster presentation by Robert Cionni, MD, at this year’s ASCRS symposium on using intraoperative aberrometry for toric IOL surgery.23 Specifically, Dr. Cionni found that use of the ORA System with VerifEye+ halved the number of patients in whom outcomes fell more than 0.50 D outside the intended astigmatic target, Dr. Hoffman said.
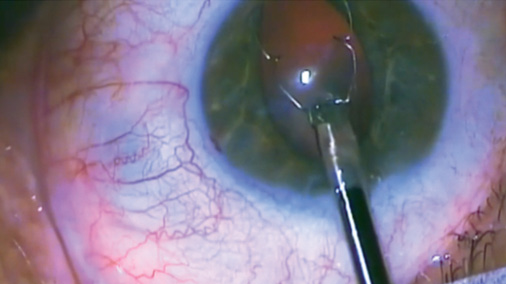
Figure 3. Dr. Chu injects the Xpand NT Iris Expansion System through a 2.75-mm clear corneal incision.
PUPILLARY EXPANSION
Dr. Chu selected the Xpand NT Iris Expansion System (Diamatrix), an expander ring made of nitinol (Figure 3). “It provides an excellent, stable, large, open pupil and can be reused, making it one of the most cost-effective devices on the market—a win for patients and a win for doctors,” he stated. “[It is] definitely worth trying for any surgeon who does cataract surgery.”
IMAGING
When choosing the best technology of 2015, Dr. Goldman went with his staff’s pick, the California (Optos). “It has the excellent widefield imaging with small pupils that the earlier models have, but it also is designed with chin- and headrests and can be controlled by the technician to make image acquisition easy in patients of all ages,” he said. “It shares a similar small footprint with the earlier Daytona model, so it’s easy to integrate into any office. My office acquired it only a month ago, and already, all staff say it’s their favorite piece of equipment we have.”
1. Koch D. Challenges In IOL power calculations. Presented at: ASCRS/ASOA Symposium and Congress; April 17-19, 2015; San Diego, CA.
2. Hoffman RS. A spectrum of scleral fixation without conjunctival dissection. Video Journal of Cataract Surgery. http://bit.ly/1MF9WbM. Accessed October 15, 2015.
3. Tamayo G. Case 1: patient with prior corneal refractive surgery now having IOL surgery seeks reduced spectacle dependence. Paper presented at: AECOS Summer Symposium; August 2, 2015; Deer Valley, UT.
4. Vukich JA. Hot pockets. Cataract & Refractive Surgery Today. April 2015;15(4):47-49. http://crstoday.com/2015/04/hot-pockets. Accessed October 15, 2015.
5. Schumer J. Presentation at: Optimal Outcomes Summit; September 19, 2015; Washington, DC.
6. McDonald J. ACES Ergonomic Survey, 1995 and 1996. Paper presented at: American College of Eye Surgeons (ACES), 1996 Annual Meeting; 1996; Walt Disney World, FL.
7. Wallace RB 3rd. The 45 degree tilt: improvement in surgical ergonomics. J Cataract Refract Surg.
1999;25(2):174-176.
8. Devgan U, Miller KM, Waring IV GO, Weinstock RJ. Cataracts after radial keratotomy. Cataract & Refractive Surgery Today. March 2015;15(3):22-25. http://crstoday.com/2015/03/cataracts-after-radial-keratotomy. Accessed October 15, 2015.
9. Trattler WB. Primary pterygia excision performed via Anduze technique with mitomycin-c 0.02% applied to subconjunctival space: review. Paper presented at: ASCRS/ASOA Congress and Symposium; April 17-21, 2015; San Diego, CA.
10. Barry P. FLACS ESCRS Study. Paper presented at: XXXIII Congress of the ESCRS; September 7, 2015; Barcelona, Spain.
11. Increased vertical spacing reduces femtosecond laser capsulotomy irregularities. Ocular Surgery News U.S. edition. August 10, 2015. http://bit.ly/1OIR1Ni. Accessed October 16, 2015.
12. Kim J, Shin HJ, Kim HC, Shin KC. Comparison of conventional versus crossed monovision in
pseudophakia. Br J Ophthalmol. 2015;99(3):391-395.
13. Goldberg D. Computer-animated model of accommodation and presbyopia. J Cataract Refract Surg. 2015;41:437-445.
14. Koury CB. Inlay to treat presbyopia gets US approval. Cataract & Refractive Surgery Today. June 2015;15(6):61-63.
15. Barrett GD. Improving the prediction of astigmatism after toric IOL implantation. Paper presented at: ASCRS/ASOA Congress and Symposium; April 17-21, 2015; San Diego, CA.
16. Ladas JG, Siddiqui AA, Devgan U, Jun AS. A 3-D “super surface” combining modern intraocular lens formulas to generate a “super formula” and maximize accuracy [published online ahead of print October 15, 2015]. JAMA Ophthalmol. doi: 10.1001/jamaophthalmol.2015.3832.
17. Loh J. The literature. Cataract & Refractive Surgery Today. April 2015;15(4):30-32. http://crstoday.com/2015/04/the-literature. Accessed October 18, 2015.
18. Nentwich MM, Ta CN, Kreutzer TC, et al. Incidence of postoperative endophthalmitis from 1990 to 2009 using povidone-iodine but no intracameral antibiotics at a single academic institution. J Cataract Refract Surg. 2015;41(1):58-66.
19. Trattler W. CXL in eyes with previous surgery. Paper presented at: Advance Refractive Congress; August 2, 2015; Deer Valley, UT.
20. Pederson IB, Ivarsen A, Hjortdal J. Three-year results of small incision lenticule extraction for high myopia: refractive outcomes and aberrations [published online ahead of print October 2, 2015]. J Refract Surg. doi:10.3928/1081597X-20150923-11.
21. Parisi V, Centofanti M, Ziccardi L, et al. Treatment with citicoline eye drops enhances retinal function and neural conduction along the visual pathways in open angle glaucoma. Graefes Arch Clin Exp Ophthalmol. 2015;253(8):1327-1340.
22. Abbott Medical Optics. Tecnis Multifocal 1-piece intraocular lens (IOL)-models ZKB00 (+2.75 D) and ZLB00 (+3.25 D). http://bit.ly/1NQ9sRG. Accessed October 19, 2015.
23. Cionni RJ. Axis determination by intraoperative aberrometry versus toric calculator. Poster presented at: ASCRS/ASOA Symposium & Congress; April 17-19, 2015; San Diego, CA.
Lisa Brothers Arbisser, MD
• emeritus position at Eye Surgeons Associates, the Iowa and Illinois Quad Cities
• adjunct associate professor, John A. Moran Eye Center, University of Utah, Salt Lake City
• (563) 343-8896; drlisa@arbisser.com
• financial interest: none acknowledged
Kenneth A. Beckman, MD
• clinical assistant professor of ophthalmology at Comprehensive EyeCare of Central Ohio, Ohio State University, Westerville, Ohio
• (614) 890-5692; kenbeckman22@aol.com; Twitter @kab822
• financial disclosure: consultant to Bausch + Lomb
William I. Bond, MD
• cataract and refractive surgeon at Bond Eye Associates, Peoria, Illinois
• assistant clinical professor, University of Illinois Medical School, Peoria, Illinois
• pekineye@yahoo.com
Y. Ralph Chu, MD
• founder and medical director, Chu Vision Institute, Edina, Minnesota
• (952) 835-0965; yrchu@chuvision.com
• financial disclosure: consultant to Bausch + Lomb/Valeant
Steven J. Dell, MD
• medical director, Dell Laser Consultants, Austin, Texas
(512) 327-7000
• financial disclosure: consultant to Abbott Medical Optics and Bausch + Lomb
Uday Devgan, MD
• private practice, Devgan Eye Surgery, Los Angeles
• clinical professor of ophthalmology, Jules Stein Eye Institute, UCLA
• chief of ophthalmology, Olive View UCLA Medical Center
• (800) 377-1969; devgan@gmail.com; Twitter @devgan
David A. Goldman, MD
• private practice at Goldman Eye, Palm Beach Gardens, Florida
• (561) 630-7120; david@goldmaneye.com
• financial interest: none acknowledged
Mitchell A. Jackson, MD
• founder and CEO, Jacksoneye, Lake Villa, Illinois
• mjlaserdoc@msn.com; Twitter @djmjspin
• financial disclosure: consultant to i-Optics and Lensar; investor in ACE Vision Group
William J. Lahners, MD
• medical director and director of laser visions services, Center for Sight, Sarasota, Florida
• (941) 925-2020; wjlahners@centerforsight.net
• financial interest: none acknowledged
Richard J. Mackool, MD
• director, Mackool Eye Institute and Laser Center, Astoria, New York
• (718) 728-3400, ext. 256; mackooleye@aol.com
• financial disclosure: consultant to Alcon
Cynthia Matossian, MD
• founder and CEO of Matossian Eye Associates, with offices in Pennsylvania and New Jersey
• clinical instructor/adjunct faculty member, Temple University School of Medicine in Philadelphia and Robert Wood Johnson Medical School in New Brunswick, New Jersey
• cmatossian@matossianeye.com
• financial disclosure: consultant to Abbott Medical Optics
Cathleen M. McCabe, MD
• cataract and refractive specialist practicing at The Eye Associates of Bradenton and Sarasota, Florida
• (941) 792-2020; cmccabe13@hotmail.com
• financial disclosure: consultant to, speaker for, and research support from Alcon and Bausch + Lomb; consultant to Allergan
Marguerite McDonald, MD
• cornea/refractive specialist with Ophthalmic Consultants of Long Island, New York
• clinical professor of ophthalmology, NYU School of Medicine, New York
• adjunct clinical professor of ophthalmology, Tulane University Health Sciences Center, New Orleans
• (516) 593-7709; margueritemcdmd@aol.com
• financial interest: none acknowledged
Kevin M. Miller, MD
• Kolokotrones chair in ophthalmology, David Geffen School of Medicine at UCLA, Jules Stein Eye Institute, Los Angeles
• (310) 206-9951; kmiller@ucla.edu
• financial disclosure: investigator for and consultant to Alcon
P. Dee G. Stephenson, MD
• president, American College of Eye Surgeons
• private practice, Stephenson Eye Associates, Venice, Florida
• associate professor of ophthalmology, University of South Florida College of Medicine, Tampa
• (941) 468-6363; eyedrdee@aol.com; Twitter @deestep03136405
• financial disclosure: speaker for Bausch + Lomb, i-Optics, Lensar, and Omeros
Richard Tipperman, MD
• attending surgeon, Wills Eye Hospital, Philadelphia
• (484) 434-2716; rtipperman@mindspring.com
• financial disclosure: consultant to Alcon
George O. Waring IV, MD
• director of refractive surgery and an assistant professor of ophthalmology, Storm Eye Institute, Medical University of South Carolina
• medical director, Magill Vision Center, Mt. Pleasant, South Carolina
• waringg@musc.edu; Twitter @georgewaring
• financial disclosure: consultant to Abbott Medical Optics
Robert J. Weinstock, MD
• director of cataract and refractive surgery, Eye Institute of West Florida, Largo, Florida
• rjweinstock@yahoo.com; Twitter @EyeInstituteWFl
• financial disclosure: consultant to Lensar