CASE PRESENTATION
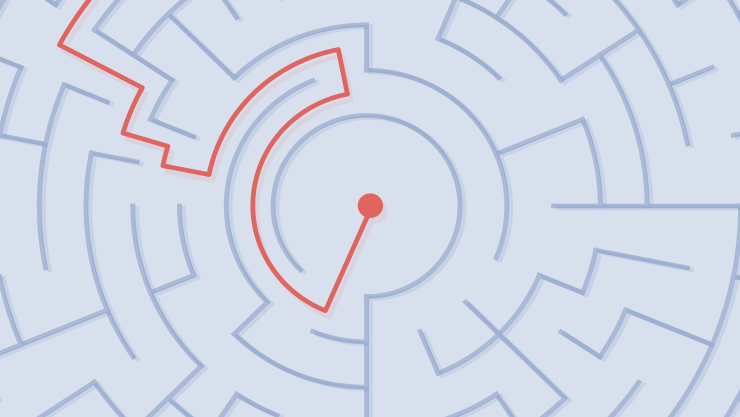
Planned, routine surgery for a visually significant cataract was wrapping up on a 72-year-old man with no history of significant trauma or pseudoexfoliation. The IOL was placed prior to the removal of a section of residual subincisional cortical material. The surgeon thought that placing the IOL would keep the posterior capsule from coming forward during cortical cleanup. During this step, however, the anterior capsule was caught, and the zonules in this area sustained damage (Figure 1A). An inspection after the cessation and removal of I/A revealed several clock hours of zonular damage but an intact capsular bag (Figure 1B).
How would you proceed?
—Case prepared by Thomas A. Oetting, MS, MD.
HARIPRIYA ARAVIND, MS
This interesting situation is not uncommon, especially if the capsulorhexis is small. The zonular damage is probably more than 5 clock hours. If there is vitreous prolapse, a bimanual anterior vitrectomy will clear the area of vitreous. A dispersive ophthalmic viscosurgical device like Viscoat (Alcon Laboratories, Inc.) would help to plug the area of zonular loss and push the vitreous back as well as distend the capsular bag.
I would stabilize the anterior capsular rim using capsule or iris retractors (Figure 2); approximately three hooks would be necessary to cover this 5- to 6-hour zonular loss. This step would help to open the bag anteriorly, which would facilitate the insertion of a capsular tension ring (CTR) and prevent further zonular loss. With the IOL still in the bag, I would insert a CTR through the paracentesis while taking care to ensure that both of its eyelets were in the bag.
There is a strong possibility that the IOL will center with the CTR. Because there is no cause for progressive zonular loss, postoperatively, the IOL should remain stable. If the IOL-capsular bag complex did not center with the CTR, however, the bag could be fixated to the sclera using an Ahmed Capsular Tension Segment (CTS; Morcher GmbH, distributed in the United States by FCI Ophthalmics, Inc.) and a 9–0 Prolene suture (Ethicon, Inc.; Figure 3). I would favor the CTS here over the Cionni Ring for Sclera Fixation (Morcher GmbH, distributed in the United States by FCI Ophthalmics, Inc.), because I find the latter more cumbersome to dial with an IOL in the bag. In contrast, being a standalone device, the CTS is implanted directly at the site of zonular dialysis. This combination of capsular retractors, a CTR, and a CTS should help with the centration and stability of the IOL (Figure 4).
SOOSAN JACOB, MS, FRCS, DNB
An intraoperatively subluxated bag-IOL complex with residual subincisional cortex and possibly vitreous loss is visible. The extent of subluxation necessitates scleral fixation of the bag. At this stage, I would opt for the glued endocapsular ring (designed by myself, manufactured by Epsilon Eye Instruments; not available in the United States).
I would create a 2.5- × 2.5-mm scleral flap centered on the dialysis. After performing a triamcinolone-assisted anterior vitrectomy, I would create a 20-gauge sclerotomy under the scleral flap. Made of polyvinylidene fluoride, the glued endocapsular ring has two arms that go into the capsular bag and expand the fornix, a double-scrolled Malyugin type of locking mechanism to engage the rim of the capsulorhexis, and a haptic that fixates the bag transsclerally (Figure 5). The handshake technique will exteriorize the haptic through the sclerotomy. Next, I would place the arms within the bag, and the double scrolls would engage the rim of the capsulorhexis. Pulling the exteriorized haptic will center the bag. I would cut the haptic to the desired length and tuck it into a coat hangertype, 26-gauge, intrascleral Scharioth tunnel. After stabilizing the bag in this way, I would perform bimanual I/A to remove the residual cortex. Finally, I would close the scleral flap and conjunctiva with fibrin glue.
The advantages of this approach include its speed; its easy intraoperative adjustability; sturdy scleral fixation; its not requiring the surgeon to maneuver long, thin needles inside the eye; and a lesser risk of posterior drop of the segment as well as less pseudophakodonesis compared with sutured rings/ segments. The approach also avoids suture-related complications, because no sutures are used for the procedure.1 In a case series, this technique provided intra- and postoperative vertical and horizontal stability to the capsular bag and its contents as well as equatorial expansion of the bag (Figure 6).2
KEITH A. WALTER, MD
The surgeon has several options at this point, but some may be better than others, depending on his or her skill level. The key here is to prevent vitreous from prolapsing around the lens capsule, which could result in a vitreous wick syndrome and hence cystoid macular edema or a retinal detachment. A second goal is to maintain stability and centration of the IOL. Both of these concerns could be easily addressed by the placement of a CTR. These devices are now readily available in the United States and easy for even an inexperienced surgeon to use. If the ophthalmologist were not comfortable with CTRs or one were not available, however, then he or she could carefully manipulate the haptic of the IOL in the area of the zonular weakness. This technique would push the capsule outward in that area and, one hopes, reduce the chance of vitreous prolapse. In addition, a miotic should be administered to constrict the pupil, thus helping to prevent vitreous from presenting to the wound.
WHAT I DID: THOMAS A. OETTING, MS, MD
I decided to place an Ahmed CTS and suture it into place. I did not think that a standard CTR without a suture would provide adequate support.
After making a conjunctival peritomy in the region of the damaged zonules, I placed both arms of a 9–0 Prolene suture via an external approach through the sclera, under the iris, and out through the cornea while avoiding the lens capsule. Both needles were cut off. I pulled one side of the suture through the main incision and placed this free end through the central eyelet of the CTS. The CTS was placed into the anterior chamber and positioned such that the device was in the bag along with the IOL and the eyelet was anterior to the capsule. I used an internal sliding knot to tie the CTS to the sclera under the iris.
After this procedure, the IOL centered nicely, and I observed little pseudophakodonesis.
Section Editor Bonnie A. Henderson, MD, is a partner in Ophthalmic Consultants of Boston and an assistant clinical professor at Harvard Medical School.
Section Editor Tal Raviv, MD, is an attending cornea and refractive surgeon at the New York Eye and Ear Infirmary and an assistant professor of ophthalmology at New York Medical College in Valhalla.
Section Editor Thomas A. Oetting, MS, MD, is a clinical professor at the University of Iowa in Iowa City. He acknowledged no financial interest in the products or companies he mentioned. Dr. Oetting may be reached at (319) 384-9958; thomas-oetting@uiowa.edu.
Haripriya Aravind, MS, is head of department, Cataract & IOL Services, Aravind Eye Hospital, Madurai, Tamil Nadu, India. She acknowledged no financial interest in the products or companies she mentioned. Dr. Aravind may be reached at +91 452 4356100; haripriya@aravind.org.
Soosan Jacob, MS, FRCS, DNB, is a senior consultant ophthalmologist at Dr. Agarwal's Eye Hospital in Chennai, India. She acknowledged no financial interest in the product or company she mentioned. Dr. Jacob may be reached at +91 442 8112811; dr_soosanj@hotmail.com.
Keith A. Walter, MD, is an associate professor of ophthalmology at the Wake Forest School of Medicine, Winston-Salem, North Carolina. Dr. Walter may be reached at kwalter@wfubmc.edu.
- Jacob S, Agarwal A, Agarwal A, et al. Glued endocapsular hemi-ring segment for fibrin glue-assisted sutureless transscleral fixation of the capsular bag in subluxated cataracts and intraocular lenses. J Cataract Refract Surg. 2012;38(2):193-201.
- Jacob S, Agarwal A. Glued endocapsular hemi-ring segment for fibrin glue assisted sutureless trans-scleral fixation of the capsular bag in subluxated cataracts and IOLs: a new device. Poster presented at: ESCRS Annual Meeting; September 8-12, 2012; Milan, Italy.